My Son Was Born Without Eyes
These include a numbness or pain in the hands or feet, a tingling sensation – similar to pins and needles or pain.
It’s important to note though that there are four different types of neuropathy and that your symptoms will differ depending on the type you are suffering with.
“Usually, symptoms develop gradually. You may not notice anything is wrong until considerable nerve damage has occurred”, experts at the Mayo Clinic said.
Peripheral neuropathy is the most common type of diabetic neuropathy.
This affects the feet and legs first and is often more noticeable at night time.
The key signs of this include: Numbness or reduced ability to feel pain or temperature changes, numbness, tingling, cramps, sensitivity and serious foot problems.
Autonomic neuropathy, is common because diabetes can impact nerves in any area of the body.
Main signs include a lack of awareness that blood sugar levels are low – so not feeling weak or tired when your levels aren’t right.
Wash Your Feet Every Day
Wash your feet with soap in warm, not hot, water. Test the water to make sure it is not too hot. You can use a thermometer or your elbow to test the warmth of the water. Do not soak your feet because your skin will get too dry.
After washing and drying your feet, put talcum powder or cornstarch between your toes. Skin between the toes tends to stay moist. Powder will keep the skin dry to help prevent an infection.
Diabetes: 12 Warning Signs That Appear On Your Skin
Diabetes can affect many parts of your body, including your skin. When diabetes affects the skin, its often a sign that your blood sugar levels are too high. This could mean that:
-
You have undiagnosed diabetes, or pre-diabetes
-
Your treatment for diabetes needs to be adjusted
If you notice any of the following warning signs on your skin, its time to talk with your doctor.
Read Also: Why Do Diabetics Need Insulin
What Should My Blood Sugar Be
Diabetics are urged to monitor their sugar levels and if you’re diabetic it’s likely you will have been given a device so you can do this at home.
You will be told what your average blood sugar level is and this is referred to as your HbA1c level.
While they differ for everyone, the NHS says that if you monitor your levels at home then a normal target is 4 to 7mmol/l before eating and under 8.5 to 9mmol/l 2 hours after a meal.
If it’s tested every few months then a normal HbA1c target is below 48mmol/mol .
Other signs include severe hip and stomach pain, weak and shrinking thigh muscles and difficulty getting out of a sitting position.
Mononeuropathy comes in two different forms and they are cranial and peripheral.
If you have mononeuropathy you might experience double vision, aching behind one eye or numbness or tingling.
Open Sores And Wounds
Having high blood sugar for a long time can lead to poor circulation and nerve damage. You may have developed these if youve had uncontrolled diabetes for a long time.
Poor circulation and nerve damage can make it hard for your body to heal wounds. This is especially true on the feet. These open wounds are called diabetic ulcers.
Diabetes and feet
- Get immediate medical care for an open sore or wound.
- Work with your doctor to better control your diabetes.
Don’t Miss: Protein Bars For Diabetics Low Carb
Keep The Blood Flowing To Your Feet
Try the following tips to improve blood flow to your feet:
- Put your feet up when you are sitting.
- Wiggle your toes for a few minutes throughout the day. Move your ankles up and down and in and out to help blood flow in your feet and legs.
- Do not wear tight socks or elastic stockings. Do not try to hold up loose socks with rubber bands.
- Be more physically active. Choose activities that are easy on your feet, such as walking, dancing, yoga or stretching, swimming, or bike riding.
- Stop smoking.
Smoking can lower the amount of blood flow to your feet. If you smoke, ask for help to stop. You can get help by calling the national quitline at 1-800-QUITNOW or 1-800-784-8669. For tips on quitting, go to SmokeFree.gov.
When Should I Seek Medical Care For Diabetes
If you have diabetes, tell your healthcare provider right away if you experience:
- Any changes in foot shape.
- Any changes to the skin on the feet, including a wound, redness or darkness, warmth or a funny smell.
- Hair loss on your toes, feet or legs.
- Loss of feeling in the toes, feet or legs.
- Pain, tingling, burning or cramping in the feet or legs.
- Thick, yellow toenails.
You May Like: High Glucose Levels In Blood
Don’t Use Your Feet To Test Hot Water
When people with diabetes develop nerve damage, or neuropathy, it can be hard to tell if bath water is too hot. They wont realize they are actually scalding their skin, explains Dr. Tillett. Stepping into a bath before checking the temperature can cause serious damage to your feet, since burns and blisters are open doors to infection. Use your elbow to check the water temperature before getting into the tub or shower.
Heres How To Reduce Your Risk Of Complications With Your Feet
A few lifestyle changes can help keep your feet healthier:
- Dont smokeit more than doubles your risk of amputation
- Control your weight and blood sugars, which reduces your risk of blindness, dialysis and cardiovascular problems, in addition to your risk of amputation
- If youve had diabetic foot wounds in the past, choose non-weightbearing exercise such as riding a stationary bike, swimming in a pool, rowing on a machine or lifting weights
Recommended Reading: Type 1 Diabetes Require Insulin
Quit Smoking To Improve Circulation In Your Feet
The dangers of smoking run from your head to your feet. The chemicals in cigarette smoke damage and constrict your blood vessels, which means that if you smoke, you’re depriving your feet of the nutrient- and oxygen-rich blood that fights infection and keeps them healthy. Diabetic patients already have risk factors that compromise their blood vessels. Its never too late to stop smoking, says Tillett.
Check In With Your Care Team For More Help
Your doctor and your diabetes healthcare team are great sources of information if you need ideas and inspiration for taking care of your feet, quitting smoking, or staying on top of your numbers your weight, blood sugar, and other measures of health, such as blood pressure. Of course, if you notice any changes in your feet that concern you, its a good idea to see your doctor before your next regularly scheduled check-up.
Recommended Reading: Stop Type 2 Diabetes Naturally
Complications Of Charcot Foot
Your bones might break and move out of place as they become weaker. When this happens:
- Your foot may lose its shape. The arch in your foot may fall until the bones are lower than your heel or toes. This is known as rocker bottom by doctors.
- Your toes may curl.
- Your ankle might become twisted and unsteady.
- Bones may press against your shoes. Its important to keep your diabetic foot properly moisturized. Sores can develop on your skin as a result of not doing so.
- Your circulation may be restricted, which makes it more difficult for infections to heal. If this persists for an extended period of time, you may require amputation of your foot.
How To Improve Circulation For People With Diabetes
Suggestions to improve your blood circulation include:
- Control your blood fat levels.
- Keep blood glucose levels as close to normal as possible.
- Dont smoke. Smoking causes spasm and narrowing of blood vessels. Smokers have more heart attacks, strokes and circulation problems than non-smokers.
- Exercise daily. A brisk walk will help keep the blood flowing around your body.
Also Check: Type 1 Diabetes Meal Delivery
When To See Your Doctor
If you experience any of these symptoms, dont wait for your next appointment. See your regular doctor or foot doctor right away:
- Pain in your legs or cramping in your buttocks, thighs, or calves during physical activity.
- Tingling, burning, or pain in your feet.
- Loss of sense of touch or ability to feel heat or cold very well.
- A change in the shape of your feet over time.
- Loss of hair on your toes, feet, and lower legs.
- Dry, cracked skin on your feet.
- A change in the color and temperature of your feet.
- Thickened, yellow toenails.
- Fungus infections such as athletes foot between your toes.
- A blister, sore, ulcer, infected corn, or ingrown toenail.
Most people with diabetes can prevent serious foot complications. Regular care at home and going to all doctors appointments are your best bet for preventing foot problems .
Darker Area Of Skin That Feels Like Velvet
A dark patch of velvety skin on the back of your neck, armpit, groin, or elsewhere could mean that you have too much insulin in your blood. This is often a sign of prediabetes.The medical name for this skin condition is acanthosis nigricans.
Acanthosis Nigricans
Often causing darker skin in the creases of the neck, AN may be the first sign that someone has diabetes.
Take action
- Get tested for diabetes
Also Check: Diabetes How To Control Blood Sugar
What To Do If You Notice A Problem
If you see something wrong, its really important to:
- take the weight off your foot
- contact your GP or foot protection team immediately
- go to your nearest out-of-hours healthcare service if your GP or foot protection team arent available.
Its really important to try and sort it out before it gets any worse – no matter how small the change. A serious foot problem for some people can lead to amputation very quickly.
You may be looked after by many different healthcare professionals, who will tell you what to do next. The important thing to remember is to keep your weight off your foot.
When To See A Doctor
Some diabetes foot complications are life-threatening, or they put you at risk for amputation. See a doctor if you have any concerns or notice unusual changes with your feet.
A seemingly minor issue like cracked skin on your feet, yellow toenails, athletes foot, or an ingrown nail can become a serious problem if left untreated. Also, see your doctor for any cuts or scrapes that dont heal to avoid an infection on your feet.
You May Like: Diabetes Kidney Failure Life Expectancy
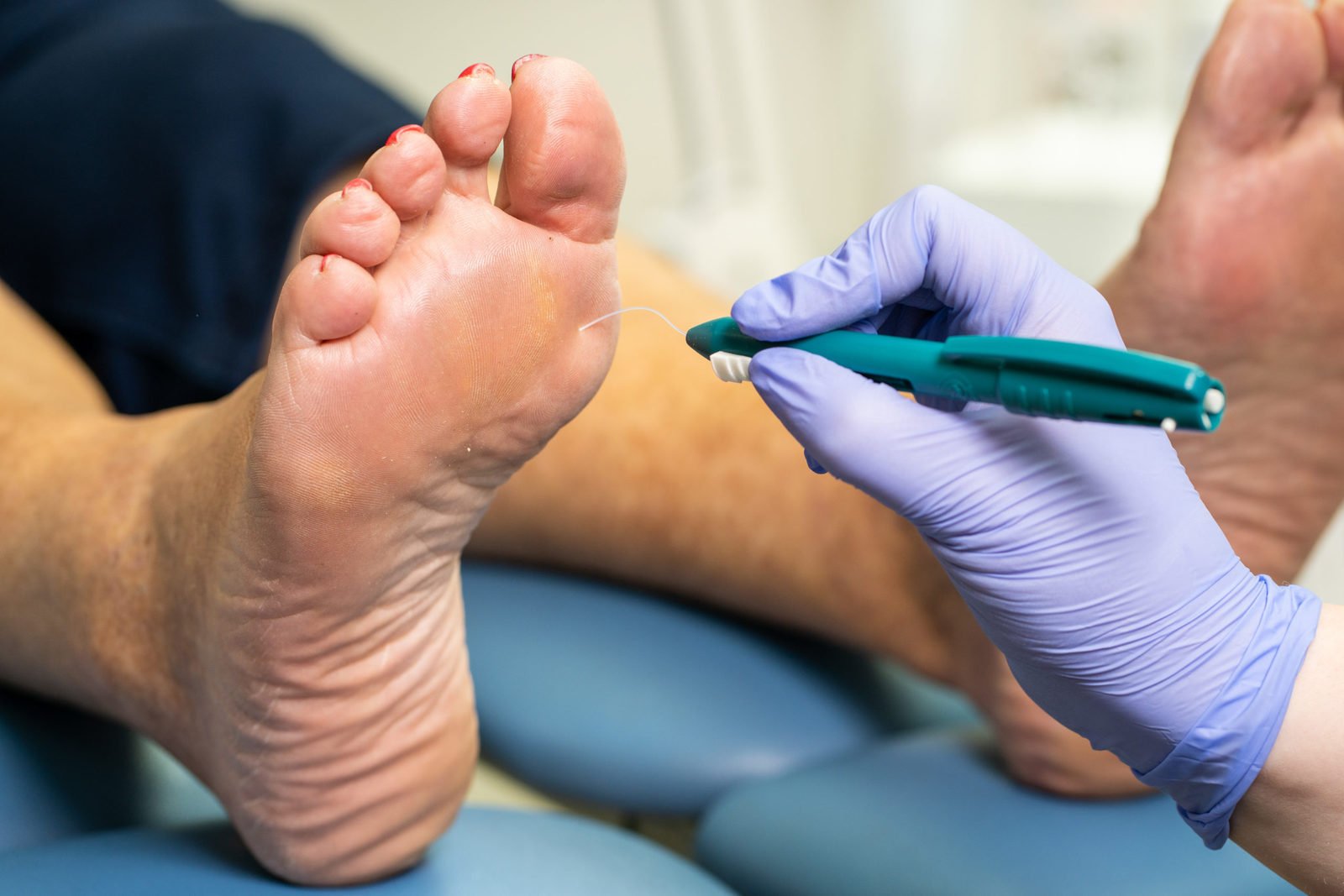
Nerve Supply To The Feet
Nerves are the wiring of the body. They carry messages to your brain from the rest of your body. The nerves to your feet are the most likely to be affected by diabetes.Damaged nerves can cause painful, numb or insensitive feet. Minor cuts, blisters or burns may not be felt and ulcers can develop, which you may not be aware of. Some people with neuropathy experience uncomfortable sensations such as burning, tingling and pain. This is often worse at night.It is important to remember that many people with nerve damage have no symptoms and are unaware of the problem. Nevertheless, they are still at risk of developing ulcers.
How Does Diabetes Affect Your Feet
There are a few words that aptly describe diabetes, namely systemic, chronic, and far-reaching. And the problem has now been called one of the largest healthcare crises of the 21st century, as 10% of the population in the United States has already succumbed to the condition, and this number increases by 5% each year. While diabetes can have a widespread impact on your health, your feet are of particular concern as diabetic neuropathy in your feet is the most common complication, affecting 50% of sufferers.
At City Podiatry, our team of board-certified podiatrists understands the clear and present danger of foot problems among our patients with diabetes. This is why we offer specialized diabetic foot care, allowing our midtown Manhattan patients in New York City to stay one step ahead of their foot health.
Heres a brief look at how diabetes can affect your feet and what we can do to help.
Read Also: Do Type 2 Diabetics Have To Take Insulin
Gangrene And Charcot Foot
Gangrene treatment involves antibiotics to kill bacteria and stop an infection, as well as surgery to remove damaged tissue. Treatment for Charcot foot involves preventing further deformity.
Wearing a cast to immobilize the foot and ankle can gradually strengthen these bones, as does wearing custom shoes or a brace. In severe cases, surgery can help correct a deformity.
Medical History And Physical Examination

Your doctor will talk with you about your symptoms and your overall health. They will want to know:
- How you may have injured your foot.
- About your diabetes, such as your most recent hemoglobin A1C number, and any history of wounds or infections in the foot.
After discussing your symptoms and medical history, your doctor will carefully examine your foot.
- If your foot is warm, red, and swollen, the doctor may elevate the foot to see if these symptoms improve.
- They will look for ulcers or bony prominences that could lead to ulcers.
- They will carefully examine the shape of your foot to look for obvious deformities, and they will try to determine whether the deformities are correctible or rigid.
- They will assess the blood flow and sensation in your foot.
Don’t Miss: What Lab Test For Diabetes
Yellowish Scaly Patches On And Around Your Eyelids
These develop when you have high fat levels in your blood. It can also be a sign that your diabetes is poorly controlled.The medical name for this condition is xanthelasma.
Take action
- Tell your doctor about the yellowish scaly patches around your eyes.
- Talk with your doctor about how to better control your diabetes. Controlling diabetes can clear the scaly patches.
Yellow Reddish Or Brown Patches On Your Skin
Necrobiosis Lipoidica
This skin condition often begins as small raised solid bumps that look like pimples. As it progresses, these bumps turn into patches of swollen and hard skin. The patches can be yellow, reddish, or brown.
You may also notice:
- The surrounding skin has a shiny porcelain-like appearance
- You can see blood vessels
- The skin is itchy and painful
- The skin disease goes through cycles where it is active, inactive, and then active again
necrobiosis lipodica.
Take action
- Get tested for diabetes, if you have not been diagnosed.
- Work with your doctor to better control your diabetes.
- See a dermatologist about your skin. Necorbiosis lipodica is harmless, but it can lead to complications.
Don’t Miss: What Do You Take For Diabetes
What Can I Do To Keep My Feet Healthy
Work with your health care team to make a diabetes self-care plan, which is an action plan for how you will manage your diabetes. Your plan should include foot care. A foot doctor, also called a podiatrist, and other specialists may be part of your health care team.
Include these steps in your foot care plan:
Is It Possible To Prevent Diabetes
Some diabetes foot-related problems can be prevented by taking careful steps to observe and care for your feet. Keeping blood sugar levels under control , and following your recommended diet and exercise program are the best way to prevent all complications of diabetes, including foot problems. In addition to keeping your diabetes under control, you can take steps to care for your feet, including the following:
- Wear comfortable, closed-toe footwear at all times. Special shoes are available for people with bunions or foot deformities if these are necessary. Be sure no objects are trapped inside the shoes that could cut or injure your feet.
- Don’t walk barefoot, even at home. Be sure your feet do not get burned by walking on very hot pavement in summer
- Always wash your feet with warm water and dry them well after washing.
- Check your feet daily for any sores or problems.
- Apply lotion to dry areas, especially heels, but don’t use lotion between the toes. Corns and calluses can be lightly smoothed with a pumice stone. Never use scissors or razors to cut away corns or calluses.
- Trim toenails straight across, and do not cut the corners shorter than the rest of the nail.
- Be sure that your doctor checks your feet at every checkup.
- Stop smoking, if you are a smoker. Smoking further increases the risk of arteriosclerosis and poor circulation to the feet.
You May Like: How Does Diabetes Lead To Renal Failure
What Should I Know About Choosing Shoes And Socks
-
Don’t wear shoes without socks.
-
Don’t wear sandals or other open-toed shoes.
-
Don’t wear high-heeled shoes and shoes with pointed toes.
-
Wear well-padded socks or stockings that are 1/2 inch longer than your longest toe.
-
Don’t wear stretch socks, nylon socks, socks with an elastic band or garter at the top, or socks with inside seams.
-
Don’t wear uncomfortable or tight shoes that rub or cut into your feet. If you’ve had problems before because of shoes that didn’t fit, you may want to be fitted for a custom-molded shoe.
-
Shop for new shoes at the end of the day when your feet are a little swollen. If shoes are comfortable when your feet are swollen, they’ll probably be comfortable all day.
-
Break in new shoes slowly by wearing them for no more than an hour a day for several days.
-
Change socks and shoes every day. Have at least 2 pairs of shoes so you can switch pairs every day.
-
Look inside your shoes every day for things like gravel or torn linings. These things could rub and cause blisters or sores on your feet.
Signs Of Foot Issues With Diabetes
Poor blood circulation and blood flow can slow the healing process of sores on your feet, putting you at risk for serious life-threatening complications.
Even if you havent lost feeling in your feet, bring the following symptoms to your doctors attention. Signs of feet issues include:
You can avoid serious diabetes complications by seeing your doctor and getting treatment early for conditions that affect your feet.
Read Also: Medicaid Coverage For Diabetic Supplies