What Are The Types Of Insulin Injections
There are five types of injectable insulins. Your provider will recommend the most effective type for you based on your lifestyle and your blood sugar levels throughout the day.
Short-acting insulin is a liquid available over-the-counter under different brand names:
OTC insulins use older forms of insulin , while newer prescription insulins better mimic human insulin. You may face different health risks when using these older insulins, so check with your provider first.
Your provider may also prescribe a type of insulin called long-acting insulin along with your regular insulin. Long-acting insulin can help keep your blood sugar controlled for 24 hours.
Is 6 Units Of Insulin A Lot
You may need it if long-acting insulin isnt enough. The right dose depends on your target blood sugar level, how many carbs youre eating, and how active you are. You might start with four to six units of insulin. Your dose may go up two to three units every 3 days until you reach your blood sugar target.
How Much Insulin Is Too Much To Take For High Blood Sugar
Ideally, you should be able to correct your blood sugar with an appropriate insulin dose. How much insulin is too much varies based on how sensitive your body is to insulin.
If you have higher-than-expected blood sugar , you should check your urine for ketones. The presence of ketones suggests your bodys cells are having trouble getting enough glucose. You could be at risk for a serious condition called diabetic ketoacidosis if you have ketones in your urine.
In this instance, you need extra help correcting your blood sugar. You should seek emergency medical attention instead of trying to keep injecting insulin to lower your blood sugar.
Recommended Reading: How Do Glucose Monitors Work
Why Is The Test Performed
Fasting insulin is an important but often overlooked test that can help identify insulin resistance.
Insulin levels are usually out of order long before there are abnormalities in blood sugar levels. Thats why a blood sugar test might come back completely normal even if you are suffering from insulin resistance .
Other than to check for insulin resistance, your doctor may order this test to:
- To help determine the cause of low blood sugar
- Check how your beta cells in the pancreas are working
- To help diagnose an insulin-producing tumor in the pancreas
- To help determine when a person with type 2 diabetes needs to start taking insulin
Not Drinking Enough Water
It’s not just what you eat, but also what you drink or don’t drink that can change the effectiveness of insulin. “Staying hydrated by drinking lots of water helps your kidneys flush out extra sugar floating around in your bloodstream,” Port explains. “It also helps medications like insulin work better, by helping to maintain good blood flow so the medicine can reach the tissues and cells where theyre needed most.” To remind yourself to drink water throughout the day, carry a refillable water bottle around with you. Use it a lot. And skip the sports and performance drinks, says Port, since they usually just give you more sugar.
Recommended Reading: Can Diabetics Eat Hamburger Meat
Example #: Formulas Commonly Used To Create Insulin Dose Recommendations
This example illustrates a method for calculating of your background/basal and bolus doses and estimated daily insulin dose when you need full insulin replacement. Bear in mind, this may be too much insulin if you are newly diagnosed or still making a lot of insulin on your own. And it may be too little if you are very resistant to the action of insulin. Talk to your provider about the best insulin dose for you as this is a general formula and may not meet your individual needs.
The initial calculation of the basal/background and bolus doses requires estimating your total daily insulin dose:
When To Take Insulin
Establishing an insulin routine is important for people with diabetes. It requires diligence on your part as a patient because the doctor can’t monitor you all the time. You’ll need to test your blood sugar regularly to discover how insulin works in your body, how much to take and why you should take insulin before or after meals.
Take too little, and your blood sugar will reach dangerously high levels, causing damage in the long term. Take too much, and your blood sugar will dip too low â a dangerous situation that could lead to coma and even death. Learning to administer insulin using a dosage scale along with regular testing will help ensure that you control the highs and lows.
Regular testing will help you understand how your body reacts to things that influence blood glucose levels. Carbohydrates are one factor, but your blood sugar may be affected, either negatively or positively, by your overall health, stress, exercise, how much sleep you get, how much insulin your body naturally produces, your weight and more.
Exercising and controlling your carb intake and the type of carbs you eat can have a profound effect on your blood sugar levels. When you lower your carb intake, get more exercise and improve your sleeping habits, you are likely to end up needing less insulin.
Read Also: When Is The Best Time To Test Blood Sugar
When Should You Take Insulin
The answer to this question depends on a few things. Most importantly, though, is the type of insulin that you take. For example, fast- or rapid-acting insulins, such as lispro , glulisine , and aspart , are meant to be taken 10 to 15 minutes before eating. The new fast-acting insulin Fiasp is taken right at the start of a meal or within 20 minutes of starting a meal. Fiasp starts to work a couple of minutes after you inject it.
What about other insulins? Heres the rundown:
Regular insulin, which is a short-acting insulin, is generally taken 15 to 30 minutes before your meal.
NPH, an intermediate-acting insulin, is typically given 30 to 60 minutes before a meal or at bedtime.
Long-acting insulins, such as glargine and detemir , are often taken at bedtime, but also in the morning. Because these insulins are considered to be peakless and are types of basal insulin, taking them is not dependent on your meal times. However, its usually recommended that you take long-acting insulins at about the same time each day, give or take an hour.
Your doctor or diabetes educator may suggest that you take your insulin differently in some situations. For example, if you have gastroparesis , you might have better blood glucose results by delaying your injection instead of taking it before you eat.
Evidence From Pharmacokinetic And Pharmacodynamic Studies
Pharmacokinetic studies carried out in people with Type 1 diabetes show that all three rapidacting insulin analogues have similar PK and pharmacodynamic profiles 22, 23. They demonstrate peak plasma insulin concentrations approximately double those of RHI, and a time to maximum concentration less than half that of RHI, with concentrations of the analogues falling more rapidly, returning to levels < 20% of peak concentrations at about 4 h 19, 20, 21.
Pharmacokinetics of bolus insulins. Panels , and are reproduced from Home et al. Diabetes Obes Metab 2012 14: 780788. Panel is reproduced with permission from Andersen et al. EASD 2016 ePoster #931. Panels and are reproduced from Heise et al. Diabetes Obes Metab 2015 17: 682688 25, under a Creative Commons licence. s.c., subcutaneous.
Don’t Miss: What If You Have Diabetes
What Is Different About Insulin Lispro
Insulin lispro is a new type of insulin. It starts working sooner than other insulin types. It also reaches peak activity faster and goes away sooner. Insulin lispro helps keep your blood sugar level from going too high after you eat. To keep your blood sugar level steady, your doctor will probably prescribe either a longer-acting insulin or another drug for you to take each day in addition to the insulin lispro.
If you need to mix insulin lispro with a longer-acting insulin, it’s best that you mix insulin lispro only with Humulin U or Humulin N, which are brand names for certain longer-acting insulins. Insulin lispro should always be drawn into the syringe first. This will keep the longer-acting insulin from getting into the insulin lispro bottle.
How Do I Know How Much Insulin I Need With Each Meal
If you take mealtime insulin, you need to know how much to give with each meal. How do you determine your dose? The latest diabetes eating fashion is to count the carbohydrates, and use an insulin-to-carb ratio to figure out how much rapid-acting insulin to take for the meal you are about to consume
The Insulin-to-Carb Ratio
In order to figure out your approximate insulin-to-carb ratio, take your total daily dose of fast-acting and basal insulin and divide it into 400. For example, 40 units of a total daily dose into 400 would be an insulin to carb ratio of 1:10.
A typical insulin-to-carb ratio for someone with type 1 may be 1:15 . If someone with a ratio of 1:15 is about to eat 90 grams of carbohydrate, the dose of rapid-acting insulin for that meal would be 90/15 or 6 units. This amount would be in addition to a correction dose if the pre-meal glucose level was high or above your goal range.
The Correction Factor
To figure out your correction factor, take your total daily dose and divide it into 1800. Using a total daily dose of 40, 40 into 1800 is 45. That means one unit will drop your blood sugar 45 points. This is also called the sensitivity factor.
Someone with type 2 diabetes may have an insulin-to-carb ratio of 1:10 or even 1:5, and would take 9 or 18 units for a meal with 90g of carb.
The W.A.G Approach
Don’t Miss: Is Coffee Healthy For Diabetics
What Is Blood Glucose Monitoring
People use blood glucose monitoring to regularly test glucose levels in the blood.
It is an essential part of effective diabetes control. Many people with diabetes must check several times each day to plan for activities and meals, as well as scheduling doses of medication or insulin.
A person can test their blood glucose levels with a glucometer. They usually come with lancets, or tiny needles, a logbook to record results, and test strips.
Dont Wait More Than 15 Minutes To Eat After Taking A Mealtime Insulin
Rapid-acting insulins, also known as mealtime insulins, were designed to be taken right before you eat to help control your blood sugar more effectively.
As the name suggests, rapid-acting insulin starts to work rapidly in the bloodstream. If you wait too long to eat, your blood sugar can get too low. This puts you at risk for hypoglycemia.
If you cant eat a meal after youve already taken your mealtime insulin, you should carry around a carbohydrate source to avoid hypoglycemia. These include:
- glucose tablets
Calculating the right dose of mealtime insulin can be complicated at first, especially if you dont know how many carbohydrates youre going to be eating at your next meal.
Try not to panic if you realize you took too much or too little insulin.
If you think youve taken too much insulin, eat some rapidly-absorbed carbs, like juice or glucose tabs. You may also want to contact your doctor.
If youve taken a lot more than you need, like double or triple the correct dose, have a friend or family member get you to a hospital. You may need to be observed for severe low blood sugar.
If you think youve taken too little insulin or forgot to take it at all before your meal, measure your blood sugar. If it gets too high, you may need to take short or rapid-acting insulin as a corrective measure to lower your blood glucose levels. If youre at all unsure about the dose, seek advice from your doctor or diabetes care team.
Also Check: Purpose Of Insulin In The Body
What Type Of Insulin Can Be Given Iv
The only type of insulin that should be given intravenously is human regular insulin. There is no advantage to using rapid-acting analogs in preparing insulin infusions because the rate of absorption is no longer a factor when administering insulin intravenously and can only result in added costs to the institution.
Dont Inject The Insulin Too Deep
Insulin is supposed to be injected into the fat layer under the skin using a short needle. This is referred to as a subcutaneous injection.
If you inject the insulin too deep and it enters your muscle, your body may absorb it too quickly. The insulin might not last very long, and the injection could be very painful.
You May Like: What Is Too High Blood Sugar
Do Count Your Carbs Before Using Mealtime Insulin
Work with your doctor to understand the amount of mealtime insulin you need to inject. This is based on the number of servings of carbohydrates you plan on eating during a meal and your blood sugar prior to eating.
Over time, youll get better at figuring out your carb intake. In the meantime, a dietitian can help you come up with a meal plan that works for you.
There are also several smartphone applications and internet-based calculators available to help you figure out your carb intake and your corresponding insulin dosage.
Hypoglycemia, also known as low blood sugar, can happen when you take the wrong insulin dose, dont eat enough carbs after taking your insulin, exercise more than usual, or feel stressed.
You should take the time to learn the signs and symptoms of hypoglycemia, including:
- being unable to speak or think clearly
- loss of muscle coordination
- visual disturbance, such as blurry vision
- feeling weak, shaky, or lightheaded
You should learn how to manage hypoglycemia if it happens to you. For example, you can eat or drink glucose tablets, juice, soda, or hard candies. You should also be extra cautious after vigorous exercise, as it can lower blood sugar for hours after the workout.
Time To Strike High Blood Glucose
Given the many short- and long-term benefits of post-meal blood glucose control, it is certainly worth the effort to start measuring and evaluating your after-meal control. If your blood glucose levels are higher than they should be, talk with your healthcare team about new or different medical treatments that might help. And take a look at your personal choices in terms of food and activity. Even without a perfectly functioning pancreas, there is still a multitude of options for tackling those high blood glucose spikes!
Disclaimer of Medical Advice: Statements and opinions expressed on this Web site are those of the authors and not necessarily those of the publishers or advertisers. The information, which comes from qualified medical writers, does not constitute medical advice or recommendation of any kind, and you should not rely on any information contained in such posts or comments to replace consultations with your qualified health care professionals to meet your individual needs.
Also Check: How Fast Can Diabetes Develop
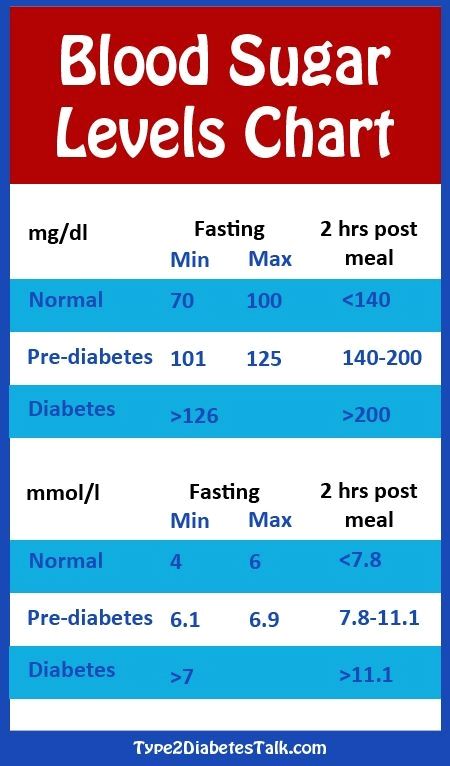
Your Blood Sugar Levels
Everything starts with monitoring your blood sugar levels.
If a patient is taking insulin, they really do need to be checking their blood sugar much more often than when they werent taking insulin, says Joanne Rinker, director of training and technical assistance at The Center for Healthy North Carolina. When theyre prescribed insulin, especially if its short-acting insulin, they should be checking their blood sugar 2 hours after every meal. Because that is the only way for us to know if that was the correct dose.
You dont want your blood sugar going too low or too high . You should stay between 80-130 mg/dL before meals and less than 180 after a meal.
Testing is the only way to know, for sure, where your levels are. Once you know your number at different times of the day â when you get up, before and after meals, or at bedtime, for example â you can start to figure out what to do about it.
Continued
Disadvantages Of Mealtime Insulin
One disadvantage of mealtime insulin is the need to inject yourself with insulin multiple times per day. Talk with a doctor for guidance if this is a challenge in any way. They can help with ways to reduce any discomfort caused by insulin injections.
Mealtime insulin also requires you to keep note of your carbohydrates and adjust your dosage accordingly. This can take a fair amount of patience and practice. A doctor and diabetes care team can give you guidance on how much insulin to take.
Blood glucose testing will be useful to help you learn One side effect of mealtime insulin is potential weight gain. Unplanned weight gain while taking insulin can be managed by working with a healthcare team, such as a doctor, registered dietitian, and exercise physiologist, to come up with a meal and an exercise plan that fit with your lifestyle, ability, and health goals.
Mealtime insulin also comes with other risks. If you take your mealtime insulin but are unable to eat, you could become hypoglycemic, which occurs when your blood glucose levels get too low and can have serious side effects. When your blood glucose is too low, you may feel tired, weak, irritable, and more.
To stop the effects of hypoglycemia, use the 15-15 rule to manage low blood glucose. In other words, have 15 grams of carbohydrates to increase your blood glucose level and check your levels again after 15 minutes.
Also Check: What Does It Mean To Have High Glucose
Whats A Spike And Why Do They Happen
After-meal, or postprandial, spikes are temporary high blood glucose levels that occur soon after eating. It is normal for the level of glucose in the blood to rise a small amount after eating, even in people who do not have diabetes. However, if the rise is too high, it can affect your quality of life today and contribute to serious health problems down the road.