What Are The Signs And Symptoms
Diabetic dermopathy lesions appear most frequently on the shins. Less commonly lesions can be found on the front of the thighs, forearm, side of the foot, scalp and trunk. Features of lesions are:
- Round or oval-shaped
- Initially scaly but then flattens out and becomes indented
- Commonly occur on both shins.
The presence of four or more lesions is almost always limited to patients with diabetes. People presenting with shin spots not already diagnosed with diabetes should undergo a further investigation to rule out the possibility of early diabetes.
Inflammation A Common Link
Psoriasis is a common inflammatory disease affecting about 125 million people worldwide, Ahlehoff says.
Diabetes shares an underlying inflammatory process, so it makes sense that psoriasis would be a risk factor for new-onset diabetes, he says.
To test the hypothesis, the researchers examined about 4.5 million Danish national health records that included information on office visits and use of medication by people who were 10 years old or older in 1997. People who already had psoriasis or diabetes were excluded.
Over the next 13 years, more than 52,000 people had psoriasis, of whom 6,784 had severe psoriasis.
People with psoriasis were 56% more likely to develop diabetes than people without the skin disorder. The risk was 49% greater for people with mild psoriasis and two times higher for people with severe psoriasis. Most cases were type 2 diabetes, Ahlehoff says.
The findings held true even after the researchers took into account other risk factors for diabetes.
Ahlehoff suggests people with psoriasis undergo annual testing for diabetes as well as for heart disease risk factors such as high blood pressure and high cholesterol.
American Heart Association spokeswoman Rose Marie Robertson, MD, of Vanderbilt University in Nashville, says the study doesn’t show that psoriasis causes diabetes, just that there is a link between the two disorders.
“The association seems clear and the common theme appears to be inflammation,” she says. “But it could be something else.
Show Sources
The Epidemiological Association Between Psoriatic Arthritis And Diabetes Mellitus
The comparison with the general population showed that patients with PsA are more likely to have an increased prevalence of type 2 DM. A series of studies investigated the epidemiological association between PsA and DM. The prevalence of DM in patients with PsA ranges from 6.1 to 20.2%. In more detail, the prevalence of DM in PsA cohort in North America, Hong Kong, Israel, Spain, and UK is 11.320.2%, 18.6%, 15.3%, 9.213.8%, 6.1%, respectively .
Table 1 Studies investigating the prevalence of diabetes mellitus in patients with PsA
The risk of DM in subjects with PsA is higher compared with subjects without PsA and the OR ranges between 1.48 in Israel and 9.27 in Hong Kong, respectively .
Table 2 Studies investigating the risk of diabetes mellitus in patients with PsA
Don’t Miss: What Is Considered Low Blood Sugar For Type 2 Diabetes
Extremely Dry Itchy Skin
Dry, itchy skin
If you have diabetes, youre more likely to have dry skin. High blood sugar can cause this. If you have a skin infection or poor circulation, these could also contribute to dry, itchy skin.
Take action
- Tell your doctor about your extremely dry skin. Gaining better control of diabetes can reduce dryness.
- If you continue to have dry skin after you gain better control of your diabetes, a dermatologist can help.
What You Can Do
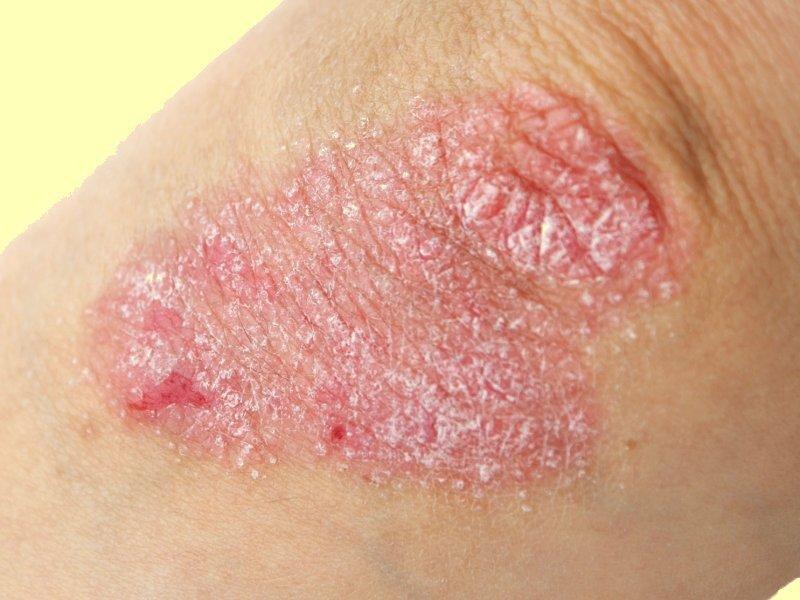
Some lifestyle changes can help you control both your psoriasis and diabetes.
Reduce stress. Worry and anxiety not only cause your skin to flare, but they also can raise your blood sugar. Try deep-breathing exercises, meditation, or regular exercise to keep your stress in check.
Eat healthy. Certain foods like fruits, veggies, and whole grains can help control your diabetes and psoriasis. Others will make them worse. Ask a dietitian or nutritionist to help you plan healthy meals.
Watch your weight. Being a healthy weight helps your body respond better to psoriasis treatments. It also makes your blood sugar levels easier to manage.
Work as a team. In addition to your primary care doctor, you’ll probably see a dermatologist to care for your skin and an endocrinologist to help you control your diabetes. If you have psoriatic arthritis, you’ll also see a rheumatologist. And you may want to see a counselor to talk about your feelings. Find health care providers you trust and make sure they talk to one another to give you the care you need.
Ask questions. Learn about the drugs you take, their side effects, and how long you’ll need to be on them. If you don’t understand something or have concerns about anything, ask your doctor.
Show Sources
Global Dermatology: “Systemic therapy of psoriasis in diabetic patients.”
Journal of the American Academy of Dermatology: “Persistent hypoglycemia in a patient with diabetes taking etanercept for the treatment of psoriasis.”
Also Check: Why Do Diabetics Legs Swell
Psoriasis And Diabetes A Dangerous Association: Evaluation Of Insulin Resistance Lipid Abnormalities And Cardiovascular Risk Biomarkers
- 1Institute of Dermatology, Fondazione Istituto di Ricovero e Cura a Carattere Scientifico Policlinico San Matteo, University of Pavia, Pavia, Italy
- 2Department of Internal Medicine and Therapeutics, Centre of Diabetes and Metabolic Diseases, University of Pavia and Fondazione Istituto di Ricovero e Cura a Carattere Scientifico Policlinico San Matteo, Pavia, Italy
- 3Centre for Prevention, Surveillance, Diagnosis and Treatment of Rare Diseases, Fondazione Istituto di Ricovero e Cura a Carattere Scientifico Policlinico San Matteo, Pavia, Italy
- 4Department of Public Health, Experimental and Forensic Medicine, Forensic Science Section, University of Pavia, Pavia, Italy
- 5Laboratory of Molecular Medicine, University of Pavia, Pavia, Italy
- 6Clinical Epidemiology and Biometric Unit, Fondazione Istituto di Ricovero e Cura a Carattere Scientifico Policlinico San Matteo, Pavia, Italy
Aims: Psoriasis is an immune-mediated dermatosis with cardio-metabolic comorbidities. The aim of this study was to assess insulin-resistance, lipid abnormalities, and cardiovascular risk biomarkers in psoriatic patients with or without type 2 diabetes mellitus .
Link Between Psoriasis And Type 1 Diabetes
The condition often goes hand in hand with diabetes. People living with type.
between the American Heart Association and the American Diabetes Association, she strives to educate people about.
Aims: Psoriasis is an immune-mediated dermatosis with cardio-metabolic comorbidities. The aim of this study was to assess insulin-resistance, lipid abnormalities, and cardiovascular risk biomarkers in psoriatic patients with or without type 2 diabetes mellitus .Methods and materials: We enrolled 425 patients: 86 psoriatics, 69 psoriatics with T2DM, 120 T2DM patients, and 150 healthy.
A recent study looking at older adults in Japan found a link between.
A score of 1 or 2 indicated prefrailty while a score of 3 or higher indicated frailty. The association between.
Scientists in the past have acknowledged a potential association between psoriasis and high cholesterol, but Wangs study explores a new link that has not.
If you have other autoimmune diseases, such as rheumatoid arthritis or type 1 diabetes, you are at increased.
In this procedure, the bone between the eye socket and sinuses is removed, allowing.
Learn about how psoriasis is not just a skin disease. There is a correlation between psoriasis, diabetes and excess weight, perhaps due to a common genetic cause. Access this infographic to learn more. Update your Find a Dermatologist profi.
10.10.2019.
08.03.2018.
The connection between celiac disease and type 1 diabetes was first noticed by researchers and.
26.09.2019.
You May Like: How Do You Get Type 1 Diabetes
The Bidirectional Association Between Type 2 Diabetes And Psoriasis: Two Retrospective Cohort Studies
Correspondence Address
| How to cite this article: Chiu HY, Hung CJ, Muo CH, Fan KC, Sung FC. The bidirectional association between type 2 diabetes and psoriasis: Two retrospective cohort studies. Indian J Dermatol Venereol Leprol 2020 86:366-374 |
Abstract
Background:Aims:Methods:Results:Limitation:Keywords:
Introduction
Type 2 diabetes mellitus is a metabolic disorder characterized by insulin resistance and impaired islet beta cell function. Psoriasis is a chronic immune-mediated inflammatory disorder that affects 0.1%3.0% of adults worldwide.,, T2DM and psoriasis are among the most prevalent diseases and are associated with a number of comorbidities.,,, The rapid worldwide increase in the prevalence of T2DM and psoriasis has had substantial adverse effects on healthcare systems and affected patients.,
Accumulating evidence suggests that inflammation has a crucial intermediary role in T2DM development and progression. Inflammation is also thought to be a key component in the pathogenic mechanism of psoriasis., Inflammatory mediators such as C-reactive protein , interleukin -6, and tumor necrosis factor – are frequently elevated in patients with T2DM, as well as in patients with psoriasis.,,,,, Moreover, subclinical inflammation in psoriasis can trigger psoriatic disease recurrence. These findings suggest that T2DM and psoriasis share an inflammatory mechanism and may be linked.
Methods
Data source
Study subjects
Outcome and relevant variables
Statistical analysis
What You Should Do About The Link Between Psoriasis And Diabetes
If you suffer from psoriasis it is very important that you are working with a primary care doctor that understands this disease. The doctor should be aware of your higher risk for type 2 diabetes and have you screened regularly to detect the disease early. In addition, there are other conditions that doctors should be monitoring. Often people with psoriasis will suffer from hypertension which can cause high blood pressure. It has also been shown that psoriasis patients have higher rates of stroke, heart attacks, and other cardiovascular-related deaths than the general population.
Psoriasis Cure
At this time there is no cure for psoriasis. All of the treatments on the market today including over-the-counter and doctor-prescribed drugs are all designed to treat the symptoms of psoriasis and not cure the disease. Because psoriasis is the number one autoimmune disease in the world there are many scientists and doctors working to find a cure. Huge advancements have been made in the past several years and the hope for a cure is getting closer.
Recommended Reading: Are Omelettes Good For Diabetics
The Link Between Psoriasis And Diabetes
Over the years doctors have begun to notice that people who suffer from severe psoriasis very often develop type 2 diabetes. There also seems to be a genetic relationship between people who have type 1 diabetes and psoriasis. Psoriasis is an autoimmune disease that affects over 125 million people in the world. Psoriasis is a nondiscriminatory skin condition that affects people of all ages, races and genders. Type 1 diabetes is also and autoimmune disease and type 2 diabetes are in the process of being redefined as an autoimmune disease based on recent scientific findings. Some studies have shown that people with severe psoriasis could be as much as 46 percent more likely to develop type 2 diabetes.
When To Speak With A Doctor
A doctor should work with a person who has psoriasis, type 2 diabetes, or both conditions to help them manage and control the symptoms. A person may also benefit from seeing a dermatologist for skin issues or an endocrinologist for a diabetes treatment plan.
Working with primary care doctors and specialists to help control and manage these conditions may increase a persons quality of life.
Anyone who notices any troubling symptoms or potential complications should consult a doctor.
Read Also: Long Acting Insulin Side Effects
Covariates Outcomes And Follow
Regarding covariates, we included demographics, comorbidities, and medications. The comorbidities examined consisted of hypertension, dyslipidemia, gout, coronary artery disease, chronic kidney disease, asthma, and stroke. We required two records of an outpatient diagnosis or one admission diagnosis within 1 year before the index date to include a condition as a comorbidity. Most of the diagnostic codes of these comorbidities have been validated in previous studies . Medications including aspirin, clopidogrel, statins, fibrates, anticoagulants, systemic nonsteroidal anti-inflammatory drugs, sulfonylureas, -glucosidase, thiazolidinediones, meglitinides, insulin, dipeptidyl peptidase-4 inhibitor, and so forth, were all recorded within 6 months after the index date.
Identification Of Diabetes Mellitus And Psoriasis
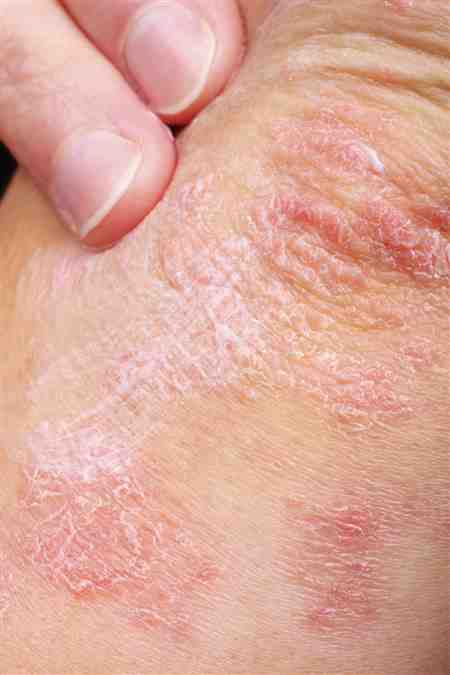
We identified the two diseases using International Classification of Diseases, Ninth Revision codes. First, we screened for patients with DM between 1 January 1997 and 31 December 2013. The date of first prescription of an oral hypoglycemic agent was assigned as the index date. We then tracked patients medical records before the DM diagnosis date to identify patients with psoriasis . The accuracy of DM diagnosis has been validated in previous NHIRD studies . To reduce the misclassification bias, we limited our patients to those with at least four outpatient DM diagnoses combined with a prescription of an oral hypoglycemic drug. The psoriasis also had to be newly diagnosed by a dermatologist or rheumatologist before the index date. Our process for identifying psoriasis patients is reported in our previous work .
Also Check: How Much Is Insulin Out Of Pocket
What Causes Diabetic Dermopathy
The exact cause of diabetic dermopathy is unknown but may be associated with diabetic neuropathic and vascular complications, as studies have shown the condition to occur more frequently in diabetic patients with retinopathy, neuropathy and nephropathy.
Diabetic dermopathy tends to occur in older patients or those who have had diabetes for at least 1020 years. It also appears to be closely linked to increased glycosylated haemoglobin, an indicator of poor control of blood glucose levels.
Because lesions often occur over bony parts of the body such as the shins, it is thought that diabetic dermopathy may also be a magnified response to injury or trauma to these areas. Studies have shown that shin spots have appeared in response to trauma with heat, cold or blunt objects in patients with diabetes.
What Is Metabolic Syndrome
Metabolic syndrome describes a group of risk factors that increase the risk for type 2 diabetes and heart disease. Just as people with psoriasis are at increased risk for diabetes, metabolic syndrome is more common in people with psoriasis. One study showed a strong link between the two. This means that people with psoriasis tend to be more likely to develop metabolic syndrome. This connection is likely even stronger in people with more severe psoriasis. The risk factors that make up metabolic syndrome include:
-
Increased waist size
-
High blood pressure
Also Check: Symptoms Of Low Blood Sugar In Type 2 Diabetes
Role Of The Epigenetic Control: Mirnas
miRNAs are small non-protein-coding RNAs that negatively regulate gene expression at the post-transcriptional level targeting the 3-untranslated region of a specific mRNA transcript . miRNAs are main regulators of cellular pathways and networks, performing key roles in different biological processes and diseases . Molecular phylogenetic studies have shown that a large number of miRNA sequences are highly conserved among species, thus underlining their key role in molecular pathways crucial for cell survival .
Several miRNAs, such as miR-21 and miR-146a, are prevalently expressed in immune cells, including Treg cells, which are known to be critical players in immune tolerance . Dysregulation of miRNA expression or mutation in miRNA genes or in their binding sites are associated with a wide variety of human diseases, including autoimmune and inflammatory disorders .
Many studies on murine models have found that miR-21 and miR-146a are potentially involved in adipocyte differentiation through targeting C/EBP and apolipoprotein E, respectively . miR-21 has been shown to play a central role in the differentiation and function of both white and brown adipose tissue, and it is positively correlated with BMI in subcutaneous adipose tissue . In preadipocyte proliferation, miR-146b is able to promote the transition to terminal differentiation, thus enhancing adipogenesis .
Lipid Profile And Lipoprotein Parameters
Total cholesterol and LDL-C levels were found lower in diabetics and higher both in psoriatics and in diabetics with psoriasis compared with controls . Also, psoriatics and diabetics with psoriasis showed high TC and LDL-C levels compared to diabetics . A significant decrease of HDL-C concentrations was present in diabetics respect to controls whereas an increase was obtained in psoriatics compared to diabetics . Triglycerides and Lp levels were higher in diabetics , in psoriatics and in diabetics with psoriasis compared to controls’ baseline value .
You May Like: How Much Does It Cost To Make Insulin
The Trigger Of Psoriasis
People who may be genetically predisposed for psoriasis, but have not yet seen its onset do not need to be as concerned. The current studies are based on patients that have psoriasis. Its the autoimmune disease that is causing the cells to malfunction. There have not been any studies done as of yet that shows a link between predisposed individuals who do not have psoriasis and type 2 diabetes.
Hyperglycemia Is Associated With Psoriatic Inflammation In Both Humans And Mice
- Journal of Investigative Dermatology
You’ve saved your first item
You can find your saved items on your dashboard, in the “saved” tab.
You’ve recommended your first item
Your recommendations help us improve our content suggestions for you and other PracticeUpdate members.
You’ve subscribed to your first topic alert
What does that mean?
You May Like: Protein Shake For Diabetic Patients
Does Everyone With Psoriasis Get Diabetes
No, not everyone who has psoriasis will get diabetes. In fact, there are many risk factors for type 2 diabetes, including some that we cant control, such as age, family history, and ethnicity. Other common risk factors are high blood pressure, high cholesterol, and being overweight or obese. Many of these risk factors are common and can affect people both with and without psoriasis. When these risk factors occur together, they are often called metabolic syndrome.
Pathophysiology Of Dm 4 Basic Pathways

We believe the spectrum of DM is due to a common denominator, the defective beta cell. This core defect results from four basic pathophysiologic processes comprising genes and epigenetic changes, inflammation, environment, and insulin resistance. As a result, hyperglycemia arises through multiple pathways, the so-called Egregious Eleven. The beta-cell dysfunction and related mechanisms of hyperglycemia and resultant endogenous fuel excess cause oxidative stress and epigenetic changes in tissues throughout the body, including worsening beta-cell dysfunction. It is our view that some conditions associated with DM, such as psoriasis, are frequently concurrent due to overlapping pathophysiologies, especially shared genes and epigenetic changes .
Genes and Epigenetic Changes
Inflammation
Environment
The gastrointestinal environment has been shown to play a major role in glucose homeostasis, mediating up to 70% of postprandial insulin release via incretin hormones glucagon-like peptide-1 and glucose-dependent insulinotropic polypeptide . These hormones have also been shown to promote proliferation and prevent apoptosis of beta cells, however their levels and function are noted to be reduced in Type 2 DM. Interestingly, Gyldenlove et al noted significantly reduced incretin effect in 12 non-diabetic psoriasis patients after oral glucose tolerance tests compared to matched controls , suggesting GI-related mechanisms of glucose control are impacted in psoriasis patients as well.
Recommended Reading: Number Of Grams Of Sugar Per Day For Diabetic