Prescription Drug Coverage For Diabetics
The passage of the Medicare Prescription Drug Improvement and Modernization Act of 2003 represents a major expansion of Medicare’s coverage responsibilities to its beneficiaries . For the first time in its history, Medicare has provided for coverage for prescription drugs, biological products and insulin, including medical supplies associated with injection. The drug coverage plan, named Medicare part D, will be administered either through prescription drug plans or through Medicare Advantage drug plans .
What Is The Average Cost Of Lantus Solostar With Medicare Part D Coverage
Specific costs of Lantus under your Part D plan are likely to vary depending on your location and specific plan. The below table offers insight into the ranges most people can expect to pay for copays and deductibles.
|
Deductible Stage |
Typical Copay Stage |
|
Deductible payments are the payments you need to make for eligible medication before Medicare coverage kicks in. During this phase, you’re responsible for the full cost of treatment. Some Medicare Part D plans have a $0 a month deductible, and as of 2019, the deductible can’t be more than $415 per month. |
Once you’ve met your Medicare drug plan deductible, the initial coverage period commences. During the typical copay stage, you pay a coinsurance percentage or copayment flat fee for eligible prescriptions. As of 2019, you can typically expect to pay between $25 to $484 per month. |
The Number Of Available Ssm Plans Will Depend On Your County
The number of SSM plans that you have access to depends on the county you live in. Hillsborough County in Florida offers the most SSM plans, with 44 plans available. The counties with the fewest SSM plans have 9 different options. We find that half of all counties in the U.S. have at least 13 SSM plans available for enrollment.
The map below displays the number of SSM plans available by county. Scroll over your county to see the number of plans to choose from in your area.
Recommended Reading: What Is A Good Score For Diabetes
How Medicare Part D Covers Diabetes
Medicare Part D is Medicare prescription drug coverage, which is available through either a stand-alone Medicare prescription drug plan or a Medicare Advantage Prescription Drug plan. Because insulin is a prescription drug used to control diabetes, Medicare Part D covers insulin. However, Medicare Part D does not cover insulin for diabetes when it is administered with an insulin pump. In that case, insulin for diabetes may be covered under Medicare Part B as durable medical equipment, as indicated above. Medicare Part D also covers other drugs that can help control diabetes.
If youre diagnosed with diabetes, you will need certain medical supplies to administer the insulin. Supplies may include syringes, needles, alcohol swabs, gauze, and inhaled insulin devices. Medicare Part D covers these medical supplies for diabetes.
Under Medicare Part D, you may pay a coinsurance or copayment as well as a potential Medicare Part D deductible, depending on your Medicare prescription drug plan or Medicare Advantage Prescription Drug plan.
Medicare information is everywhere. What is hard is knowing which information to trust. Because eHealths Medicare related content is compliant with CMS regulations, you can rest assured youre getting accurate information so you can make the right decisions for your coverage. Read more to learn about our Compliance Program.
Find Plans in your area instantly!
How Do Insulin Pumps Work
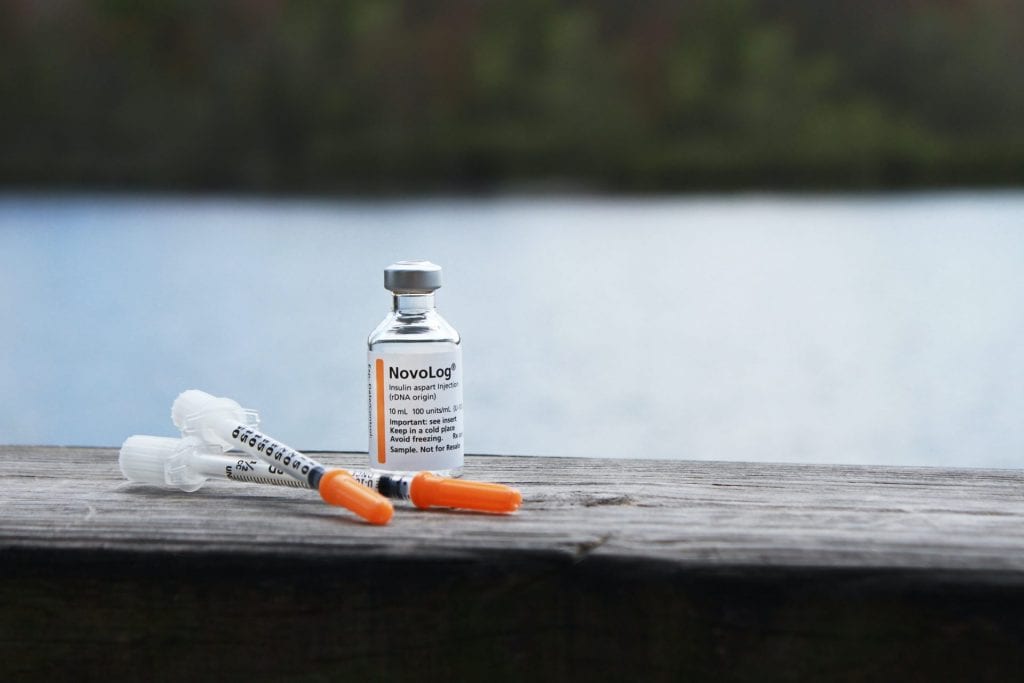
When you have diabetes, your body either doesnt produce insulin or doesnt properly produce it or use it to help keep your blood sugar at an expected level .
As a result, you may need extra insulin to maintain your blood sugar and prevent negative effects, such as nerve damage, that can result from blood sugar thats too high.
Insulin pumps deliver a continuous or sometimes bolus dose of insulin to help you better regulate your blood sugar levels. You wear the pump outside your body, and a portion of the pump transfers insulin from the pump to an insert in your subcutaneous of tissue. In this way, it delivers insulin into your body.
Tubed pumps have a small tube or tubes that extend from the insulin in the pump to deliver the insulin to you. Patch pumps dont have tubes, so that means fewer connections.
Currently only one patch pump, called the Omnipod, is on the market, though several companies are developing other versions. Some Medicare Part D plans cover the Omnipod.
Insulin pumps are a little different from a continuous glucose monitor .
You wear a continuous glucose monitor outside your body, too, but it doesnt necessarily deliver insulin for you. A continuous glucose monitor will tell you what your blood sugar is in real time, so you can know how much insulin you need or if your blood sugar is getting low.
Also Check: Type 1 Vs Type 2 Diabetes Diet
Risks Associated With Lantus
Insulin medication has a number of potential side effects, including hypoglycemia, allergic reaction, low electrolytes, runny nose, fluid retention and weight gain. Low blood sugar, or hypoglycemia, can be life threatening, so it’s extra important to monitor glucose levels when using this drug.
If blood sugar levels fall below 70mg/dL, you should consume 15 grams of carbohydrates and recalculate blood glucose after 15 minutes. Signs of low blood sugar include shakiness, confusion, fatigue, hunger, rapid heart rate and sweating.
Medicare Coverage For Insulin
Unfortunately, Original Medicare doesnt cover much when it comes to insulin. Medicare Part B covers external insulin pumps and insulin if medically necessary. However, Medicare Part B does not cover:
- Insulin
- Insulin pens
- Alcohol swabs
- Gauze
If you require monthly insulin, you will need to enroll in a Medicare prescription drug plan for coverage. Medicare Part D covers all of the above items including insulin and supplies needed to administer the insulin.
Don’t Miss: Type 2 Diabetes Age Range
What Tier Os Lantus Solostar
As of 2019, the majority of Part D plans included insulin medication products such as Lantus in Tier 3. The cost of each prescription in the initial coverage phase was a little less than $50, but this increases significantly for many people. Once the coverage gap phase commences, there’s an additional 25% coinsurance levy. This raises the cost of insulin therapy to over $100 per prescription in out-of-pocket costs, unless you qualify for the low income subsidy .
Do I Automatically Get Part D Senior Savings Model
The savings are not automatic. Its essential to remember that Part D plans are optional, and beneficiaries must actively opt into those plans.
You must select and enroll in the new plans participating in the Part D Senior Savings Model to get these savings. You also need to adhere to the available insulins from participating pharmaceutical companies to receive the price cap otherwise, you may face higher costs if you remain at a different insulin brand. The policy also applies only to people ages 65 and older.
According to the CMS, the average monthly premium for basic Medicare drug plans is $32.09 in 2020, while enhanced plans, which include plans such as those plans that are participating in the Medicare Part D Senior Savings Model, have an average premium of $49.32 a month.
Its important to also note that the Part D Senior Savings Model is a pilot program and subject to changes and adjustments based on the results and success of the program in 2021. CMS has noted that will review how the program performs in 2021 and determine whether any amendments are needed as time goes on.
CMS Administrator Seema Verma also said that: If it goes well, well extend this to other drugs. Were starting with insulin, but depending on the progress, we will consider offering this flexibility to manufacturers and plans with other drugs, depending on the results. We think this creates a foundation and a platform to fix things, some of the problems that we have in the Part D plans.
You May Like: Cerave Moisturizing Cream For Diabetics Dry Skin
What Does Medicare Pay For Diabetes Supplies And Services
In general, Medicare pays 80% and you pay 20% of the Medicare-approved amount for diabetes supplies and services covered by Part B after the yearly deductible is met. Your percentage share of the cost is called coinsurance.
You may pay a coinsurance amount or a copayment for items covered by Part D. What you pay depends on the terms of your specific Part D plan.
Some services, such as medical nutrition therapy and A1C tests, may be provided at no additional cost to you.
Medicare Advantage plans cover diabetes supplies and services, too, and often additional services such as vision, dental and hearing care. The costs and items covered will depend on the specific plan you have.
When it comes to managing diabetes, be sure to review how your Medicare coverage may cover what you need. Also, your annual Medicare Wellness Visit is a great time to talk to your doctor and make sure youre up to date with preventive care services that support your diabetes care.
Medicare Coverage For Insulin And Diabetic Insulin Pumps
Patients with Type 1 and Type 2 diabetes that cannot be treated with diet, exercise or oral medication may have to have insulin injections. Insulin injections can be given via a syringe, a pre-filled injectable device called an insulin pen or by using an insulin pump.
Insulin pumps are a fairly new type of insulin delivery system. Type 1 diabetics who are no longer able to produce insulin at all in their pancreas usually use insulin pumps. The insulin pump is a computerized pump that is connected to a soft needle called a cannula that is permanently inserted under the skin. The pump includes an easy disconnection to the cannula so that the pump can be disconnected for showers and maintenance. The insulin pump then delivers the correct amount of insulin to the patient throughout the day. The patient is able to program the machine to deliver more insulin during meal times and less at night when they are sleeping. Insulin Pumps have been revolutionary for the treatment of severe diabetes. While the cannula is initially uncomfortable once the patient adapts to the sensation the discomfort goes away. The computerized system allows a diabetic to have greater freedom of mobility and negates the constant injections that are part of traditional insulin treatment.
You May Like: Mens Low Cut Diabetic Socks
Medicare Coverage Of Insulin
Under Original Medicare Parts A and B insulin is not covered. You are required to pay 100% of the cost for insulin and insulin pens, in addition to related insulin supplies such as alcohol swabs, insulin needles, syringes, and gauze.
The reason that Original Medicare does not cover insulin and supplies related to its administration is that prescription drugs does not fall under the services covered by hospital insurance or medical insurance, which are the areas Part A and Part B deal with respectively.
Instead, seniors who wish to receive coverage for prescription medications like insulin must enroll in Medicare Part D, also known as a Medicare prescription drug plan, or they must enroll in a Medicare Advantage plan that includes prescription drug benefits.
Medicare Part D Costs For Insulin
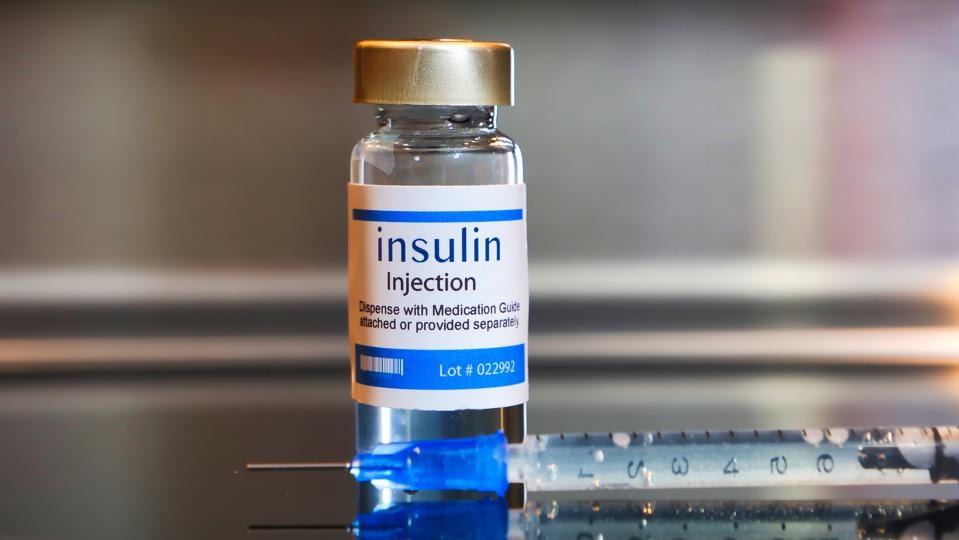
The cost for insulin can vary depending on the Medicare Part D plan you choose and the coverage phase you are in. Typically there are four phases of Medicare Part D Coverage. Your cost for insulin will change depending on the phase you are in. The phases and costs include:
Deductible Phase: You are responsible for 100% of the cost of your insulin until you reach your plan deductible. The standard deductible for a Part D plan is around $445.
Initial Coverage Phase: During this phase, you are responsible for the copay amount for your insulin which is set by your Part D plan carrier. Copays can vary between drug plans. However, Insulin usually lands higher on the tier list and thus requires a larger copay.
Coverage Gap : During the donut hole phase you are responsible for 25% of the cost of your insulin. For example, if your insulin costs $400 a vile you will have to pay around $100.
Catastrophic Coverage: In this phase, you are responsible for about 5% of the cost of your insulin.
Also Check: Type One Diabetes Side Effects
Medicare Coverage For Diabetes Screenings
If you have Medicare and your doctor considers you at risk for diabetes, you may be eligible for up to two blood sugar screenings per year under Medicare Part B you dont pay anything for the screening itself if you use a Medicare-assigned provider at a Medicare-approved facility. However, you may have to pay 20% of the Medicare-approved amount for the visit to the doctors office.
Risk factors that may qualify you for a Medicare-covered diabetes screening include:
- High blood pressure
- High blood sugar levels when fasting
How To Afford Insulin On Medicare
Which plan do you need? | Medicare Part B | Medicare Part D | Medicare insulin costs | How to afford insulin on Medicare
According to the American Diabetes Association, as of 2018, there were 14.3 million seniors age 65 or older with either diagnosed or undiagnosed diabetes. The Centers for Disease Control and Prevention reports that diabetes diagnoses among this age group more than doubled from 2000 to 2010.
With age being a risk factor for developing Type 2 diabetes, many expect to see a trend of higher insulin use among seniorsmainly related to the increase in the senior population. It wasnt until 2006 that Medicare began covering a portion of most prescription drugs, including insulin, for Medicare consumers diagnosed with diabetes. Prior to that, Medicare generally only paid for prescription drugs that were administered in a physicians office or in a hospital or skilled nursing facility.
Recently, in 2021, Medicare rolled out a new insulin saving program for Part D plans called the Senior Savings Model. The new program offers insulin coverage at no more than $35 per month for Medicare Part D consumers with diabetes. These changes will help combat the rising costs of insulin and decrease out-of-pocket expenses for seniors with diabetes.
Don’t Miss: What Is Normal Blood Sugar For Type 2 Diabetes
Other Useful Information On Diabetic Supplies
- Generally, you pay 20% of Medicare-approved amounts for your supplies, and the Medicare Part B deductible applies.
- Make sure you refill your supplies in a timely manner, and only accept supplies you have requested. Medicare wont pay for supplies you didnt order for example, if a supplier automatically sends you items, you cannot get reimbursed by Medicare.
- You may rent or purchase certain diabetic supplies. For more information, call 1-800-MEDICARE . TTY users call 1-877-486-2048. Customer service representatives are available 24 hours a day, seven days a week.
- Ask if the supplier is a participating supplier in the Medicare program before you get durable medical equipment for diabetes. If the supplier is a participating supplier, he or she must accept assignment. If the supplier is enrolled in Medicare but isnt participating, he or she has the option to accept assignment or not. If a DME supplier doesnt accept Medicare assignment, there is no limit to what you can be charged. You also may have to pay the entire bill at the time you get the DME.
- All Medicare-enrolled pharmacies and suppliers must submit claims for diabetic testing supplies. You cant send in the claim yourself.
Dont Miss: When Does Medicare Coverage Start
Get The Insulin Coverage You Need With Clover Health
Are you ready to get better insulin coverage? Find out if your Clover Health plan is participating in the Part D Senior Savings Model. Select Clover Health Medicare Advantage plans will offer Senior Savings Model coverage starting in January 2022.
Call us at 1-800-836-6890 between 8 am and 8 pm local time, 7 days a week* to find out if your plan is participating. You can also contact us by filling out an online form. Let us know the best way to reach you, and we’ll be in touch soon.
You May Like: Is Niacin Good For Diabetes
Early And Comprehensive Provider And Patient Education Regarding Medicare Part D
The introduction of Medicare part D will necessitate greater patient and provider education regarding numerous aspects of the MMA including PDP enrollment, potential credits, PDP characteristics, formularies, and the appeals process for uncovered drugs. Both patients and providers will need to be educated regarding paperwork, guides, and web-based systems introduced to assist Medicare beneficiaries enroll in and compare part D plans. There will be a mass of patients with information needs regarding the Medicare part D benefit and the earlier the provider and patient undertake education initiatives, the more efficient the transition under MMA will be. There are several resources available to both patients and providers . Additional education and implementation efforts must be launched to address the unique needs of certain populations including dual-eligible beneficiaries and minorities. In addition to basic outreach strategies, community-based initiatives involving personal interactions between providers and beneficiaries will be critical.
Medicare Part D And Insulin Coverage
Medicare Part D plans are required to cover injectable insulin. However, external insulin pumps may be covered under Medicare Part B if they are prescribed by a doctor. Medicare Part D coverage includes insulin pens, syringes, needles, alcohol swabs, and gauze.
Now, suppose you want to enroll in a Medicare Advantage plan. In that case, you can enroll in an Advantage plan that includes Part D coverage, but before you make a decision, make sure that the insulin prescribed by your doctor will be covered.
You can also get assistance from the Part D Extra Help Program. If you have full benefits from Extra Help, your copayment for insulin will be lower than usual.
Read Also: Where Is The Best Place To Inject Insulin