Do I Have Other Treatment Options For My Diabetes
When medicines and lifestyle changes are not enough to manage your diabetes, a less common treatment may be an option. Other treatments include bariatric surgery for certain people with type 1 or type 2 diabetes, and an “artificial pancreas” and pancreatic islet transplantation for some people with type 1 diabetes.
The Different Insulin Types And How They Work
- Rapid-acting: Rapid-acting insulin starts working about 15 minutes after injection, peaks in about 1 hour and continues to work for 2 to 4 hours after injection. , insulin lispro , and insulin aspart
- Regular or Short-acting: Regular or short-acting insulin starts working 30 minutes after injection, peaks anywhere from 2 to 3 hours after injection, and continues to work for about 3 to 6 hours.
- Intermediate-acting: Intermediate-acting insulin starts working 2 to 4 hours after injection, peaks about 4 to 12 hours later, and lasts approximately 12 to 18 hours.
- Long-acting: Long-acting insulin is most often combined with rapid- or short-acting insulin. It starts working several hours after injection and tends to lower glucose levels up to 24 hours or almost a full day.
- Ultra long-acting: Ultra long-acting insulin starts working in 6 hours, but it does not peak and lasts about 36 hours, and in some cases longer than that.
Hyperglycemia And Diabetic Ketoacidosis
Studies have also shown improved glycemic control in patients using insulin pumps compared with patients using multiple daily insulin injections. Another study showed that the incidence of DKA is equivalent for pump users and patients on MDIs. In particular, nocturnal and predawn glycemic control is improved on insulin pump therapy, as hour-by-hour preprogrammed basal rate changes facilitated by the pump help counteract prebreakfast blood glucose increases that are not easily addressed with injection therapy.
However, hyperglycemia and DKA can occur with insulin pump use, whether due to user error in programming or to device malfunction. Studies show that device problems leading to hyperglycemia include diminished insulin delivery due to a depleted or malpositioned battery, occlusion or crimping of the cannula, disruption of the infusion set , or complete pump failure. DKA in particular occurs more frequently early after starting insulin pump use, suggesting that acclimation to the device has a learning curve.
Finally, continuous use of the same infusion set for an extended period increases the risk of cannula occlusion and changes the physiochemical environment at the delivery site, altering the rate of insulin absorption and increasing the risk of hyperglycemia, as well as other problems described below. One study has found that there was a slow but steady increase in average daily serum glucose concentrations as patients wore an infusion set continuously beyond 3 days.
Read Also: What Will Diabetes Do To Your Body
What Are The Advantages
Insulin pump users like managing their type 1 diabetes this way for lots of different reasons. Some of the most common reasons are:
- feeling like you are more in control
- having the flexibility to have a lazy morning, skip a meal or eat late
- delivering food boluses in the most appropriate way, eg spreading it over 7 hours for pizza
- setting a temporary basal increase or decrease when ill, having your cycle, or stressed
- managing the dawn phenomenon
- only needing one needle every 2 or 3 days
Insulin pump users may also find the following things easier:
- managing blood glucose levels around planned or spontaneous exercise
- treating hypers with precise correction doses
- treating hypos with just fast-acting carbohydrate
- managing changing shift work patterns
- managing toddlers meal-time battles
- keeping good control through growth spurts and hormonal changes in adolescence
How Do Insulin Pumps Work
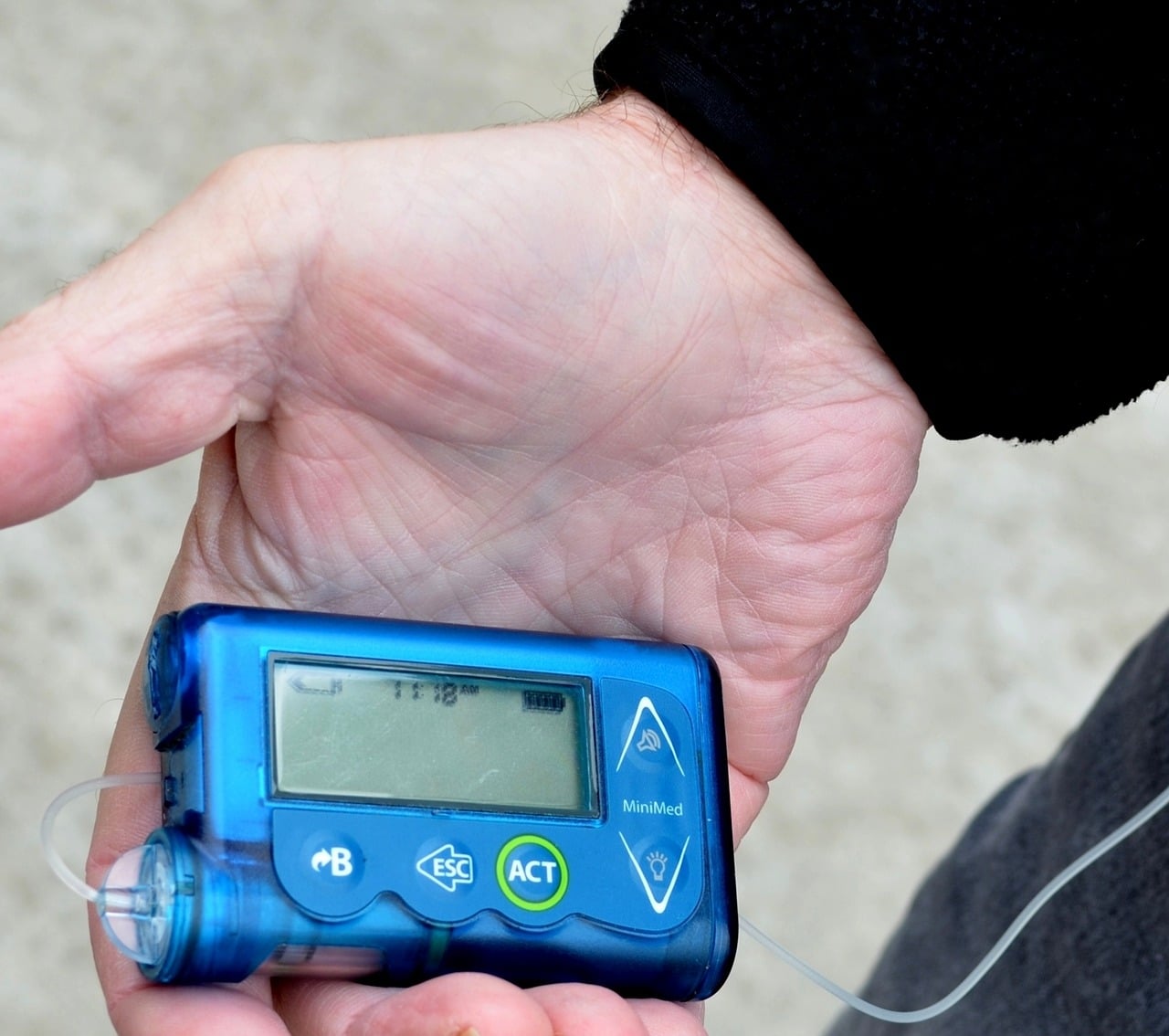
An insulin pump delivers a steady supply of insulin into your body using battery power. The device contains a reservoir that stores insulin, which attaches to your body through a fine tube called a cannula. The pump inserts the cannula into the fat under your skin. The device pumps insulin from the reservoir into your body.
Many insulin pumps use a remote control or smartphone app to programme the insulin pump. You can set the pump up to deliver a steady supply of basal insulin around the clock. When you eat or drink, you can count the carbs and add a bolus of insulin through the pump at the touch of a button.
At the moment, around one in a thousand people with diabetes in the UK have a pump- but they are becoming more popular. The NHS has quite strict requirements for pump eligibility. However, a wide range of pumps is available privately for adults and children living with diabetes.
Insulin pumps are beneficial for adults and children with type 1 diabetes, especially if it is brittle, very poorly controlled, requires multiple insulin injections or if there are frequent hypos or hypers. An insulin pump can also help people who are struggling with multiple insulin injections for type 2 diabetes.
You May Like: How Does Diabetes Affect Your Feet
Disadvantages Of An Insulin Pump
- Youâll need to enter information into the pump all day and change out the infusion set every few days.
- Youâll need to commit to using it safely, including checking your blood sugar to make sure the pump is working right. Otherwise, you risk a life-threatening problem called diabetic ketoacidosis .
- Youâll need training to learn to use the pump, which means several visits with your health care team or a full day of outpatient training.
- Pump supplies can be expensive.
An insulin pump may not be right for you if:
- You donât want to wear a device that lets people know you have diabetes.
- You donât like the feeling of wearing a device.
- Youâre not comfortable operating the pump.
- You donât want to check your blood sugar at least four times a day.
- Youâre not sure you want to do the work to figure out insulin dosing, carbs, and physical activity.
Types Of Insulin Pumps
There are many different types of insulin pumps available, with 15 devices currently licenced in the UK. Insulin pumps are rapidly evolving and harnessing new technology to ensure more stable blood sugars, fewer hypos and hypers and protection against the long term complications of diabetes.
Insulin pumps are battery-powered, portable devices that deliver insulin into your bloodstream 24 hours a day. Pumps supply basal or background insulin around the clock you can also add insulin boluses to match the carbohydrates in your diet.
When you have diabetes, it can feel like your life is all about controlling your food, insulin and blood sugar. An insulin pump allows you greater flexibility to eat, exercise and live without sticking to a rigid timetable.
You May Like: How Do You Get Type 1 Diabetes
Benefits Of Insulin Pumps
Insulin pumps have many benefits over traditional insulin injection therapy. Research evidence shows that pumps are better at controlling blood sugar and cause fewer complications. People using insulin pumps have fewer episodes of severe hypoglycaemia and less than half the admissions for the serious complication of diabetic ketoacidosis. Insulin pump advantages include:
- Better diabetes control
- The pump is small and discreet â usually smaller than a pack of cards
- Delivers a steady supply of insulin 24 hours a day
- You can add a bolus of insulin at meals quickly and easily
- The insulin is introduced through a cannula, meaning fewer injections
- You only need to change the cannula every 2-3 days
- Pumps simplify your regime because you only need rapid-acting insulin
Adjust Your Basal Dose
To calculate your basal dose for daily injections, find the sum total of your daily basal rate on your pump. For example, your basal rate may be .85 units every hour for the entire day. This would total out to 20.4 units for the entire day. So, your starting long-acting insulin dose should be about 20 units per day in this case. You can then make adjustments to the dose based on your blood sugar readings. You should not make any major or rapid adjustments to your insulin dosages without first consulting your doctor.
You May Like: 30 Carb Meals For Diabetics
What Should I Know About Side Effects Of Diabetes Medicines
Side effects are problems that result from a medicine. Some diabetes medicines can cause hypoglycemia, also called low blood glucose, if you dont balance your medicines with food and activity.
Ask your doctor whether your diabetes medicine can cause hypoglycemia or other side effects, such as upset stomach and weight gain. Take your diabetes medicines as your health care professional has instructed you, to help prevent side effects and diabetes problems.
How An Insulin Pump Works
The device releases insulin almost the way your body naturally would: a steady flow throughout the day and night, called basal insulin, and an extra dose at mealtime, called a bolus, to handle rising blood sugar from the food you eat. You program the pump for both basal and bolus doses. If you eat more than normal, you can program a larger bolus to cover the carbs in your food. A bolus can bring down high blood sugar at other times, too.
The pump is about the size of a smartphone. You attach it to your body using an infusion set: thin plastic tubing and either a needle or a small tapered tube called a cannula you put under the skin. The place where you put it in — your belly, buttock, or sometimes thigh — is called the infusion site. Some pumps come with inserters for easier placement even in hard-to-reach areas.
Insulin pumps use short-acting and rapid-acting insulin, but not long-acting, since the pump is programmed to deliver a small amount continuously to keep your blood sugar levels even.
Recommended Reading: Can You Reverse Diabetic Neuropathy
Whats Not So Great About The Pump
There are downsides to any therapy, and the insulin pump is no exception.
- Wearing it can be unsettlingMost of the time, youll be wearing your pump on your body, clipped to your waistband or in your pocket. Fortunately, many accessories are available to make wearing the pump discreet and convenient.
- CostInsulin pumps cost thousands of dollars. Insurance coverage for insulin pumps varies. Some companies will cover all of the cost, while others may cover only half. Some might also pay for only certain brands. Dont forget to factor in the cost of disposable items, such as cartridge syringes, infusion sets and skin preparation items.
- Higher risk for ketoacidosisThere is a greater risk for ketoacidosis in pump therapy, because long-acting insulin is not used. Because of this, high levels of ketones may develop when there is not enough insulin in the bloodstream. This can happen if there is air in the tubing, a bad infusion set, insertion site infection, or if the insulin pump is disconnected for too long. See also Ketones and pump therapy. As a result, ketoacid levels rise, which can lead to diabetic coma.
- Risk of infusion site infectionInfections can occur if an infusion set is left in for too long. To lessen your chance of infection, change the set as directed by your doctor or pump educator. It is also crucial to wash your hands and the site properly in order to reduce chances of infection. See also Infusion set tips.
Why Choose Pump Or Pen Therapy

Our motto in advising our patients is that the form of insulin delivery should suit you, but increasingly we will advise you to use diabetes technology to achieve your desired goals. We know by now, that the more you use technology, the better your diabetes goals and guidelines can be achieved, such as an HbA1c of 7%. Before starting insulin pump therapy, we, as practitioners, impose some conditions on your knowledge of diabetes control, such as carbohydrate counting, uploading your blood glucose values to us at least every four weeks and, not unimportantly, keeping in touch with your diabetes team.
Also Check: Cheapest Insulin In The World
What Do Insulin Pumps Cost
This can be a tricky question, because when it comes to diabetes technology the cost often varies based on ones insurance coverage.
Generally, you can spend thousands of dollars on the initial purchase because youre buying a new device along with that first set of supplies to use it. The starting cost can be anywhere from $3,000 to $8,000 depending on the device, and monthly supplies can also add up quickly. Most companies do offer payment plans, too.
Keep in mind, this is just the first-time buy and doesnt include the needed pump supplies including infusion sets, tubing, cartridges or reservoirs for insulin, as well as adhesives wipes for site prep. Of course, youd also need to purchase the insulin to fill the pump and any separate CGM supplies that you might use alongside this pump.
Even with insurance, it can cost hundreds of dollars per month to afford an insulin pump.
Most private insurance companies cover insulin pumps under the durable medical equipment portion of the policy. Youll need to work with a doctor to get a prescription and Letter of Medical Necessity confirming your diagnosis and medical need.
The paperwork can be somewhat daunting, so most insulin pump companies offer help in the form of dedicated insurance service teams that work with patients to apply for coverage.
The terms of coverage vary, and your choice of covered device may be limited because some insurance companies have preferred deals with certain pump makers.
Closed Loop Insulin Pump
Closed loop insulin pumps, also commonly referred to as an artificial pancreas , are insulin pumps which are linked up to respond automatically to readings given by a continuous glucose monitor which also needs to be worn by the user through each day.
A comprehensive set of rules and algorithms are required to respond to changes in blood glucose levels and ensure blood glucose levels stay within safe levels and to date these pumps are still in the research stage of development.
It is likely to be a few years, if not more, before closed loop insulin pumps become available to a significant number of people with diabetes in the UK.
You May Like: Why Are Insulin Prices So High
Where Do You Carry Your Pump
A very practical issue is where you leave your pump. Our diabetes nurses often get questions about this. Again, we’re happy to give you some places and options.
With a wireless pump
You can carry the wireless pump in various places. Your abdomen is of course a possibility, but also your upper arms, upper legs or lower back can be good places for you. Make sure that your pump can still be operated properly ????. You can discuss the locations with your diabetes nurse. There are also various straps and bags on the market for the wireless Omnipod. These allow you to “customize” your pump a bit to your liking.
For an insulin pump with a tube
With a clamp
A clamp allows you to clip the pump to the top of your waistband or to your pocket. For women, the center of the bra is often used. Clamps can be ordered from your diabetes device supplier.
With a strap, pocket or belt pouch
Special protective bands can also be ordered for your waist, thigh or arm. The manufacturer of your insulin pump has special accessories for this, which fit well and, if necessary, have anti-slip features.
Again, there are special solutions for women to wear their insulin pump in the bra. For example, with a bra pouch with clamp. With a pump bag, you can give your pump a more conspicuous place by wearing it on your waistband via a clip or strap. Pump bags are available in many styles through your device provider.
The Freestyle Libre Sensor
So, unless youâve been hiding under a rock, youâll know what the FreeStyle Libre Sensor is, and Iâve done a mammoth post on it here. But, itâs not technically a CGM, but the closest thing to it for an affordable price.
It monitors your blood sugar my scanning a sensor placed on your arm and can bring indications of blood sugar rising or dropping. It can help you detect patterns too.
In 2019, the FreeStyle Libre 2 will be released which WILL have the capabilities to bring alarms to notify you of going low and high, making it a CGM.
It will probably be a postcode lottery again in the UK for who gets the new FreeStyle Libre, but if you canât wait until then, there is another solution.
You May Like: How Many Carbs Should A Pre Diabetic Eat Per Day
When Pumps Are Funded By The Nhs
The National Institute for Health and Care Excellence recommends an insulin pump if:
- you’re having frequent hypos or hypers without warning
- your HbA1c is 69mmol/mol or above even though you have tried to manage your blood glucose levels
Your consultant may recommend a pump if this is happening and you can show you’re:
- regularly injecting insulin
- checking your blood glucose at least 4 times a day
- carb counting
What Knowledge And Skills Should I Have
- A thorough understanding of diabetes self-management skills: You should understand insulin action, carbohydrate counting and how to treat high and low blood sugars.
- Manual dexterity: Manual dexterity is necessary to load or fill an insulin cartridge and depress buttons on the pump for technical functions. Severe limitations from hand arthritis or neuropathy may hinder this.
- Vision: People with vision impairment should carefully evaluate which pumps may be the most helpful for them. Pump features such as screen size, screen contrast, size of letters and numbers, audio functions, alerts, alarms, and backlighting should all be assessed.
Also Check: Psoriasis And Diabetes Type 1
Taking A Break From Insulin Pump
If you have been using an insulin pump for some time, you may be getting tired of having it attached to your body. This may warrant a time to take a break from the insulin pump just to keep your sanity.
When taking a break from the insulin pump, there are some things you need to consider first to ensure your safety and health. Here are some tips to help you with taking a break from your insulin pump.