Avoiding Blood Sugar Problems
Here are some ways to avoid or manage low and high blood sugar when you have an insulin pump.
- Check your blood sugar often.
You can help prevent low or high blood sugar by checking your blood sugar often.
- People whose blood sugar levels don’t vary much may not be able to sense when they have low blood sugar.
- Pumps use only rapid-acting insulin. So if something goes wrong with the pump and you don’t get enough insulin, your blood sugar may rise.
Talk with your diabetes team about high and low blood sugar so you’re prepared when it happens. For example, if you have low blood sugar, you can slow down or stop your insulin pump for up to an hour until your blood sugar comes back up.
Keep track of your blood glucose results, your carbohydrate intake, changes in your insulin doses, and your exercise. Having records can help you see patterns. It’s very important for managing your blood sugar.
Sometimes the catheter gets a clog or a kink in it, falls out, or gets pulled out. Most pumps have an alarm that will tell you if your catheter is blocked. But if it simply pulls out of your skin, you may not know it until you have symptoms of high blood sugar.
Some insulin pumps include a CGM or work with one.
Ways To Sleep With An Insulin Pump
While not necessarily fashion, many people wonder where to wear the pump while sleeping.We have 12 tips shared with the MiniMed Care team, about what they do with the pump.
1. The PJ Clip
Try clipping your pump to your pyjama waistband. Thicker bands can be really helpful, so the clip doesnt make holes through the material over time.
2. The Undies
Just clip your pump onto your undergarment and tuck the tubing inside the undergarment. The pump is safe and secure and out of the way.
3. The Body Pillow
Some people sleep with a body pillow by their side and put the pump under the pillow. When they switch sides in the middle of the night, they move the pillow with the pump while sleeping.
4. The Blanky Buddy
Make a pouch out of the same material as your childs favorite blanket!
5. The Classic Pocket-T
Wear a T-Shirt with a breast pocket to put your pump in turning the T-Shirt inside out is a top tip.
6. The Bra Clip
Ladies if you are happy to wear a bra to sleep, this can be a good place to clip your pump day and night.
7. The Skilled Sewer
Insulin Pump Cases And Clips
With our selection of cases and clips, there are plenty of ways to wear your insulin pump. You can attach your pump to your waistband or belt, protect it in your pocket, or even clip it under your clothing to stay discreet. Our cases and clips come in a number of different colors and fabrics, from black to pink and from leather to soft neoprene. Choose a case or clip that lets you wear your pump the way you want and lets you express your personal style.
Read Also: Can I Take My Insulin After A Meal
Why Are Insulin Pumps Used
People who have diabetes dont make enough insulin naturally. Instead, they have to use insulin injections to manage their blood sugar.
Pumps offer a steady stream of insulin so that you can have fewer needle sticks. Theyre also a good option for children or anyone who has trouble remembering their insulin injections. Because insulin pumps stay attached to the body, some people find an insulin pump more convenient than insulin pen injections.
Will I Pull Out The Infusion Set
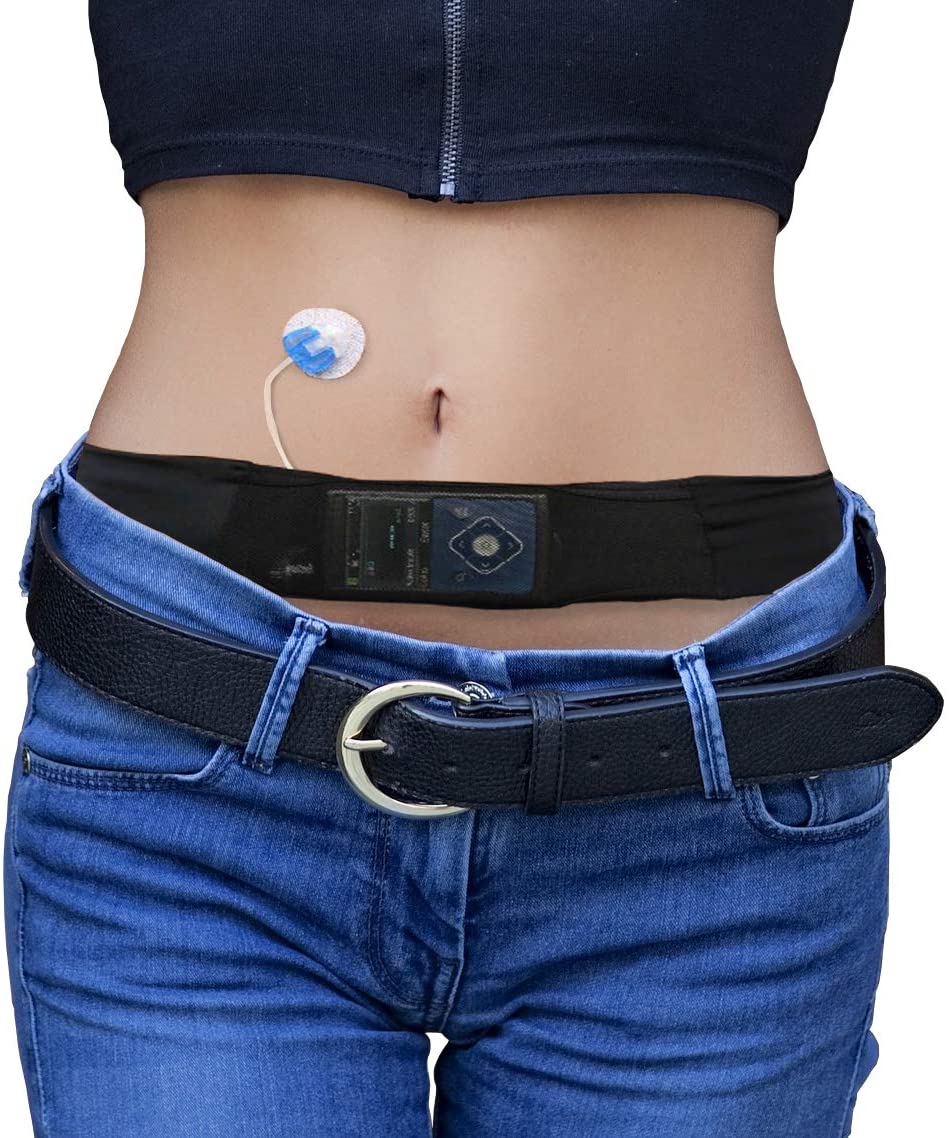
Its unlikely that the infusion set will get pulled out during sleep. In a rare case when the infusion does come out, some pumps will sound an alarm to wake you to reconnect it.
Nobody wants to reconnect their pump in the middle of the night but if you have a spare infusion set near to the bed itll make reconnecting your pump that little bit easier.
Don’t Miss: Heart And Diabetic Friendly Recipes
What Are The Drawbacks
Using an insulin pump isnt always the best option for everyone. Lets take a closer look at some of the drawbacks of this device.
An insulin pump and daily injections are both effective methods of controlling your blood sugar levels. Whats most important is that you monitor your blood sugar carefully and follow your doctors instructions for managing your diabetes.
Its very important that you spend time with a diabetes educator or your doctor to learn how to use your insulin pump properly.
Before you start using an insulin pump, its important that you know how to:
Most pumps contain a bolus dose calculator. This helps you calculate how much extra insulin you may need based on your daily carbohydrate intake.
Some pumps also offer an extended bolus option. This allows you to administer the dose over 2 to 3 hours. This option can help prevent hypoglycemia, or low blood sugar. Hypoglycemia is a potentially dangerous condition.
You must change the insulin in the pump according to the manufacturers recommendations. For example, rapid-acting insulin formulations such as lispro and aspart must be replaced every 144 hours or every 6 days, according to a 2019 study. Glulisine, on the other hand, should be replaced every 48 hours.
Remember that insulin pumps cannot do everything to manage your diabetes. You play the most important role in managing your care, including:
- checking your blood sugar regularly
Which Pump Is Best
All insulin pumps have benefits and drawbacks. Your choice will depend on whatâs most important to you. Do you want easy setup? Low up-front cost? Ease of use? Since most insurance companies will replace your pump only after several years of use, itâs important to find one that works for you.
Some things to think about:
- Which is best for your lifestyle: a traditional pump, tubeless pump, or pump with handheld remote?
- Pump reservoirs hold between 176 and 315 units of insulin. Kids may be fine with smaller reservoirs adults may want larger.
- Can the pump deliver insulin in small amounts? Kids and people who are very sensitive to insulin may want one that does.
- Does the pump come with carb counts of common foods to help you decide how much insulin you need?
- Can the pump interact with a blood glucose meter or continuous glucose meter ?
- Does the pump software work with your phone or laptop?
Read Also: Can A Dentist Tell If You Have Diabetes
Athleta Rincon Bermuda Boardshort
These shorts are perfect for swimming, hiking or casual everyday wear. They have two pockets on the front and two back zippered pockets. The lightweight fabric dries quickly, and the shorts have a 7-inch inseam. When wearing these to the pool or beach, keep your insulin pump in your pocket until you are ready to swim.
Disadvantages Of An Insulin Pump
- Youâll need to enter information into the pump all day and change out the infusion set every few days.
- Youâll need to commit to using it safely, including checking your blood sugar to make sure the pump is working right. Otherwise, you risk a life-threatening problem called diabetic ketoacidosis .
- Youâll need training to learn to use the pump, which means several visits with your health care team or a full day of outpatient training.
- Pump supplies can be expensive.
An insulin pump may not be right for you if:
- You donât want to wear a device that lets people know you have diabetes.
- You donât like the feeling of wearing a device.
- Youâre not comfortable operating the pump.
- You donât want to check your blood sugar at least four times a day.
- Youâre not sure you want to do the work to figure out insulin dosing, carbs, and physical activity.
Read Also: Lantus Insulin Pens For Diabetes
What Are The Advantages
Insulin pump users like managing their type 1 diabetes this way for lots of different reasons. Some of the most common reasons are:
- feeling like you are more in control
- having the flexibility to have a lazy morning, skip a meal or eat late
- delivering food boluses in the most appropriate way, eg spreading it over 7 hours for pizza
- setting a temporary basal increase or decrease when ill, having your cycle, or stressed
- managing the dawn phenomenon
- only needing one needle every 2 or 3 days
Insulin pump users may also find the following things easier:
- managing blood glucose levels around planned or spontaneous exercise
- treating hypers with precise correction doses
- treating hypos with just fast-acting carbohydrate
- managing changing shift work patterns
- managing toddlers meal-time battles
- keeping good control through growth spurts and hormonal changes in adolescence
The Different Types Of Insulin Pumps:
Pumps to administer your insulin come in different shapes and sizes, with and without tubing.
On the website of diabetesexperts.nl there is a guide to choosing an insulin pump. You can find this guide here. Note: the diabetes nurse can tell you something more specific about these insulin pumps. You discuss with her or him what you want to achieve after switching to the pump. Less hypo, for example. Together with your diabetes nurse you decide which one suits you and your goals best.
In our October 2020 livestream we focused extensively on the new generation of insulin pumps, which work together with a continuous glucose meter . Diabetes technology is developing rapidly, so we will have this topic in our livestreams regularly. You can find all the livestreams here.
Recommended Reading: Proliferative Diabetic Retinopathy Icd 10
Modcloth Alfresco Glow Sundress
This dress has patch pockets on the front that can hold your insulin pump. Feed the tubing through on one of the button holes on the front and then slip the pump into your pocket. I find patch pockets on skirts and dresses work well to hold my pump because the pump cannot slip out of the pocket easily.$75.
Minimed 630g Insulin Pump With Optional Cgm

The MiniMed 630G insulin pump delivers precise doses of insulin to your body. When combined with our CGM, it takes action for you with the SmartGuard Suspend on low feature – providing protection that can help keep your glucose levels stable. ,3
Individuals pictured and/or quoted here were compensated for spending the day with us and allowing us to photograph them and their family. Their thoughts and opinions are their own.
Important Safety Information: MiniMed 770G System With SmartGuard TechnologyThe MiniMed 770G system is intended for continuous delivery of basal insulin and administration of insulin boluses for the management of type 1 diabetes mellitus in persons two years of age and older requiring insulin as well as for the continuous monitoring and trending of glucose levels in the fluid under the skin. The MiniMed 770G System includes SmartGuard technology, which can be programmed to automatically adjust delivery of basal insulin based on continuous glucose monitoring sensor glucose values and can suspend delivery of insulin when the SG value falls below or is predicted to fall below predefined threshold values.
The Medtronic MiniMed 770G System consists of the following devices: MiniMed 770G Insulin Pump, the Guardian Link Transmitter, the Guardian Sensor , one-press serter, the Accu-Chek® Guide Link blood glucose meter, and the AccuChek®Guide Test Strips. The system requires a prescription.
Also Check: How Does Insulin Work In Type 1 Diabetes
Disconnecting Your Insulin Pump For Showering Or Bathing
Disconnecting your insulin pump before you take a bath or a shower is the safest way to protect it from getting damaged by the water. Instructions for disconnecting and reconnecting your insulin pump depend on the specific one you’re using. Whether you’re wearing a Medtronic MiniMed, a Tandem T:Slim, a Dexcom, or another insulin pump, you should already be aware of how to disconnect it or read its instruction manual.
It’s important to realize that your insulin pump is constantly injecting microdoses of insulin into your body, so disconnecting it may have an impact on your blood sugar levels. To avoid a rise in glycemia caused by a lack of insulin, it’s recommended to never disconnect your insulin pump for more than one hour. In most cases, disconnecting your device for the time of a shower shouldnt be a problem. But if you want to take a long bath, you should check your blood sugar levels before, during, and after the bath to see how your body responds.
Reasons I Dont Use An Insulin Pump
I get it all the time: What? Why dont you use an insulin pump?
It blows peoples minds that I would choose multiple daily injections over wearing an insulin pump that sits in my skin 24/7.
For many people, an insulin pump offers freedom, flexibility, less stress, and better blood sugars. Not for me. Not even during two pregnancies!
Ive lived with T1D for 23 years, and Ive used an insulin pump exclusively for at least seven of those years. The last time I tried to go back to pumpinggiving the ol tubeless pump a tryI quit within weeks.
Ive figured out how to make multiple daily injections work for me in a way that allows me to achieve my blood sugar goals, be very physically active, eat a flexible diet, and show my diabetes whos boss on a daily basis.
Heres why I dont use an insulin pump.
Don’t Miss: How Many Carbs Allowed For Type 2 Diabetes
Will An Insulin Pump Be Right For Me
Pumps are not right for everyone. You have to be motivated enough to use this tool properly. That means:
- mindfully managing your type 1 diabetes on a day to day basis
- counting carbohydrates and adjusting insulin doses
- checking glucose levels at least four times a day
- checking that your basal rates are correct by occasionally missing meals
- checking your insulin-to-carbohydrate ratios
If you are having to deal with highs and lows despite your best efforts on multiple daily injections , or you have frequent hypos that affect your day-to-day choices, then a pump may help you.
National audits published in 2018 show that just over 15% of adults with type 1 diabetes in England, and just over 32% of children and young people in England & Wales are using an insulin pump.
Important To Realize When Using An Insulin Pump:
- There is something about your body that you can see clearly and that raises questions for those around you.
- You have to bolus for everything you eat. This means that you always have to think about it, even at times when it might not be convenient or when you have many other things on your mind.
- The pump’s operation can malfunction for any reason. If the insulin does not enter properly, for example due to a kink/clog in the tube, you can become very ill due to excessively high glucose levels. This is called a ketoacidosis. So you have to be very aware of your glucose levels and be really careful with your pump, the tube and the cannula.
With the insulin pump, you can generally achieve better glucose control than with injections, but you have to do something to do that. Unfortunately, the pump doesn’t work by itself yet. Meanwhile, technology is advancing by leaps and bounds, as we see with the Tandem T:Slim X2, and the Medtronic 780G. These pumps can take over a lot from you, both with a threatening low blood sugar and with a threatening high blood sugar. Developments in diabetes technology are rapid and our medical team follows them closely. So it is very important to be well informed by your team. What is not appropriate now may change completely in a year.
Read Also: Whats A Good A1c For A Type 2 Diabetes
Type 1 Diabetes: Tips For Summer Fashion
Wear what makes you feel comfortable and confident. Diabetes does not define who you are and it does not have to limit your summer style.
Letting your devices show can be a conversation starter. You never know who you will meet because of it.
Be proud of who you are, use and wear your medical devices with confidence. If people ask about them, it can be an opportunity to educate on the reality of diabetes.
Womens bathing suits can be challenging to find a place to put your pump. Choose a style of bathing suit bottoms with a thicker waistband and clip the pump to your waistband. Or wear your pump in a pair of swim shorts with pockets.
One-piece swimsuits with a cutout in the pack provide a nice place to clip your pump. Or wear a tankini and clip your pump to your waistband and hide the pump under the tankini swimsuit top.
For mens bathing suits, choose a style with pockets or with a liner that has a built in cellphone pocket.
Dont let your insulin pump hold you back from wearing outfits you love. Get creative and find ways to make the outfit work with the pump. You can hide your pump in your bra, a small running belt around your waist, a pair of spandex/ biking shorts under a dress, or by using a leg garter or arm band to hold the pump.
If you do not want your insulin pump tubing to show you can cut a little hole in the pocket of your favorite shorts. Feed the tubing through the hole into your pocket where your pump is kept.
Choosing And Using An Insulin Pump Infusion Set
When a person uses an insulin pump to control his diabetes, one of the decisions he has to make is what model of infusion set to use. Pumps are often an excellent choice for people who use insulin and seek tight control of their diabetes but need some flexibility in their diabetes regimen.
Most insulin pumps require the use of an infusion set to deliver insulin from the pump to the user. An infusion set consists of a length of thin plastic tubing, a very thin stainless steel or Teflon cannula that is inserted just under the skin, and a plastic connector that joins tubing and cannula together. The connector is generally mounted on an adhesive patch that is stuck to the skin at the insertion site to help keep the cannula in place. The connector allows a person to disconnect from his pump temporarily without removing the infusion set.
Insulin infusion sets come in a variety of styles to suit individuals unique needs and preferences. In addition to having either a Teflon or steel cannula, infusion sets may be designed to have the cannula inserted straight into the subcutaneous tissue or at an angle. Some cannulas can only be inserted manually, while others can be inserted either manually or with an insertion device. All infusion sets offer a variety of tubing lengths.
You May Like: How Many Carbs Should A Pre Diabetic Eat Per Day