Check Proper Shoe Fit
Purchasing properly fitting shoes is the simplest way to prevent diabetic wounds on your feet. Ill-fitting shoes rub and cause blisters to form, and those blisters quickly lead to diabetic foot ulcers. The right shoes will be tight enough to stop fabric from rubbing against the skin, but loose enough to fit all toes comfortably. Many diabetic patients even choose specialty orthopedic shoes that are custom made to fit the size, shape, and contours of their feet.
A Word From Mantracare
If you are looking for more information on this topic or Diabetes treatment, Online Therapy, Hypertension, PCOS treatment, Weight Loss, and Physiotherapy, please visit mantracare.org or feel free to reach out to us at +91-9711118331 or email at . You can also download our free Android App or IOS app.
Here at Mantra Care, we have an incredibly skilled team of health care professionals and coaches who will be happy to answer any questions and provide further information so you know whats best for your unique needs.
The Bodys Normal Wound
A wound is considered a break or opening in the skin. Since your skin protects the rest of your body from pathogens and bacteria, its easy for a wound like a puncture or cut to cause infection.
In a body unaffected by diabetes, every wound triggers a natural healing process that begins within minutes of the injury. Blood flows and eventually clots to form a scab, which serves the valuable purpose of protecting underlying tissues from bacteria.
Once the scab has formed, the immune system fights off infection by opening nearby blood vessels to deliver oxygen and nutrients to the wound. This makes it possible for powerful white blood cells to prevent infection, combat germs, and support the wound as it heals.
This entire process usually only takes about two to five days, but invisible healing continues for weeks as the body repairs broken blood vessels and grows new tissue.
Also Check: How Do Diabetics Check Their Blood Sugar
The Reality Is Diabetic Wounds Require High Attention To Achieve Healing
To help achieve the best possible healing environment and protect against infection, here are six key factors to keep in mind when treating diabetic wounds.
Wound AssessmentDiabetic wounds fall into three basic categories: neuropathic, ischemic, and neuroischemic. Knowing the distinct features of each category is essential to identifying wound progression, infection, and healing. Failure to properly identify the type of wound that exists can lead to an ineffective diabetic wound treatment plan, causing long-term complications or even amputation. So in a nutshell, see a doctor who is qualified to identify and classify your wound.
Tissue Debridement the removal of necrotic tissue from a wound will reduce pressure, stimulate healing, allow for inspection of underlying tissue and help with secretion or drainage. Only an experienced practitioner, who knows which section of the tissue to remove without damaging blood vessels, nerves, or tendons, should perform debridement. Debridement is an important part of a treatment plan for advanced diabetic wounds.
Infection Control Infections are the main concern with diabetic wounds. Typically, oral and topical antibiotics will be used. Additionally, topical antimicrobials can reduce bacteria, protect against further contamination, and prevent the spread of infection deeper into the wound. Typical wound dressings used in treating diabetic wounds are infused with antimicrobial agents to help fight infection.
What Causes A Diabetes Rash
For people who dont have diabetes, a skin rash may be the first sign of high blood sugar or prediabetes. Your healthcare provider can help you take steps to prevent diabetes.
If you take medications for diabetes, a skin rash may indicate that you need to adjust treatments to lower your blood sugar levels. Some other rashes result from reduced blood flow to your extremities .
Read Also: How To Treat A Corn When Diabetic
The Most Common Diabetic Wounds
Wounds can develop anywhere on the body, but diabetics are most vulnerable to cuts, scrapes, and sores on their lower extremities.
Diabetic wounds do occur on the knees and legs, but theyre most frequently found on the feet in the form of diabetic foot ulcers. Given that diabetic foot problems are the most common cause of hospitalization among diabetic patients, proper treatment is essential to long-term health.
What Is A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, 6 percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of non-traumatic lower extremity amputations in the United States, and approximately 14-24 percent of patients with diabetes who develop a foot ulcer will require an amputation. Foot ulceration precedes 85 percent of diabetes-related amputations. Research has shown, however, that development of a foot ulcer is preventable.
Recommended Reading: Can Someone With Type 1 Diabetes Join The Military
How Do You Treat Dermopathy
Treatment of Graves dermopathy is usually aimed at correcting the overactive thyroid responsible for Graves disease. Youll also be advised to quit smoking and to avoid trauma to the skin as much as possible. Treatment of the affected skin may also include: Cortisone creams to reduce inflammation.
Do You Have A Diabetic Foot Ulcer
Since nerve damage may prevent you from feeling the pain of your diabetic foot ulcer, its important to visually inspect your feet every day. If you notice any of the following signs, seek medical care immediately:
- Drainage from your foot is staining your socks or leaking from your shoe
- Unusual swelling
- Strong, irregular odor from one or both feet
- Black tissue surrounding a wound on the foot
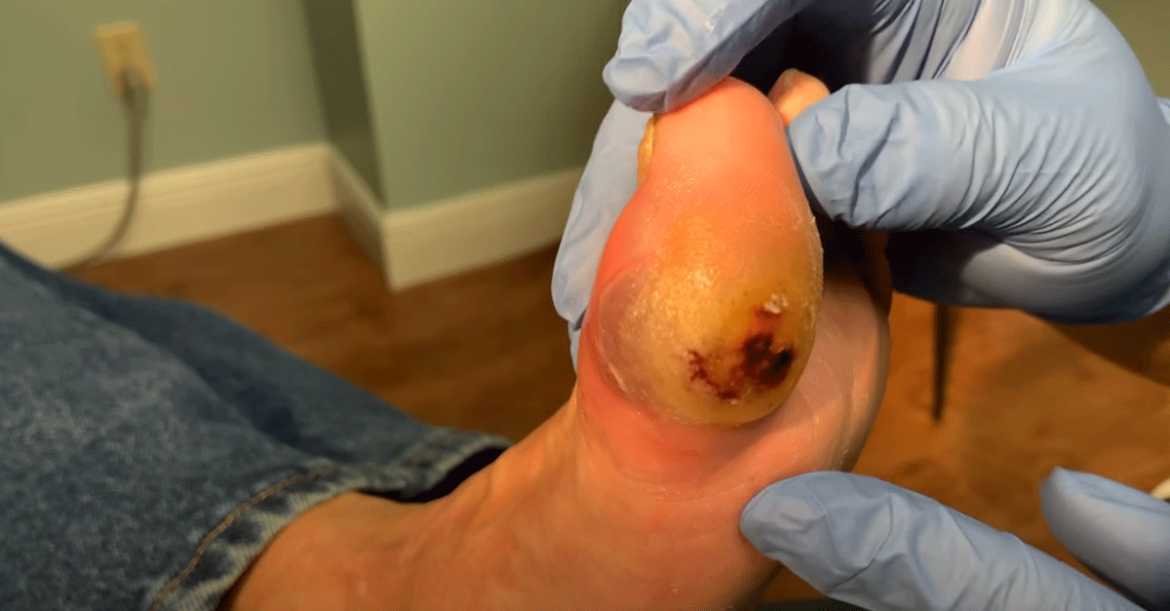
Many diabetic foot ulcers develop under the big toe and along the balls of the feet. The earlier you can identify your diabetic foot ulcer and receive treatment, the better your chances of preventing severe complications.
Also Check: Is Equal Good For Diabetics
When To See A Dermatologist
Diabetes can cause many other skin problems. Most skin problems are harmless, but even a minor one can become serious in people who have diabetes. A board-certified dermatologist can recognize skin problems due to diabetes and help you manage them.
Are all dermatologists board certified?
No. See what it takes to become board certified.
ImagesImage 1: Image Courtesy of Clark C. Otley, MD. All Rights Reserved
Images 3, 7, 8, 9: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2 from DermNetNZ
Some images used with permission of Journal of the American Academy of Dermatology
ReferencesCohen Sabban, EN. Cutaneous manifestations of diabetes mellitus from A to Z. Focus session presented at: 74th Annual Meeting of the American Academy of Dermatology March 4-8, 2016 Washington D.C.
Duff M, Demidova O, et al. Cutaneous manifestations of diabetes mellitus. Clinical Diabetes. 2015 33:40-8.
Kalus AA, Chien AJ, et al. Diabetes mellitus and other endocrine disorders. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine . McGraw Hill Medical, New York, 2008:1461-70.
McKinley-Grant L, Warnick M, et al. Cutaneous manifestations of systemic disease. In: Kelly AP and Taylor S. Dermatology for Skin of Color. . The McGraw-Hill Companies, Inc. China, 2009:481-4.
Morgan AJ and Schwartz RA. Diabetic dermopathy: A subtle sign with grave implications. J Am Acad Dermatol. 2008 58:447-51.
Natural Remedies To Treat Diabetic Ulcers
Natural Remedies to Treat Diabetic Ulcers Diabetic Ulcers are pretty much worse than a nightmare. These are extremely ugly and can lower your overall confidence. In diabetes blood, sugar level is higher than the normal and when there is a lack of healthy blood circulation it leads to ulceration. Therefore, neuropathy and vascular complication cause diabetic Ulcer. It is really important to treat diabetic ulcers with the time to avoid other health complication. You can try some ayurvedic home remedies for diabetic ulcer treatment.
Diabetic Ulcer is the problem arising in most of the diabetic patient and is a matter of concern. According to the stats around 6.3% of people are suffering from diabetic foot ulceration globally. It also matters of concern that diabetic Ulcer found in the 19-34% patients as a lifetime problem. Thus, it is important to treat the diabetic ulcer on time for preventing serious health issues in the future.
Recommended Reading: What Is Type Ii Diabetes
How Are Diabetic Feet Diagnosed
To diagnose diabetic foot, a healthcare provider will:
- Ask about your symptoms and how well youre controlling blood glucose.
- Examine your toes, feet and legs.
- Touch the toes, feet and legs with various tools to check whether you have numbness.
If a diabetic ulcer or blister is present, the healthcare provider will likely:
- Examine it for any signs of infection, such as redness, swelling, warmth, discoloration or discharge.
- Order tests to take pictures deeper than the skin, such as X-ray or MRI.
- Take a sample of the skin or discharge to test for infection.
Preventing Cuts And Scrapes
Of course, the best way to protect yourself is to make a serious effort to prevent wounds. Make sure you never walk barefoot, even inside your home, and always wear good-fitting shoes. I also tell my patients to check the inside of their shoes for stones, Weber said. If you have neuropathy, you could get a small stone in your shoe and not know it.
Protect your feet by letting your podiatrist handle even minor foot issues. Dont try to remove calluses or warts yourself.You might be tempted to try commercial preparations you see at your pharmacy, but they can burn your skin, which could cause serious damage to your foot. If you attempt to cut a callus or wart with a razor blade or other instrument, you could end up cutting yourself and have an even more serious problem than you started with. If you have calluses, warts, or corns, have your podiatrist treat them.
If you develop a callus, use a pumice stone to keep it under control. Apply it when your skin is wet, and use lotion immediately afterward.
Also Check: Medical Management Of Diabetes Mellitus
What To Expect At Home
Diabetes can damage the nerves and blood vessels in your feet. This damage can cause numbness and reduce feeling in your feet. As a result, your feet are more likely to get injured and may not heal well if they are injured. If you get a blister, you may not notice and it may get worse.
If you have developed an ulcer, follow your health care provider’s instructions on how to treat the ulcer. Also follow instructions on how to take care of your feet to prevent ulcers in the future. Use the information below as a reminder.
Extremely Dry Itchy Skin
Dry, itchy skin
If you have diabetes, youre more likely to have dry skin. High blood sugar can cause this. If you have a skin infection or poor circulation, these could also contribute to dry, itchy skin.
Take action
- Tell your doctor about your extremely dry skin. Gaining better control of diabetes can reduce dryness.
- If you continue to have dry skin after you gain better control of your diabetes, a dermatologist can help.
Recommended Reading: How To Treat Diabetes Without Insulin
Tips To Prevent Ulcers
Thereâs a lot you can do to lower your chance of having ulcers in the first place:
Keep your blood sugar in check. Good blood sugar control is the single best way to prevent small cuts and sores from becoming ulcers. If you have trouble managing your blood sugar, tell your doctor. They can work with you to make changes to your medication and lifestyle that will keep your blood sugar from getting too high. Even if your blood sugar level is fairly steady, itâs still important to see your doctor regularly. Thatâs especially key if you have neuropathy, because you may not feel damage to your skin and tissue.
Check your skin every day, and pay special attention to your feet. Look for blisters, cuts, cracks, sores, redness, white spots or areas, thick , discoloration, or other changes. Donât rely on pain even feeling more warmth or cold than usual can be a sign that you have an open wound on your skin, and itâs possible that you may feel nothing at all.
Ulcers are most likely to form on the ball of your foot or the bottom of your big toe, so be sure to check your feet every night. If you notice a problem, or you arenât sure if somethingâs normal, call your doctor.
Donât smoke.Smoking damages your blood vessels, decreases blood flow, and slows healing. Those things raise your risk of ulcers and amputation.
Show Sources
Caring For A Pressure Sore
Stage I or II sores will often heal if cared for carefully. Stage III and IV sores are harder to treat and may take a long time to heal. Heres how to care for a pressure sore at home.
Relieve the pressure on the area.
- Use special pillows, foam cushions, booties, or mattress pads to reduce the pressure. Some pads are water- or air-filled to help support and cushion the area. What type of cushion you use depends on your wound and whether you are in bed or in a wheelchair. Talk with your health care provider about what choices would be best for you, including what shapes and types of material.
- Change positions often. If you are in a wheelchair, try to change your position every 15 minutes. If you are in bed, you should be moved about every 2 hours.
Care for the sore as directed by your provider. Keep the wound clean to prevent infection. Clean the sore every time you change a dressing.
Avoid further injury or friction.
- Powder your sheets lightly so your skin doesnt rub on them in bed.
- Avoid slipping or sliding as you move positions. Try to avoid positions that put pressure on your sore.
- Care for healthy skin by keeping it clean and moisturized.
- Check your skin for pressure sores every day. Ask your caregiver or someone you trust to check areas you cant see.
- If the pressure sore changes or a new one forms, tell your provider.
Take care of your health.
Don’t Miss: New Cures For Type 1 Diabetes
Diabetic Leg Ulcers: Home Remedies To Heal Leg Sores
Among the more significant side effects of diabetes are diabetic leg ulcers, open leg sores that may afflict the feet or legs, once or recurrently, and break down the skin’s protective barrier so that infection may more easily enter the body to cause disease and further tissue damage at the site of the ulcer. These ulcers often occur with advanced diabetes because the diabetic patient does not feel the damage occurring to the skin, where neuropathy has affected pain receptors in the legs and feet.
There are other health concerns that can cause leg ulcers including trauma, impetigo, tuberculosis, and cellulitis. However, diabetic leg ulcers are the most common. These result from blocked arteries and as a secondary effect of the neuropathy that often comes with an uncontrolled diabetic condition. The atherosclerosis that blocks leg arteries causes arterial insufficiency, a lack of circulation to the area where ulcers subsequently occur.
Preventing A Diabetic Foot Ulcer
Holistic treatment of the individual with diabetes can help treat the underlying health issues and not only promote faster wound healing but also minimize risk factors that may have contributed to the development of a diabetic foot ulcer. Good diabetic control and lifestyle modification include:
- Keeping blood glucose levels optimal.
- Good nutrition and eating habits.
- Reducing high blood pressure.
- No smoking.
Individuals with diabetes should be instructed to:
- Examine their feet daily with a mirror and to look carefully for fungal infections or any abnormality.
- Wash and dry feet at least once a day in lukewarm water , paying special attention to dry between the toes.
- Not use heating pads or put feet close to heaters.
- Always use footwear inside and outdoors.
- Use close-toed shoes if they cant feel their feet.
- Always use socks and change them daily.
- Have their nails cut carefully straight across by a trained professional .
- Treat dry feet with lubricants containing urea or salicylates, but dont apply between toes.
In addition, every patient with diabetes should have a comprehensive foot exam yearly. Along with a careful physical exam, health care professionals should reinforce best practices of diabetic foot self-care at each visit to make sure the individual understands the recommendations and importance of caring for their feet.
Recommended Reading: What Is The Most Common Form Of Diabetes
What Causes Diabetic Foot Ulcer
People with diabetes have an increased chance of developing foot ulcers because you are more likely than other people to damage the skin on your feet. This is because diabetes can cause nerve damage, so you don’t notice if your foot is injured or sore. Diabetes also causes blood vessel damage so your skin can’t heal easily.
Diabetic Wound Care: 6 Ways To Treat Diabetic Foot Ulcers
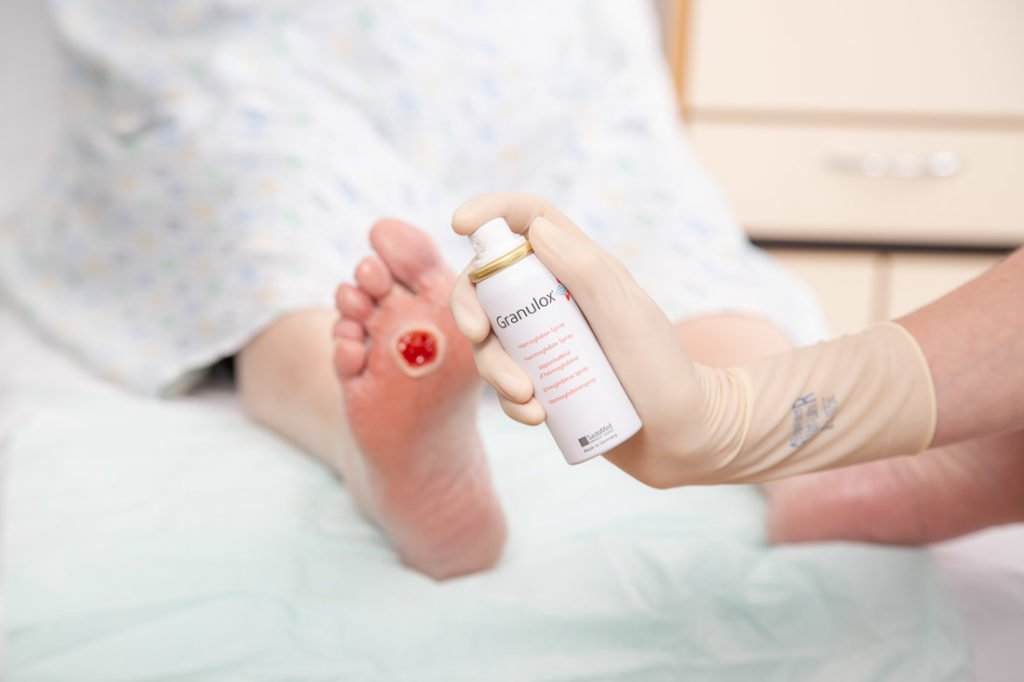
Neuropathic ulcers, often caused by diabetes, are slow to healeven more so as patients age, if they have longer-term diabetes, or if theyre smokers. Other factors that may stall healing include hypertension, hypercholesterolemia, and abnormal blood sugar levels, often associated with diabetes.
Diabetic ulcers typically occur below the ankle at any site of pressure, friction, shear, or trauma. The wound is likely to be round, with margins often characterized by a periwound callus. The presence of diabetes increases the risk for infection.
Treating neuropathic/diabetic ulcers can be challenging, so be sure to take the following steps to simplify the process and help improve outcomes:
Recommended Reading: Does Insulin Cause Erectile Dysfunction
How To Prevent Diabetic Ulcers
For those who are diabetic or who have experienced ulcers in the past, there are some ways to prevent foot ulcers. If a foot wound has occurred due to a diabetic ulcer, there is a risk that it may return.