Normotensive With Microalbuminuria Or Hypertensive Without Microalbuminuria
Studies have shown that ACE inhibitors and ARBs are beneficial in reducing the progression of microalbuminuria in normotensive patients with type 1 diabetes17 and in normotensive patients with type 2 diabetes.3,18
Patients with hypertension and diabetes clearly benefit from lowering of blood pressure, regardless of the presence of nephropathy. A number of studies suggest that a variety of agents may be appropriate first-line treatments for blood pressure. Because ACE inhibitors and ARBs have been shown to decrease or slow the progression of complications in diabetes, it seems reasonable to use a medication from one of these two classes of antihypertensive drugs as a first-line agent in hypertensive patients who have diabetes without microalbuminuria.8,14,19
Urine Samples And Microalbuminuria
A urine sample is taken and checked for signs of protein in your urine.
One of those proteins is albumin, which is made in the liver and normally found in your blood plasma. When albumin appears in the urine it is called microalbuminuria .
Microalbuminuria is also considered a risk marker for cardiovascular disease along with early kidney disease. Often, your doctor will order a microalbuminuria test if they believe you might be at risk for kidney damage or disease.
Definitive Treatment Of Diabetic Nephropathy
As with most complications of diabetes, there is no definitive âcureâ for diabetic nephropathy. However, a recent study4 followed nearly 400 patients with type 1 diabetes and micro-albuminuria for six years, and more than one half of the patients in the study experienced regression of microalbuminuria. This suggests that not all patients with microalbuminuria progress to diabetic nephropathy. Patients with low systolic blood pressure, low levels of cholesterol, and low levels of glycosylated hemoglobin were more likely to experience regression.
Don’t Miss: Grams Of Sugar Per Day For Diabetic
What Causes Chronic Kidney Disease
The two main causes of chronic kidney disease are diabetes and high blood pressure, which are responsible for up to two-thirds of the cases. Diabetes happens when your blood sugar is too high, causing damage to many organs in your body, including the kidneys and heart, as well as blood vessels, nerves and eyes. High blood pressure, or hypertension, occurs when the pressure of your blood against the walls of your blood vessels increases. If uncontrolled, or poorly controlled, high blood pressure can be a leading cause of heart attacks, strokes and chronic kidney disease. Also, chronic kidney disease can cause high blood pressure.
Other conditions that affect the kidneys are:
- Glomerulonephritis, a group of diseases that cause inflammation and damage to the kidneys filtering units. These disorders are the third most common type of kidney disease.
- Inherited diseases, such as polycystic kidney disease, which causes large cysts to form in the kidneys and damage the surrounding tissue.
- Malformations that occur as a baby develops in its mothers womb. For example, a narrowing may occur that prevents normal outflow of urine and causes urine to flow back up to the kidney. This causes infections and may damage the kidneys.
- Lupus and other diseases that affect the bodys immune system.
- Obstructions caused by problems like kidney stones, tumors or an enlarged prostate gland in men.
- Repeated urinary infections.
Other problems that can cause kidney failure include 15):
Treatment For Patients With Microalbuminuria
Lifestyle measures and drug therapies are used to slow the progression of renal disease in patients with diabetes. Tight control of BP and blood glucose can slow the progression of microvascular disease . Numerous studies have examined the impact of antihypertensive agents on the progression of CKD in patients with diabetes. Drugs that act on the renin-angiotensin-aldosterone system are effective antihypertensive agents that have been shown to slow progression of kidney disease, and their use is recommended in treatment guidelines for patients with diabetes at risk for CKD., These and other agents have been evaluated in patients with microalbuminuria or at risk for microalbuminuria . The various clinical trials provide a wide spectrum of results as to the protective effects of RAAS agents relative to other drugs or placebo. In considering the results of the various clinical studies, it is important to consider where patients were on the continuum that encompasses normoalbuminuria through macroalbuminuria when the intervention was introduced . It is also necessary to consider baseline BP and CVD risk, as well as the details of the treatment regimens employed and the extent of BP lowering achieved with antihypertensive treatment.
| Study |
|---|
Also Check: Islet Cell Transplant For Type 1 Diabetes
Comparison Of General Clinical Data Between Groups A And Groups B
The average age of patients in group A was 43.13±11.34, while that of patients in group B was 44.13±12.39, and there was no significant difference between the two groups . In addition, there was no significant difference in diabetes duration, smoking history, drinking history, systolic blood pressure, diastolic blood pressure, fasting insulin level, TC, LDL, creatinine, glomerular filtration rate and glycosylated hemoglobin level between the two groups . The levels of BMI, WHR, TG, SUA, MAU, FBG, HOMA-IR and AIP in group A were higher than those in group B, and the differences were statistically significant . HDL-C level was lower than that of group B, and the difference was statistically significant . The results are shown in Table 1.
|
Table 1 The General Data of Group A and Group B Patients |
Can Microalbuminuria Be Reversed
Yes and it depends of the cause, because kidney disease does not happen overnight. If kidney disease is found and treated early, you can help slow or even stop it from getting worse.
Kidney disease happens slowly over many years, and in stages. There are five stages of kidney disease. In each stage, the kidneys dont work as well as the stage before. With treatment and lifestyle changes, you can help slow or stop your kidney disease from getting worse.
Each stage of chronic kidney disease is related to the level of kidney function and kidney damage.
- Stage 1 a normal eGFR greater than or equal to 90 ml per minute per 1.73 m2, and albuminuria, hematuria, a pathological abnormality or a structural abnormality.
- Stage 2 a slightly decreased eGFR between 60 and 89 ml per minute per 1.73 m2, and albuminuria, hematuria, a pathological abnormality or a structural abnormality.
Note: If your kidney function is at stage 1 or 2, you only have chronic kidney disease if you have albuminuria, hematuria, a pathological abnormality or a structural abnormality.
- Stage 3a a mild to moderate decrease in eGFR between 45 and 59 ml per minute per 1.73 m2.
- Stage 3b a moderate to severe decrease in eGFR between 30 and 44 ml per minute per 1.73 m2.
- Stage 4 a severe decrease in eGFR between 15 and 29 ml per minute per 1.73 m2.
- Stage 5 end stage kidney disease, as eGFR decreases to less than 15 ml per minute per 1.73 m2 or dialysis is started.
You May Like: My Husband Has Diabetes Erectile Dysfunction
Treatment Of Albuminuria And Cardiovascular Outcomes
In the PREVEND Intervention Trial , patients with albuminuria treated with fosinopril experienced a significant decrease in urinary albumin excretion and a trend toward a decrease in cardiovascular events . In the LIFE study, patients with a urinary ACR greater than the median value at baseline , but who were able to decrease their ACR to less than the median value at 1 year , had a reduced risk for cardiovascular mortality, stroke, and myocardial infarction compared with patients who were not able to decrease their ACR . This suggests that there may be a cardiovascular benefit to reducing albuminuria in patients with essential hypertension but also in type 2 diabetes. Future trials are needed in patients with type 2 diabetes to explore the relationship between reduction in albuminuria and improvement in cardiovascular events.
What Is Potassium And Why Is It Important To You
Potassium is a mineral found in many of the foods you eat. It plays a role in keeping your heartbeat regular and your muscles working right. It is the job of healthy kidneys to keep the right amount of potassium in your body. However, when your kidneys are not healthy, you often need to limit certain foods that can increase the potassium in your blood to a dangerous level. You may feel some weakness, numbness and tingling if your potassium is at a high level. If your potassium becomes too high, it can cause an irregular heartbeat or a heart attack.
A normal amount of potassium in a typical diet of a healthy American is about 3500 to 4500 milligrams per day. A potassium restricted diet is typically about 2000 milligrams per day. Your physician or dietitian will advise you as to the specific level of restriction you need based on your individual health. A kidney dietitian is trained to help you make modifications to you diet in order to prevent complications for kidney disease.
What foods are high in potassium ?
The following table lists foods that are high in potassium. The portion size is ½ cup unless otherwise stated. Please be sure to check portion sizes. While all the foods on this list are high in potassium, some are higher than others.
Table 1. High-Potassium Foods
What is a safe level of potassium in my blood?
Ask your doctor or dietitian about your monthly blood potassium level and enter it here:
How can I keep my potassium level from getting too high?
Read Also: Nature Made Diabetes Health Pack Side Effects
Abnormal Levels Of Urine Albumin
Technically, microalbuminuria is defined as urinary excretion of albumin between 30 and 300 milligrams of albumin per day. You also might see it defined as between 20 and 200 micrograms per minute.
Values less than that are not technically microalbuminuria. Values higher than that would be called simply albuminuria or sometimes macroalbuminuria or proteinuria.
Effect Of Pentoxifylline On Microalbuminuria In Diabetic Patients: A Randomized Controlled Trial
1Isfahan Kidney Disease Research Center, Isfahan University of Medical Sciences, Isfahan, Iran
2Isfahan Endocrine and Metabolism Research Center, Isfahan University of Medical Sciences, Isfahan, Iran
3Department of Epidemiology, School of Health and Nutrition, Shiraz University of Medical Sciences, Shiraz, Iran
Abstract
1. Introduction
Diabetes is among the most common and major diseases in the world and recently in most countries the number of patients with diabetes has strikingly increased. Diabetic nephropathy is enlisted as one of the chronic microvascular complications of diabetes which is associated with considerable morbidity and mortality and is a main cause for approximately 50% of all end stage renal disease, and this results in increasing renal replacement therapy and healthcare costs . Though many pathophysiologic processes are involved in the pathogenesis of diabetic nephropathy, the fundamental mechanisms of it are not fully established . Diabetic nephropathy is characterized by proteinuria, hypertension, and advanced renal insufficiency. More than 350 million people will be afflicted by diabetes by 2030 and about 20 to 30 percent of these diabetic patients, either type 1 or type 2, will be suffering from diabetic nephropathy, which has a greater incidence as the disease becomes more chronic .
2. Materials and Methods
3. Results
| 0.82* |
| 0.06 |
| 0.97 |
4. Discussion
Ethical Approval
This work complies with all relevant ethical and privacy requirements.
Also Check: Diagnosing Type 1 Diabetes In Children
How Can I Manage My Type 2 Diabetes
Managing your blood glucose, blood pressure, and cholesterol, and quitting smoking if you smoke, are important ways to manage your type 2 diabetes. Lifestyle changes that include planning healthy meals, limiting calories if you are overweight, and being physically active are also part of managing your diabetes. So is taking any prescribed medicines. Work with your health care team to create a diabetes care plan that works for you.
Measures For Prevention Of Diabetic Nephropathy

Efforts should be made to modify and/or treat associated risk factors such as hyperlipidemia, smoking, and hypertension.
Specific goals for prevention include the following:
-
Optimal blood glucose control
-
Control of hypertension
-
Avoidance of potentially nephrotoxic substances such as nonsteroidal anti-inflammatory medications and aminoglycosides
-
Early detection and optimal management of diabetes, especially in the setting of family history of diabetes
Read Also: The Effects Of Diabetes On Your Body
A Review Of The Prevention And Treatment Of Microalbuminuria In Normotensive Type 2 Diabetes
Brookdale Department of Geriatrics and Palliative Medicine at the Icahn School of Medicine at Mount Sinai, New York, New York
B. Brent Simmons, MDAssociate Professor, Department of Family, Community, and Preventive Medicine, Drexel University College of Medicine, Philadelphia, Pennsylvania
CITATION:Patel MP, Simmons BB. A review of the prevention and treatment of microalbuminuria in normotensive type 2 diabetes. Consultant. 2019 59:195-198.
ABSTRACT: Type 2 diabetes mellitus has become the leading cause of nephropathy in the United States. Diabetic kidney disease affects a large percentage of persons with diabetes in their lifetime, and its progression is associated with significant health care costs and decreased quality of life. Microalbuminuria is a well-established early marker for cardiovascular and kidney disease and is associated with increased morbidity and mortality even in healthy individuals. Angiotensin converting enzyme inhibitors and angiotensin receptor blockers both have been shown to reduce microalbuminuria across a wide cohort of patients and therefore are first-line agents for treatment of hypertension and kidney disease in persons with T2DM. However, the role of these medications in the setting of normotensive T2DM with and without microalbuminuria is less clear. This article reviews the guidelines for treatment and prevention of microalbuminuria in T2DM and the evidence from recent research.
EVALUATION AND DIAGNOSIS
GUIDELINES AND TREATMENT
SUMMARY
Study Design And Participants
This was a cross-sectional study among 175 newly diagnosed diabetic patients at Mulago National referral hospital in Uganda conducted between June 2014 and January 2015. All newly diagnosed diabetic patients aged 18 years and above attending the diabetic clinic or admitted to the medical wards of Mulago hospital during the study period who met the inclusion criteria and provided informed consent were recruited consecutively. We excluded patients with urinary tract infection and patients who were unable to provide information.
Recommended Reading: Where To Throw Away Diabetic Needles
Management Of Diabetes With Renal Disease
Slowing the progression of diabetic nephropathy includes optimizing glycemic control , controlling hypertension, and using angiotensin-converting enzyme inhibitors or angiotensin receptor blockers . More controversial interventions include the use of a protein-restricted diet for patients with type 1 diabetes7 and nondihydropyridine calcium channel blockers in the event that ACE inhibitors or ARBs cannot be used for patients with microalbuminuria or nephropathy. Dihydropyridine calcium channel blockers are not effective.3
Albuminuria And Cardiovascular Outcomes In Type 2 Diabetes
A strong association has been reported between microalbuminuria and cardiovascular outcomes in patients with type 2 diabetes. An analysis of 3,498 patients with diabetes and 5,545 patients without diabetes in the Heart Outcomes Prevention Evaluation study found that microalbuminuria increased the adjusted relative risk of major cardiovascular events . Participants with diabetes had a RR of 1.97 and those without diabetes had an RR of 1.61 .
The IDNT study, described above, also reported that albuminuria was an independent risk factor for cardiovascular events . The study defined a cardiovascular composite end point consisting of cardiovascular death, nonfatal myocardial infarction, hospitalization for heart failure, stroke, amputation, and coronary and peripheral revascularization. The ACR was associated with an increased risk of this cardiovascular composite end point . Data from the RENAAL study also demonstrated that the presence of albuminuria was associated with increased cardiovascular events . Cardiovascular events were defined as a composite of myocardial infarction, stroke, first hospitalization for heart failure or unstable angina, coronary or peripheral revascularization, or cardiovascular death. It was found that patients with a high baseline ACR had a 1.92-fold higher risk for the cardiovascular end point and a 2.70-fold higher risk for heart failure compared with patients with low baseline levels of ACR .
Also Check: Type 2 Diabetes Blood Sugar Range
How Can I Lower My Chances Of Developing Type 2 Diabetes
Research such as the Diabetes Prevention Program, sponsored by the National Institutes of Health, has shown that you can take steps to reduce your chances of developing type 2 diabetes if you have risk factors for the disease. Here are some things you can do to lower your risk:
- Lose weight if you are overweight, and keep it off. You may be able to prevent or delay diabetes by losing 5 to 7 percent of your current weight.1 For instance, if you weigh 200 pounds, your goal would be to lose about 10 to 14 pounds.
- Move more. Get at least 30 minutes of physical activity, such as walking, at least 5 days a week. If you have not been active, talk with your health care professional about which activities are best. Start slowly and build up to your goal.
- Eat healthy foods. Eat smaller portions to reduce the amount of calories you eat each day and help you lose weight. Choosing foods with less fat is another way to reduce calories. Drink water instead of sweetened beverages.
Ask your health care team what other changes you can make to prevent or delay type 2 diabetes.
Most often, your best chance for preventing type 2 diabetes is to make lifestyle changes that work for you long term. Get started with Your Game Plan to Prevent Type 2 Diabetes.
Research Design And Methods
We identified 204 patients with a clinical diagnosis of type 1 diabetes for > 30 years in 1995 from the clinic database. Notes could not be found for three cases, three had longstanding insulin-treated type 2 diabetes that had been misclassified, and eight had no urinary albumin measurement recorded in 1995 and were excluded from further study. Therefore, 190 had complete data available from clinic visits in 1995.
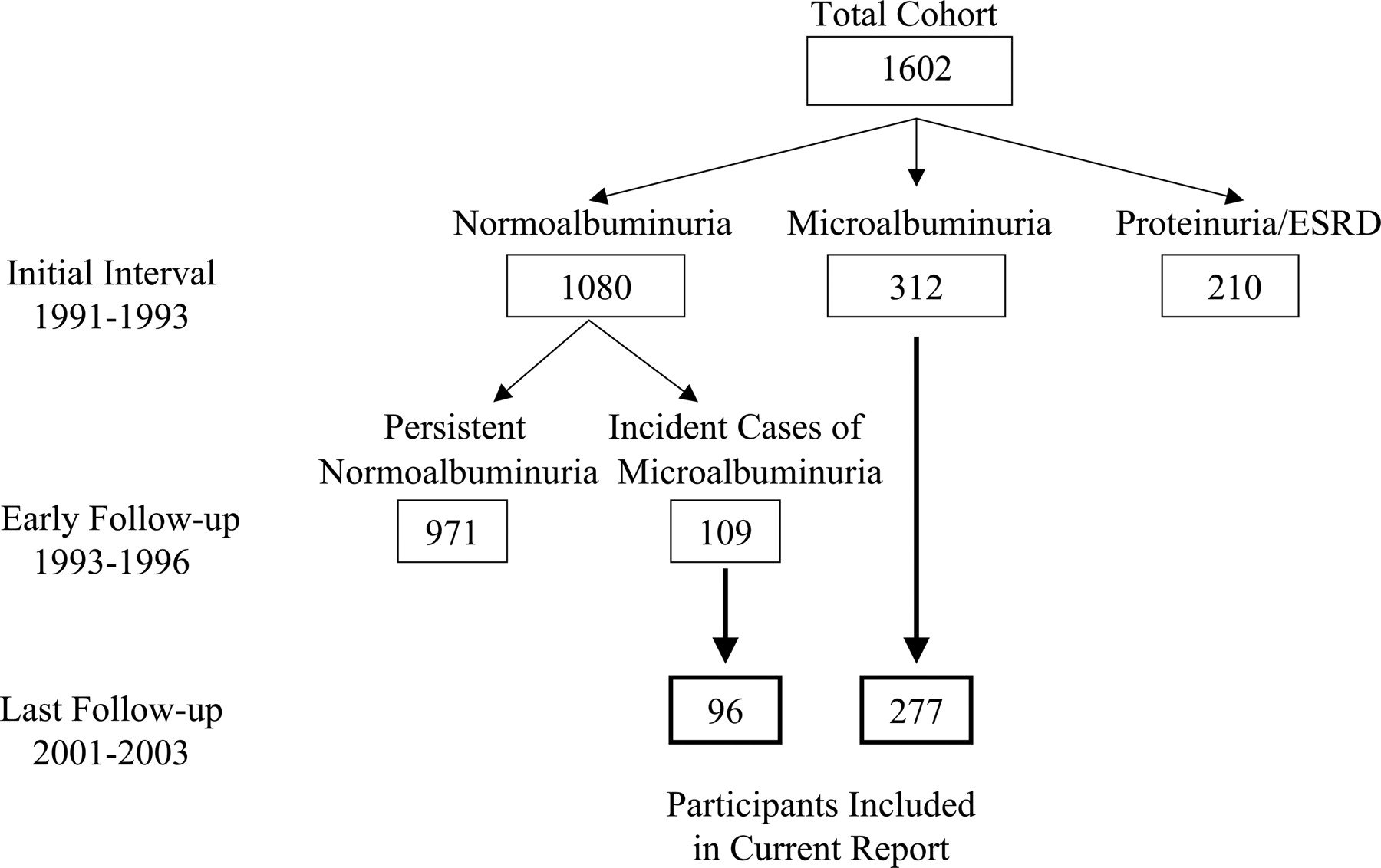
Details of microvascular diabetes complications were obtained by reviewing clinical records along with age, year of diagnosis, BMI, blood pressure, HbA1c, serum creatinine, urine albumin:creatinine ratio, or 24-h urinary protein estimation. Subjects were divided into four groups according to their renal status at baseline: normoalbuminuria , microalbuminuria , proteinuria , or end-stage renal failure due to diabetic nephropathy .
At follow-up in 2000, serum creatinine, urine albumin:creatinine ratio, or 24-h urinary protein estimation were recorded. For those dying before 2000, the cause of death was obtained from death certificates and verified from clinical records review wherever possible. Cardiovascular death was defined as death from ischemic heart disease, heart failure, or cerebrovascular disease. British government actuarial life tables for 19982000 for the U.K. were used to determine life expectancy for nondiabetic individuals .
You May Like: Cost Of Tandem Insulin Pump