Whats Next For Research
Currently, the cell infusion treatment requires cells that are within a class of immunosuppressants that depress the immune system, said professor Douglas Melton, whose lab pioneered the science behind the therapy, per The Harvard Gazette
Without the immunosuppressants, these cells would be rejected by the body. We want to find a way to make cells by genetic engineering that are not recognized as foreign, he said.
- Melton sees this as a solvable problem When a woman has a baby, that baby has two sets of genes. It has genes from the egg, from the mother, which would be recognized as self, but it also has genes from the father, which would be non-self. Why does the mothers body not reject the fetus? If we can figure that out, it will help inform our thinking about what genes to change in our stem cell-derived islets so that they could go into any person, he said.
A Clinical Trial With ‘unprecedented’ Results
Vertex Pharmaceuticals last month released the results of an early-stage clinical trial for a stem cell replacement therapy, called VX-880. It is designed to treat people with severe Type 1 diabetes, a disease that occurs when the body’s immune system breaks down the pancreas’s insulin-producing islet cells. The therapy does not aim to treat people with Type 2 diabetes.
According to the New York Times,VX-880 has been in development for decades by Doug Melton, a Harvard University biologist who set out to find a cure for Type 1 diabetes after his infant son and teenage daughter were diagnosed with the disease. The disease, which is lethal without insulin injections, can currently be “cure” only with a transplant of the pancreas or islet cells, the Times reportsbut an organ shortage makes that treatment impossible for most with the disease.
According to a Vertex press release, an ongoing trial for VX-880 will enroll approximately 17 participants and last for five years. However, early, unpublished data on the trial’s first patient suggests that it may “cur” the disease, the Times reports.
“It’s a whole new life,” Shelton said. “It’s like a miracle.”
Who Could Get The Treatment
Peter Senior, MBBS, PhD, director at the Alberta Diabetes Institute, told Verywell that most stem cell-based treatments have been focused on people with severe forms of type 1 diabetes because they are the most at-risk for serious, detrimental health outcomes, and have often experienced dangerous blood sugar levels.
According to Senior, these patients have “problems with erratic blood sugars, but that’s not their only problemthey’ve got eye problems and kidney problems and other things like that.”
Stem cell-derived treatment in humans is new, which means that its going to take time to prove long-term benefits. However, the potential for short-term successas in Sheltons caseis being seen already.
If stem cell-derived therapies prove effective over time and researchers can find a way to deliver the treatments without the need for immunosuppressants, Senior said that the candidate pool would open up.
Effectively curing someone of type 1 diabetes before the disease has progressed and caused serious health complications will help improve patients’ overall quality of life.
If I was a parent with a child with type 1 diabetes, I would want a treatment that meant they never had to worry about diabetes, Senior said. But it may take 40 years for us to be able to show those long-term benefits.
You May Like: How Does Diabetes Lead To Renal Failure
How Stem Cells Could Fix Type 1 Diabetes
Encapsulated stem cell-derived islets could shield cells from the immune system.Credit: Ref. 8
Insulin has been one of the most transformative discoveries in medicine. The isolation of this hormone in 1921 made type 1 diabetes a treatable, rather than a terminal, illness. However, there is growing hope that 100 years later, insulin therapy for T1D might be on the brink of obsolescence.
Insulin is crucial to maintaining safe levels of glucose in the blood. It is produced in the pancreas by cells, which continuously detect circulating glucose concentrations and secrete insulin accordingly the higher sugar levels go, the more hormone is released to counteract the increase. In T1D, however, the cells are destroyed by a persons own immune system.
The cause of this autoimmunity, which typically manifests in childhood, is incompletely understood, but the effect is clear: with neither cells nor insulin, circulating sugar levels remain constantly, toxically elevated. This chronic hyperglycaemia damages blood vessels and nerves, leading to an accumulation of ill-health effects and, if untreated, death.
Now, though, a growing number of scientists and physicians are talking about curing T1D. Their focus is not supplying the body with insulin, but rather replacing the cells that make it.
Type 1 Diabetes Cured In Mice Using Stem Cells
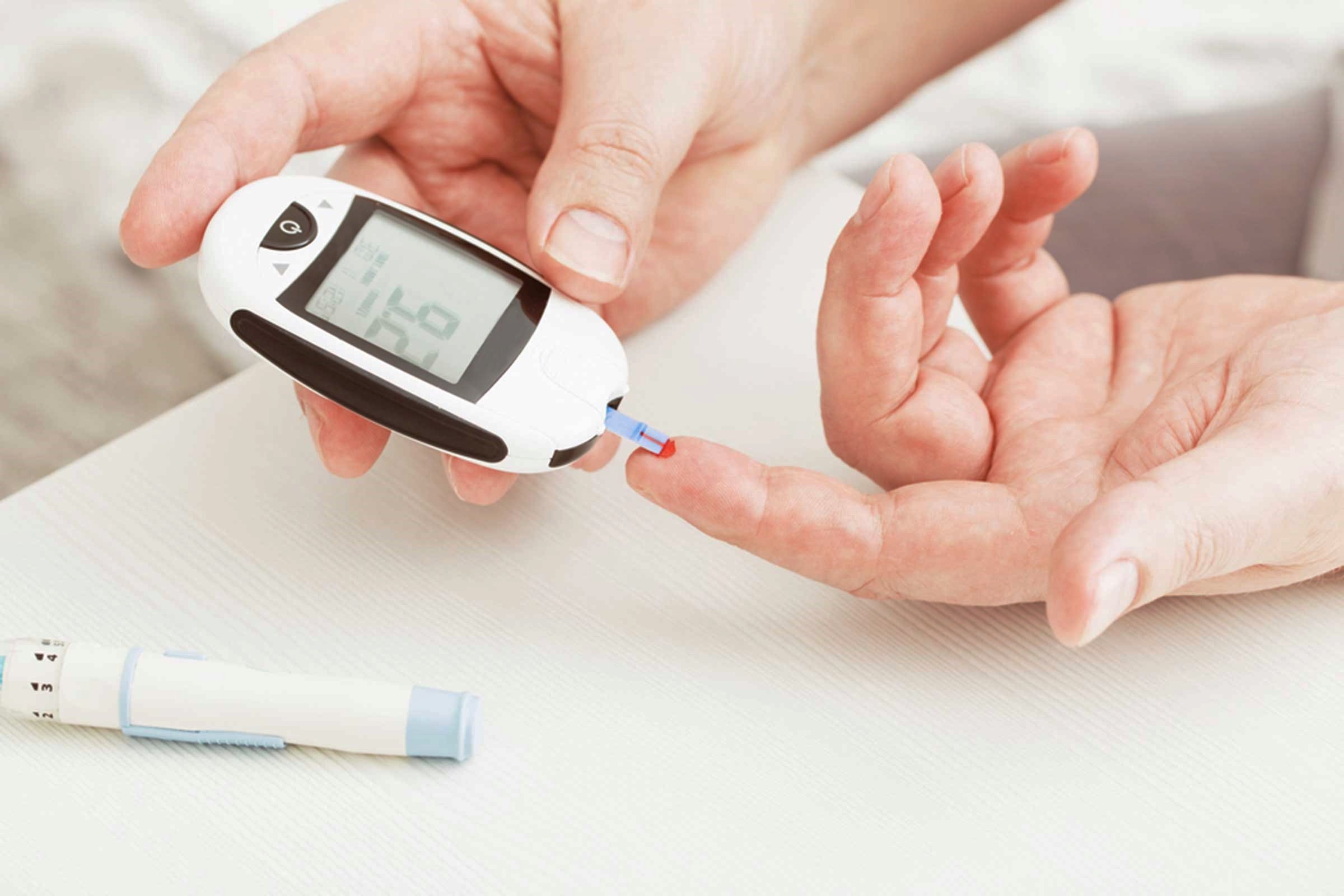
New research uses an innovative technique to convert human stem cells into insulin-producing beta cells much more effectively. The insulin-producing cells created rapidly cured type 1 diabetes in mice, and the benefits lasted for 9 months.
As many as 187,000 children and adolescents in the United States were living with type 1 diabetes in 2018.
An additional 1.4 million people aged over 20 years have the condition and manage it with insulin, according to the same statistics from the Centers for Disease Control and Prevention .
In type 1 diabetes, a faulty autoimmune response causes the immune system to attack and destroy insulin-producing beta cells within the pancreas.
Previous research has pointed to human pluripotent stem cells as a potential therapeutic avenue for type 1 diabetes.
Pluripotent stem cells are an attractive option for researchers from a therapeutic standpoint because they can self-renew in lab cultures and can differentiate into a variety of cell types.
Researchers have previously used hPSCs to create insulin-producing beta cells. However, they were not able to do so effectively enough to cure type 1 diabetes.
Jeffrey R. Millman, Ph.D., an assistant professor of medicine and biomedical engineering at Washington University School of Medicine in St. Louis, is the principal investigator of the new study, which managed to overcome these previous obstacles.
The principal investigator continues to report on the highly significant findings.
Don’t Miss: Non Insulin Injections For Type 2 Diabetes
Political Issues: Ada/jdrf Vs Dr Faustman
Despite Faustmans passion and dedication to finding a cure, both the legitimacy of her work and the results have come under great scrutiny by the American Diabetes Association and the JDRF.
I am still not sure why they chose to issue it, but it was a political not a scientific response to our work, which neither group has funded, said Faustman.
Fortunately for the type 1 diabetes population, Dr. Faustman continues steadfastly on her work towards a cure despite lack of support from the larger diabetes organizations.
Promising Early Results Show That Longstanding Harvard Stem Cell Institute Research May Have Paved The Way For A Breakthrough Treatment Of Type 1 Diabetes Utilizing Research From The Melton Lab Vertex Pharmaceuticals Has Developed Vx
The patient was treated with a single infusion of VX-880 at half the target dose in conjunction with immunosuppressive therapy. The patient, who was diagnosed with T1D 40 years ago and has been dependent on exogenous insulin, achieved successful engraftment and demonstrated rapid and robust improvements in multiple measures. These included increases in fasting and stimulated C-peptide, improvements in glycemic control, including HbA1c, and decreases in exogenous insulin requirement, signifying the restoration of insulin-producing islet cells.
VX-880 is not only a potential breakthrough in the treatment of T1D, it is also one of the very first demonstrations of the practical application of embryonic stem cells, using stem cells that have been differentiated into functional islets to treat a patient, explained Doug Melton, Ph.D., co-director of HSCI, is the Xander University Professor at Harvard and an Investigator of the Howard Hughes Medical Institute. Unlike prior treatments, this innovative therapy gives the patient functional hormone producing cells that control glucose metabolism. This potentially obviates the lifelong need for patients with diabetes to self-inject insulin as the replacement cells provide the patient with the natural factory to make their own insulin, explained Melton.
You May Like: How Can Diabetes Be Managed
What Is Type 1 Diabetes
According to the Centers for Disease Control and Prevention, for Type 1 diabetes, the pancreas doesnt make enough insulin. Without insulin, blood sugar can build up in the bloodstream, instead of entering cells to be used for energy.
- Type 1 diabetes is less common and diagnosed in children, teens, and young adults, but can develop at any age.
- People suffering from this disease are at high risk for nerve damage, which can lead to amputations, heart disease, stroke, eye problems such as glaucoma and cataracts, and skin infections.
- In 2019, it was the ninth leading cause of death, with 1.5 million deaths that year, according to the World Health Organization.
And In 9 Humans With Type 1 Diabetes
She has tested her research on a total of 9 patients with type 1 diabetes. While none are cured, most experienced significant reductions in insulin needs.
We have a fully enrolled Phase IIb clinical trial underway that will read out in as early as 2022, explains Faustman told DiabetesStrong. Because of the size of our Phase II trial and BCGs known safety profile and its generic drug status, we are hoping to pursue approval coming out of Phase II trial.
Faustman adds that the BCG vaccine has demonstrated a clear and clinically significant response in the primary endpoint for type 1 diabetes trials: a stable and long-term return of blood sugars to the near normal range for over 5 years without hypoglycemia.
- Read more about the clinical trials and potential to participate at Faustman Labs.
Recommended Reading: Does Water And Baking Soda Help Diabetes
Ohio Man Appears To Be First In The World To Be Cured Of Type 1 Diabetes
ELYRIA, Ohio â A northeast Ohio man has a whole new grasp on life while making medical history after the successes of participating in a clinical trial.
What You Need To Know
- An Ohio resident may be the first person to be cured of type 1 diabetes
- The man, who lives in Elyria, participated in a clinical trial through Vertex Pharmaceuticals
- His body now controls its own insulin and blood sugar levels
- The results have amazed experts who are now hopeful for the more than 1.5 million people living with the disease
Type 1 diabetes has controlled Brian Sheltonâs life for more than 40 years.
He was diagnosed at the age of 21. As he aged, the autoimmune disease became harder to control. Heâs what doctors called a brittle diabetic, meaning his blood sugar swings were severe and frequent.
âI was a mail carrier for 30 years, and I would start walking up the street and then by the time I get to the end of the street I would pass out and start seizing right on somebody’s front yard, and I couldn’t get up,â Shelton said. âThat would almost be a daily thing.â
Heâs had an ambulance called for him hundreds of times, and even passed out on his motorcycle and crashed into a wall in 2020. Shelton currently lives with his ex-wife, Cynthia, who goes by Cindy.
Stimulating Younger Generations To Have A Proper Nutrition Plan
One of the most important studies related to diabetes is that the main factor that is causing it lies in the nutrition of people, especially younger generations. The main cause of type 2 diabetes is fast food, processed meat, and sugar in beverages. The lack of psychical activity can have negative effects as well. In that matter, the best way to prevent diabetes is to teach children to have a healthier diet and to exercise more.
You May Like: Chromium Picolinate Dosage For Diabetes
How The New Therapy Is Different
The new treatment is designed to help patients with type 1 diabetes preserve the function of their insulin-producing beta cells for as long as possible. As von Herrath explains, people with type 1 diabetes need to take insulin because they “experience a progressive loss of their own insulin production by pancreatic beta cells, due to an autoimmune attack on beta cells.”
People with the condition need to be vigilant about their health, which can be difficult. “They never get a break from measuring their blood sugar, watching what they eat, and calculating how much insulin they might need,” von Herreth says. It has become pretty clear, that preserving someones own beta cells is better than relying on external insulin substitution.
When patients can use what functioning beta cells they have, von Herrath says that it can cause fewer complications and an easier time managing blood sugars.” The goal is for the treatment to be given soon after a patient is diagnosed with type 1 diabetes to preserve function of the still-remaining beta cells,” according to von Herreth.
The Main Contender For A Type 1 Diabetes Cure
While you may see a variety of news articles each year with researchers claiming theyve found a successful cure for type 1 diabetes, the majority fail in animal trial and are never heard from again because they dont pass the early stages of long-term efficacy and safety.
The majority of it is really lined with hope, explainsKristina Figueroa, MSPH, who is an expert in type 1 diabetes clinical research and public health, and a passionate patient advocate.
Like most of us, Figueroa says that after her own type 1 diabetes diagnosis at age 6 in 1996, her healthcare team told her a cure was just around the corner. Due to the half dozen cures of type 1 diabetes in mice each year, it can seem that way.
Weve made huge advances, adds Figueroa, but were still nowhere close.
The researched treatment efforts closest to a successful cure come down to one, maybe two, that have the potential to progress through each critical trial phase.
And hopefully, one day becoming available to all patients with type 1 diabetes.
You May Like: Type 2 Diabetes Dry Mouth
Amid Praise Experts Urge Caution
Although industry experts celebrated the hope that a potential cure could be coming for many of the 1.5 million Americans suffering from Type 1 diabetes, many urged caution due to the early stage of the treatment’s clinical trials, voicing concerns about possible unforeseen side effects and questions about how long the effect of treatment would last.
For instance, some experts have voiced concern over Shelton’s immunosuppression. John Buse, a diabetes expert at the University of North Carolina, said, “We need to carefully evaluate the trade-off between the burdens of diabetes and the potential complications from immunosuppressive medications.”
However, “bottom line, it is an amazing result,” said Irl Hirsch, a diabetes expert at the University of Washington who was not involved in the research. “We’ve been looking for something like this to happen literally for decades.”
Separately, Peter Butler, a diabetes expert at the University of California, Los Angeles who was not involved with the research, agreed that “t is a remarkable result.” He added, “To be able to reverse diabetes by giving them back the cells they are missing is comparable to the miracle when insulin was first available 100 years ago.”
Experts involved in the trial also expressed surprise that such positive results stemmed from only a half dose, the Times reports.
What This Means For You
If you have type 1 diabetes, there could eventually be a new treatment option to help preserve your beta cells, supporting your bodys ability to make insulin on its own. The treatment has only just finished its phase 2 clinical trial, which means it will likely be years yet before it could be available to consumers.
Don’t Miss: Can Diabetics Eat Activia Yogurt
Scientific Research Shows A Possible Diabetes Type 1 Cure
Type1 diabetes patientsdepend on lifelong insulininjection to manage their condition. It is an autoimmune disease that causes theimmune system to wrongly detect beta cells, necessary for insulin production, as foreign bodies. Once Type 1 diabetes develops inyour body, it progresses and destroys the pancreatic insulin-producing cells.
Most Read Nation & World Stories
Melton had been studying frog development but abandoned that work, determined to find a cure for diabetes. He turned to embryonic stem cells, which have the potential to become any cell in the body. His goal was to turn them into islet cells to treat patients.
One problem was the source of the cells they came from unused fertilized eggs from a fertility clinic. But in August 2001, President George W. Bush barred using federal money for research with human embryos. Melton had to sever his stem cell lab from everything else at Harvard. He got private funding from the Howard Hughes Medical Institute, Harvard and philanthropists to set up a completely separate lab with an accountant who kept all its expenses separate, down to the light bulbs.
Over the 20 years it took the lab of 15 or so people to successfully convert stem cells into islet cells, Melton estimates the project cost about $50 million.
Also Check: How Do You Get Type 1 Diabetes
Stem Cell Treatment Offers Potential Cure For Type 1 Diabetes
CEDAR RAPIDS, Iowa – A stem cell treatment is giving hope to the 1.6 million Americans living with Type 1 diabetes. A diagnosis means a lifetime of watching blood sugar levels, managing diet and injections or infusions of insulin. Those who have Type 1 cant produce their own insulin, or manage their bodys blood sugar. It can cause blindness, kidney failure and can be deadly.
This cell treatment injects insulin producing cells into a patients body that help restore the bodys ability to create and regulate insulin. This summer, a 64-year-old man from Ohio became the first person to receive this treatment. And now, his body is controlling its own insulin and blood sugar a promising result for Type 1 patients.
Eastern Iowa JDRF has long supported Dr. Doug Melton, who is behind this treatment. Though its early, JDRF staff say local families are excited about the possibilities. I think theres a a bit of disbelief, you know, weve worked very hard to find cures. And I say thats plural because theres many shots on goal right now to try to cure this very complicated disease, says Iowa Market Director AnnElise Walsh. But hope is a really strong medicine.
Walsh says theres another study that will test a new gene therapy in patients that will start yet this month in Canada. It will not require immuno-suppressing drugs, which is a caveat to the cell treatment.
Most Read