Medical Science And Progress Towards A Cure
Discoveries that may one day contribute to a diabetes cure do occur often, however. Be it better understanding of the immune system or discoveries in the natural world, advancement towards a diabetes cure may one day be possible.
However, at this stage a diabetes cure remains impossible.
Please check the Diabetes News for updates on potential diabetes cures and news of research on similar areas.
However, this isnt the case for all type 2 diabetes patients and needs further research before clear conclusions can be drawn.
Remissions may not be considered a cure, however, but it may mean type 2 diabetes patients can stop taking medication.
How About Pancreas Transplantation
Getting a transplanted pancreas is a possibility for some people with type 1 diabetes. It’s usually done in those who also have end-stage kidney disease.
A pancreatic transplant would help restore blood sugar control. Like anyone else who gets a transplant, the patient would need to take medicine for the rest of their life to help their body accept their new pancreas.
Show Sources
Islet Cell Encapsulation Therapy
In October 2014, the first person with diabetes was implanted with an islet cell encapsulation system, with insulin-producing cells injected into the body and protected from destruction by the immune system.
Further trials are currently in progress to test its safety among participants with type 1 diabetes, with this treatment set to allow patients to produce their own insulin automatically.
Islet cells are derived from stem cells, the foundation for another advancement made by Harvard University, who have used them to create large quantities of insulin-producing beta cells.
The Harvard team have been able to manufacture the millions of beta cells necessary for human transplantatio, and trials could take place within a matter of years.
In the meantime, the need for patients to take immunosuppressive drugs and insulin is unavoidable, but a cure for type 1 diabetes is more within reach than ever before.
Should ongoing trials prove successful in negating insulin dependence, with no side effects or issues with safety, an end to type 1 diabetes could yet be discovered.
You May Like: Diet For Diabetics With Heart Disease
Steglatro Segluromet And Steglujan
As we have seen, patients with type 2 diabetes often need a combination of medications to control their blood sugar.
Pfizer and Mercks new SGLT2 inhibitor Steglatro , as well as two new combination agents that contain ertugliflozin: Segluromet , and Steglujan have been FDA-approved. These are all oral agents used together with diet and exercise to improve blood sugar control in adults with type 2 diabetes mellitus.
In Phase 3 studies for Steglatro approval, Steglatro was studied alone and in combination with metformin and/or sitagliptin, as well as with insulin and a sulfonylurea. Steglatro on top of metformin plus sitagliptin resulted in significant A1C reductions of 0.7% and 0.8% compared with 0.2% for placebo, and weight loss of roughly 6.2 to 6.6 pounds.
Eat Foods With Low Glycemic

Foods which are high in glycemic cause a fast increase in blood sugar level compared to low glycemic foods . The reason behind this is the foods with high glycemic digested and converted to sugar faster than the low glycemic foods.
Low Glycemic foods include:
Foods rich in magnesium include:
- Nuts and seeds
- Green leafy vegetables like spinach and kale
- Seafood etc
Read Also: Fasting For Type 1 Diabetes
What Are The Consequences Of High Blood Sugar
Without taking action, high blood sugar causes severe symptoms, which require dramatic diet and lifestyle changes.
Chronically high blood sugar levels impose significant stress on your internal organs, placing you at risk for cardiovascular issues, “pins and needles” nerve pain, and even progressive vision loss. At this stage, permanent lifestyle changes are required, such as avoiding sugar consumption entirely.
What can we do to protect ourselves from this outcome?
The answer is to improve your body’s natural sensitivity to two key dietary hormones which are essential for healthy blood sugar management.
Is Glucoven Vegan Gluten
Yes, all of the above!
Before formulation, each raw ingredient in the Glucoven formula is thoroughly inspected to ensure that it is non-GMO, vegan, and gluten-free. Next, we use only non-GMO vegetable capsules to deliver the natural ingredients safely and efficiently inside your body. Finally, we test each finished batch of Glucoven again before the bottles are sealed to ensure that the product is definitively non-GMO, vegan, and gluten-free.
Recommended Reading: Is Coffee Healthy For Diabetics
How Might Treatment Evolve
The current standard of care for T2DM consists of screening for elevated HbA1c levels or, in some cases, fasting plasma glucose, with diagnosis followed by management with lifestyle modifications and metformin except where contraindicated . For patients who do not achieve HbA1c targets, antidiabetes medications are added to metformin subsequently, patients are monitored and further oral antidiabetes drugs or insulin are added if needed.
Clearly, the care of patients with T2DM is currently suboptimal, largely because our healthcare system has traditionally been based on an acute-care model. In contrast, chronic disease management emphasizes a team approach, medication management and patient adherence, prevention of complications, lifestyle modifications as well as coordination of care among subspecialists. Guidelines for the prevention of T2DM emphasize moving beyond the healthcare system towards integration with other areas, such as government and the media . There is already evidence that intervention at the public health level could significantly impact rates of T2DM . In the future, coordination of care using case managers, technology that helps patients between medical visits, such as mobile health and telemedicine, and restructuring care using patient-centered medical homes and accountable care organizations may be better suited for T2DM management .
Preliminary Study Shows Promise For Long
Human embryonic stem cells
Wikimedia Commons
This story is part 8 of an occasional series on the current progression in Regenerative Medicine. In 1999, I defined regenerative medicine as the collection of interventions that restore to normal function tissues and organs that have been damaged by disease, injured by trauma, or worn by time. I include a full spectrum of chemical, gene, and protein-based medicines, cell-based therapies, and biomechanical interventions that achieve that goal.
Results of a preliminary study show that we may be one step closer to achieving a long-term cure for Type 1 diabetes. After decades of research, there now seems to be at least partial success at transplanting functional insulin-producing islet cells into the human pancreas.
Type 1 diabetes is a major public health crisis. The disease occurs when the bodys immune system attacks its own insulin-producing pancreatic cells. Without these insulin-producing cells, patients are at risk for blindness, disabilities, and are at increased risk for Covid-19.
The process of developing this method began with understanding which chemical signals were needed to steer stem cells into insulin-producing cells. Stem cells are a type of cell that can be reprogrammed into earlier, embryonic stages of development. With the right chemical signals, stem cells can then be transformed into almost any other cell in the body.
Don’t Miss: Are Brussel Sprouts Good For Diabetics
How Stem Cells Could Fix Type 1 Diabetes
Encapsulated stem cell-derived islets could shield cells from the immune system.Credit: Ref. 8
Insulin has been one of the most transformative discoveries in medicine. The isolation of this hormone in 1921 made type 1 diabetes a treatable, rather than a terminal, illness. However, there is growing hope that 100 years later, insulin therapy for T1D might be on the brink of obsolescence.
Insulin is crucial to maintaining safe levels of glucose in the blood. It is produced in the pancreas by cells, which continuously detect circulating glucose concentrations and secrete insulin accordingly the higher sugar levels go, the more hormone is released to counteract the increase. In T1D, however, the cells are destroyed by a persons own immune system.
The cause of this autoimmunity, which typically manifests in childhood, is incompletely understood, but the effect is clear: with neither cells nor insulin, circulating sugar levels remain constantly, toxically elevated. This chronic hyperglycaemia damages blood vessels and nerves, leading to an accumulation of ill-health effects and, if untreated, death.
Now, though, a growing number of scientists and physicians are talking about curing T1D. Their focus is not supplying the body with insulin, but rather replacing the cells that make it.
What Is The Main Cause Of Type 2 Diabetes
First, its important to understand what causes 2 diabetes in the first place, and that culprit is insulin resistance.
What does it mean to be insulin resistant? It occurs when your body needs more and more insulin to bring your blood sugar levels down. This happens when someone engages in an activity that raises their blood sugar levels up, over and over again.
What easily raises your blood sugar levels?
You guessed it.
Eating sugar.
Well, sugar and refined carbs are two of the worst for your blood sugar levels. So, not only should you avoid sugar because it rots your teeth but also because its a major contributor to type 2 diabetes.
A quick side note: Insulin resistance happens in type 1 diabetes but its due to an immune system attack on the insulin-producing cells and therefore considered an autoimmune disease there are different solutions to these two types of illnesses. This article is focusing on type 2 diabetes.
Recommended Reading: Type 1 Diabetes Snack List
Prompting New Cells To Produce Insulin
The Edmonton Protocol has sparked a flurry of research worldwide, much of it aimed at providing alternative sources of the insulin-secreting cells needed to cure juvenile diabetes. One of the more promising discoveries, documented in the May issue of the U.S. medical journal Diabetes, is the result of research conducted at the University of Calgary and Shiga University in Japan. It began with the understanding that pancreatic cells, which routinely produce insulin, and intestinal cells, which do not, share a common origin in the embryo. The question: could an intestinal cell be tricked into performing like a pancreatic cell? The answer: yes, at least judging by experiments conducted in rats.
Maclean’s June 10, 2002
Type 2 Diabetes: Experimental Therapy Could Remove Need For Insulin
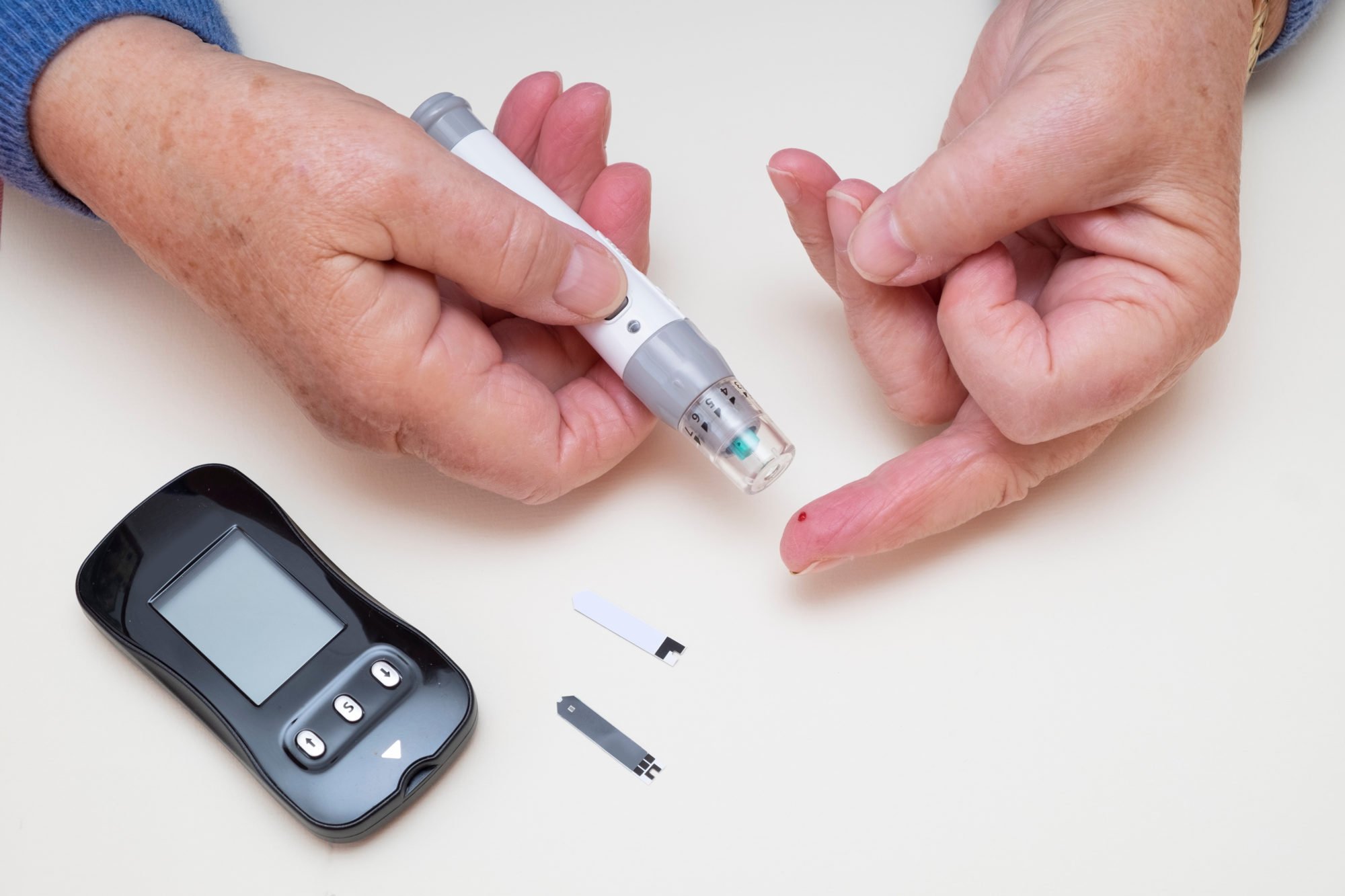
Scientists have proposed a new therapy for type 2 diabetes. If proven effective, the therapy could help some people discontinue insulin treatment.
Scientists have proposed a new therapy for the treatment of type 2 diabetes, with a proof-of-concept study showing positive initial results. If effective, the therapy may mean that some people can stop taking insulin treatment.
The authors of the research presented their findings at UEG Week Virtual 2020, a conference organized by United European Gastroenterology, a professional nonprofit organization for specialists in digestive health.
National Institute of Diabetes and Digestive and Kidney Diseases , a person may have type 2 diabetes when their blood sugar is too high.
People gain blood sugar, or blood glucose, mainly from the food they eat. Insulin helps cells access this glucose to use as energy. However, for a person with type 2 diabetes, either their body does not make enough insulin or their cells do not respond to insulin correctly.
This then means that the glucose in their blood increases, which can lead to complications of diabetes, such as heart and kidney disease, visual impairment, and loss of sensation in the limbs. The higher the blood glucose over time, the
Centers for Disease Control and Prevention , about 1 in 10 adults in the United States have diabetes, and 9095% of these individuals have type 2 diabetes.
You May Like: Type One Diabetes Side Effects
Andrew Pepper And Gregory Korbutt
Andrew Pepper and Gregory Korbutt are working to make islet transplants safer and more accessible, closing in on a cure for the masses.
How it works
Andrew Pepper
Islet transplants pave a promising path toward the end of insulin. But viable donor islets are hard to come by. Korbutt and Pepper have identified a reliable supply of islet cells from neonatal pigs that can be transplanted into patients with diabetes. Patients would receive localized anti-rejection drugs directly to the cells instead of throughout the whole body, which would thwart the usual side-effects caused by immunosuppression.
Yesterdays research, tomorrows treatment
Two giants stand between islet transplants and a cure: limited islet supply and the severe side effects of anti-rejection drugs.
Korbutt and Pepper are socking them both with one swing. Since immunosuppressants can pose more risk than reward, currently only about five to 10 per cent of patients living with diabetes are eligible for a transplant, says Pepper, an assistant professor in the Department of Surgery. He and Korbutt have developed a way to carry anti-rejection drugs directly to the site of the transplant using microscopic bubbles that will release over time to keep the immune response at bay.
Gregory Korbutt
What a cure looks like
Is There A Cure For Type 2 Diabetes
Theres no cure yet, but our scientists are working on a ground-breaking weight management study, to help people put their type 2 diabetes into remission.
Remission is when blood glucose levels are in a normal range again. This doesnt mean diabetes has gone for good. Its still really important for people in remission to get regular healthcare checks. But being in remission can be life changing.
Our ground-breaking study is called DiRECT, short for Diabetes Remission Clinical Trial, and it could completely change the way type 2 diabetes is treated in the future.
Don’t Miss: Are Diabetic Test Strips Universal
Whats Next In Diabetes Treatment
The global diabetes drugs market is expected to reach a massive 68B by 2026, and we can expect all sorts of revolutionary technologies to come forward and claim their market share.
Researchers are already speculating about microchips that can diagnose diabetes type 1 before the symptoms appear, nanorobots traveling in the bloodstream while they measure glucose and deliver insulin, or silica particles that can slow down the digestion of food to prevent diabetes and obesity.
Whatever the future brings, it will undoubtedly make a huge difference in the lives of millions of people worldwide.
This article was originally published in November 2016 and has since been updated to reflect the latest developments in diabetes treatment.
Images via DRI Biohub MaSTherCell
Who Could Get The Treatment
Peter Senior, MBBS, PhD, director at the Alberta Diabetes Institute, told Verywell that most stem cell-based treatments have been focused on people with severe forms of type 1 diabetes because they are the most at-risk for serious, detrimental health outcomes, and have often experienced dangerous blood sugar levels.
According to Senior, these patients have “problems with erratic blood sugars, but that’s not their only problemthey’ve got eye problems and kidney problems and other things like that.”
Stem cell-derived treatment in humans is new, which means that its going to take time to prove long-term benefits. However, the potential for short-term successas in Sheltons caseis being seen already.
If stem cell-derived therapies prove effective over time and researchers can find a way to deliver the treatments without the need for immunosuppressants, Senior said that the candidate pool would open up.
Effectively curing someone of type 1 diabetes before the disease has progressed and caused serious health complications will help improve patients’ overall quality of life.
If I was a parent with a child with type 1 diabetes, I would want a treatment that meant they never had to worry about diabetes, Senior said. But it may take 40 years for us to be able to show those long-term benefits.
Also Check: A1 Diabetes And Medical Supply
Stop The Immune Attack
In type 1 diabetes, the immune system is unable to tell the difference between harmful germs and the body’s cells and tissues, so the immune system attacks the bodys own insulin producing beta cells.
One way to cure diabetes could be to persuade a badly behaved immune system to accept the beta cells as part of the body.
Some of the immune system culprits attacking the beta cells are T cells. T cells develop in the thymus gland and, from a naïve or undifferentiated state, they are gradually educated to become helpers, warriors, or regulators.
In type 1 diabetes, the helper and warrior T cells work together to kill the beta cells, while the regulators appear unable to stop this from happening.
A/Prof Grey’s team worked up a vaccine, called BCMA-Fc, that re-dressed this imbalance. When given to mice with a disease similar to type 1 diabetes, the vaccine prevented diabetes by increasing the number of regulator T cells and reducing the number of warriors.
This work shows the potential of stopping the immune attack as a way to prevent type 1 diabetes. It has supported the testing of a related compound, called rituximab, in people with promising results. In a USA trial, people kept the ability to produce their own insulin, after diabetes had started, for up to 18 months. Further study will test whether taking this drug repeatedly will continue to maintain insulin production.
How Soon Will My Order Arrive
Currently, we ship all orders from the United States, so delivery times depend on the country and region we are shipping to. If you add the product to your cart, you will be able to enter your postal code to compare delivery times and shipping rates specific to your region. That way, you can choose the shipping option that best suits you!
Read Also: A 1 Diabetic And Medical Supplies
Mouthwash Could Help Those Infected With Covid
Unfortunately, islet cell implantation has major limitations. Transplant recipients are forced to take immunosuppressant anti-rejection drugs that come with a grocery list of side effects, such as high blood pressure and increased risk of infections. Then theres the lack of supply organ donations and the risk that, in most cases, the diabetic patient will slowly have to start reintegrating insulin over the years.
The stem cell therapy that Dr. Shapiro is proposing has none of these drawbacks. The University of Alberta team foresee a one-time injection with possible re-ups later on of insulin-producing cells derived from human stem cells. No need for immunosuppressants or organ donations.
Now, the team is ready to move on to human trials. The only obstacle: money. A small volunteer group, Heading to 2022, wants to raise $22 million by 2022 to help bring Dr. Shapiros new treatment to the next phase of trials.