What Is Type 1 Diabetes
Youve probably heard of diabetes. But did you know there are two types?
Typically, people with type 2 diabetes have opportunities to rid their bodies of the disease. Oftentimes, treatment involves lifestyle changes, like diet and exercise.
For those with type 1 diabetes, theres no cure. However, those with the disease manage their condition with insulin.
Dr. Stephen Rich, one of the studys researchers, serves as the director of the Center for Public Health Genomics within the University of Virginias School of Medicine. He also serves as a professor of Public Health Sciences and a professor of Biochemistry, Microgenetics and Biology.
Rich explained that the immune system is responsible for type 1 diabetes. Normally, the immune system fights off viruses and pathogens. With type 1 diabetes, instead of attacking the virus or pathogen, the immune system attacks the body.
Theres a whole series of autoimmune diseases. Type 1 diabetes is probably the most common, but its also rheumatoid arthritis, juvenile idiopathic arthritis, lupus, inflammatory bowel disease. Theres a whole series of myasthenia gravis, multiple sclerosis, Rich said. And in fact, these auto-immune diseases tend to cluster together. So sometimes you might have families where someone has type 1 diabetes and some family member might have an autoimmune thyroid disease like Graves disease or Hashimotos thyroiditis or something else.
A Cure For Type 1 Diabetes For One Man It Seems To Have Worked
A new treatment using stem cells that produce insulin has surprised experts and given them hope for the 1.5 million Americans living with the disease.
- Read in app
-
Send any friend a story
As a subscriber, you have 10 gift articles to give each month. Anyone can read what you share.
Give this article
- Read in app
Brian Sheltons life was ruled by Type 1 diabetes.
When his blood sugar plummeted, he would lose consciousness without warning. He crashed his motorcycle into a wall. He passed out in a customers yard while delivering mail. Following that episode, his supervisor told him to retire, after a quarter century in the Postal Service. He was 57.
His ex-wife, Cindy Shelton, took him into her home in Elyria, Ohio. I was afraid to leave him alone all day, she said.
Early this year, she spotted a call for people with Type 1 diabetes to participate in a clinical trial by Vertex Pharmaceuticals. The company was testing a treatment developed over decades by a scientist who vowed to find a cure after his baby son and then his teenage daughter got the devastating disease.
Mr. Shelton was the first patient. On June 29, he got an infusion of cells, grown from stem cells but just like the insulin-producing pancreas cells his body lacked.
Now his body automatically controls its insulin and blood sugar levels.
Its a whole new life, Mr. Shelton said. Its like a miracle.
But, he said, bottom line, it is an amazing result.
Researchers May Be Close To A Cure For Type 1 Diabetes
Science could be well on its way to a cure for type 1 diabetes, as researchers hone transplant therapies designed to restore patients’ ability to produce their own insulin, experts say.
At least one patienta 64-year-old Ohio man named Brian Sheltoncan now automatically control his insulin and blood sugar levels without the need for medication, following a transplant of experimental pancreatic stem cells.
Shelton’s therapy isn’t a perfect cure. He must take a heavy dose of immune-suppressing drugs to keep his body from rejecting the transplant, and those drugs pose their own health hazards.
But the therapy created by Vertex Pharmaceuticals could provide immediate relief to thousands who are lined up for a pancreas transplant because their type 1 diabetes has progressed to the point where it’s life-threatening, said Sanjoy Dutta, chief scientific officer for JDRF International.
Some of these folks are suffering hypoglycemic shock and landing in an emergency room multiple times a month, while others have developed resistance to the insulin shots or other diabetes medications that have helped keep them alive.
“Today, there are probably 5,000 to 10,000 people or more cued up for pancreatic or islet transplantation, but they’re not going to get it because there’s not enough supply,” Dutta said.
“The first goal is to do this at multiple centers. They’ve only reported one patient at this point,” he said. “They want to do 17 people and probably have the same approach in all 17.”
Recommended Reading: How To Get Diabetes Under Control
Approaching A Cure: Treatments Offer Promise To Delay Improve Life With Type 1 Diabetes
View Issue Disclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact .
For people living with type 1 diabetes and the clinicians and researchers who treat and study the disease, 2021 was a year of groundbreaking achievements and cause for optimism. Though as with any new experimental treatments, caveats abound.
Developments in the fields of beta-cell regeneration, investigational cell therapy, stem cell transplantation and immunotherapy, among others, have yielded big gains in type 1 diabetes research during the past year, seemingly month after month. In April, the FDA granted breakthrough therapy designation for an oral, once-daily glucokinase activator as an adjunct to insulin shown to improve glycemic control without increasing risk for hypoglycemia. That same month, an FDA advisory panel voted in favor of the investigational cell therapy donislecel , shown to increase insulin independence and decrease the number of severe hypoglycemic events among patients with difficult-to-control type 1 diabetes.
In May, an FDA advisory panel recommended approval of the immunotherapy teplizumab , shown to delay development of type 1 diabetes for some high-risk children and adults, in some cases by years, although the agency ultimately declined to approve the therapy.
Progress accelerating
Its not a fantasy … it can happen
Teplizumab: Promise of delayed diagnosis
Ensuring access to new discoveries
How To Find Out If You Have Diabetes
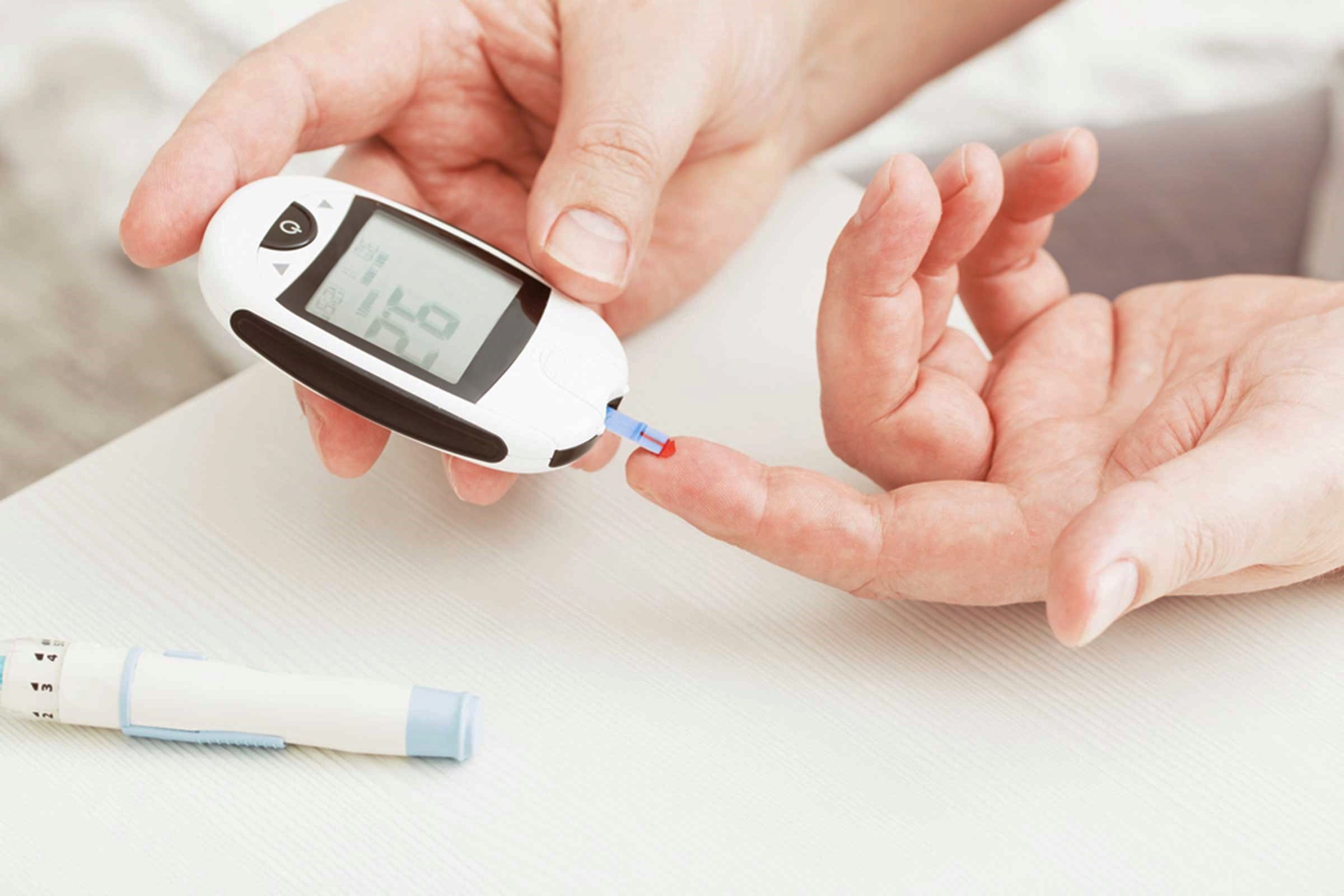
There are a couple of tests available for detecting type 1 diabetes. These include fasting plasma glucose test , oral glucose tolerance test , and blood glucose level test . These tests are long-term and are designed to be duplicated on a weekly basis after a specified quantity of time. If after a week your blood glucose level is still elevated, you must see a medical professional for a glucose screening to be done. However, there are other diabetes symptoms you can keep an eye out for, and if youre experiencing any of them you must seek advice from a medical professional as soon as possible.
Don’t Miss: Telehealth For Diabetes Self Management
Can Type 1 Diabetes Be Cured With Diet
Blood sugar and insulin production are both connected to digestion. Because of this link, it may seem logical to think that certain foods or minerals can cure diabetes. However, its not that simple.
The American Diabetes Association is straightforward in its nutrition advice to people with type 1 diabetes. Diets are as unique as individuals, and nutrition guidelines for people with diabetes have much in common with those for people without diabetes:
- Eat portions that are appropriate for your health goals.
- Choose foods rich in fibers, vitamins, and minerals.
Islet Autoantibody Seroconversion In Type
Here, by characterizing gut metagenomes of at-risk children in the TEDDY project, the authors associate onset of autoimmunity leading to Type-1 diabetes with certain sets of microorganisms in the gut microbiota, and identify metabolic capabilities encoded in the genomes of these microorganisms that provide functional insights to the association.
Recommended Reading: Who Buys Diabetic Testing Supplies
Nanotherapy Offers New Hope For The Treatment Of Type 1 Diabetes
- Date:
- Northwestern University
- Summary:
- Individuals living with Type 1 diabetes must carefully follow prescribed insulin regimens every day, receiving injections of the hormone via syringe, insulin pump or some other device. And without viable long-term treatments, this course of treatment is a lifelong sentence. Now a team of researchers has discovered a better way.
Individuals living with Type 1 diabetes must carefully follow prescribed insulin regimens every day, receiving injections of the hormone via syringe, insulin pump or some other device. And without viable long-term treatments, this course of treatment is a lifelong sentence.
Pancreatic islets control insulin production when blood sugar levels change, and in Type 1 diabetes, the body’s immune system attacks and destroys such insulin-producing cells. Islet transplantation has emerged over the past few decades as a potential cure for Type 1 diabetes. With healthy transplanted islets, Type 1 diabetes patients may no longer need insulin injections, but transplantation efforts have faced setbacks as the immune system continues to eventually reject new islets. Current immunosuppressive drugs offer inadequate protection for transplanted cells and tissues and are plagued by undesirable side effects.
Specifying the body’s attack
Scott, also a member of CARE, said he wanted to see how the drug could be enhanced by putting it in a nanoparticle and “controlling where it goes within the body.”
Research hits close to home
Specifying The Bodys Attack
Guillermo Ameer has been working on improving the outcomes of islet transplantation by providing islets with an engineered environment, using biomaterials to optimize their survival and function. However, problems associated with traditional systemic immunosuppression remain a barrier to the clinical management of patients and must also be addressed to truly have an impact on their care, he said.
This was an opportunity to partner with Evan Scott, a leader in immunoengineering, and engage in a convergence research collaboration that was well executed with tremendous attention to detail by Jacqueline Burke, a National Science Foundation Graduate Research Fellow, Ameer said.
Rapamycin is well-studied and commonly used to suppress immune responses during other types of treatment and transplants, notable for its wide range of effects on many cell types throughout the body. Typically delivered orally, rapamycins dosage must be carefully monitored to prevent toxic effects. Yet, at lower doses it has poor effectiveness in cases such as islet transplantation.
Scott, also a member of CARE, said he wanted to see how the drug could be enhanced by putting it in a nanoparticle and controlling where it goes within the body.
Also Check: Where To Get Diabetic Test Strips
A Pipe Dream Come True In Diabetes Research
The team tested the hypothesis on mice, introducing diabetes to the population before treating them with a combination of islet transplantation and rapamycin, delivered via the standard Rapamune® oral regimen and their nanocarrier formulation. Beginning the day before transplantation, mice were given injections of the altered drug and continued injections every three days for two weeks.
The team observed minimal side effects in the mice and found the diabetes was eradicated for the length of their 100-day trial but the treatment should last the transplants lifespan. The team also demonstrated the population of mice treated with the nano-delivered drug had a robust immune response compared to mice given standard treatments of the drug.
The teams discovery could have far-reaching implications. This approach can be applied to other transplanted tissues and organs, opening up new research areas and options for patients, Ameer said. We are now working on taking these very exciting results one step closer to clinical use.
Jacqueline Burke, the first author on the study and a National Science Foundation Graduate Research Fellow and researcher working with Scott and Ameer at CARE, said she could hardly believe her readings when she saw the mices blood sugar plummet from highly diabetic levels to an even number. She kept double-checking to make sure it wasnt a fluke, but saw the number sustained over the course of months.
See More Of Type 1 Diabetes Cure Related Research News On Facebook
Stanford researchers devise method for bone marrow transplants without using chemotherapy. “Once a patient’s blood and immune system can safely be replaced, any disease caused by the patient’s own blood and immune cells could potentially be cured by a one-time application of blood stem cell transplantation, they said. Safely replacing a patient’s blood and immune cells will get rid of the cells that attack their own tissues and produce disease like rheumatoid arthritis and Type 1 diabetes.” Tightly and automatically matching the release of hormones such as insulin to control blood sugar levels for Type 1 diabetics is the Holy Grail in the development of an artificial pancreas. Now researchers may have come one step closer with a fully implantable insulin delivery and glucose sensing system that is guided by a novel algorithm. The device is intended to be implanted in the intraperitonea… See MoreContinue reading > >
Read Also: Healthy Diet Plan For Diabetic Patient
Stop The Immune Attack
In type 1 diabetes, the immune system is unable to tell the difference between harmful germs and the body’s cells and tissues, so the immune system attacks the bodys own insulin producing beta cells.
One way to cure diabetes could be to persuade a badly behaved immune system to accept the beta cells as part of the body.
Some of the immune system culprits attacking the beta cells are T cells. T cells develop in the thymus gland and, from a naïve or undifferentiated state, they are gradually educated to become helpers, warriors, or regulators.
In type 1 diabetes, the helper and warrior T cells work together to kill the beta cells, while the regulators appear unable to stop this from happening.
A/Prof Grey’s team worked up a vaccine, called BCMA-Fc, that re-dressed this imbalance. When given to mice with a disease similar to type 1 diabetes, the vaccine prevented diabetes by increasing the number of regulator T cells and reducing the number of warriors.
This work shows the potential of stopping the immune attack as a way to prevent type 1 diabetes. It has supported the testing of a related compound, called rituximab, in people with promising results. In a USA trial, people kept the ability to produce their own insulin, after diabetes had started, for up to 18 months. Further study will test whether taking this drug repeatedly will continue to maintain insulin production.
Stem Cells May Finally Offer A Cure For Type 1 Diabetes
There are 537 million people around the world living with diabetes. And that number is growing.
When people have Type 1 diabetes, the immune system attacks and destroys the beta cells in the pancreas that make insulin. These cells regulate glucose levels in the blood which the body needs for energy. Blood sugar will continue to rise without insulin, so Type 1 diabetics must inject insulin for the rest of their lives.
But over the past 20 years, significant advancements in stem cell research and therapies have revealed promising methods of creating new insulin-making cells, which are needed to cure Type 1 diabetes.
Biotech company Vertex Pharmaceuticals recently began a clinical trial where it plans to treat 17 participants who have Type 1 diabetes with new insulin-making cells derived from stem cells. The first patient in the trial, Brian Shelton, has had positive results. After 150 days, Shelton was able to reduce the amount of insulin he injects by 92%.
Other global companies are also working to cure diabetes, such as ViaCyte, CRISPR, and , one of the biggest insulin manufacturers in the world.
Watch the video to hear how stem cell therapy has changed Shelton’s life and what other diabetes cures are being developed.
You May Like: What Insulin Pumps Are Covered By Medicaid
Whole Genome Sequencing For Type 1 Diabetes
Using very new genome technologies and cutting edge scientific methods, my team is embarking on a new program with the aim of functionally annotating the gene changes in type 1 diabetes. To start, we have sequenced the entire genomes of 50 individuals with type 1 diabetes.
Already, even at this early stage of this newest program, we have made an exciting discovery. We have shown how single-nucleotide polymorphism changes in one particular gene called A20 not only contributes to diabetes susceptibility, but also enhances rejection in islet transplantation.
This exciting data provides tantalising new information that will help to bring us closer to a better understanding of type 1 diabetes and hopefully, to a cure.
Every day, scientists all around the world are making progress toward a cure for type 1 diabetes. While it is difficult to say how long it will be before a cure is finally realised, we can reflect on how far we have come since the discovery of insulin in the early twentieth century, and look forward to more new and exciting discoveries that will bring us closer to a cure for type 1 diabetes.
When Will This Become Available To More People With Type 1 Diabetes
Similar to people who receive other organ transplants, those who receive VX-880 must continually take immunosuppressants to prevent the bodys immune system from rejecting the new beta cells. We use a standard regimen of immunosuppressants, also used in patients receiving kidney transplants, an established regimen weve found to be generally well-tolerated, Markmann said.
Currently, because of the risks of infection associated with immunosuppressants, only those with severe hypoglycemia unawareness have been eligible to be candidates for this initial research. This is because these candidates specifically have the most to gain from this type of therapy given the risks associated with hypoglycemia unawareness.
Unlike other interventions such as full pancreas transplants or beta cell islet transplants from human donors, VX-880 has the potential to be used on a much larger scale.
Right now in the US, there are only about 1,000 pancreas transplants available, so the supply is a significant problem, Markmann said. Additionally, islets tend to be variable in quality. One of the most important aspects of this work is that there can be an unlimited supply of beta cells for transplantation going forward.
However, on May 2, 2022, the FDA paused the trial after concluding that there was not enough evidence to support increasing the dosage of beta cells to the full planned amount.
Read Also: Best Frozen Yogurt For Diabetics