Diabetes Can Affect Your Eyes
Being familiar with how diabetic retinopathy develops is helpful when it comes to understanding its treatment. Blood vessel damage is a common complication of diabetes. Diabetic retinopathy occurs when the blood vessels that supply your retina, the delicate tissue layer in the back of your eye that senses light, are damaged.
The damaged vessels can leak blood and fluid into the retina. The blood and fluid can build up and cause swelling in the center of the retina, called the macula. This is known as macular edema. As diabetic retinopathy advances, these diseased blood vessels close and the retina is deprived of oxygen. In an attempt to keep a good blood supply to your retina, abnormal new blood vessels may grow. But the new blood vessels tend to be fragile, resulting in more bleeding and membrane formation. This can lead to symptoms such as blurry vision, dark spots or blank spots in your visual field, difficulty seeing colors, and even permanent vision loss over time.
Are You Looking For Retinopathy Treatment
Can diabetic retinopathy be reversed? No, but it doesnt have to lead to blindness, either. If you catch it early enough, you can prevent it from taking your vision.
Thats why its vital to have regular visits with an Ophthalmologist or Optometrist whos familiar with diabetes and retina treatment. The team at Drs. Campbell, Cunningham, Taylor & Haun have been treating patients in the Knoxville area for over 60 years. Our retina specialists would love to help you manage your eye health and preserve your sight for years to come.
Its clear to see that your vision should be a priority. Put our experience to work for you and contact us to schedule an appointment today.
Other Eye Transplant Surgeries
Other types of eye transplant procedures, some of which are still in the early stages, include:
- Amniotic Membrane Transplantation . This is a well-established surgery. The amniotic membrane is replaced to treat problems affecting the sclera, the outer layer or âwhiteâ of the eye, and the conjunctiva, the clear tissue covering the white part of the eye.
- Eyelash transplants. Eyelashes do not need to be long to be effective, but they are an important part of the eyeâs overall system, helping to maintain the microbiome. If eyelashes are lost due to injury, burns, medical conditions, or radiation treatment, they can be replaced with transplant surgery.
- Tear duct replacement. This procedure is still in its early phases, but in 2010, French eye surgeons transplanted eyelids with tear ducts as part of a full-face transplant. Eyelids with tear ducts have also been part of other transplants in the past few years. For people who suffer problems with clogged or insufficient tear ducts, this transplant could change how their eyes manage moisture.
- Retinal pigment epithelium transplant. Some early retinal cell testing has been very successful. In clinical trials, researchers have used human stem cells to create retinal pigment epithelial cells, which can be beneficial for those suffering from macular degeneration or other conditions that involve degradation and loss of cells in the retina.
You May Like: What’s New In Diabetes Treatment
Role Of Oxidative Stress And Use Of Antioxidant Compounds
Production of reactive oxygen species has been implicated in the development of diabetic complications . Diabetes may cause ROS production through glucose auto-oxidation, increased flux through the polyol pathway, and increases in protein glycation . ROS may activate aldose reductase and PKC and increase AGE production and DAG formation .
The pervading role of ROS in the biochemical processes leading to microvascular damage has prompted an investigation of antioxidants as preventive therapy for diabetic complications . Inhibition of superoxide production can effectively block sorbitol accumulation, AGE formation, and PKC activation . These findings suggest that ROS production is associated with at least three mechanisms of diabetes-induced vascular damage. Antioxidants are effective inhibitors of pericyte loss secondary to diabetes in experimental models . Tocopherol also inhibits hyperglycemia-induced DAG production and PKC . Tocopherol prevents retinal hemodynamic abnormalities in diabetic rats . In patients with type 1 diabetes and little or no baseline retinopathy, retinal blood flow was significantly increased after 4 months of tocopherol therapy . Recent results of the Heart Outcomes Prevention Evaluation study and other trials showed a lack of effect of tocopherol in the prevention of cardiovascular risks, despite suggestive evidence to the contrary .
How To Prevent Diabetic Eye Disease
The best way to prevent diabetic eye disease is to manage diabetes and lead a healthy lifestyle. The diabetes ABCs include blood sugar, blood pressure and cholesterol, and managing these concerns can maintain your ocular health and overall well-being. Eating a good diet and regular exercise can significantly improve your odds of diabetic eye disease. Quitting smoking is another way to prevent these conditions and annual dilated eye exams.
You May Like: What Is An Acceptable A1c Level For A Diabetic
Laser Treatment For Diabetic Retinopathy
Diabetic retinopathy is an eye condition that can cause vision loss and blindness in people who have diabetes. It affects blood vessels in the retina .
If you have advanced diabetic retinopathy, your doctor may use a type of laser treatment called scatter laser surgery as part of your treatment plan. In scatter laser surgery , your doctor will use a medical laser to shrink blood vessels in your eye that are causing vision problems.
You may also need other treatments, like injections, in addition to laser treatments.
Conventional Thinking On Diabetic Retinopathy Turned Upside Down
| In Brief The SEATTLE Phase IIb/III clinical trial of emixustat did not meet its primary endpoint of showing a significant difference in the growth of lesions in geographic atrophy compared to placebo. Acucela said it will further analyze the SEATTLE data with its partner, Otsuka Pharmaceutical. Acucela also has an ongoing pilot study of emixustat for proliferative diabetic retinopathy and is considering an initiation study in Stargardt disease. SanBio has been granted a U.S. patent for its proprietary modified stem cells, SB623, for the treatment of retinal degeneration. SanBio developed SB623 to promote regenerative processes in the central nervous system and provide therapeutic options for debilitating neurological disorders, including retinal degeneration by enhancing photoreceptor function. The Food and Drug Administration has approved an update to prescribing information for Eylea . The label language clarification recognizes that while most patients receiving Eylea will require dosing once every eight weeks after an initial monthly dosing period, some patients will still require monthly dosing. A retrospective analysis of the Phase III RIDE and RISE clinical trials, published in Ophthalmology, showed that people with less advanced diabetic macular edema and who responded better to initial treatment with ranibizumab needed fewer injections over the long-term, suggesting that treating people with DME earlier may help reduce long-term treatment burden. |
REFERENCE
Read Also: What Diet Is Best For Type 1 Diabetes
Types Of Diabetic Eye Disease
Both type 1 and type 2 diabetes put you at higher risk for certain eye diseases and complications that may lead to blindness if left untreated. Diabetic eye disease is a group of eye problems that affect this population. The longer you live with diabetes, the more likely you are to experience vision changes and vision loss.
Diabetes damages the blood vessels in your eye when you have high blood glucose levels. While short-term high blood sugar only causes temporary vision changes, such as blurry vision, long-term uncontrolled diabetes can wreak havoc on your eyesight.
The increased blood glucose levels damage the tiny blood vessels in the back of your eye, and these issues can arise before you know you have diabetes or are considered prediabetic. The damaged vessels can leak fluid and swell, and new, weak blood vessels grow in their place. These growths can bleed into the middle of the eye, cause scarring and increase eye pressure to dangerous levels.
There are four types of diabetic eye diseases, as follows:
Eye Surgery Success And Risks
Despite unmatched success rates of a corneal transplant and other eye surgeries, organ rejection is the main challenge associated with these procedures. Organ rejection occurs if your body’s immune system does not recognize the transplanted tissue and attacks it.
Corneal rejection occurs in three out of 10 patients who undergo full-thickness transplants. Rejection risks are lower in partial-thickness surgery patients. Warning signs of impending rejection include:
- Sudden eye pain
- Redness in the eye
- The eye becomes extra sensitive to light
You should inform your eye surgeon if you have any of these symptoms after a corneal transplant. That aside, corneal transplants may also cause other eye problems, such as bleeding, infection, detached retina, and glaucoma.
Even if the transplant works as expected, other eye problems, such as macular degeneration, diabetic retinopathy, and astigmatism can impair your vision.
You May Like: Type 2 Diabetes And Eyes
Where Should You Go For Help On Organic Brain Damage
Organic brain damage, where there’s no known cause for the damage, is a contraindication to corneal donation. There are many causes for organic brain damage. Among them are chronic abuses of alcohol or hardening of the arteries. Organic brain damage may lead to clinical dementia and patients with organic brain damage are usually helped through their family doctor or internist with the assistance of a neurologist.
Treatment Of Diabetic Retinopathy
Other than controlling blood pressure, blood cholesterol and the levels of blood sugar, treatment is not needed during the first three stages of diabetic retinopathy. The fourth stage, proliferative retinopathy is treated with a laser surgery procedure known as scatter laser treatment. During the procedure the abnormal blood vessels are ablated causing them to shrink. This procedure works best once the blood vessels begin to bleed. Severe blood vessel bleeding may need to surgically corrected with a vitrectomy procedure to remove the blood from the eye.
Treatment for macular edema usually includes a laser procedure called focal laser treatment. During this procedure, several hundred small laser burns are placed in the areas of retinal leakage around the macula to prevent leakage from occurring and reduce the amount of fluid in the retina. This helps reduce the risk of vision loss and may improve lost vision in a small number of cases. Focal laser treatment is performed in your doctors office and can usually be completed in just one session.
Don’t Miss: What Are The Best Foods For Type 1 Diabetics
Symptoms Of Diabetic Retinopathy
In the early stages of diabetic retinopathy, patients usually do not show symptoms, and treatment is not always required. Patients have to monitor their blood-sugar levels to prevent the condition from worsening. If it does, prompt treatment is necessary to preserve vision.
Patients who develop diabetic retinopathy may not, at first, notice any changes to their vision. In its earliest stages, the condition causes tiny areas of swelling in the small blood vessels of the retina.
Once symptoms are present, they include the following:
- Blurred or double vision
- Seeing flashing lights, blank spots or dark floaters
- Pain or pressure in either or both eyes
- Problems with peripheral vision
In its advanced stages, diabetic retinopathy can cause irreversible blindness.
During any stage of diabetic retinopathy, a condition known as macular edema can develop. Macular edema is the buildup of fluid in the macula, the light-sensitive part of the retina that allows objects to be seen with great detail. As the macula swells, vision becomes blurred. About half of the people with proliferative retinopathy are diagnosed with macular edema.
Other Problems That May Develop Are:
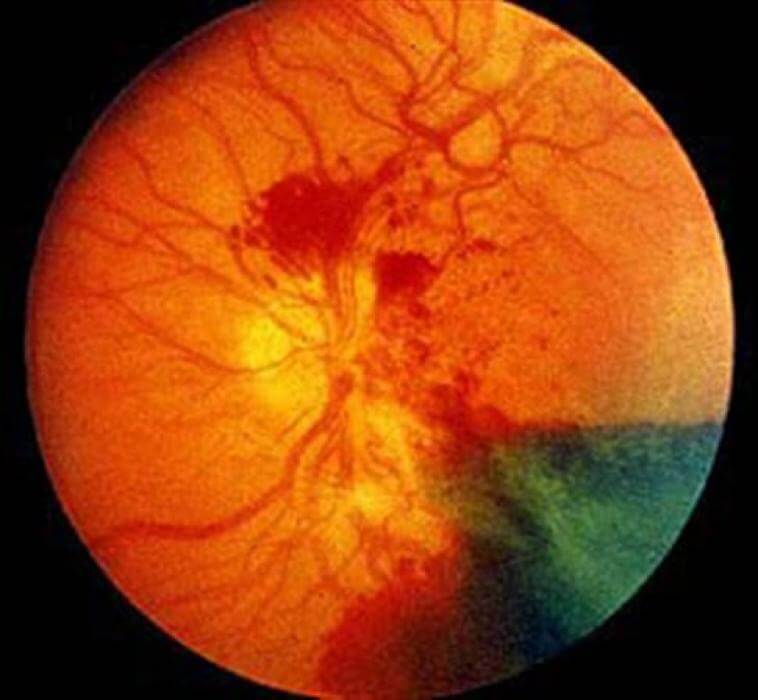
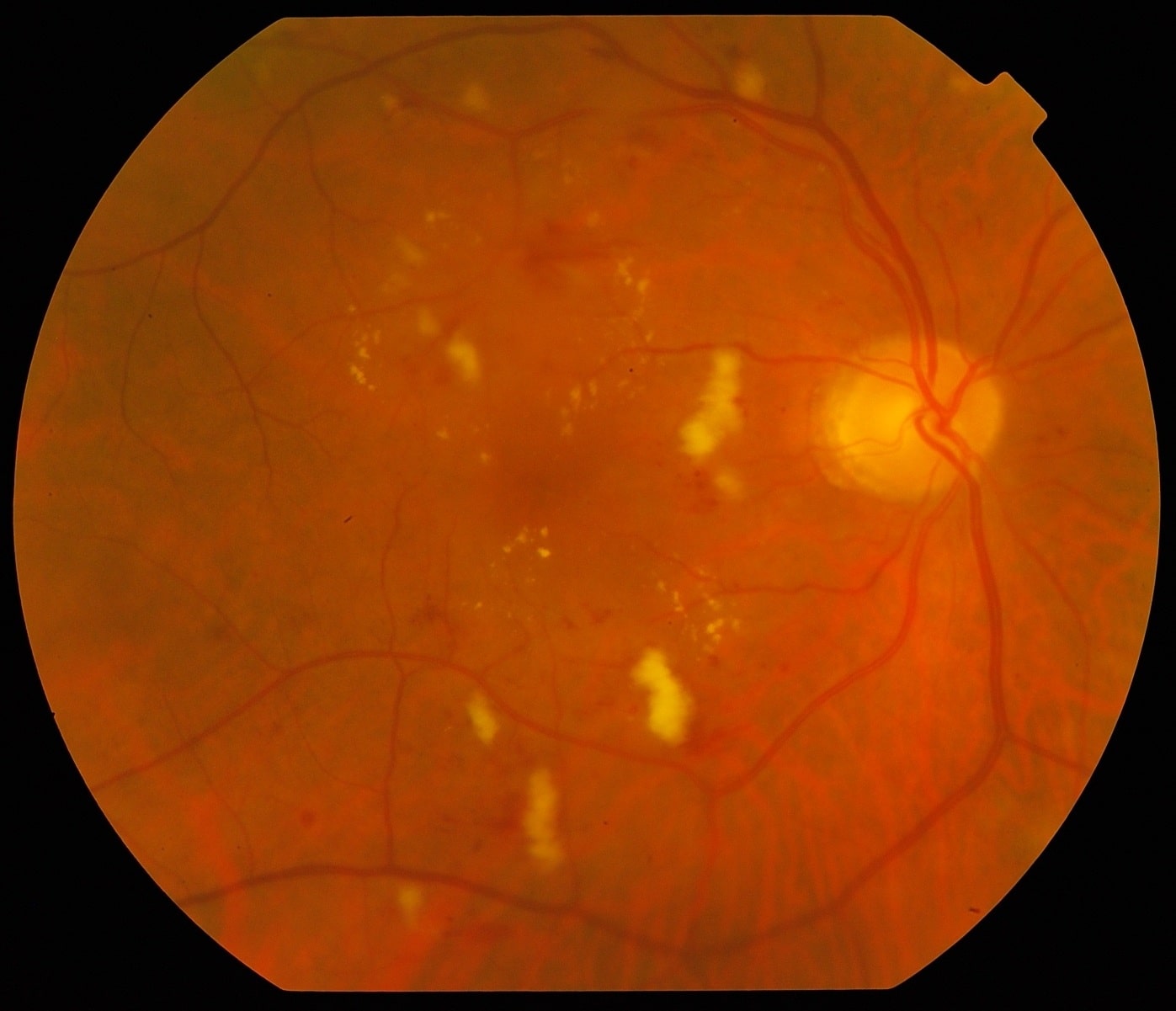
A comprehensive eye examination by your doctor is the only way to find any changes in your eyes. An ophthalmologist can usually diagnose and treat serious Retinopathy before you are aware of any vision changes. The doctor will dilate your pupil and examine the inside of your eye with special equipment and lenses.If your doctor finds Retinopathy, color photographs of the retina or a special test called fluorescein angiography will be requested to further evaluate your eye condition.
You May Like: Why Do Diabetics Get Utis More Often
Is There Any Way To Prevent Diabetic Retinopathy
Theres no way to prevent diabetic retinopathy entirely, but there are things you can do to lower your risk. The team at Marano Eye Care recommends managing your diabetes, monitoring your blood sugar levels throughout the day, quitting smoking, and eating a healthy, balanced diet.
In addition, its important you pay attention to vision changes. If your vision becomes blurry, spotted, or hazy at any time, contact the team at Marano Eye Care right away.
Must An Eye Donor Be Dead
For the most part, corneal donation comes from people who are dead. In very rare circumstances, a donor may be living. For example a patient who has an ocular tumor in the back of the eye may be able to donate the eye at the time the eye is removed. If an eye is blind and it is removed, but is healthy in the front, that cornea might also be used. There are no instances of donation between people who are living in other circumstances. Another special circumstance where a person may donate a cornea to themselves is where one eye can still see and one can’t. That is very rare.
Also Check: Is Insulin Used To Treat Type 2 Diabetes
How Do You Treat Diabetic Eye Disease
Although considered one disease, there are many types of diabetic retinopathy.
The two main categories of diabetic retinopathy:
The level of severity and the area of the retina involved determine the type of treatment for diabetic retinopathy.
Injectable medications used in the treatment of Macular Degeneration like Lucentis, Eylea, Avastin, or Kenalog have proved effective in managing the swelling and fluid leakage associated with diabetic eye disease.
Laser photocoagulation is also used to safely and reliably stabilize and improve vision. By focusing the laser onto diseased areas in the retina, swelling can be reduced, abnormal vessels destroyed, and weak vessels sealed.
Managing Background And Pre
You may have been told you have background or pre-proliferative retinopathy. Pre-proliferative retinopathy means that more severe and widespread changes are seen in your retina, including bleed into the retina. The retina is a light-sensitive layer of tissue at the back of the eye and is important for vision. It converts light into electrical signals, which are sent to the brain which turns them into the images you see.
All the same advice on preventing retinopathy applies here – whether you have signs of eye problems or not, managing your diabetes is critical to reduce the chances of the problem progressing.
- Keep blood sugar, cholesterol and blood pressure at your target levels – your healthcare team may give you blood pressure tablets even if you dont have high blood pressure.
- Get your eyes screened as advised – to check for any changes in your eyes. This maybe every three to six months if you have pre-proliferative retinopathy to monitor your eyes.
- Take your diabetes medication – to manage your blood sugar levels.
- Keep to a healthy weight by eating well and moving more.
- Stop smoking – smoking increases your blood pressure and your blood sugar levels, making it harder for you to manage your diabetes.
All these things can reduce your risk of more damage and so prevent or delay your eyes from getting worse. And its not just about eye problems, the more you do these things, the lower your risk of developing serious problems with your feet, heart and kidneys too.
Don’t Miss: Are Headaches A Symptom Of Diabetes
Role Of Ages And Use Of Age Inhibitors
Carbohydrates interact with protein side chains in a nonenzymatic fashion to form Amadori products, and these may subsequently form AGEs, especially in the presence of high glucose . Excessive formation of AGEs has been proposed as another biochemical link between diabetes and the development of microvascular complications. AGEs may affect such functions as enzyme activity, binding of regulatory molecules, and susceptibility of proteins to proteolysis . The chronic interaction of these products with at least one specific cell surface receptor for AGEs may perpetuate a proinflammatory signaling process and a pro-atherosclerotic state in vascular tissues . In vitro, the AGEAGE-specific receptor interaction has been associated with oxidative stress and the activation of nuclear factor-B, which leads to hyperexpression of proinflammatory cytokines, lymphocyte adhesion molecules , vasoactive mediators, and pro-coagulant factors . These processes may result in disruptions of retinal hemodynamics and/or damage to vascular endothelial cells. Accordingly, strategies to reduce AGE formation in the absence of achieving euglycemia have been investigated as potential preventive therapies for diabetic microvascular complications .
What If Theres No Possible Donors Due To Lasik
First of all, not everyone will have Lasik surgery because only about 25 percent of the population needs it. At the present time, less than 1 percent of the population who needs Lasik surgery has had it. There will always be people who have not had eye surgery who can be donors. It merely means we have to get the word out to everyone. People who need corneal transplants will be able to get corneal transplants.
Don’t Miss: How To Treat Type 2 Diabetes
Does Having Diabetes Prevent Someone From Being A Eye Donor
Only the advanced stages of diabetes that require insulin prevent a patient from being a donor. Patients who have diet-controlled diabetes may still be eye donors. Patients who have severe forms of diabetes may donate their eyes for research rather than for corneal transplantation. Research is a very valuable mission and may lead to prevention or cure of blindness for many more than one patient.
What Is Diabetic Maculopathy

Diabetic maculopathy is a type of diabetic retinopathy, also known as diabetic macular oedema . In diabetic maculopathy the blood vessels in the part of the eye called the macula can become blocked.
Blood vessels that enlarge to compensate for blocked blood vessels become leaky and this leaked fluid builds up in the macular causing swelling. At first, you may not notice changes to your vision. Over time patients develop poor central vision and are unable to read or drive, but the vision to the side usually remains normal. If this is detected there is a high risk your vision could be affected, and you may be advised to have more frequent testing.
Recommended Reading: When Should I Test My Blood Sugar