Check Proper Shoe Fit
Purchasing properly fitting shoes is the simplest way to prevent diabetic wounds on your feet. Ill-fitting shoes rub and cause blisters to form, and those blisters quickly lead to diabetic foot ulcers. The right shoes will be tight enough to stop fabric from rubbing against the skin, but loose enough to fit all toes comfortably. Many diabetic patients even choose specialty orthopedic shoes that are custom made to fit the size, shape, and contours of their feet.
What Happens If A Diabetic Gets A Cut On Their Foot
A wound is an injury to the skin or other external part of the body that breaks its surface. A wound may be caused by blunt force trauma, a cut from a sharp object, or pressure. Diabetes can increase your risk for wounds because it affects blood circulation and nerve function in your feet. It also makes you more prone to infection than someone without diabetes. If you get a cut on your foot, elevated protein levels will make your cells vulnerable to forming scar tissue which blocks red and white corpuscles called platelets from joining together to form clots during the healing time.
If a diabetic gets a cut on their foot, it can lead to ulceration that may eventually result in amputation of the limb, when not treated correctly. There wound treatment is very important for people with diabetes.
Diabetic wounds are often very difficult to heal. There are a lot of reasons why they may not heal well, but one common cause is that the person has poor diabetes management including high blood glucose levels and poor blood flow in their feet. This means that even if someone cuts themselves or gets an open wound on their foot, it’s harder for them to get better at healing because there is less blood flowing through the area around the cut or wound site.
What Causes Diabetic Foot Ulcer
People with diabetes have an increased chance of developing foot ulcers because you are more likely than other people to damage the skin on your feet. This is because diabetes can cause nerve damage, so you don’t notice if your foot is injured or sore. Diabetes also causes blood vessel damage so your skin can’t heal easily.
You May Like: What Should Blood Sugar Be At Bedtime For Non Diabetic
How To Treat Ulcers
If you do get an ulcer or notice a change in your skin that youâre not sure about, tell your doctor right away. Youâll likely get a procedure called debridement, which removes unhealthy tissue from the wound to spur healing.
Your doctor will also work with you to try to keep your sore or ulcer from getting infected and becoming bigger. Some of the steps they may recommend include:
Clean your ulcer daily. Use soap and water, unless your doctor recommends another cleanser. Donât use hydrogen peroxide or soak your wound in a bath or whirlpool, because this could reduce healing and may boost your odds of infection.
Keep your ulcer bandaged or covered with a wound dressing. While you may have heard that itâs important to âair outâ wounds, experts now know that not covering a wound actually increases the odds of infection and slows healing.
Keep pressure off your ulcer, especially if itâs on your foot. This may mean you need to use crutches, special footwear, a brace, or other devices. Reducing pressure and irritation helps ulcers heal faster.
Use the topical medications your doctor recommends. These may be saline, growth factors, and/or skin substitutes.
Keep your blood sugar under control. In addition to reducing your risk of ulcers, tight blood sugar control helps your body heal existing ulcers.
Custom Orthotics And Braces
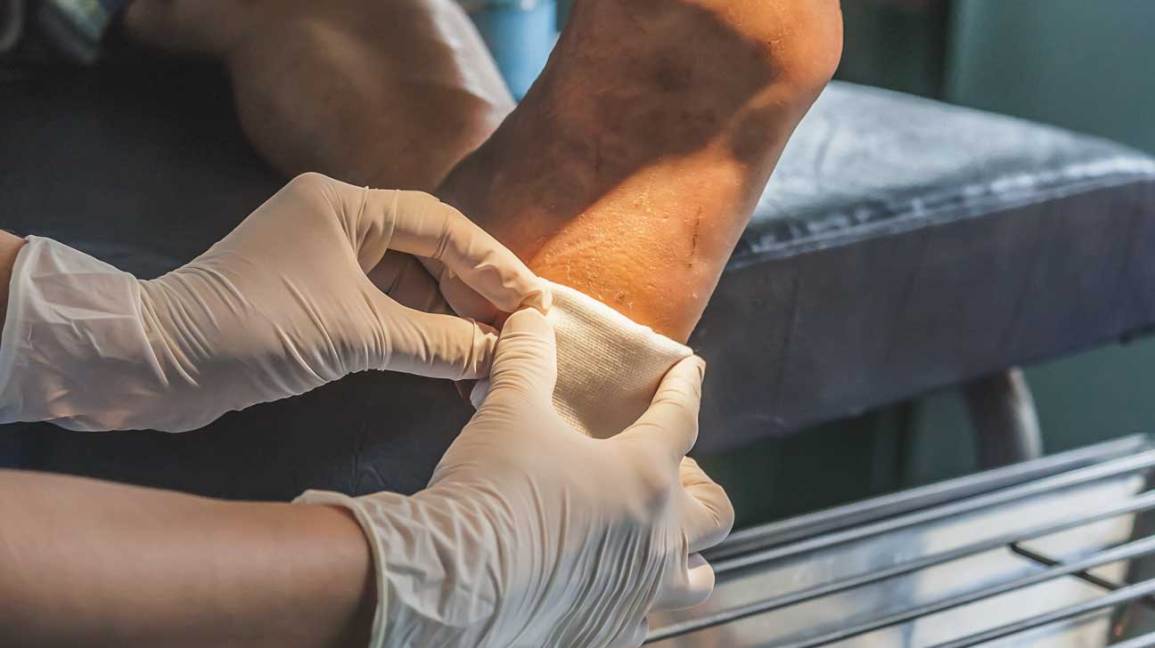
To relieve pressure from an ulcer and help it heal, NYU Langone doctors can provide custom-fit orthotic shoe inserts or braces.
Orthotics, or shoe inserts, help redistribute the weight of your body across the bones and joints of your foot while you walk. These inserts are firm but soft and may contain foam or gel to support your foot and make walking more comfortable.
Our doctors can create inserts with soft, donut-shaped padding to surround and support an ulcer. This helps relieve pressure and protect the ulcer from friction when you wear shoes. A custom shoe insert can also shift weight away from the area of the injury to further relieve pressure and help the ulcer heal.
If your doctor recommends taking more weight off of the affected foot, he or she can provide a custom-fit brace that is worn over the foot and leg. There are many types of braces. One version, called a patellar tendon bearing brace, shifts the weight of the body off of the affected part of the foot and onto the strong tendon in the front of the knee, called the patellar tendon.
Our diabetic foot specialists take a mold of your foot to ensure that the custom orthotic insert or brace fits you well and is comfortable. It takes about two weeks for the device to be made, at which time your doctor schedules an appointment to show you how to use it.
Also Check: What Problems Can Diabetes Cause
Wound Healing Starts With Homeostasis
Immediately after wounding, degranulation of mast cells induces capillary permeability, in addition to vasodilation, increasing bleeding and allowing the influx of immune cells. Furthermore, the coagulation system is activated, and a scab is formed of provisional components . Simultaneously, activated keratinocytes, fibroblasts, and platelets release soluble mediators: growth factors, such as platelet-derived growth factor , epidermal growth factor , and vascular endothelial growth factor chemokines, including IL-8 and CXCL-2 danger-associated molecular patterns such as histones, genomic DNA, adenosine 5-triphosphate , high mobility group box protein 1 and cytokines namely, thymic stromal lymphopoietin , IL-33, and IL-25 . Notably, all of the above-mentioned inflammatory mediators act as danger signals. Consequently, they trigger the infiltration of patrolling inflammatory cells and the induction of local immune responses and subsequent proliferative induction of tissue-resident cells.
When To See Your Doctor
A diabetic wound or ulcer is that health issue which cant be solved by only self-care. Diagnosis and medical observation would be necessary to barricade further complications of diabetes.
Diabetic patients may need a doctor, your Family Doctor or General Practitioner , for every minor change in their body.
Remember, the neuropathic foot is traditionally checked by a podiatrist and perform mono filament, which is a painless procedure. So, if you are diagnosed with a neuropathic foot regular visits to the Podiatrist is a must.
Some of the alarming signs indicating that you need to arrange a visit soon to your Family Doctor are below.
- Numbness in the foot and hands, which means they do not show any or less sensation of pain, touch, tear, and prick.
- Unexpected cuts and wounds and they are mostly less sensitive .
- Unstoppable bleeding in case of open wounds.
- Delayed blood clotting, possibly due to the inefficiency of the blood clotting factors cascade mechanism.
- Delay in the healing process due to blood sugar levels, and possibly due to immune system failure along with the nervous system.
- Lack of sensation due to reduced blood flow to the extreme parts of the body as diabetes thickens the diameter of the blood vessels.
- Redness, and dryness of the skin.
- Open wounds, cuts that are resistant to the healing with open ends.
- Inflammation and pus formations, other discharges in the wounds due to the infections.
- Bruise s, blisters, sores and fissures in the limbs.
Recommended Reading: How To Cure Diabetes 2
How Diabetes Impacts Wound Healing
For individuals with diabetes, all wounds are a serious health concern and require careful attention. Because of diabetic peripheral neuropathy, skin cuts and blisters often go unnoticed until they become more complicated to heal. In addition, internal wounds such as ingrown toenails, skin ulcers, or calluses can cause breakdown of tissue and an increased risk of infection. Even small cuts and insect bites can cause wound healing difficulties in patients with diabetes. Here are common factors of diabetes that impact wound healing:
Leveraging Nanoparticles To Prevent Diabetic Wounds
Even better than faster healing is a wound that never occurs. For that the team is developing another nanoparticle, this one derived from silk.
“You think about silk sutures, they’re strong. They don’t break,” says Dr. Zgheib. “We found this nanosilk solution we make in the lab actually strengthens diabetic skin. The idea is, imagine a spray bottle. You spray it on, give it a minute to dry off, that’s it.”
It’s a kind of invisible armor that could protect skin ulcers of all kinds, from diabetic wounds to pressure injuries in hospitals or nursing homes. It’s also effective, coupled with Dr. Krebs’ gel, for protecting wounds as they heal.
Recommended Reading: Type 2 Diabetes Dry Mouth
Barriers To Wound Healing
- Dead skin dead skin and foreign materials interfere with the healing process.
- Infection an open wound may develop a bacterial infection. The body fights the infection rather than healing the wound.
- Haemorrhage persistent bleeding will keep the wound margins apart.
- Mechanical damage for example, a person who is immobile is at risk of bedsores because of constant pressure and friction.
- Diet poor food choices may deprive the body of the nutrients it needs to heal the wound, such as vitamin C, zinc and protein.
- Medical conditions such as diabetes, anaemia and some vascular diseases that restrict blood flow to the area, or any disorder that hinders the immune system.
- Age wounds tend to take longer to heal in elderly people.
- Medicines certain drugs or treatments used in the management of some medical conditions may interfere with the body’s healing process.
- Smoking cigarette smoking impairs healing and increases the risk of complications.
- Varicose veins restricted blood flow and swelling can lead to skin break down and persistent ulceration.
- Dryness wounds that are exposed to the air are less likely to heal. The various cells involved in healing, such as skin cells and immune cells, need a moist environment.
Why Wound Healing Is Slower In Diabetic Patients
Wounds are more difficult to heal in diabetic patients for some reasons:
- Untreated wounds are infected more easily, and in diabetic peoples body, the immune system is lowered, so that their wounds are more prone to infection.
- Diabetic people have inhibited blood vessels, which cause poorer blood circulation to the wound site.
- Poor blood circulation, which results in fewer nutrients brought into the wound site.
- Diabetic patients might have certain substances deficit, which are required in proper wound healing.
These risk factors inhibit proper wound healing in people with diabetes, making the wound and the entire body more prone to:
- Fungal infectionhappens mostly on the surface of the skin. Fungal infection may initially occurs in a form of blisters and calluses, which left untreated, may be infected by fungus found externally. Fungal infection may cause infection on the skin surface and results in pus-filled surfaces, which heals very slowly.
- Bacterial infectionStaphylococcus bacteria is the most common culprit to cause complication to skin wounds. This bacteria causes the wound to worsen and may complicate other parts of the body.
The risk of slow wound healing in diabetic people can be lowered by:
- Keeping blood glucose levels lower or under good control.
- Performing a good wound care.
- Change the diet into something healthier and lower in cholesterol.
- Exercise well and frequently.
Also Check: How To Know If Your Getting Diabetes
Avoid Sources Of Infection
Its also important to avoid major potential sources of infection, especially public swimming pools and hot tubs. These areas are breeding grounds for bacteria that effortlessly find their way into diabetic wounds and wreak havoc. Even soaking in the bathtub can give bacteria the opportunity to create an infection, so do your best to keep your shoes on and your feet dry.
It Is Very Important To Take Care Off Any Cuts And Injuries That You May Have If You Have Diabetes Read On To Know More
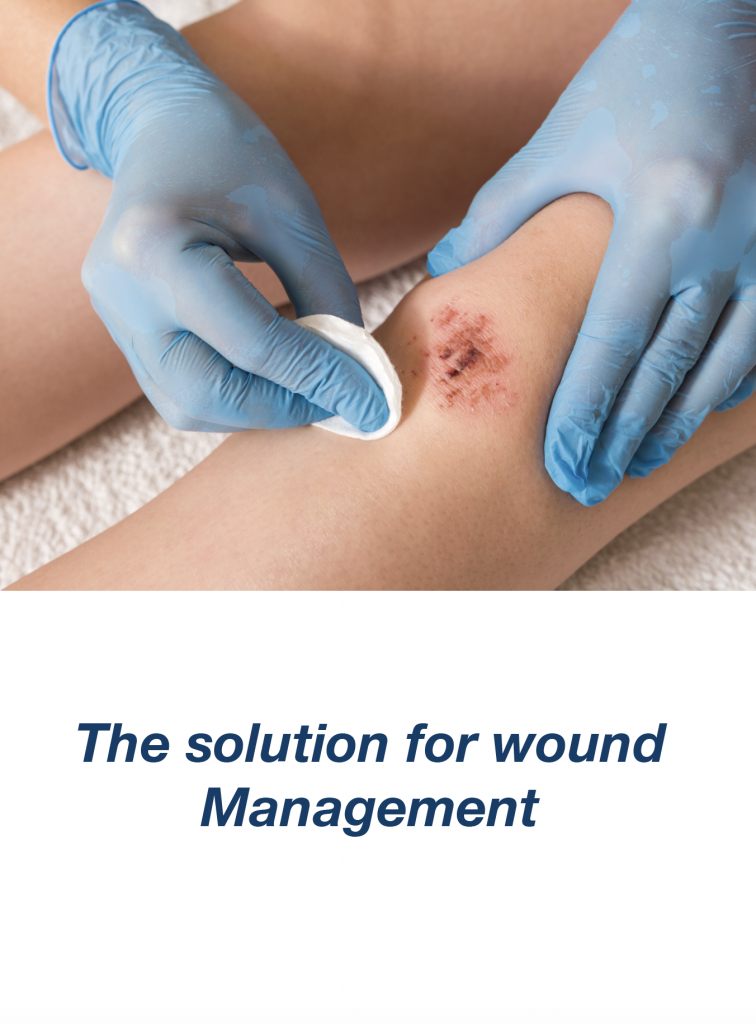
Written by Jahnavi Sarma | Published : May 23, 2020 8:06 PM IST
Cuts and abrasions are a part of life and all of us deal with this on a daily. Most of us don’t even think much of it as minor injuries heal fast and does not even leave a mark. A quick application of first aid and you are done. But the same is not true if you have diabetes. Diabetic wounds fall in a different category altogether.
If you have diabetes, you may have noticed that it takes a long time for wounds to heal. In fact, the higher your blood sugar levels, the more time it takes for wounds to heal. Moreover, because of diabetic neuropathy, you may also not notice injuries on your feet. The numbness on your feet can lead to a false sense of security that everything is all right. It is, therefore, very important to take care off any cuts and injuries that you may have if you have diabetes. Any neglect on your part can lead to unwanted complications that can be easily avoided. Your feet are more at risk. So, you have to take extra care of your feet if you have diabetes.
Recommended Reading: Being Diabetic And Losing Weight
Finding Diabetic Wound Care In The Oakland Area
Yuko Miyazaki, DPM understands treatment for diabetic feet and how it can protect you from serious consequences. Well also explain preventive measures you can take such as lowering blood sugar, increasing your circulation, and reducing friction and pressure from shoes. If you have developed an open sore on your feet, call our office on Colby Street in Berkeley, CA at 647-3744 to set up an appointment. We will evaluate the seriousness of your situation and start the treatment process right away, so your feet will heal and not limit your activity longer than necessary.
Contact Information
Hours:Phone:
Why Is Wound Care Important For People With Diabetes
People with diabetes may be at higher risk of wounds than people who dont have the disease. Also, their wounds tend to heal more slowly and progress more quickly. Wounds that arent treated properly or take a long time to heal can lead to skin breakdown, infections and other complications.
The two main causes of wounds in people with diabetes are:
Recommended Reading: Type 2 Diabetes Would Be Considered An
How Does Diabetes Affect Wound Healing
Diabetic ulcers and chronic wounds are made worse by prolonged periods of heightened blood sugar levels. High blood sugar leads to nerve damage and can impair the function of your blood vessels, thus restricting blood flow to your extremities. This reduction in blood flow leads to slower healing times and a higher risk for infection.
Why Does It Take Longer For Wounds To Heal For Diabetic Patients
April 2, 2016 by woundcaresociety
People with diabetes might notice that they develop wounds easily and these wounds do not easily heal properly, following the common timeline for wound healing. In diabetic person, a tiny wound which is not noticed immediately can be a serious injury eventually. Cuts or blisters develop in diabetic persons body may not heal within days as it would in non-diabetic persons one. Diabetes is an illness which cause major changes in bodys function. One of the well-known effect of diabetes is delayed wound healing. Some diabetic patients are reported to have the feet amputated because of small wound which appeared as blisters initially.
You May Like: Sex And Diabetes Type 2
Keeping Your Feet Healthy
Patients with diabetes must be diligent about wound prevention. The first step is properly managing the diabetes itself which includes maintaining a balanced diet and exercise routine, keeping blood glucose levels in the recommended range, avoiding alcohol and tobacco, and addressing any co-occurring disorder such as cardiovascular disease or obesity.
The next step is to commit to daily skin inspections, and especially your feet when sensation is impaired, Estocado said. This inspection should be thorough, and include the sole, sides and in between the toes. Even the smallest blister or scrape can escalate for diabetic patients, so call your doctor at the first discovery of any abnormality.
Changing The Mechanism Of Healing
The implications of their work plumb deeper than skin. With its dual mechanisms of attack, the conjugate has potential to revise the mechanism of healing all over the body, wherever inflammation exists. Dr. Liechty’s collaborators at the University of Pennsylvania found it can prevent cardiac remodeling after a heart attack. Others showed it can decrease fibrosis and promote lung function. More studies are in the works.
“Hopefully we’ll have this online by the time I have heart disease,” Dr. Liechty says, only half-joking. “It’s really the future.”
Read Also: What Is The Best Thing For Diabetes
Dos And Donts For People With Diabetic Wounds
A checklist of the dos and donts for a person with diabetes is always useful as a guide to making sure you take proper care of your health.
Knowing a little and not knowing a lot, may end up making you still prone to many complexities, especially in case of diabetes wounds.
Things To Do As A Diabetic Patient
Regular Checks
- Check your feet regularly for abscesses, open cuts, sores, blisters, redness, in toe growths, swelling/edema. Do it daily, if not at least weekly.
- Never underestimate an open wound or cut, a bleeding, and delayed clotting. They may free deadlier to cause even amputations.
Blood Glucose Monitoring
- Not only the checks of your legs, but regular Blood Glucose Monitoring is also important.
Doctors for Diabetes Ulcers
- Learn How To Choose The Best Doctors To Treat Diabetes. Make sure to include a Podiatrist, Orthopedics and Skin Specialist in your care team.
- Visit the Podiatrist regularly.
- Be in touch always with your doctors, get your regular regimes done, tingling, bruises, numbness, fungal infections, skin diseases, etc. are nothing to be ignored about.
- And, if required, depending on the severity of your wounds and ulcers, not to forget to visit a Vascular Surgeon too, regularly.
Moisturizing
- When your leg is ulcer free, apply lotion and keep your feet rejuvenated. Moisturizers prevent dryness and itching, cracking of feet and scaling of the skin. Remember, the lotion must not be applied in between the toes with infection as they exaggerate it.
Hygiene
Diet