Diabetes And Your Feet
Get your feet checked at every health care visit.
If you have diabetes, heres a way to keep standing on your own two feet: check them every dayeven if they feel fineand see your doctor if you have a cut or blister that wont heal.
Theres a lot to manage if you have diabetes: checking your blood sugar, making healthy food, finding time to be active, taking medicines, going to doctors appointments. With all that, your feet might be the last thing on your mind. But daily care is one of the best ways to prevent foot complications.
About half of all people with diabetes have some kind of nerve damage. You can have nerve damage in any part of your body, but nerves in your feet and legs are most often affected. Nerve damage can cause you to lose feeling in your feet.
Circulation In People With Diabetes
Poor blood circulation can affect the blood supply to your feet. When this is reduced, cuts and sores may not heal. An early sign of poor circulation to the feet may be pain or cramps in the backs of your legs when walking.Circulation problems can be caused by hardening or narrowing of arteries as they become clogged up. Common causes include:
- smoking
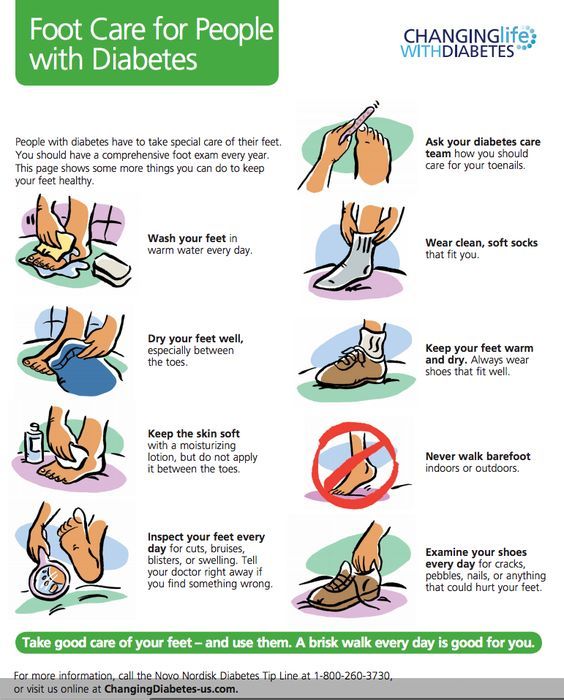
Take Care Of Your Feet
When you have diabetes, caring for your feet is very important in avoiding serious foot complications. Take care of your feet by doing the following:
- Wash your feet thoroughly everyday
- Dry them thoroughly, and dont forget to dry between your toes
- Moisturize your feet, but avoid moisturizing between your toes
- Keep your toenails trim, and use an emery board to file down sharp edges
- Check your feet for sores, cuts, blisters, corns, or redness daily. Let your doctor know if you find any of these.
- Wear moisture-wicking socks
- Before putting your shoes on, check for sharp objects
- Wear shoes that fit well and dont rub your feet
While youre at it, avoid these:
- Dont walk around barefoot
- Dont soak your feet
You May Like: Protein Bars For Diabetics Low Carb
How Does Diabetes Affect Your Feet And Legs
If you’re managing diabetes, you may encounter problems with your feet and legs, two common complications of the disease. Diabetes puts you at higher risk for calluses, corns, bunions, blisters, and ulcers and high blood sugar means these minor injuries and alterations may become gateways to potentially disabling infections.
But you can take several steps to help keep your feet in good shape, including wearing specialized footwear, having regular foot exams, and performing low-impact exercise.
Why does this complication occur in the first place? First, know that high blood sugar levels damage nerves. Researchers arent exactly sure how this damage happens, but they think that blood sugar may have a negative effect on the nervous systems cells and enzymes, according to the Joslin Diabetes Center. These damaged nerves may lead to diabetic neuropathy, a condition in which you lose feeling in your feet or your hands.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, neuropathy occurs in about 70 percent of people with diabetes, and its symptoms can result in harmful infections. After all, if you can’t feel your feet, you won’t be able to notice cuts, sores, or pain. And if you cant feel these irritations and wounds, they may lead to infection, and untreated infections can lead to gangrene, which in turn can require amputation.
Additional reporting by Carlene Bauer
Don’t Use Your Feet To Test Hot Water
When people with diabetes develop nerve damage, or neuropathy, it can be hard to tell if bath water is too hot. They wont realize they are actually scalding their skin, explains Dr. Tillett. Stepping into a bath before checking the temperature can cause serious damage to your feet, since burns and blisters are open doors to infection. Use your elbow to check the water temperature before getting into the tub or shower.
Don’t Miss: Can Diabetes Make You Nauseous
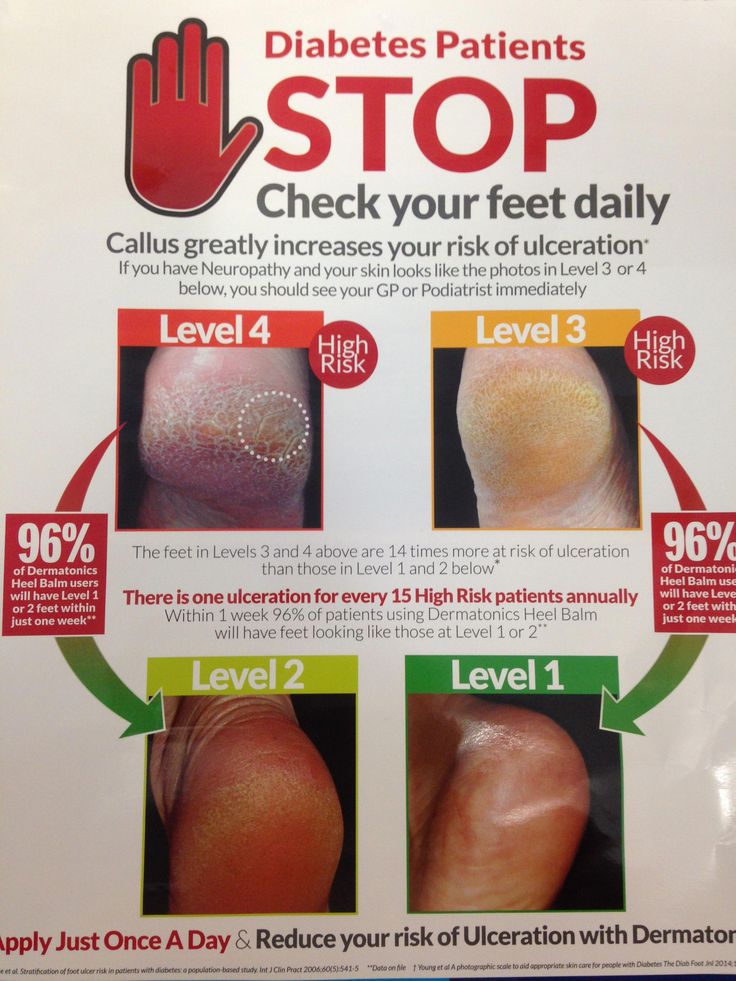
What Is Your Risk Of Developing A Foot Problem
Ask your diabetes health professional if you have very-low, low, moderate, or high-risk feet. Discuss foot checks and how to best look after your feet with them.
How healthy are your feet? Do you know your risk level? Take the Foot Forward foot health quiz to find out.
You have very low-risk feet if you:
- do not have any nerve damage in your feet
- have normal blood flow in or to your feet.
You have low-risk feet if you:
- have reduced blood flow and weak pulses in your feet
- have reduced sensation from nerve damage in your feet
- do not have any changes in the skin or shape of your feet.
You have moderate-risk feet if you:
- have any combination of changes in the shape, reduced blood flow and reduced sensation in your feet.
You have high-risk feet if you have any of the following:
- reduced blood flow and sensation together with a history of foot ulcer, previous lower limb amputation or kidney disease.
How To Avoid Diabetes
For people with diabetes, the smallest blister, bug bite or foot sore could lead to a difficult-to-heal foot infection, a skin ulcer and even the possibility of amputation. Risks are high with diabetes, your lifetime risk for a foot ulcer is 25%.¹And between 9 and 20% of foot ulcers lead to amputations in the US..²
The causes: Nerve damage due to peripheral diabetic neuropathy that can rob you of protective skin sensations plus circulation problems and high blood sugar that can interfere with rapid healing.
That is why diabetes experts recommend that everyone with type 1 or type 2 diabetes protect their feet with daily foot checks, smart choices in socks and shoes, and comprehensive foot exams by a healthcare practitioner at least once a year.
People with diabetes should have feet checked by a doctor once a year or more.
Recommended Reading: Free Insulin For Diabetics Without Insurance
Tips For Everyday Foot Care
Looking after your feet on a daily basis can be tough especially if youve lost any sensation in them. If this is the case, its a good idea to speak to your healthcare team as you may need help from a podiatrist.
Weve put together some everyday tips which should help you keep your feet in check. We’ve also got . You can order a printed version of this leaflet for free from our shop as well.
If you smoke, stop
Most people know that smoking isnt good for you. But when you have diabetes, smoking causes even more problems.
Smoking makes it harder for blood circulation, which is when blood moves around your body, including to your feet. So this puts you at even more of a risk of amputation.
If you think you might need help to stop smoking, take the first step and ask your healthcare team for support.
Manage your blood sugar levels, cholesterol and blood pressure
Keeping your blood sugar within target will help prevent damage to your feet and can stop things getting worse. Easier said than done. Maybe you need help knowing how to eat well and stay active? Or your medication isnt working as well as it could be? Or perhaps it just feels like things are getting on top of you?
We’ve got lots of information to help you manage your blood pressure, cholesterol and know your blood sugar levels.
And there are a number of courses you can go on that can help you manage your diabetes. Speak to a healthcare professional about which course is right for you.
Check your feet every day
How Should A Diabetic Foot Ulcer Be Treated
The primary goal in the treatment of foot ulcers is to obtain healing as soon as possible. The faster the healing of the wound, the less chance for an infection.
There are several key factors in the appropriate treatment of a diabetic foot ulcer:
- Prevention of infection
- Taking the pressure off the area, called off-loading
- Removing dead skin and tissue, called debridement
- Applying medication or dressings to the ulcer
- Managing blood glucose and other health problems
Not all ulcers are infected however, if your podiatric physician diagnoses an infection, a treatment program of antibiotics, wound care, and possibly hospitalization will be necessary.
Preventing Infection
There are several important factors to keep an ulcer from becoming infected:
- Keep blood glucose levels under tight control
- Keep the ulcer clean and bandaged
- Cleanse the wound daily, using a wound dressing or bandage
- Do not walk barefoot
Off-Loading
For optimum healing, ulcers, especially those on the bottom of the foot, must be off-loaded. Patients may be asked to wear special footgear, or a brace, specialized castings, or use a wheelchair or crutches. These devices will reduce the pressure and irritation to the ulcer area and help to speed the healing process.
Applying Medication and Dressings
For a wound to heal there must be adequate circulation to the ulcerated area. Your podiatrist may order evaluation test such as noninvasive studies and or consult a vascular surgeon.
Managing Blood Glucose
You May Like: Does High Glucose Mean Diabetes
Who Can Get A Diabetic Foot Ulcer
Anyone who has diabetes can develop a foot ulcer. Native Americans, African Americans, Hispanics and older men are more likely to develop ulcers. People who use insulin are at a higher risk of developing a foot ulcer, as are patients with diabetes-related kidney, eye, and heart disease. Being overweight and using alcohol and tobacco also play a role in the development of foot ulcers.
Study Design And Subjects
In the current study, having one or two more complications was considered a positive condition. The sample size was determined 375 considering 95% confidence interval with d=0.05 and P=0.58. A total of 375 out of 395 distributed questionnaires were completed and returned the response rate was 94.4%.
Also Check: How Does Diabetes Cause Heart Disease
The Basics Of Foot Complications
Although it can hurt, diabetic nerve damage can also lessen your ability to feel pain, heat, and cold. Loss of feeling often means you may not feel a foot injury. You could have a tack or stone in your shoe and walk on it all day without knowing. You could get a blister and not feel it. You might not notice a foot injury until the skin breaks down and becomes infected.
Nerve damage can also lead to changes in the shape of your feet and toes. If your foot doesnt fit comfortably in regular shoes, ask your doctor about special therapeutic shoes or inserts, rather than forcing your feet and toes into shoes that dont fit and can cause more damage.
Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. This problem is caused by nerve damage that affects your bodys ability to control the oil and moisture in your foot.
After bathing, dry your feet and seal in the remaining moisture with a thin coat of plain petroleum jelly, an unscented hand cream, or other such products. Do not put oils or creams between your toes. The extra moisture can lead to infection. Also, don’t soak your feetthat can dry your skin.
Using a pumice stone every day will help keep calluses under control. It is best to use the pumice stone on wet skin. Put on lotion right after you use the pumice stone.
Wash Your Feet Every Day
Wash your feet with soap in warm, not hot, water. Test the water to make sure it is not too hot. You can use a thermometer or your elbow to test the warmth of the water. Do not soak your feet because your skin will get too dry.
After washing and drying your feet, put talcum powder or cornstarch between your toes. Skin between the toes tends to stay moist. Powder will keep the skin dry to help prevent an infection.
Read Also: Can Diet And Exercise Cure Type 2 Diabetes
The Right Shoes And Socks Matter
Choose shoes wisely. Skip the high heels, flip-flops and going barefoot . Comfortable, supportive shoes that fit well and with dry socks will help protect your feet from damage. Heres what to look for and when to wear your footwear:
Go for comfort. Visit a shoe store where the staff will carefully measure your feet, such as a store that sells comfort shoes or athletic shoes. Have both feet measured and buy shoes that fit your larger foot. Dont buy shoes that youll have to break in. Leather and natural fibers are good choices. Wear shoes all the time except when youre in bed or bathing. . Check your shoes inside and out — every day for problems that could harm your feet such as small pebbles, a torn lining or tacks or nails stuck in the bottom.
Choose foot-friendly socks. Look for socks without seams and that isnt tight. Change your socks once a day, more often if your feet get sweaty. Toss socks with holes in them.
Get a Comprehensive Foot Exam, It is important to visit your health practitioner at least once a week to have your feet checked.
Be sure to take off your shoes and socks when you get into the exam room at your doctors office that will remind both of you that you need a foot check. Your doctor or another healthcare practitioner will look for circulation problems, nerve damage, skin changes, and deformities . He or she will ask you about symptoms, your home care routine and about your shoes and socks, too.
Related
When Should I See My Health Care Provider About Diabetic Foot Problems
Serious foot problems can develop quickly. See your health care provider right away if you notice:
- A cut, blister, or bruise on your feet that doesn’t start to heal in a few days
- Red, warm, or painful skin on your feet
- A callus with dried blood inside
- A foot infection that becomes black and smells bad that could be gangrene
Remember, controlling your blood sugar and caring for your feet every day are the best steps you can take to prevent serious diabetic foot problems.
NIH: National Institute of Diabetes and Digestive and Kidney Diseases
Don’t Miss: What Is Considered Low Blood Sugar For Type 2 Diabetes
Protect Your Feet With Shoes And Socks
Never go barefoot or only in socks. You donât want to step on rocks, tacks, or small pieces of glass that could cut your feet. Always protect your feet with shoes, hard-soled slippers, or similar footwear. Wear shoes/boots that will protect your feet from weather conditions like cold and moisture. Wear slippers at home.
Don’t wear shoes with high heels and pointed toes. Avoid shoes that leave your toes or heels unprotected, like open-toed shoes, flip-flops, or sandals. They leave you vulnerable for injury and infections.
Change your socks daily. Wear natural-fibers: cotton, wool, or a cotton-wool blend. Donât use socks with seams that might rub against your skin and cause blisters. Avoid tight socks.
Try on new footwear with the type of socks you usually wear. Don’t wear new shoes for more than an hour at a time.
Look and feel inside your shoes before putting them on to make sure there’s nothing irritating in them or rough areas.
Wear special shoes if your doctor recommends them. Replace your shoes when they show signs of wear, such as heels that are worn down on one side or lining that is torn.
Wash And Dry Your Feet Daily
Keep your feet clean. But donât soak them for a long time. This can dry your skin.
Use mild soaps and warm water.
Pat your skin dry do not rub. Thoroughly dry your feet.
After washing, put lotion or petroleum jelly on them to prevent cracking. But not between your toes — this can lead to an infection! Sprinkle on a nonmedicated powder before putting on your socks and shoes to help keep your feet dry.
In winter, cold weather and central heating can dry out your skin. Take extra care to moisturize your feet and keep them warm. Wear socks to bed if your feet get cold.
Read Also: What Is High Glucose Levels
Check Your Feet Daily
Neuropathy can cause loss of feeling in your feet. As a result, you may not notice if you get a sore or blister.
Check your feet carefully for any wounds or redness. If you develop a sore, its best to talk to your doctor right away regarding the best treatment. Its easy for an infection to occur when you have neuropathy, so early intervention is key.
What Is A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, and approximately 14 to 24 percent of patients with diabetes who develop a foot ulcer have an amputation. Research, however, has shown that the development of a foot ulcer is preventable.
Read Also: Type 2 Diabetes Glucose Range
Go Easy On Your Feet With Low
People with diabetes benefit from exercise, but what is the best kind? While exercise for diabetes certainly isn’t one-size-fits all, be mindful that many fitness classes and aerobics programs include bouncing, jumping, and leaping, which may not be good for your feet. This is especially true if you have neuropathy. Instead, look into programs, such as walking or swimming, that dont put too much pressure on your feet. Just make sure you have the right shoe for whatever activity you choose.
Why Foot Care Is So Important If You Have Diabetes

Diabetes is a group of conditions that affect how your body uses sugar for fuel. It can also impact different areas of the body, with one of the most common areas impacted being the feet. Diabetics can have problems with nerve damage and blood flow that can harm their feet. The two primary foot conditions that patients with diabetes have are diabetic peripheral neuropathy and peripheral vascular disease.
Recommended Reading: Alternative Medicine For Diabetes Type 1