You’ve Heard That Insulin Causes Blindness And Kidney Failure
Nothing could be further from the truth. High blood glucose cause blindness, kidney failure, and other problems, such as nerve damage that can lead to amputations. But eye, kidney, and nerve damage can be delayed or prevented by good control. Insulin will NOT make your diabetes worse, and it is one of the most natural diabetes treatments available.
Some Treatments Can Cause Side Effects
Different types of medication, surgery, and other treatments can cause side effects. The type and risk of side effects varies, from one treatment to another.
Before you start taking a new medication, talk to your doctor about the potential benefits and risks of using it. Ask them if it can interact with any other medications or supplements that you take. You should also let your doctor know if youre pregnant or breastfeeding, since some medications arent safe for pregnant or breastfeeding people to use.
Surgery can also put you at risk of side effects, such as infection at an incision site. Before you undergo any operation, ask your doctor about the potential benefits and risks. Talk to them about the recovery process, including steps you can take to reduce your risk of postsurgery complications.
If you suspect that youve developed side effects from treatment, contact your doctor. They can help pinpoint the cause of your symptoms. In some cases, they might adjust your treatment plan to help relieve or prevent side effects.
Common Questions About Type 2 Diabetes:
- Can type 2 diabetes go away?
- Will I need to take insulin?
- Do I have to take it forever?
How do you treat type 2 diabetes?
When you have type 2 diabetes, you first need to eat a healthy diet, stay physically active and lose any extra weight. If these lifestyle changes cannot control your blood sugar, you also may need to take pills and other injected medication, including insulin.
Eating a healthy diet, being physically active, and losing any extra weight is the first line of therapy. Diet and exercise is the foundation of all diabetes management because it makes your bodys cells respond better to insulin and lowers blood sugar levels.
If you cannot normalize or control the blood sugars with diet, weight loss and exercise, the next treatment phase is taking medicine either orally or by injection.
Diabetes pills work in different ways some lower insulin resistance, others slow the digestion of food or increase insulin levels in the blood stream. The non-insulin injected medications for type 2 diabetes have a complicated action but basically lower blood glucose after eating. Insulin therapy simply increases insulin in the circulation.
Many people with type 2 diabetes have elevated blood fats and blood pressure, so you may be given medications for these problems as well.
Can type 2 diabetes go away? And if my blood sugar becomes normal, do I still have diabetes?
Will I need to take insulin if I have type 2 diabetes?
Also Check: How To Lower Insulin Resistance
Do Count Your Carbs Before Using Mealtime Insulin
The amount of mealtime insulin you need to inject is based on the number of servings of carbohydrates you plan on eating during a meal. Over time, youll get better at figuring out your carb intake. In the meantime, a dietitian can help you come up with a meal plan that works for you.
There are also several smartphone applications and internet-based calculators available to help you figure out your carb intake and your corresponding insulin dosage.
Hypoglycemia can happen when you take the wrong insulin dose, dont eat enough carbs right after taking your insulin, exercise more than usual, or when youre stressed.
You should take the time to learn the signs and symptoms of hypoglycemia, including:
- tiredness
- seizures
- loss of consciousness
You should also learn how to manage hypoglycemia if it happens to you. For example, you can eat or drink glucose tablets, juice, soda, or hard candies. You should also be extra cautious after vigorous exercise, as it can lower blood sugar for hours after the workout.
Insulin For Type 2 Diabetes
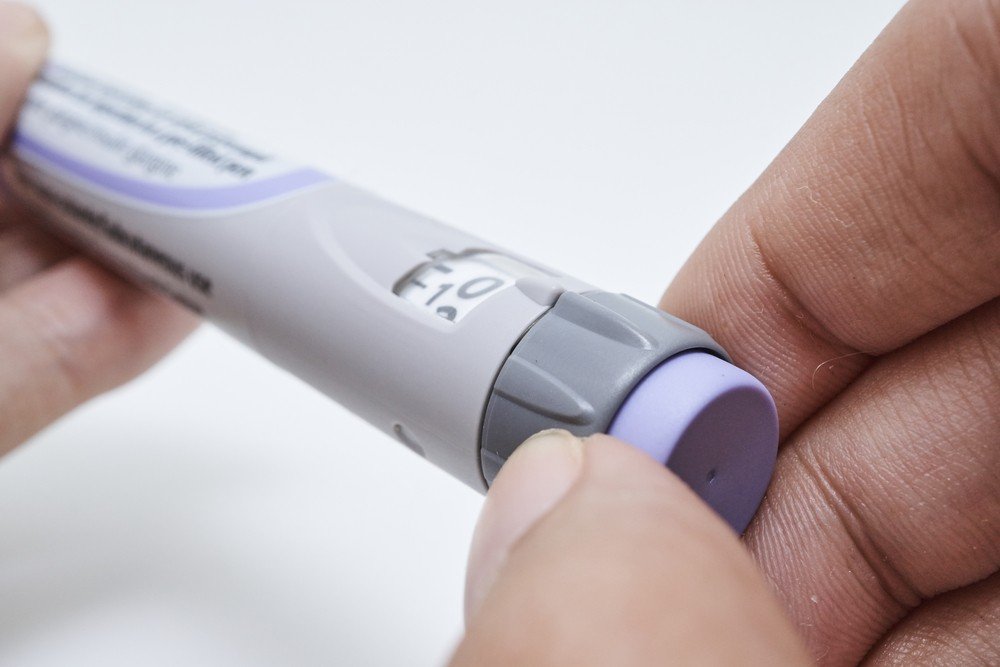
If you have type 2 diabetes and your doctor thinks insulin can help you, it doesnt mean you now have type 1 diabetes. You still have type 2 diabetes, but you’ve changed treatment.
If you have type 2 diabetes, you may not need to use insulin straight away. But some people have very high blood sugar levels when they are first diagnosed. Insulin can be used as a short-term treatment to help quickly bring down your blood sugar levels.
Some people may need to take insulin for a particular reason, like during pregnancy or a severe illness, or after surgery. But you may also need to start it as a treatment if other medications havent helped managed your blood sugar levels or are not appropriate for you.
If you need insulin it isnt your fault and it doesnt mean you havent managed your diabetes well. It’s simply another medication that can help to keep you as healthy as possible. Managing blood sugars effectively is really important in reducing your risk of future diabetes complications and insulin may be the most appropriate treatment choice for you. Many people with type 2 diabetes need to use it as treatment at some point.
Its still important to keep going to your appointments and manage your condition with healthy lifestyle choices. Staying active and eating a healthy diet will reduce the risk of complications from your diabetes.
You May Like: Where Can I Put My Insulin Shot
Travelling With Diabetes Medicines
If you’re going on holiday:
- pack extra medicine speak to your diabetes nurse about how much to take
- carry your medicine in your hand luggage just in case checked-in bags go missing or get damaged
- if you’re flying with a medicine you inject, get a letter from your GP that says you need it to treat diabetes
Page last reviewed: 18 August 2020 Next review due: 18 August 2023
What Is Different About Insulin Lispro
Insulin lispro is a new type of insulin. It starts working sooner than other insulin types. It also reaches peak activity faster and goes away sooner. Insulin lispro helps keep your blood sugar level from going too high after you eat. To keep your blood sugar level steady, your doctor will probably prescribe either a longer-acting insulin or another drug for you to take each day in addition to the insulin lispro.
If you need to mix insulin lispro with a longer-acting insulin, it’s best that you mix insulin lispro only with Humulin U or Humulin N, which are brand names for certain longer-acting insulins. Insulin lispro should always be drawn into the syringe first. This will keep the longer-acting insulin from getting into the insulin lispro bottle.
Types of insulin
Each type of insulin works at a different speed and lasts for a different length of time.
-
Quick-acting, such as insulin lispro , begins to work very quickly and lasts for 3 to 4 hours.
-
Short-acting, such as Regular insulin, starts working within 30 minutes and lasts about 5 to 8 hours.
-
Intermediate-acting, such as NPH or Lente insulin, starts working in 1 to 3 hours and lasts 16 to 24 hours.
-
Long-acting, such as Ultralente insulin, doesn’t start to work for 4 to 6 hours, but lasts 24 to 28 hours.
-
NPH and Regular insulin mixture, two types of insulin mixed together in 1 bottle, starts working in 30 minutes and lasts 16 to 24 hours.
Also Check: Does Diabetes Raise Your Blood Pressure
Newly Diagnosed With Type 2 Diabetes
Knowing where to get started following a type 2 diagnosis can be a challenge. You may feel overwhelmed, but its important to know there isnt a one-size fits all approach to managing the condition.
As well as using the information on this page to understand your condition, you can meet other people with type 2 diabetes in our Learning Zone. Youll hear advice from others in your position, and get practical tools to help you feel more confident managing your condition.
What Are The Symptoms Of Type 2 Diabetes
Symptoms of Type 2 diabetes tend to develop slowly over time. They can include:
- Urinary tract infections and bladder infections.
Rarely, Type 2 diabetes leads to a condition called diabetic ketoacidosis . DKA is a life-threatening condition that causes your blood to become acidic. People with Type 1 diabetes are more likely to have DKA.
Read Also: When Is Insulin Prescribed For Type 2 Diabetes
Do Check Your Blood Sugar Regularly And Write Down Each Measurement
Your insulin treatment involves much more than injecting insulin. You need to check your blood sugar level regularly using a blood glucose monitor. The constant need to test your blood sugar can feel like a burden, but its a crucial part of your diabetes care plan.
Blood sugar measurements can change depending on your stress level, how much exercise youre getting, illness, changes in your diet, and even hormonal changes during the month. Major changes could mean that you have to adjust your insulin dose.
Write down each measurement or record it in an app on your phone to show to your doctor. Your doctor needs this information to determine how much insulin is right for you.
Do Rotate The Place Where You Inject Insulin
Try not to inject your insulin in the same exact place on your body every time. This is to prevent a condition called lipodystrophy. In lipodystrophy, the fat under the skin either breaks down or builds up and forms lumps or indentations that can obstruct insulin absorption.
Instead, rotate injection sites. The best places for injecting insulin are your abdomen, front or side of thighs, upper buttocks, and upper arms due to their higher fat content. Each injection should be at least two inches from the previous site. Try not to inject too close to your belly button or into any moles or scars.
For mealtime insulin, its best to consistently use the same part of the body for each meal. For example, you can inject in your stomach prior to breakfast, your thigh prior to lunch, and your arm prior to dinner.
Clean your skin with cotton dipped in alcohol or an alcohol pad before you inject yourself. Wait 20 seconds for the area to dry before you inject. This helps avoid infections.
You should also wash your hands thoroughly with soap and warm water before you handle any needles.
You May Like: What Size Syringe For Insulin
Do I Need To Monitor My Blood Sugar Level
Yes. Monitoring and controlling your blood sugar is key to preventing the complications of diabetes. If you dont already monitor your blood sugar level, you will need to learn how. Checking your blood sugar involves pricking your finger to get a small drop of blood that you put on a test strip. You can read the results yourself or insert the strip into a machine called an electronic glucose meter. The results will tell you whether your blood sugar is in a healthy range. Your doctor will give you additional information about monitoring your blood sugar.
Reasons To Continue Insulin
Although none of these four drug classes cause hypoglycemia, they all have potential side effects and risks to consider. And since beauty and the risk/benefit ratio of any treatment is ultimately in the eye of the beholder, one can reasonably decide to continue with insulin despite deteriorating health or advancing age .
In particular, some people with Type 2 diabetes no longer produce any insulin on their own, and it may be hard to obtain even reasonable blood sugar control without it. And although hypoglycemia is rightly feared, significant and persistent blood sugar elevations are not completely harmless. They can cause dehydration, fatigue, vision change and slow wound healing and increase infection risk.
If older patients do continue with insulin, it’s common practice to stick with a daily, long acting insulin. These carry a lower of risk of hypoglycemia compared to shorter acting insulins, which are designed to quickly capture the carbohydrate load of a meal.
Like a turtle, a diamond cutter or Father Time playing the back nine, slow and smooth wins the day.
Recommended Reading: Can You Join The Airforce With Diabetes
Symptoms Of Type 2 Diabetes
The symptoms of diabetes include feeling very thirsty, passing more urine than usual, and feeling tired all the time.
The symptoms occur because some or all of the glucose stays in your blood and isn’t used as fuel for energy. Your body tries to get rid of the excess glucose in your urine.
The main symptoms of type 2 diabetes are:
- urinating more often than usual, particularly at night
- itchiness around the genital area, or regular bouts of thrush
- cuts or wounds that heal slowly
- blurred vision caused by the lens of the eye becoming dry
The signs and symptoms of type 1 diabetes are usually obvious and develop very quickly, often over a few weeks.
These signs and symptoms aren’t always as obvious, however, and it’s often diagnosed during a routine check-up.
This is because they are often mild and develop gradually over a number of years. This means you may have type 2 diabetes for many years without realising it.
Early diagnosis and treatment for type 2 diabetes is very important as it may reduce your risk of developing complications later on.
Weight Loss Surgery May Be An Option
If your body mass index a measure of weight and height meets the criteria for obesity, your doctor might recommend weight loss surgery to help treat type 2 diabetes. This procedure is also known as metabolic or bariatric surgery. It can help improve your blood sugar levels and lower your risk of diabetic complications.
In a joint statement issued in 2016, multiple diabetes organizations recommended weight loss surgery to treat type 2 diabetes in people with a BMI of 40 or higher. They also recommended weight loss surgery for people who have a BMI of 35 to 39 and a history of unsuccessfully trying to manage their blood sugar with lifestyle and medications.
Your doctor can help you learn if weight loss surgery is an option for you.
Also Check: When Is Insulin Needed For Diabetes
Too Much Insulin Or Not Enough
High morning blood sugar levels before breakfast can be a puzzle. If you haven’t eaten, why did your blood sugar level go up? There are two common reasons for high before-breakfast blood sugar levels. One relates to hormones that are released in the early part of sleep . The other is from taking too little insulin in the evening. To see which one is the cause, set your alarm to self-monitor around 2 or 3 a.m. for several nights and discuss the results with your health care provider.
Monitoring Blood Glucose Levels
If you have type 2 diabetes, your GP or diabetes care team will need to take a reading of your blood glucose level about every two to six months.
This will show how stable your glucose levels have been in the recent past and how well your treatment plan is working.
The HbA1c test is used to measure blood glucose levels over the previous two to three months.
HbA1c is a form of haemoglobin, the chemical that carries oxygen in red blood cells, which also has glucose attached to it.
A high HbA1c level means that your blood glucose level has been consistently high over recent weeks, and your diabetes treatment plan may need to be changed.
Your diabetes care team can help you set a target HbA1c level to aim for. This will usually be less than 53 mmol/mol or individualised as agreed with your diabetes team.
Read more about the HbA1c test
Also Check: At What Blood Sugar Level Should I Take Insulin
Medicines For Type 2 Diabetes
Most people need medicine to control their type 2 diabetes.
Medicine helps keep your blood sugar level as normal as possible to prevent health problems. You may have to take it for the rest of your life.
Diabetes usually gets worse over time, so your medicine or dose may need to change.
Adjusting your diet and being active is usually necessary to keep your blood sugar level down.
How To Know When You’ll Need Insulin
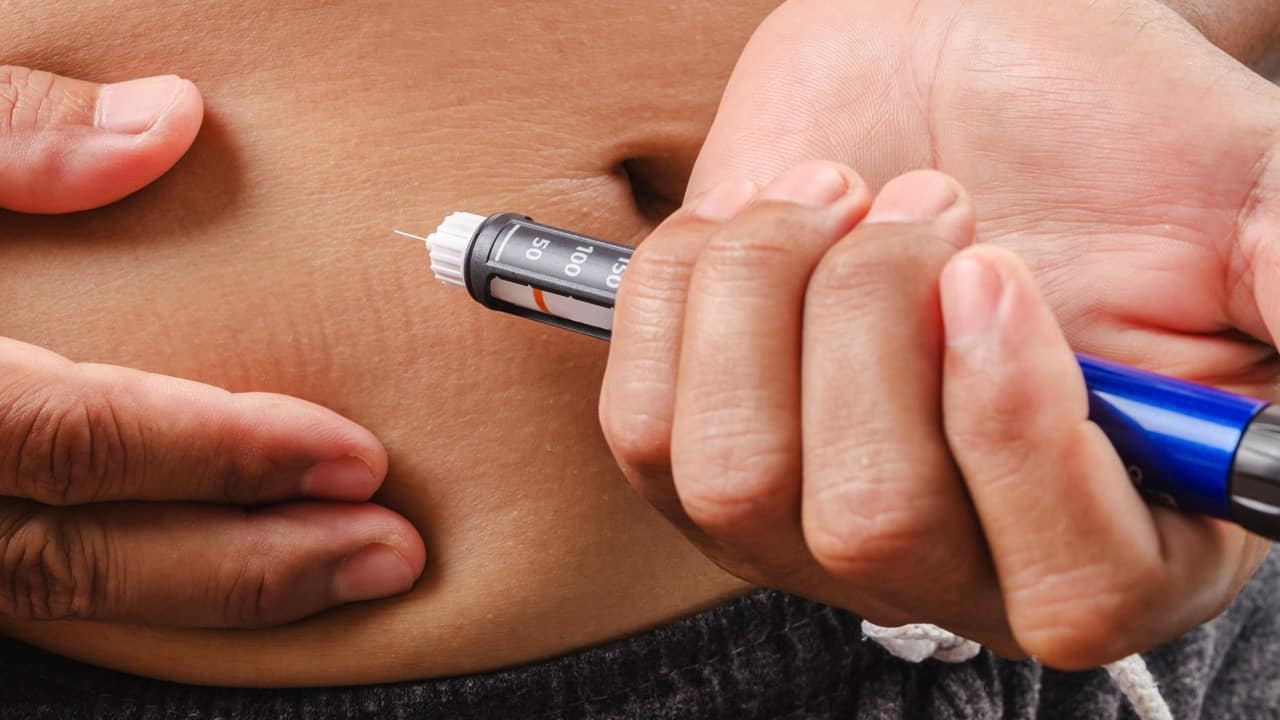
Injecting insulin above and to the side of the belly button can result in more consistent results.
There’s no simple way to tell when a patient with type 2 would do best on insulin, says Richard Hellman, MD, former president of the American Association of Clinical Endocrinologists. But there are guidelines.
“In general if a patient has a hemoglobin A1C that is higher than the agreed upon goal and they are not on insulin, we recommend insulin therapy,” Dr. Hellman says. The American Diabetes Association recommends an A1C of 7% or below, and the American College of Endocrinology and the American Association of Clinical Endocrinologists recommend an A1C of 6.5% or below.
If you can’t lower your A1C with diet, exercise, or other medications, you may need insulin to do the job.
Exceptions to the insulin ruleThere are exceptions, of course. Someone who otherwise seems to be a good candidate for insulin may not be able to manage such a regimen if he or she has limited vision and dexterity and no family support. Good News About Today’s Improved Insulins
If you do need insulin in the short- or long-term, your doctor may prescribe one of four different types. These vary by how quickly or slowly they reach the bloodstream , the amount of time they work at maximum strength , and how long they continue to be effective .
According to the American Diabetes Association , your need for insulin is based on several factors.
Don’t Miss: How To Use Insulin Pump Video