What Is Bolus Insulin
A bolus dose is insulin that is specifically taken at meal times to keep blood glucose levels under control following a meal. Bolus insulin needs to act quickly and so short acting insulin or rapid acting insulin will be used.
Bolus insulin is often taken before meals but some people may be advised to take their insulin during or just after a meal if hypoglycemia needs to be prevented.
Your doctor will be able to advise you if you have any questions as to when your bolus insulin should be taken.
When To Take Tresiba If You Miss A Dose
Since Tresiba is a once-daily insulin, its quite easy to forget it.
Its fine if an adult misses the dose because, again, its extremely flexible.
Simply take your missed dose as soon as you remember, as long as its 8 hours apart between doses. So, your next dose should be greater than 8 hours after the late dose.
Try to then revert back to your regular schedule for taking Tresiba if you follow one.
Again, taking the missed dose is applicable only for adults and not for children.
If you feel any uncomfortable symptoms or side effects as a result of the missed dose, consult with your doctor.
Refrain from doubling your Tresiba dose if/when you miss one. As the brand emphasizes, they should be taken at least 8 hours apart despite its dosing flexibility.
Lets discuss what happens if you take too much Tresiba.
Example #: Formulas Commonly Used To Create Insulin Dose Recommendations
This example illustrates a method for calculating of your background/basal and bolus doses and estimated daily insulin dose when you need full insulin replacement. Bear in mind, this may be too much insulin if you are newly diagnosed or still making a lot of insulin on your own. And it may be too little if you are very resistant to the action of insulin. Talk to your provider about the best insulin dose for you as this is a general formula and may not meet your individual needs.
The initial calculation of the basal/background and bolus doses requires estimating your total daily insulin dose:
Read Also: Type 1 2 3 Diabetes
Types Of Basal Insulin
All types of basal insulin are long-acting.
A doctor might prescribe this type of insulin for types 1 and 2 diabetes. It generally acts in the body for up to 24 hours, although some varieties can last longer than this.
Depending on the type of insulin used and patient needs, a person should inject long-acting basal insulin either once or twice daily.
Long-acting insulin tends to have no peak activity and mimics the natural function of the pancreas. It allows for consistent delivery, keeping blood sugar levels steady throughout the day and night.
There are three different long-acting insulins.
Forgetting Blood Sugar Checks
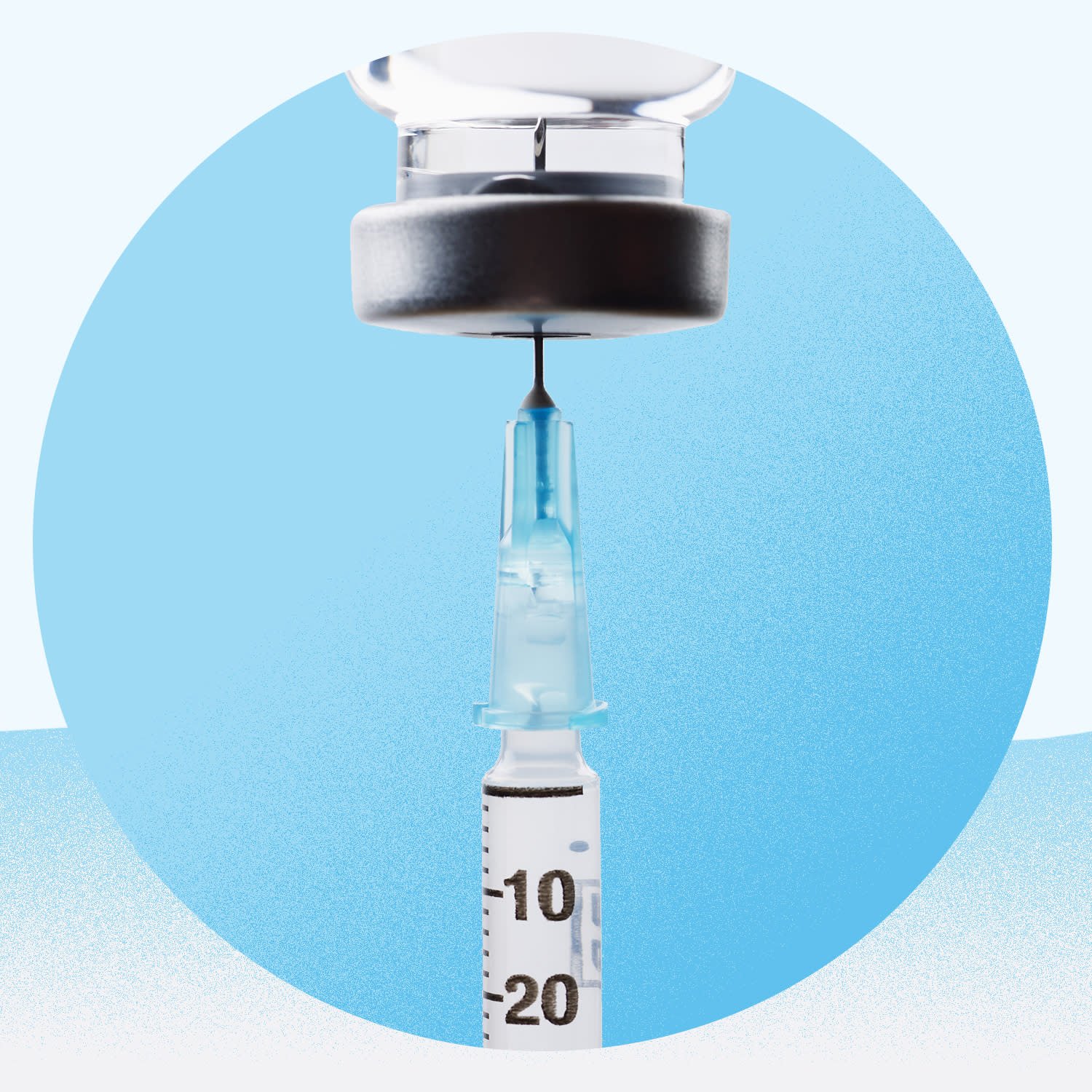
Checking your blood sugar levels regularly helps you stay tuned in to how your body responds to your medications, food, and lifestyle habits, Dr. Port says. It can help you and your doctor determine the right amount of basal and bolus insulin to take. Fasting blood sugar levels reflect how basal insulin is working in the background, whereas pre-meal and evening blood sugar levels are a better barometer of how the bolus insulin dosing is matching up with your food and carbohydrate intake. âMany people stop checking their blood sugar because they dont feel badly,â Port says. Or, despite having symptoms of high or low blood sugar, they simply ignore the fact that their diabetes may be out of control, she adds.
Smart strategies to stay on top of your blood sugar testing routine include choosing a glucose meter that works for your lifestyle, keeping the meter where its easy to get to and use, and finding ways to remind yourself to do the checks. It can be a note on your refrigerator, an alarm on your phone, or some other device that prompts you to use it whatever works for you. You might also be eligible to use a continuous glucose monitor, a special device placed just under the skin that tracks blood sugar readings continuously and sends this information to a reader or to a phone app. Most devices require minimal or no calibration with finger stick blood glucose readings and can typically be worn for up to 7 to 14 days, depending on the brand.
Don’t Miss: Diabetes Feet Tingling At Night
When To Consider Using Basal
If you have type 1 diabetes, you will require a combination therapy called basal-bolus insulin. This therapy includes an injection of rapid or fast-acting insulin before meals, as well as a daily injection of background basal insulin. Because your body doesnt make insulin, its key to work with your doctor to come up with an effective treatment approach.
Why Is Metformin Taken After Food
Metformin may show some side effects in the first few weeks of medication. Doctors recommend taking it after a meal as it proves to be beneficial in reducing the symptoms of bowelâs side effects.
Dr. SM Kamal Hasan, MBBS, Rangpur Medical College and HospitalRangpur- Dinajpur Highway, Cantt, Near Central Jail, Rangpur 5400, Bangladesh
Also Check: How Much Does Metformin Lower Blood Glucose
Read Also: What Foods To Eat For Insulin Resistance
Example #: Carbohydrate Coverage At A Meal
First, you have to calculate the carbohydrate coverage insulin dose using this formula:
CHO insulin dose = Total grams of CHO in the meal ÷ grams of CHO disposed by 1 unit of insulin .
For Example #1, assume:
- You are going to eat 60 grams of carbohydrate for lunch
- Your Insulin: CHO ratio is 1:10
To get the CHO insulin dose, plug the numbers into the formula:
CHO insulin dose =
- The carbohydrate coverage dose is 6 units of rapid acting insulin.
- The high blood sugar correction dose is 2 units of rapid acting insulin.
Now, add the two doses together to calculate your total meal dose.
Carbohydrate coverage dose + high sugar correction dose = 8 units total meal dose!
The total lunch insulin dose is 8 units of rapid acting insulin.
The Takeaway: The Right Dose And Type Of Insulin For A Healthy Life
Insulin is instrumental in energizing your body. If your body doesnt make insulin or use insulin properly because of type 1 or type 2 diabetes, basal injections can help stabilize your blood sugar and reduce the likelihood of diabetes complications like kidney damage, eye damage, nerve damage, and heart problems.
Make sure you follow your doctor’s instructions and take your insulin as prescribed. If you feel your insulin isnt working effectively, speak to your doctor about fine-tuning your dosage.
Don’t Miss: Diabetes How To Control Blood Sugar
Analogue Versus Human Insulin
Glucose control, adverse effects, cost, adherence, and quality of life need to be considered when choosing a type of insulin. In general, analogue insulin is similar to human insulin in controlling diabetes, although some trials have found higher mean A1C levels in patients taking analogue insulin compared with human insulin. 17 Analogue insulin usually causes less postprandial hyperglycemia and delayed hypoglycemia. 18,19 In a recent meta-analysis, glycemic control was not improved with analogue insulin compared with human insulin, but nocturnal hypoglycemia was reduced.17
An industry-funded cost-effectiveness analysis found that the increased cost of medication is more than off set by the reduction in hypoglycemic events. 20 However, the analysis assumed a cost differential of 14 percent, which is inconsistent with current pricing . 20,21 Cost-effectiveness analyses have differed regarding the long-term cost savings of using analogue insulin in patients with type 2 diabetes, with industry-sponsored studies finding reduced cost22 and government-sponsored studies finding no cost reduction. 23 Measures of adherence and quality of life have been improved with analogue insulin compared with human insulin. 24,25
Tip #: Have A Sleep Routine
The goal of basal insulin is to maintain a steady blood sugar level during fasting periods. Ideally, basal insulin should produce at most a 30 milligrams per deciliter change when blood sugar levels are stable and in your target range during sleep times. Thats why your healthcare provider will most likely advise you to inject basal insulin at night, preferably before bedtime.
Its recommended that people administer the injection at a regular time. Keeping consistent sleeping hours will help you and your doctor monitor how the insulin works in your body while youre sleeping and throughout the day. This is necessary so that you can predict the window of time when the insulin is working.
Long-acting insulin is available in liquid form, and the only way to get it inside your body is by injecting it. There are two ways of injecting insulin into your body: by syringe and by pen.
Read Also: Is Equal Good For Diabetics
The High Blood Sugar Correction Factor:
Correction Factor = 1800 ÷Total Daily Insulin Dose = 1 unit of insulin will reduce the blood sugar so many mg/dl
This can be calculated using the Rule of 1800.
Example:
= 1800 ÷ TDI = 1 unit insulin will drop reduce the blood sugar level by 45 mg/dl
While the calculation is 1 unit will drop the blood sugar 45 mg/dl, to make it easier most people will round up or round down the number so the suggested correction factor may be 1 unit of rapid acting insulin will drop the blood sugar 40-50 mg/dl.
Please keep in mind, the estimated insulin regimen is an initial best guess and the dose may need to be modified to keep your blood sugar on target.
Also, there are many variations of insulin therapy. You will need to work out your specific insulin requirements and dose regimen with your medical provider and diabetes team.
Insulin Management Of Type 2 Diabetes Mellitus
ALLISON PETZNICK, DO, Northern Ohio Medical Specialists, Sandusky, Ohio
Am Fam Physician. 2011 Jul 15 84:183-190.
Insulin therapy is recommended for patients with type 2 diabetes mellitus and an initial A1C level greater than 9 percent, or if diabetes is uncontrolled despite optimal oral glycemic therapy. Insulin therapy may be initiated as augmentation, starting at 0.3 unit per kg, or as replacement, starting at 0.6 to 1.0 unit per kg. When using replacement therapy, 50 percent of the total daily insulin dose is given as basal, and 50 percent as bolus, divided up before breakfast, lunch, and dinner. Augmentation therapy can include basal or bolus insulin. Replacement therapy includes basal-bolus insulin and correction or premixed insulin. Glucose control, adverse effects, cost, adherence, and quality of life need to be considered when choosing therapy. Metformin should be continued if possible because it is proven to reduce all-cause mortality and cardiovascular events in overweight patients with diabetes. In a study comparing premixed, bolus, and basal insulin, hypoglycemia was more common with premixed and bolus insulin, and weight gain was more common with bolus insulin. Titration of insulin over time is critical to improving glycemic control and preventing diabetes-related complications.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Analogue insulin is as effective as human insulin but is associated with less postprandial hyperglycemia and delayed hypoglycemia.
Also Check: Type 2 Diabetes Occurs When
General Insulin Needs To Help Decide When To Take Tresiba
Each persons basal insulin requirement is unique.
But in general, basal insulin needs are at their peak during the early morning hours and lower in the middle of the day.
However, ones basal insulin needs will depend upon which stage of life they are in. This is because of all the different hormones that are present at different life stages.
Therefore, a persons growth over the years has a huge impact on the best time to take Tresiba, or when you should take any long-acting insulin.
Below is a short breakdown of basal insulin needs based on age:
Total Daily Insulin Requirement:
= 500 ÷ TDI = 1unit insulin/ 12 g CHO
This example above assumes that you have a constant response to insulin throughout the day. In reality, individual insulin sensitivity varies. Someone who is resistant in the morning, but sensitive at mid-day, will need to adjust the insulin-to-carbohydrate ratio at different meal times. In such a case, the background insulin dose would still be approximately 20 units however, the breakfast insulin-to-carbohydrate ratio might be breakfast 1:8 grams, lunch 1:15 grams and dinner 1:12 grams.
The insulin to carbohydrate ratio may vary during the day.
Also Check: Diabetes Kidney Failure Life Expectancy
Other Basal Insulin Developments
Therapeutic inertia is pronounced for starting insulin therapy in type 2 diabetes and is commonly attributed to fear of injections and fear of hypoglycemia. An alternative route of administration of insulin, for example via oral administration in the form of an insulin tablet, would be obviously beneficial and more convenient for patients. Furthermore, oral insulin administration results in a more physiological insulin delivery , because the absorption via the portal vein mimics more closely pancreatic insulin secretion. In a recent article in The Lancet that we published together with authors from Novo Nordisk, we investigated the efficacy and safety of an oral basal insulin versus injection of the long-acting insulin glargine. The main outcome of the trial was that the oral basal insulin could control fasting glucose levels in a safe manner to the same extent as the commercially available and widely used insulin glargine after 8 weeks of treatment. This is a great achievement and created a lot of enthusiasm for the future development of oral insulin. Nevertheless, the development of this particular oral basal insulin was stopped due to relatively low absorption and subsequent need for administration of high insulin amounts to achieve a metabolic effect. Better technologies to increase the absorption of insulin in the gastro-intestinal tract are therefore needed and being explored .
What Are The Drawbacks To Insulin Treatment For Diabetes
The biggest issue with insulin right now is unaffordability. A box of rapid-acting insulin can cost $400 without insurance. As so many people continue to lose their health coverage, its becoming an enormous problem, Dr. Zilbermint says.
Consistently rising costs have led some patients to ration their insulin, which can be dangerous and even deadly. The cost of testing strips is also an issue, and both have led to a black market in testing strips and insulin. Its illegal, says Dr. Zilbermint, but its happening.
Also Check: Are Omelettes Good For Diabetics
Development In Insulin Injections
Ultra-long acting insulins, such as insulin glargine U300 , are more concentrated than regular strength insulin. Most insulin contains 100 units per milliliter , whereas U300 insulin has 300 units per milliliter. This means people requiring large amounts of insulin can take a lower volume of insulin without lowering the actual units of insulin taken.
Insulin degludec is a newer type of basal insulin, but it lasts longer than traditional basal insulins such as Lantus and Levemir. Longer-acting insulins may help reduce hypoglycemia risk.
Those wanting insulin that doesnt require an injection is in luck! The FDA approved an inhaled version of rapid-acting insulin called Afrezza in 2014. Its inhaled, similar to how asthma sufferers use an inhaler to deliver their asthma medication.
Rules Of Engagement For Basal Insulin Adjustment
It seems like there are rules for everything these days. Rules for dating. Rules for e-mail etiquette. Even rules for raising kids. And so, it only seems fair that I get to create some rules of my own.
Since nothing drives me battier than people who make ill-conceived changes to the basal settings on their insulin pumps, I think Ill take this opportunity to offer some experience-laden insight on the subject.
Before getting down to rule-writing, it should be understood that the role of basal insulin is to match the livers normal output of glucose, thus keeping blood glucose levels steady between meals and during sleep. The only true way to determine whether the existing basal settings are working properly is to perform fasting tests at each phase of the day and night. During a basal test, the only thing raising blood glucose should be the liver, and the only thing lowering it should be basal insulin. All other influences need to be eliminated.
Read Also: Sure Comfort Insulin Syringes 30 Gauge
How Do I Use An Insulin Pen
Select a clean, dry work area. The supplies you will need include:
- The prescribed insulin pen
- Pen needles and alcohol wipes
- A container for used equipment. You can use a hard plastic container with a screw-on or tight lid, or a commercial sharps container.
Here are the steps you will take: