In The Weeds: Gaps Between Hiv+ And Hiv
While the overall gap in comorbidity-free years between people living with HIV and HIV-negative people was wide, that width varied between comorbiditiesas did the extent to which the gap size changed over time, and the effect of starting HIV treatment with a high CD4 count.
Specifically, three of the six complications exhibited a gap that closed only slightly from the 2000-2003 period to the 2014-2016 period:
- chronic liver disease: 24-year gap in 2014-2016
- chronic kidney disease: 17-year gap
- chronic lung disease: 14-year gap
The other three complications exhibited a gap that had narrowed over time, but was still substantial:
- cancer: 9-year gap in 2014-2016, improving from a 20-year gap in 2000-2003
- average age at onset in 2014-2016 was 80 among HIV-negative people vs. 71 among people living with HIV
- cardiovascular disease: 8-year gap in 2014-2016, improving from an 18-year gap in 2000-2003
- average age at onset in 2014-2016 was 82 among HIV-negative people vs. 74 among people living with HIV
- diabetes: 8-year gap in 2014-2016, improving from a 15-year gap in 2000-2003
- average age at onset in 2014-2016 was 73 among HIV-negative people vs. 65 among people living with HIV
Marcus noted that for just two of the comorbiditiescancer and cardiovascular diseasetreatment initiation at a CD4 count of 500 or higher delayed the average age of incidence and further closed the gap with HIV-negative people.
Growing Older With Hiv
Today, thanks to improvements in the effectiveness of treatment with HIV medicine , people with HIV who are diagnosed early and who get and stay on ART can keep the virus suppressed and live long and healthy lives. For this reason, nearly half of people living with diagnosed HIV in the United States are aged 50 and older. Many of them have been living with HIV for many years others were diagnosed with HIV later in life.
Thats a significant change from the early years of the epidemic when people who were diagnosed with HIV or AIDS could expect to live only 1-2 years after their diagnosis. This meant that the issues of aging were not a major focus for people with HIV disease.
According to the Centers for Disease Control and Prevention , in 2018, over half of people in the United States and dependent areas with diagnosed HIV were aged 50 and older. In addition, people aged 50 and older accounted for 17% of the 37,968 new HIV diagnoses in 2018 in the United States and dependent areas. Though new HIV diagnoses are declining among people aged 50 and older, around 1 in 6 HIV diagnoses in 2018 were in this group.
People over age 50 with HIV make up 46.8% of the over half a million clients served by the Ryan White HIV/AIDS Program . In 2019, 92.2% of clients aged 50 and older receiving RWHAP HIV medical care were virally suppressed, which was higher than the national RWHAP average .
How To Live A Long Life With Diabetes
type 2 diabetes life expectancy Exercise helps control blood sugar and increase life expectancy
The most important thing about living with T2D is its constant management. Proper diabetes management goes a long way. The life of a diabetic person can be improved greatly by making a few simple and daily lifestyle changes.
Recommended Reading: Type 2 Diabetes Can It Be Reversed
Macrovascular Endpoint Preventionadditional Considerations
CVD risk factors should be assessed annually. Routine noninvasive CVD screening in asymptomatic patients, with the exception of annual pedal pulse assessment, is not recommended. Peripheral arterial disease screening includes annual assessment of pedal pulses and consideration of ankle-brachial index testing. Screening for cerebrovascular disease is not recommended .
Strategies To Manage Hyperglycemia
Guidelines for management of diabetes in the OPD set up have been discussed in detail elsewhere. However, these do not focus on HIV-associated diabetes.
Management strategies for diabetes are somewhat different in HIV patients than in the general population. The unique features of diabetes management in HIV are listed and discussed below:
Also Check: 30 Carb Meals For Diabetics
Study Findings: Large Improvements In Lifespan But Large Differences In Comorbidity
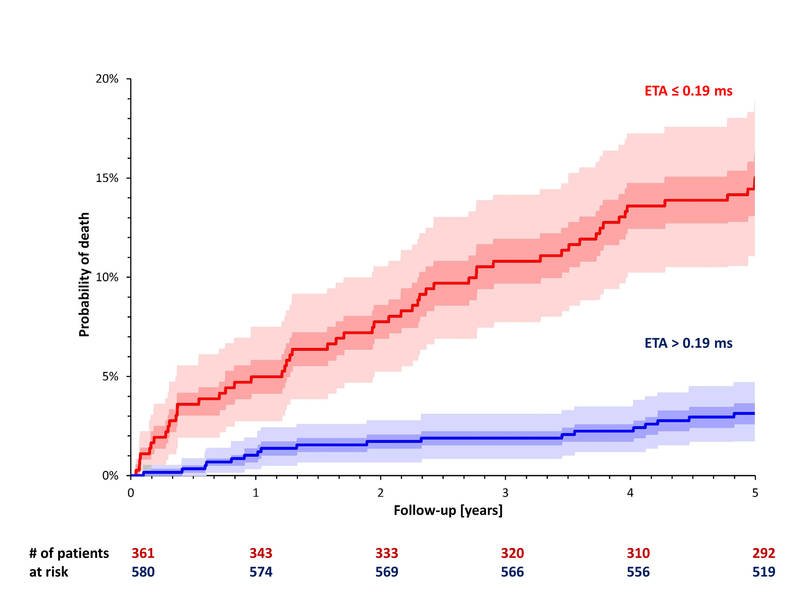
The answer to the life expectancy question was an unambiguous yes: People living with HIV in the U.S. continue to close the lifespan gap with the HIV-negative population. Specifically, within this cohort of people age 21 or older:
-
Overall life expectancy for people living with HIV improved from 71 in the 2008-2010 period to 77 in the 2014-2016 period.
-
By comparison, life expectancy for HIV-negative people was 86 in the 2014-2016 period, shrinking the HIV status lifespan gap to 9 years.
-
Among people who started HIV treatment with a CD4 count of 500 or higher, life expectancy in the 2011-2016 period was 87, compared to 85 for HIV-negative people.
-
In the 2011-2016 period, people who started HIV treatment at that higher CD4 count lived an average of 11 years longer relative to the overall HIV-positive cohort.
The answer to the comorbidity question was more complexand more sobering. Marcus et al focused their analyses on six categories of incident health complications:
- cancer
- chronic lung disease
- diabetes
They found that, in the 2014-2016 period, people living with HIV developed their first comorbidity at age 36, on average16 years earlier than HIV-negative people. The 16-year gap was the same in this more recent period as it was in the 2000-2003 period, although the age of first comorbidity incidence increased for both HIV-positive and HIV-negative people in the intervening years.
What Cdc Is Doing In Lesotho
HIV is a leading cause of death and a health threat to millions worldwide. As a key implementer of the U.S. Presidents Emergency Plan for AIDS Relief , CDC works with Lesotho to build a sustainable, high-impact national HIV response program to accelerate progress towards the UNAIDS global targets to control the HIV epidemic.
CDC supports the Ministry of Healths efforts around HIV and tuberculosis treatment, improving health information systems, increasing laboratory capacity, preventing mother-to-child transmission of HIV, and HIV counseling and testing. Additionally, CDC works with the ministry on diagnosis, treatment, and management of TB, multidrug- resistant TB, and HIV/TB co-infection. CDC provides technical leadership in building human capacity for HIV/TB treatment programs by supporting training and mentoring for health workers. CDC also supports Lesothos efforts to strengthen surveillance, monitoring and evaluation, and health information systems needed for the national HIV response.
CDC provides technical assistance to implement quality laboratory systems, diagnosis and monitoring tests, and new diagnostic technologies. In partnership with implementing partners, CDC provides technical expertise in developing local capacity for effective coordination of laboratory programs to improve service quality.
- Life expectancy at birth: F 56/M 52 years
- Infant mortality rate: 59/1,000 live births
You May Like: What Number Is Too High For Diabetes
Why There Is An Increased Risk
One reason more people have HIV and diabetes now is that better diagnosis and treatment of HIV means that people with this infection are living longer today. As people with HIV live longer, more of them are getting diabetes for the same reasons other people do. Some estimates show that on average, people treated for HIV early can live nearly as long as people without HIV.
But some things make diabetes more likely for people with HIV.
High blood sugar is a side effect of some medicines that treat HIV. Doctors call high blood sugar hyperglycemia. Though people with uncontrolled diabetes also have high blood sugar, you can have high blood sugar without having diabetes. But people taking some of these medicines may be at greater risk for both hyperglycemia and diabetes. Newer HIV medicines donât seem to come with the same risk.
Some medicines used to treat HIV may cause people to gain weight. Because weight gain increases the risk for diabetes, this may put people with HIV at more risk.
Many people with HIV have also have a hepatitis C infection. Hepatitis C has been linked to diabetes.
People with HIV have inflammation as a result of the infection. This inflammation may play a role in the development of diabetes.
Study Setting And Participants
This was a longitudinal comparison study using multisite national HIV cohort data from the Centers for AIDS Research Network of Integrated Clinical Systems . The data are from CNICS patients over 18 years old who had received cART for over six months and had visited at least one of the eight CNICS clinics. The clinics are located at Case Western Reserve University, the University of Alabama at Birmingham, University of California San Francisco, the University of Washington, University of California San Diego, Fenway Health/Harvard University, the University of North Carolina at Chapel Hill, and Johns Hopkins University. The data were extracted from the CNICS medical records for people who visited a clinic at least once from 2006 to 2015. Post hoc analysis indicated that a sample size of 183 participants would be sufficient for this study the size of the sample obtained from CNICS was much larger . The study was exempted by the Institutional Review Board at the University of Texas at Austin because the data were de-identified.
You May Like: How Does Diabetes Cause Heart Disease
Oral Anti Diabetic Drugs
OADs are frequently used in patients with T2DM. The patient with coexistent HIV infection, however, poses a special challenge.
This patient is at greater risk of comorbidity such as hepatitis C, tuberculosis or other opportunistic infections. He or she may have severe insulin resistance. The number of concomitant medications is greater, leading to an increased chance of drug interactions. Because of impaired renal and hepatic function, the risk of adverse events and drug toxicity may be higher. Cachexia and impaired appetite may increase the risk of hypoglycemia. Gastrointestinal infections and dysfunction may worsen tolerability of various oral drugs, and alter their absorption .
One should therefore choose an OAD regime in patients with diabetes and HIV with great care .
Metformin is the first line drug of choice in most persons with T2DM, but should be used with caution in HIV.
Though it improves insulin sensitivity, it may not be well tolerated by cachexic patients. Metformin is more likely to cause diarrhea than other drugs
It is contraindicated in renal or hepatic dysfunction, and may lead to metformin-associated lactic acidosis . It should be avoided in combination with drugs such as stavudine, which also increase the risk of lactic acidosis. Abacavir, lamivudine and tenofovir are the least likely drugs to cause elevation of lactate levels.
Epidemiology Of Dm In Hiv
The prevalence of DM in HIV-infected patients has been reported to range from 2% to 14% and varies by the composition of the cohort studied, how DM diagnosis is ascertained, and how DM risk factors are accounted for in the analysis . There is conflicting evidence on whether HIV infection is an independent risk factor for DM, with some studies showing increased risk and others showing no independent effect of HIV on DM or showing an inverse effect .
Despite the conflicting evidence on the independent role of HIV in DM, certain factors are clearly associated with DM, including increasing age, obesity, and genetic factors. Other factors influence DM incidence in the general population but are more common in HIV-infected patients: hepatitis C virus infection , use of certain medications , opiate use, and low testosterone . Furthermore, ART-associated lipoatrophy and visceral fat accumulation/lipohypertrophy and HIV-related inflammation are DM risk factors in HIV-infected patients. For additional information regarding etiology of DM in HIV-infected patients, readers are referred to a comprehensive article .
Also Check: Is Coffee Healthy For Diabetics
Uk Doctor: ‘i’d Rather Have Hiv Than Diabetes’
Doctor pens controversial op-ed comparing HIV to diabetes.
World AIDS Day: History of the Epidemic
April 16, 2014 — A U.K. doctor has stirred up controversy after writing an op-ed in the U.K. paper The Spectator where he argued that hed rather have HIV than diabetes.”
Dr. Max Pemberton, author of The Doctor Will See You Now and who works in mental health, wrote the article to highlight how having diabetes, particularly Type 2 diabetes, can be thought of as worse than being HIV-positive, which is now often treated as a chronic, and not necessarily fatal, disease.
The risk of stroke in newly treated type 2 diabetes is more than double that of the general population, Pemberton wrote in his article. To put it starkly, the latest statistics show that because of Haart , HIV now no longer reduces your life expectancy, while having type 2 diabetes typically reduces it by ten years. But this isnt an easy thing to say publicly.
Pemberton highlighted facts such as the life expectancy in the U.K. for those with HIV is only minimally lower.
Porn Star Tests Positive For HIV
However, at least one expert says that Pembertons argument does a disservice to both diabetes and HIV, by arguing that one life-threatening disease is better than another.
My whole point shouldnt be either or. Theyre both important, said Mayer. There may be more people at risk for diabetes , but HIV is transmissible, between people.
How Does Hiv Affect A Person In The Long Term
Though the outlook has gotten much better for those with HIV, there are still some long-term effects that they might experience.
As time passes, people living with HIV may begin to develop certain side effects of treatment or HIV itself.
These may include:
The body may also undergo a shift in how it processes sugars and fats. This can lead to having more fat in certain areas of the body, which can change the bodys shape. However, these physical symptoms are more common with older HIV medications. Newer treatments have far fewer, if any, of these symptoms affecting physical appearance.
If treated poorly or left untreated, HIV infection can develop into stage 3 HIV, or AIDS.
A person develops stage 3 HIV when their immune system is too weak to defend their body against infections. A healthcare provider will likely diagnose stage 3 HIV if the number of certain white blood cells in an HIV-positive persons immune system drops below 200 cells per mL of blood.
Life expectancy is different for every person living with stage 3 HIV. Some people may die within months of this diagnosis, but the majority can live fairly healthy lives with regular antiretroviral therapy.
Read Also: How Much Insulin Should I Take
Facts About Hiv: Life Expectancy And Long
Overview
The outlook for people living with HIV has significantly improved over the past two decades. Many people who are HIV-positive can now live much longer, healthier lives when regularly taking antiretroviral treatment.
Kaiser Permanente researchers found that the life expectancy for people living with HIV and receiving treatment increased significantly from 1996 on. Since that year, new antiretroviral drugs have been developed and added to the existing antiretroviral therapy. This has resulted in a highly effective HIV treatment regimen.
In 1996, the total life expectancy for a 20-year-old person with HIV was 39 years. In 2011, the total life expectancy bumped up to about 70 years.
The survival rate for HIV-positive people has also dramatically improved since the first days of the HIV epidemic. For example,
, a person with undetectable levels of HIV in their blood isnt able to transmit the virus to a partner during sex.
Between 2010 and 2014, the annual number of new HIV infections in the United States fell by
Intensive Therapy Does Not Incur Increased Risk Of Overall Mortality
These results provide reassurance that adoption of 6.5 years of intensive therapy in type 1 diabetes does not incur increased risk of overall mortality, write the authors.
The study is limited by a population sample that is unrepresentative of patients with type 1 diabetes, according to experts from the Joslin Diabetes Center in Boston, MA. A relatively low number of deaths among the participants also makes it difficult to fully associate mortality reduction with intensive treatment.
In an associated editorial, Dr. Michelle Katz and Dr. Lori Laffel of the Joslin Diabetes Center refer to the study as providing strong evidence of improved survival in the 21st century. However, they also state that more needs to be done to improve the life expectancy of patients with type 1 diabetes:
The search for genetic factors and biomarkers related to risk of diabetes complications generally and risk of diabetic nephropathy specifically needs to accelerate. There continues to be inadequate access to advanced diabetes technologies, education and support from health care professionals, and, at times, even family encouragement, which all need to improve.
Read Also: Does One High A1c Mean Diabetes
United Kingdom Prospective Diabetes Study Outcomes Model
The United Kingdom Prospective Diabetes Study Outcomes Model is a computer simulation model for forecasting the likely first occurrence of major diabetes-related complications and death in patients with diagnosed type 2 diabetes a full description of the model has been published elsewhere. The UKPDS model is as a probabilistic discrete-time model with annual cycles based on a system of parametric proportional hazards risk equations that have been estimated from 3642 patients participating in the UKPDS. A summary of the characteristics of the UKPDS patients based on previously published information, is shown in Table .
Parallel Protocols: Treating Diabetes And Hiv/aids
As HIV-positive patients live longer, their risk for developing diabetes has increased along with their lifespans. Treating both of these conditions concurrently is challenging, but as with any other patient, lifestyle modification is a crucial component.
Last year, Max Pemberton, a psychiatrist in the United Kingdoms National Health Service and a regular columnist for a number of publications, wrote an op-ed in The Spectator titled As a doctor, Id rather have HIV than diabetes.
Pemberton makes the case that HIV has become a manageable chronic disease, and people with the disease have about the same life expectancy as healthy people. He writes that HIV is regarded in public health terms in the same category as, for example, type 2 diabetes, but goes on to say that the prognosis for patients with T2D is much worse for those with HIV. The article raised some eyebrows, publicly and in the medical community, with some disagreeing with Pemberton because HIV and T2D are contracted and treated in very different ways.
So for some there is no choice, and that means living with both dangerous diseases, while their physicians must treat both diseases in concert.
Read Also: Do You Need A Prescription To Buy Diabetic Test Strips