What Are Diabetic Feet
People with diabetes often have problems with their feet. Diabetic feet develop sores, deformities and infections more easily.
If not treated quickly, a diabetic foot ulcer or blister can get infected. Sometimes a surgeon must amputate a toe, foot or part of the leg to prevent the spread of infection.
Foot Problems That Might Mean You Have Diabetes
Did you know there is a connection between your feet and diabetes? Diabetes is a condition in which the level of glucose in the blood is too high. This is caused by a problem with the hormone insulin and its role in controlling blood glucose levels. Diabetes may lead to higher risk of health complications including developing foot problems.
Every five minutes an Australian develops diabetes
The number of people with diabetes in Australia is three times higher today than it was 25 years ago. Every day, 280 Australians develop diabetes. That’s around one person every five minutes. Around 1.7 million Australians have diabetes and don’t even know it.In the Yarra Ranges, the number of people with diabetes has risen by nearly 180% over the past ten years and each week seven new cases are diagnosed.
Is diabetes affecting you feet?Having diabetes may increase your risk of developing related complications that include nerve damage or poor circulation in your feet. Nerve damage may affect how you feel pressure or pain and may lead to numbness in your toes or feet. Changes to your circulation may delay your ability to heal any cuts or sores, and may also increase your risk of developing ulcers that could even lead to amputations.
Seven signs to look out for
As feet are often the first place to show diabetes-related symptoms, it is important to get your feet checked by a podiatrist. Here are 7 signs and symptoms to look out for include:
What you can do to look after your feet
Signs Of Problems With Diabetic Feet
People with diabetes may not know that they are experiencing neuropathy. Up to 50% of diabetic peripheral neuropathy may be asymptomatic.
However, the most common symptoms of peripheral neuropathy include:
- Numbness
- Inability to feel hot and cold
- Changes to the shape of feet or toes
If you see any changes in your feet or have any physical symptoms, you should be examined by your healthcare provider. Early detection and treatment can prevent complications, such as injuries and ulcers.
Don’t Miss: Signs Of Diabetes In Toddler Girl
Peripheral Neuropathy And Diabetes
Diabetic foot pain is mainly due to a condition called peripheral neuropathy. Approximately 50% of people who have type 2 diabetes will develop peripheral neuropathy, which happens when high blood sugar levels cause damage to the nerves in the legs and the feet.
If you are frequently feeling foot pain, your type of neuropathy may be sensory, where even the slightest touch can cause overwhelming pain. The reaction is not proportional to the stimulus, because the nerves are overly sensitive.
Another type of peripheral neuropathy is motor neuropathy, wherein the nerves that connect to the muscles are weakened and therefore hurt. As a result, it may be a challenge to balance yourself with weakened legs and feet. This imbalance may lead to the development of corns, calluses, cuts, scrapes, and swelling.
For diabetics with motor neuropathy, customized orthotics may help address the balance issues and prevent the development of other foot issues. Its important that you keep your muscles in use so that your legs and feet stay strong.
Can I Prevent Diabetes
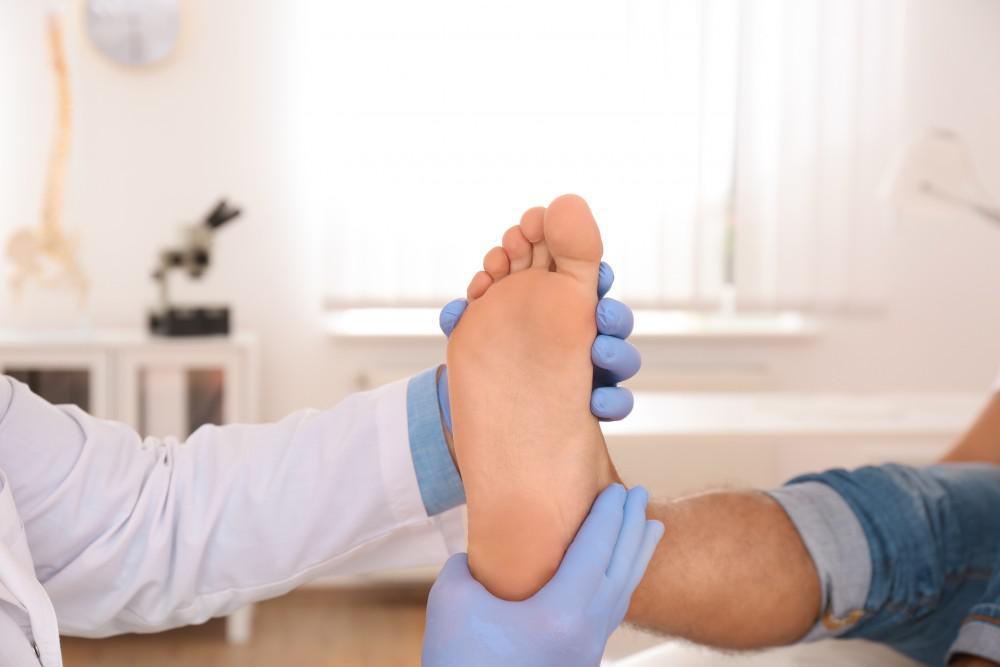
The best way you can prevent diabetes-related foot pain is by managing your diabetes as best as you can. Remember, high sugar levels is what causes the nerve pain. By managing your blood sugar levels through diet, exercise, and medications, youre taking steps to prevent the various complications of diabetes.
If youre already experiencing diabetes-related foot pain, its still important to manage your sugar levels. As we discussed, lowering your blood sugar can actually improve your symptoms. Talk to your doctor to discuss proper foot care and the best treatment options for you.
You May Like: Simple Diabetic Diet Meal Plan
Who Gets Charcots Foot
Charcots foot is most commonly seen in diabetic patients, but it can also be caused by other factors. These include injuries to the nerves or blood vessels of the lower legs and untreated high blood pressure which results in poor circulation.
The condition mostly affects people who have had diabetes for a while , although it can occur earlier.
When To See A Dermatologist
Diabetes can cause many other skin problems. Most skin problems are harmless, but even a minor one can become serious in people who have diabetes. A board-certified dermatologist can recognize skin problems due to diabetes and help you manage them.
Are all dermatologists board certified?
No. See what it takes to become board certified.
ImagesImage 1: Image Courtesy of Clark C. Otley, MD. All Rights Reserved
Images 3, 7, 8, 9: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2 from DermNetNZ
Some images used with permission of Journal of the American Academy of Dermatology
ReferencesCohen Sabban, EN. Cutaneous manifestations of diabetes mellitus from A to Z. Focus session presented at: 74th Annual Meeting of the American Academy of Dermatology March 4-8, 2016 Washington D.C.
Duff M, Demidova O, et al. Cutaneous manifestations of diabetes mellitus. Clinical Diabetes. 2015 33:40-8.
Kalus AA, Chien AJ, et al. Diabetes mellitus and other endocrine disorders. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine . McGraw Hill Medical, New York, 2008:1461-70.
McKinley-Grant L, Warnick M, et al. Cutaneous manifestations of systemic disease. In: Kelly AP and Taylor S. Dermatology for Skin of Color. . The McGraw-Hill Companies, Inc. China, 2009:481-4.
Morgan AJ and Schwartz RA. Diabetic dermopathy: A subtle sign with grave implications. J Am Acad Dermatol. 2008 58:447-51.
Read Also: How To Lower High Blood Sugar Without Insulin
When Should I Seek Medical Care For Diabetic Foot Pain
If you have diabetes, tell your healthcare provider right away if you experience:
- Any changes in foot shape.
- Any changes to the skin on the feet, including a wound, redness or darkness, warmth or a funny smell.
- Hair loss on your toes, feet or legs.
- Loss of feeling in the toes, feet or legs.
- Pain, tingling, burning or cramping in the feet or legs.
- Thick, yellow toenails.
Tip #: Watch Your Blood Sugar
Living with diabetes requires you to pay special attention to your health and your condition. Follow your doctor’s instructions regarding diet, exercise and medication. Keeping your blood sugar levels within the recommended range is one of the best things you can do to control your condition and protect your feet.
Also Check: How Do You Treat Diabetic Retinopathy
Signs Of Foot Issues With Diabetes
Poor blood circulation and blood flow can slow the healing process of sores on your feet, putting you at risk for serious life-threatening complications.
Even if you havent lost feeling in your feet, bring the following symptoms to your doctors attention. Signs of feet issues include:
You can avoid serious diabetes complications by seeing your doctor and getting treatment early for conditions that affect your feet.
What Can I Do To Care For My Feet And Prevent Problems
There are many things you can do to keep your feet healthy, such as:
You May Like: Ways To Manage Type 2 Diabetes
What Are Some Risks If I Dont Get Treatment
Diabetes-related foot pain is more than just pain its a warning sign from your body. This type of nerve pain can lead to complications if you dont see a doctor and get treated. Below are some of the problems that can come from untreated diabetes nerve pain:
-
Dry, cracked skin. This may not sound too bad, but when your skin is too dry, your risk of getting skin infections goes up. If this happens, plain petroleum jelly or unscented hand creams can help. Just avoid placing moisturizers between your toes.
-
. This is an area of thickened skin that has less feeling. People with diabetes get calluses faster and more often than those without diabetes. You can use a pumice stone daily to help keep them at a minimum. If they get really thick, a doctor can cut or shave them down. Never attempt to do this at home as it can lead to infections.
-
Ulcers. These are sores that happen to some people with diabetes due to poor blood circulation. All ulcers need to be seen by a doctor. The longer you go without seeing a doctor, the more likely it is that it will become infected. Infected ulcers can spread and cause you to lose your foot or leg.
-
Amputations. If the previously listed complications are not treated properly, they can all become infected. Skin infections can cause the skin and muscle tissues to die. Once this happens, it cant be fixed. The only way to stop the infection from continuing to spread is by amputating the infected limb.
Get A Foot Check At Every Health Care Visit
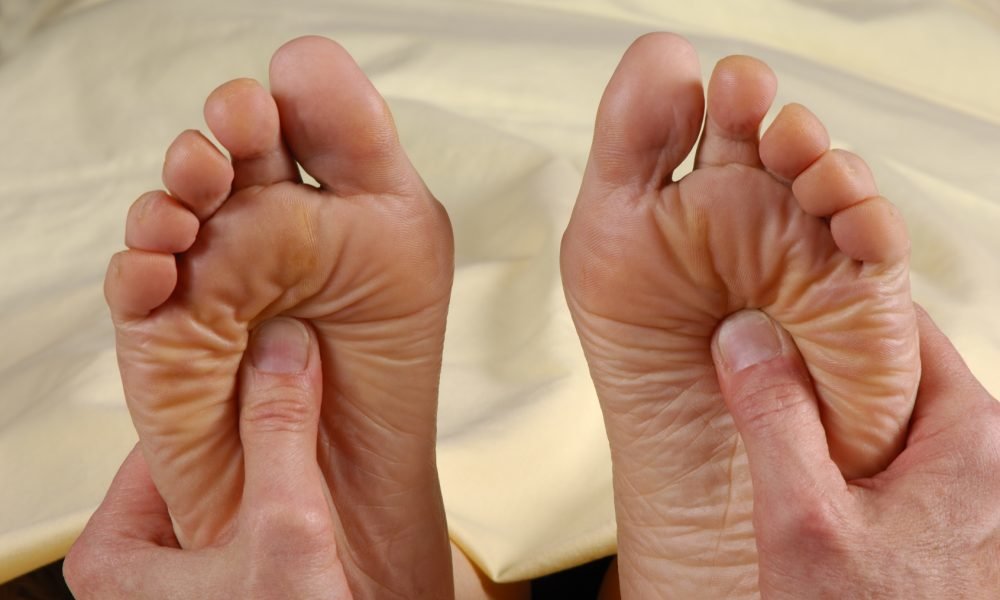
Ask your health care team to check your feet at each visit. Take off your shoes and socks when youre in the exam room so they will remember to check your feet. At least once a year, get a thorough foot exam, including a check of the feeling and pulses in your feet.
Get a thorough foot exam at each health care visit if you have
- changes in the shape of your feet
- loss of feeling in your feet
- had foot ulcers or an amputation in the past1
Ask your health care team to show you how to care for your feet.
Don’t Miss: What Is A Smart Insulin Pen
Peripheral Artery Disease Symptoms
Peripheral artery disease symptoms include:
- Intermittent claudication
In the most severe case, as mentioned above, due to a combination of decreased sensation and reduced blood flow to the feet, ulcers may develop. If the tissues continue to receive insufficient oxygen, tissue death occurs. Gangrene is a serious and potentially life-threatening condition. Other potentially serious problems that may develop include cellulitis and osteomyelitis also is possible.
People with diabetes are at increased risk for milder problems with the feet that are not specific to diabetes but may occur more frequently due to problems with the nerves and circulation to the feet.
Some of these conditions are:
- and corns, that may develop due to abnormal alignment of the feet or abnormal gait
- Fungal infections of the nails, which can appear as thickened, discolored, and at times brittle nails
- Tinea pedis, or athlete’s foot, a fungal infection of the skin of the feet
- Hammertoes, or bent toes due to muscle weakness.
- Bunions, or the angling of the big toe toward the second toe. The area of the bunion may become reddened and irritated, leading to formation.
Other types of foot problems can be relieved by proper footwear, sometimes with orthotic devices, and splinting or bracing. For some conditions like hammertoes, bunions, and ingrown toenails surgery may be necessary to correct severe cases.
How Diabetes Can Affect Your Eyes
There are several different ways that diabetes can cause eye complications. All of the following diseases can cause severe vision loss and even blindness.
Your vision is just one reason that regular blood tests should be performed and blood sugar levels need to be checked. Its also vital that annual eye appointments be made to track vision for any complications.
You May Like: How Can An Ophthalmologist Help A Diabetic
Diabetic People May Not Immediately Feel These Ulcers
DesPrés says patients don’t always notice that they have a wound or ulcer on their foot. This is because nerve damage, also known as neuropathy, is one of the “most common medical conditions associated with diabetes,” she saysand this condition can cause feelings of burning, tingling, and numbness in the feet, which can mask the pain of ulcers and lead to a total loss of sensation in the foot.
Neyla Lobkova, DPM, a board-certified podiatrist from NYC, further explains that neuropathy “occurs when there is a prolonged period of uncontrolled diabetes,” which means if you’re experiencing this, you likely have not yet been diagnosed with diabetes and are unaware you even have this condition. “When this occurs, cuts, blisters, and areas of excess friction aren’t able to be felt, and as the patient continues to walk, these sites can further break down to become an ulcer,” DesPrés says. And for more useful information delivered straight to your inbox, .
Foot Care For People With Diabetes
All people with diabetes should have their feet checked at least once a year by a doctor or podiatrist. This is important to detect problems early and to prevent ulcers and other complications. You may have heard it said that diabetes causes gangrene . Most cases of gangrene result from delayed treatment of foot injuries.
Read Also: Insulin How Much Does It Cost
The Basics Of Foot Complications
Although it can hurt, diabetic nerve damage can also lessen your ability to feel pain, heat, and cold. Loss of feeling often means you may not feel a foot injury. You could have a tack or stone in your shoe and walk on it all day without knowing. You could get a blister and not feel it. You might not notice a foot injury until the skin breaks down and becomes infected.
Nerve damage can also lead to changes in the shape of your feet and toes. If your foot doesnt fit comfortably in regular shoes, ask your doctor about special therapeutic shoes or inserts, rather than forcing your feet and toes into shoes that dont fit and can cause more damage.
Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. This problem is caused by nerve damage that affects your bodys ability to control the oil and moisture in your foot.
After bathing, dry your feet and seal in the remaining moisture with a thin coat of plain petroleum jelly, an unscented hand cream, or other such products. Do not put oils or creams between your toes. The extra moisture can lead to infection. Also, don’t soak your feetthat can dry your skin.
Using a pumice stone every day will help keep calluses under control. It is best to use the pumice stone on wet skin. Put on lotion right after you use the pumice stone.
Outbreak Of Small Reddish
When these bumps appear, they often look like pimples. Unlike pimples, they soon develop a yellowish color. Youll usually find these bumps on the buttocks, thighs, crooks of the elbows, or backs of the knees. They can form anywhere though.
Eruptive-xanthomatosis
These bumps appear suddenly and clear promptly when diabetes is well-controlled.
When these bumps appear, they often look like pimples. Unlike pimples, they soon develop a yellowish color. Youll usually find these bumps on the buttocks, thighs, crooks of the elbows, or backs of the knees. They can form anywhere though. No matter where they form, they are usually tender and itchy. The medical name for this skin condition is eruptive xanthomatosis.
Take action
- Tell your doctor about the bumps because this skin condition appears when you have uncontrolled diabetes.
- Talk with your doctor about how to better control your diabetes.
Don’t Miss: Is Bluechew Safe For Diabetics
Talk To A Professional
The thought of losing a limb is a very real threat if you have diabetes. The best way to avoid this is to care for your arms or legs and keep your blood sugar under control. But if you find yourself struggling to do this, consult a doctor. Go to a diabetes specialist or endocrinologist for help keeping your blood sugar under control. And go to a foot doctor or podiatrist to get checked for ulcers or other infections in your lower limbs.
The Orthopaedic Associates of Central Maryland can direct you to the professional that you need so you can get treated. Call 644-1880 today to ask about OACMs diabetic foot program. Alternatively, you can sign up through the online form to schedule an appointment.
What Can I Do To Keep My Feet Healthy
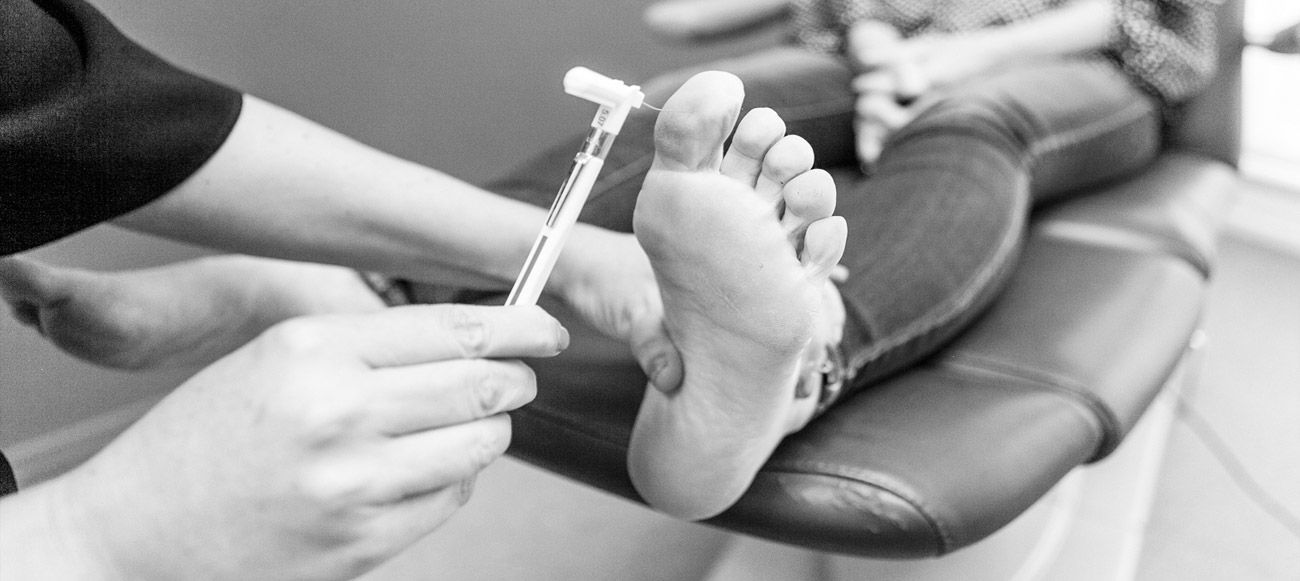
Work with your health care team to make a diabetes self-care plan, which is an action plan for how you will manage your diabetes. Your plan should include foot care. A foot doctor, also called a podiatrist, and other specialists may be part of your health care team.
Include these steps in your foot care plan:
Recommended Reading: How To Cure Early Signs Of Diabetes
What Preventative Steps Can I Take
If left untreated or unmanaged, foot problems can lead to problems such as losing a toe, foot, or leg. Keeping your diabetes well managed and preventing injury is the key to maintaining proper foot health.
In addition to managing your diabetes, there are some steps you can take to help further protect your feet from injury and infection. It is important to wash and check your feet daily and address any issues immediately to avoid further problems. Here are some preventative steps you can take:
- Keep your skin well moisturized, soft, and smooth.
- Gently smooth corns and calluses that may be on your feet.
- Trim your toenails straight across on a regular basis. If you are unable to reach your feet or do this safely, ask your podiatrist or a loved one to help you.
- Always wear shoes and socks, even when indoors. Unprotected feet can lead to increased risk of injury.
- Protect your feet from hot and cold temperatures. Wear socks that will keep your feet warm.
- Check your feet every day and report any abnormal changes to your doctor.
- Wear shoes that fit well and are designed for your specific condition and/or level of activity.
Let’s Talk
Contact Castro Podiatry to request an appointment or to request additional information about our services. We look forward to hearing from you.