Treatment Interventions To Ameliorate Cardiovascular Autonomic Dysfunction Via Nonpharmacological Agents
It is well known that exercise plays an important role in the treatment of diabetes. The role of exercise in the improvement of cardiovascular autonomic function is not as clear. Numerous studies both in diabetic and nondiabetic populations have tried to determine whether HRV can be improved by exercise. For example, chronic endurance exercise training in sedentary adult males and a single bout of submaximal endurance exercise in healthy males were associated with increased HRV with a shift toward parasympathetic influence on cardiovascular function. Endurance training was also shown to improve vagal activity in nondiabetic patients who had a MI and in insulin-requiring diabetic individuals with early CAN . Other studies showed no benefit or only minimal benefit for healthy men and individuals with type 2 diabetes . The discordant findings are most likely due to differences in patient populations, lack of randomization, differences in length and type of exercise, and various measurements of autonomic function. Thus, more intervention studies are needed to determine the best exercise protocol that results in improved autonomic function for diabetic persons with CAN. In addition, it will be important to evaluate whether beneficial effects in autonomic function result in favorable effects on the clinical outcome of these patients.
Angiotensin Type 1 Blockers
Angiotensin type 1 receptor mediates all potentially deleterious effects of angiotensin II . AT1 antagonists block the AT1 receptor, thus blocking the harmful effects of angiotensin II. We conducted a 1-yr clinical trial in 44 diabetic individuals to determine the effect of losartan on HRV. We hypothesized that losartan would improve nerve function by increased nerve blood flow and inhibition of angiotensin II-induced facilitation of sympathetic neurotransmission. Although 50 mg of losartan appeared to slow the expected decline in RR variation, there was no significant improvement . Improved cardiovascular autonomic function was, however, shown in another study, in which 23 diabetic individuals were treated with 100 mg of losartan for 1 yr . Twelve weeks of treatment of losartan was also shown to reduce muscle sympathetic activity and improve cardiac baroreceptor sensitivity for 10 nondiabetic males with hypertension . In contrast, a 7-d trial in nondiabetic males treated with eprosartan was shown to lower HRV .
What Problems Does Diabetic Neuropathy Cause
Peripheral neuropathy can lead to foot complications, such as sores, ulcers, and infections, because nerve damage can make you lose feeling in your feet. As a result, you may not notice that your shoes are causing a sore or that you have injured your feet. Nerve damage can also cause problems with balance and coordination, leading to falls and fractures.
These problems may make it difficult for you to get around easily, causing you to lose some of your independence. In some people with diabetes, nerve damage causes chronic pain, which can lead to anxiety and depression.
Autonomic neuropathy can cause problems with how your organs work, including problems with your heart rate and blood pressure, digestion, urination, and ability to sense when you have low blood glucose.
Don’t Miss: What Do You Give A Diabetic With High Blood Sugar
Symptoms Of Peripheral Neuropathy
Peripheral neuropathy tends to develop slowly over months or years. In general, symptoms may include:
- Reduced feeling or numbness in the feet.
- Over time, tightness, burning, shooting, or stabbing pain in the feet, hands, or other parts of the body. Bone and joint deformities can develop, especially in the feet .
- Greatly reduced or greatly increased sensitivity to light touch or temperature.
- Weakness and loss of balance and coordination.
What Causes Diabetic Neuropathy
Over time, high blood glucose levels, also called blood sugar, and high levels of fats, such as triglycerides, in the blood from diabetes can damage your nerves. High blood glucose levels can also damage the small blood vessels that nourish your nerves with oxygen and nutrients. Without enough oxygen and nutrients, your nerves cannot function well.
You May Like: Cauliflower Pizza Crust For Diabetics
Heart Rate Response To Standing
To test the heart rate response to standing, the patient is connected to the heart rate monitor while in the supine position. The patient then stands to a full upright position, and the ECG is monitored for an additional period while standing. Standing causes an immediate rapid increase in heart rate with the maximum rate generally found at or around the 15th beat after standing. The heart rate slows at or around the 30th beat. The heart rate tracing is used to calculate the ratio of the longest R-R interval after the stand to the shortest R-R interval . This measure, called the 30:15 ratio, reflects the overall condition of the parasympathetic fibers. Normal ranges are age dependent.
Figure 1
Treatment Interventions To Ameliorate Cardiovascular Autonomic Dysfunction Via Pharmacological Agents
Interventions to ameliorate reduced HRV are being evaluated in clinical trials based on theories of the pathogenesis of diabetic neuropathy. Development of diabetic neuropathy is the result of a multifactorial process including metabolic insult to nerve fibers, neurovascular insufficiency, increased oxidative stress, reduction in neurotrophic growth factors, deficiency of essential fatty acids, formation of advanced glycosylation end products, and autoimmune damage . Various pharmacological agents that are directed at components of the pathogenic process are described below.
Also Check: Does Diabetes Cause Red Eyes
Can Diabetic Neuropathy Be Prevented
Keeping your blood sugar levels in your target range, set with your doctor, may help prevent neuropathy from ever developing. The best way to do this is by checking your blood sugar and adjusting your treatment. It is also important to get to and stay at a healthy weight by exercising and eating healthy foods.
The Stomach And Autonomic Neuropathy
If neuropathy affects the vagus nerves, which help to control the functioning of the stomach, a condition called gastroparesis develops. Gastroparesis causes emptying of the stomach to become impaired leading to food staying in the stomach too long. This can result in symptoms such as abdominal bloating, nausea, heartburn and unpredictable changes in blood glucose levels.
Read more on the symptoms and treatment of gastroparesis
Also Check: When Are You Diagnosed With Type 2 Diabetes
Assessing Cardiovascular Adrenergic Function
Systolic blood pressure response to standing.
Blood pressure normally changes only slightly on standing from a sitting or supine position. The response to standing is mediated by sympathetic nerve fibers. In healthy subjects, there is an immediate pooling of blood in the dependent circulation resulting in a fall in blood pressure that is rapidly corrected by baroreflex-mediated peripheral vasoconstriction and tachycardia. In normal individuals, the systolic blood pressure falls by < 10 mmHg in 30 s. In diabetic patients with autonomic neuropathy, baroreflex compensation is impaired. A response is considered abnormal when the diastolic blood pressure decreases more than 10 mmHg or the systolic blood pressure falls by 30 mmHg within 2 min after standing . A task force of the American Academy of Neurology and the American Autonomic Society defined orthostatic hypotension as a fall in systolic blood pressure of 20 mmHg or diastolic blood pressure of 10 mmHg accompanied by symptoms .
Diastolic blood pressure response to sustained handgrip.
Response to tilting.
Sweating And Temperature Regulation Problems
Autonomic neuropathy may affect the nerves that control sweating.
- Reduced sweating is common, especially in the hands and feet. It may be hard to recognize when your blood sugar is dropping because sweating is one of the main symptoms of low blood sugar. You can develop dry skin that may be more prone to cracking, injury, and infection. Profuse sweating of the torso, face, or neck may occur at night or while eating.
- Changes in the body’s ability to regulate temperature may make you more prone to body chilling or heat-related illness, such as heatstroke or heat exhaustion.
You May Like: How Much Is Insulin At Walmart
Relationship Between Cass And Asp
presents the Spearman correlations between CASS and ASP scores for the type 1 and type 2 diabetic groups. As shown, the pattern of correlations differed somewhat between groups. Among the type 1 patients, the most significant relationships were among CASS and secretomotor, urinary, sleep, and pupillomotor symptoms. In contrast, there were virtually no significant relationships between the CASS and the ASP in patients with type 2 diabetes. Correlations that are significantly different between patients with type 1 and type 2 diabetes are presented in bold.
How Is Dan Diagnosed
DAN is diagnosed based on symptoms, by taking a family and medical history and by performing a physical exam which includes checking the heart rate and blood pressure , and other tests to check for different types of autonomic nerve damage. Other causes of digestive symptoms will need to be ruled out, for example through gastric emptying studies. For urinary complaints an abdominal ultrasound to check the bladder function may be performed.
Don’t Miss: How To Tell If Diabetes Is Affecting Your Feet
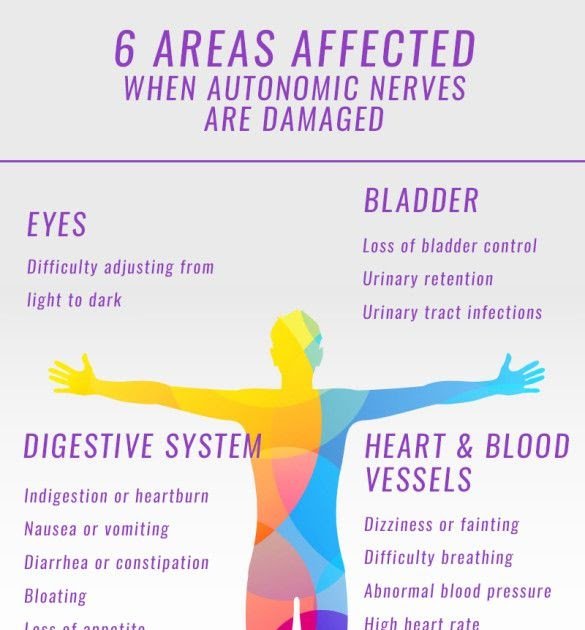
Symptoms Of Autonomic Diabetic Neuropathy
The symptoms of autonomic neuropathy are different depending on the area of the body that has been affected. Lets discuss them one by one.
1. Heart Rate and Blood Pressure
When the nerves responsible for heart rate and blood pressure are affected, they begin to respond slowly. Because of this, you may faint when you stand up suddenly from lying down or sitting, or when you are doing any physical activity or exercise. You might feel fluctuations in your heart rate. The heart rate might speed up or slow down.
Nerve damage around this area is so bad that it prevents you from feeling chest pain even when you are having a heart attack, or when your heart is unable to receive enough oxygen.
2. Digestive System
Diabetic neuropathy can cause damage to the nerves in the digestive system as well. after which you notice the following:
- nausea,
Nerve damage in the bladder will show up the following symptoms:
- no feeling to urinate
- leaking drops of urine
4. Sex Organs
When nerves present in sex organs are affected due to diabetic neuropathy, men suffer through:
- erectile dysfunction
- problems with ejaculation
And when women are badly affected by diabetes, the nerves in the sex organs get damaged due to which she suffers through dryness in the vagina while having sex. It also happens that a woman might feel less sensation around the vagina or have difficulty having an orgasm.
5. Eyes
Diabetes affects your vision, you may:
How Is Diabetic Neuropathy Diagnosed
Your doctor will check how well you feel light touch and temperature and will test your strength and your reflexes. Tests such as electromyogram and nerve conduction studies may be done to confirm the diagnosis. You may need other tests to see which type of neuropathy you have and to help guide your treatment.
Doctors can’t test for all types of nerve damage. So it’s important to tell your doctor about any pain or weakness you feel. Also mention heavy sweating or dizziness and any changes in digestion, urination, and sexual function.
Also Check: What Foods To Eat For Insulin Resistance
Treatment For Diabetic Autonomic Neuropathy
Treatment focuses on managing the symptoms of autonomic neuropathy. For example, taking medicines and eating small, frequent meals that are low in fiber and fat may help digestive problems like gastroparesis. Or you may take medicines for urinary or blood pressure problems. Medicines, lubricants, and creams may help with sexual problems.
Association Of Cerebrovascular Disease And Can
The frequency of ischemic cerebrovascular events is increased in individuals with type 2 diabetes. The impact of autonomic dysfunction on the risk of the development of strokes was examined by Toyry et al. , who followed a group of 133 type 2 diabetic patients for 10 years. During the study period, 19 individuals had one or more strokes. Abnormalities of parasympathetic and sympathetic autonomic function were found to be independent predictors of stroke in this cohort .
Also Check: What Eye Problems Does Diabetes Cause
Management Implications Of Cardiovascular Autonomic Neuropathy
Identifying individuals at risk is only the first step in managing patients and ultimately affecting outcomes. After identification, effective management must be provided. Proactive measures are required, because if those patients at high risk or those shown to be in early stages are not treated until advanced symptomatology is present, little has been achieved.
Unfortunately, information presented at the fifth Regenstrief conference on the intensive management of type 2 diabetes indicated that physicians may feel that screening is not of value because treatment options for identified complications are limited . Such a view does not take into account the clinical research advances that have been made in the treatment of diabetes. Tests that provide evidence of further health consequences may bring patients to medical attention before other signs of diabetic end-organ injury emerge, making proactive treatment, particularly the establishment of intensive diabetes care, possible. The results of autonomic function testing can contribute to good patient management in the following ways.
Assessing Cardiovascular Autonomic Function
Quantitative tests of autonomic function have historically lagged behind measures of motor nerve function and sensory nerve function deficits. The lack of interest in the development of such measures was partly due to the erroneous but commonly held view that autonomic neuropathy was only a small and relatively obscure contributor to the peripheral neuropathies affecting individuals with diabetes .
In the early 1970s, Ewing et al. proposed five simple noninvasive cardiovascular reflex tests that have been applied successfully by many. The clinical literature has consistently identified these five tests as they have been widely used in a variety of studies. The tests are valid as specific markers of autonomic neuropathy if end-organ failure has been carefully ruled out and other potential factors such as concomitant illness, drug use , lifestyle issues , and age are taken into account. A large body of evidence indicates that these factors can, to various degrees, affect the cardiovascular ANS and potentially other autonomic organ systems .
Heart rate response to deep breathing .
Heart rate response to standing.
Valsalva maneuver.
The response to performance of the Valsalva maneuver has four phases and in healthy individuals can be observed as follows:
The Valsalva ratio is determined from the ECG tracings by calculating the ratio of the longest R-R interval after the maneuver to the shortest R-R interval during or shortly after the maneuver .
Power spectral analysis.
Read Also: Does Sleeve Gastrectomy Cure Diabetes
What Are The Symptoms Of Autonomic Neuropathy
4.7/5What are the symptoms of autonomic neuropathycausesymptomssymptoms
Also, is autonomic neuropathy curable?
Cardiovascular autonomic neuropathy is associated with high risk of sudden cardiac death. Regardless of what the condition is called, and contrary to the common misperception, autonomic dysfunction is treatable.
One may also ask, what causes autonomic neuropathy? An abnormal attack by the immune system that occurs as a result of some cancers can also cause autonomic neuropathy. Diabetes, especially with poor glucose control, is the most common cause of autonomic neuropathy. It can gradually cause nerve damage throughout the body.
Likewise, people ask, how is autonomic neuropathy diagnosed?
To diagnose autonomic neuropathy, your doctor may use a few tests to assess changes in your heart rate in response to simple movements such as deep breathing or standing. Your doctor may also use tests to check your sweat function to know how your nerves and sweat glands are working.
What are the symptoms of autonomic dysfunction?
Symptoms of autonomic dysfunction
Prevention And Reversibility Of Cardiac Autonomic Neuropathy

Prevention of CAN should be a primary focus of lifestyle and other clinical interventions. Intense glycemic control utilizing a step-by-step progressive lowering of hyperglycemia, lipids, and BP, in addition to the use of antioxidants and ACE inhibitors , reduces the odds ratio for CAN . In the EDIC study, patients with T1DM showed continuously favorable effects of past glucose control on microvascular complications in spite of the loss of glycemic separation . CAN progressed in both treatment groups during the EDIC follow-up, but the prevalence and incidence continued to be decreased in the previous intensive group compared to the standard group despite comparable levels of glycemic control. To diminish the development of CAN, intense glucose control of T1DM ought to be started as soon as possible . However, in patients with established CAN, glycemic control may need to be less stringent to avoid hypoglycemia and adverse drug effects . The American Diabetes Association also recommends that individuals with CAN have a cardiac evaluation before starting or increasing physical activity for safety reasons .
Also Check: Diabetes Kidney Failure Life Expectancy
Safety Of Testing Procedures
An expert panel from the AAN reviewed a number of standardized measures and found that noninvasive autonomic tests were found to have a high value-to-risk ratio . Some tests do, however, carry a small risk for an adverse event. The Valsalva maneuver transiently increases intrathoracic, intraocular, and intracranial pressure, creating, for example, a small theoretical risk of intraocular hemorrhage and lens dislocation . In practical terms, the risk is minimal because comparable intrathoracic pressures occur in the performance of daily activities. In the published literature of over 100 studies, there have been no reports of deaths during testing and no reports of adverse events after completion of the tests attributable to the procedures. The Diabetes Control and Complications Trial , one of the largest trials to use cardiovascular autonomic function tests, evaluated 1,441 patients with type 1 diabetes in 29 centers over a mean duration of 6.5 years without procedural complications . When used by properly trained individuals, autonomic function tests are a safe and effective diagnostic tool.
Patient cooperation is required for performing autonomic function tests. Thus, children may pose some challenges related to performance and the cooperation and attention requirements of the test situation. These same challenges may also apply to elderly patients, where deterioration of physiological response is of concern, and to developmentally and cognitively disabled individuals.
Treatment Of Autonomic Diabetic Neuropathy
Treatment for this type of diabetic neuropathy depends on the symptoms and the affected areas. For example, if the nerves in your digestive system are affected badly your doctors would ask you to change your diet to treat digestive problems. He might prescribe some medicines if need there be.
They will advise you to follow a proper bathroom routine because the damage caused to the nerves in the bladder prevents you know when the bladder is full and there is a need for you to pee. In case of bladder infection, the doctors will prescribe some medicines.
For erectile dysfunction, some devices or medicines are recommended. For curing vaginal dryness as a result of diabetic neuropathy, gynecologists suggest lubricants.
Don’t Miss: Protein Shake For Diabetic Patients