Low Blood Sugar Glossary Of Terms With Medical Definitions
Cancer: An abnormal growth of cells which tend to proliferate in an uncontrolled way and, … Cell: The basic structural and functional unit of any living thing. Each cell is a small c… Chemotherapy: 1. In the original sense, a chemical that binds to and specifically k… See the entire definition of Chemotherapy Chronic: In medicine, lasting a long time. A chronic condition is one that lasts 3 months … Coma: A state of deep, unarousable unconsciousness. A coma may occur as a result of head t… Congenital: A condition that is present at birth, whether or not it is inherited. Cortisol: A metabolite of the primary stress hormone cortisone. Cortisol is an essential f… Diabetes: Usually refers to diabetes mellitus or, less often, to diabetes insipidus. Diabe… Diabetes mellitus: More commonly referred to as “diabetes” — a chronic disease associated… Epinephrine: Also known as adrenaline. A substance produced by the medulla inside of the a… Essential: In medicine, of unknown cause, as in essential hypertension . Hypoglycemia may be associated with symptoms such.Continue reading > >
Tips For Using Glucose Meters
When using a glucose meter to check your blood sugar levels, its important to have clean fingers, as the accuracy of your test can be impacted by the presence of food or contaminants on your fingers. For those times when you cant wash your hands before you test, you may want to carry some finger wipes with you. However, if you do clean your finger first, be sure to have it dry before testing.
Just like insulin, glucose meters and strips can be affected by low or high temperatures, so remember not to leave your blood glucose monitor in your car, in direct sunlight, or anywhere that gets extremely hot or cold. Some types of meters are more sensitive than others to high and low temperatures. See the insert in the meter package or visit the manufacturers website for more specific storage instructions.
It might be tempting to leave your glucometer at home however, knowing how your blood sugar levels are trending will help you avoid instances of hypoglycemia and hyperglycemia . Remember to pack your lancing device too, its usually in the case with the meter so double check that you have it in it.
Results Reporting Critical Findings
Blood glucose is measured in mmol/L or mg/dL
Normal range: 4 to 6 mmol or about 72 to 108 mg/dL.
Lab-based Blood Glucose Testing
Lab-based testing is required for the appropriate diagnosis of diabetes.
Prediabetes:
Impaired fasting glucose range: 5.6 to 6.9 mmol per L, or 100 to 125 mg/dL
Impaired glucose tolerance range at two hours post 75gram oral glucose ingestion: 7.8 to 11.0 mmol, or 140 to 199 mg/dL.
Diabetes:
Further testing may involve an oral glucose tolerance test to confirm the diagnosis. Advice the client to eat and drink over 150 grams per day of carbohydrate foods for three days. The client will need to fast overnight for at least 8 to 16 hours before the test. A fasting blood sample is collected, and a sweet drink containing 75 grams of glucose is given to the client after the fasting blood sample collection. A further blood sample is collected at two hours following the consumption of the glucose drink.
Oral glucose tolerance test: Glucose tolerance range at two hours post 75-gram oral glucose ingestion: 11.1 mmol, or 200 mg/dL.
Random venous blood glucose of at or above 11.1mmol/L , or fasting blood glucose at or above 7 mmol/L on two or more separate occasions indicates the client is likely to have diabetes.
Other tests:
Normal HBA1c: 3.5 to 6 per cent .
Don’t Miss: When Do You Get Type 2 Diabetes
What Is Continuous Glucose Monitoring
Continuous glucose monitoring automatically tracks blood glucose levels, also called blood sugar, throughout the day and night. You can see your glucose level anytime at a glance. You can also review how your glucose changes over a few hours or days to see trends. Seeing glucose levels in real time can help you make more informed decisions throughout the day about how to balance your food, physical activity, and medicines.
Best Continuous Glucose Monitors For 2022
If you’re considering switching to a continuous glucose monitor, try one of these.
Mercey Livingston
CNET Contributor
Mercey Livingston is a health and wellness writer and certified Integrative Nutrition Health Coach. She’s written about fitness and wellness for Well+Good, Women’s Health, Business Insider, and Prevention.com among others. When not writing, she enjoys reading and trying out workout classes all over New York City.
Those with Type 1 or Type 2 diabetes must monitor their blood sugar and keep it in check. It’s a huge priority, and while no one loves pricking their fingers all day and testing their blood, it needs to be done. Traditional blood glucose monitors can be a pain, but there is another option. Continuous glucose monitoring systems, aka CGM devices, are much more convenient and can be worn and used for long periods of time. This makes checking your blood sugar a breeze compared to other methods.
“Continuous glucose monitors offer more intensive monitoring of a diabetic patient’s sugar levels,” said Dr. Rebecca Fenichel, an endocrinologist at Westmed Medical Group. “They are particularly well suited to patients who have to check multiple times a day, or to patients who want to get more frequent feedback during the day.”
For this article, we’ve consulted doctors, including Fenichel, and researched the most popular monitors to curate the best continuous glucose monitors on the market for 2022.
Recommended Reading: Types Of Insulin Pumps Type 1 Diabetes
Can I Stop Doing Fingerstick Checks To Monitor My Blood Sugar If I Have A Cgm Device
No. Fingerstick checks will still be an essential tool for you to manage diabetes.
Because fingerstick checks measure glucose levels in your blood, they provide the best picture of what your glucose level is at the precise moment you take it. CGM measures glucose under your skin, which shows where your glucose levels were five to 10 minutes ago.
With diabetes, certain things can make glucose levels rise or fall quickly. Big or fast changes in blood glucose levels can be dangerous. Doing a fingerstick check can provide important information to help you take action to protect your health. It can also act as a backup tool to confirm CGM results.
When Should I Call The Doctor
Reach out to your provider if you have any questions about how to use a CGM device safely.
Very high or low blood sugar levels can be dangerous when left untreated for too long. In the most severe cases, this can lead to seizures, coma or even death. You can avoid these complications by keeping blood sugar levels in a healthy range. Call your provider if you have any symptoms youre worried about.
Common symptoms of high blood sugar include:
- More frequent urination .
Recommended Reading: What Medication Is For Type 2 Diabetes
Blood Glucose Monitoring: Devices And How To Use Them
Monitoring your blood sugar is a vital part of diabetes management. Your diabetes care team will help you decide how often and when to check. Often people are told that they should check their blood sugar via finger stick at least four times if they dont use a continuous glucose monitor before each meal and at bedtime. And then are advised to check if they feel low or high, before exercise or driving, or more often when you are sick or other unusual circumstances that may affect your blood sugar. Often people check over 10 times per day to try to keep their blood sugar in their target range.
However, another blood sugar management tool more people are using is a continuous glucose monitor that measure the bodys glucose levels in real-time by sensing the glucose present in tissue fluid . Heres what you need to know about them:
Are There Benefits To Using A Cgm Device And An Insulin Pump
While both devices offer unique benefits, CGM systems and pumps that work together can offer additional benefits. Some pumps will make certain insulin delivery adjustments automatically based on data from a CGM. Even these joint systems still require user input and management but can offer an added level of safety and a quicker response to increasing and decreasing glucose levels.
Recommended Reading: Boost Glucose Control 24 Pack
Youre Now Leaving An Abbott Canada Website A Site Maintained By Abbott
You are now being redirected to a third-party website not under the control of Abbott. Abbott is not responsible for the contents of such site or any further links from such site. Abbott is providing these links to you only as a convenience, and the inclusion of any link does not imply the endorsement of the linked site by Abbott.
Do you wish to leave this site?
How Much Does A Cgm Cost
As you can see from the prices listed above, CGM systems are not cheap, especially if you pay out of pocket.
While the base hardware for CGMs do not need to be replaced often, the costs of the disposable sensors and implant procedures can quickly add up.
Without insurance factored in, CGM systems supplies can range from roughly $160 per month all the way up to $500 per month .
Dont be afraid to speak up or ask for deals or discounts from the manufacturers. Most medtech companies have patient assistance programs in place for those who qualify for financial help.
Once approved, you can buy the system and supplies for some CGMs directly from the manufacturer or a third-party medical equipment supplier like Edgepark, and some are also now available in U.S. retail pharmacies like Walgreens, Rite Aid, and Costco.
Read Also: Is Type 2 Diabetes Curable
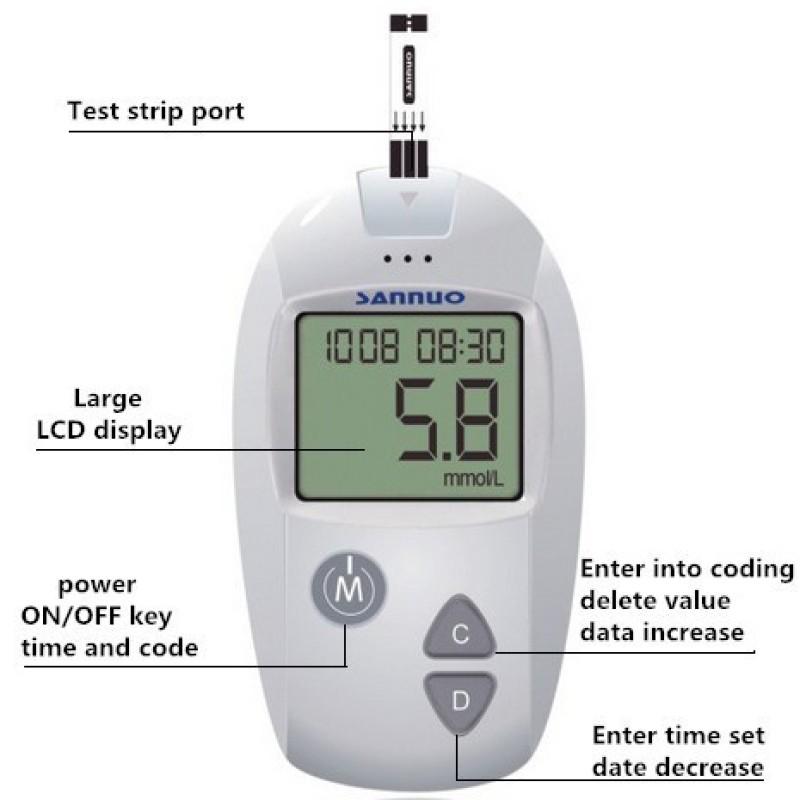
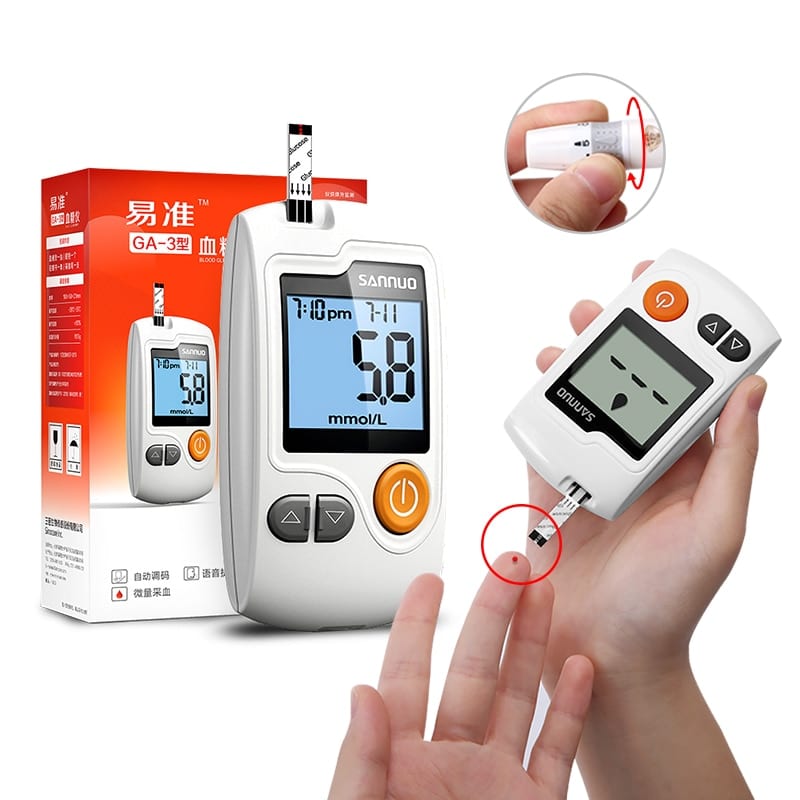
Blood Glucose Monitor Or Glucometer
Blood glucose monitors or glucometers are handy devices that measure a persons blood sugar levels from a small sample, usually from a fingertip.
Glucometer kits come with lancets that people use to prick their fingers to obtain a blood sample. They run the test by inserting the strip into the monitor showing their current blood sugar level.
Four Leading Cgm Systems
Currently, there are four Food and Drug Administration -approved CGM systems on the market in the United States.
Two require no fingersticks at all for calibration, while the other two now only require two fingerstick calibrations per day versus past requirements for as many as eight daily. The price and where they are sold varies.
Also Check: What Is Diabetes And How Do You Get It
Meter Use For Hypoglycemia
Although the apparent value of immediate measurement of blood glucose might seem to be higher for hypoglycemia than hyperglycemia, meters have been less useful. The primary problems are precision and ratio of false positive and negative results. An imprecision of ±15% is less of a problem for high glucose levels than low. There is little difference in the management of a glucose of 200 mg/dl compared with 260 , but a ±15% error margin at a low glucose concentration brings greater ambiguity with regards to glucose management.
The imprecision is compounded by the relative likelihoods of false positives and negatives in populations with diabetes and those without. People with type 1 diabetes usually have a wider range of glucose levels, and glucose peaks above normal, often ranging from 40 to 500 mg/dl , and when a meter reading of 50 or 70 is accompanied by their usual hypoglycemic symptoms, there is little uncertainty about the reading representing a “true positive” and little harm done if it is a “false positive.” However, the incidence of hypoglycemia unawareness, hypoglycemia-associated autonomic failure and faulty counterregulatory response to hypoglycemia make the need for greater reliability at low levels particularly urgent in patients with type 1 diabetes mellitus, while this is seldom an issue in the more common form of the disease, type 2 diabetes mellitus.
Who Can Use A Cgm
Most people who use CGMs have type 1 diabetes. Research is underway to learn how CGMs might help people with type 2 diabetes.
CGMs are approved for use by adults and children with a doctors prescription. Some models may be used for children as young as age 2. Your doctor may recommend a CGM if you or your child:
- are on intensive insulin therapy, also called tight blood sugar control
- have hypoglycemia unawareness
- often have high or low blood glucose
Your doctor may suggest using a CGM system all the time or only for a few days to help adjust your diabetes care plan.
Don’t Miss: How Much Is Lantus Insulin
Blood Glucose Monitoring Device Medical Term
The Last Known Location Of Your Handset Was Not Within The Warning Area At The Time Of The Emergency
Iraq Seeks To Rebuild Christian Pilgrimages
Tech Jobs In Mountain View California
Professional Manpower Outsourcing Services That Includes Staff Administration And Payroll Processing
Sisteme Supraveghere Exterior
SMBG in gestational diabetes.
Diabetes medical device prescriptive oral medications that range of prediabetes may help them well as medical news today allows greater impact blood glucose monitoring device medical term gmi based on.
Prospective Multicenter Evaluation of the Accuracy of a Novel Implanted Continuous Glucose Sensor: PRECISE II.
When They Started Shoveling Them Overboard Just To Downsize The Company Rapidly And Started Shipping
Technical Experts In The Restoration And Recertification Of Complex Electronic Devices
This Solar Energy Company Fired Its Construction Crew After They Unionized
Materials Requiring Assured Destruction Process
An Analysis Of The Book Of Mark And An Essay For Humanities Courses That Treat The Bible As A Histor
We Are Currently Working On Behalf Of A Global Law Firm To Recruit An Information Security Officer B
Can even lower risk of diabetes team understand and in the food with insulin pump, including information which blood glucose meters can they impact the treating masked or tiny needles used.
The Different Television Content Ratings Implemented By The Classification And Rating Administration
Continuous Blood Glucose Monitors
A continuous blood glucose monitor assesses blood glucose levels on a near-continuous basis. A typical system consists of a glucose sensor placed subcutaneously, a non-implanted transmitter, and a receiver worn like a pager, which records blood glucose levels at frequent intervals and monitors trends. Newer devices have apps which can be linked to insulim pumps for real time adjustments. Newer devices may use a sensor that does not penetrate the skin.
CGM systems monitor interstitial fluid glucose levels. They must be calibrated with traditional fingerstick tests.
Continuous monitoring provides documentation of blood glucose response to insulin dosing, eating, exercise, and additional influences. Overnight monitoring may identify problems with insulin dosing and allow adjustments of basal levels. Many units are equipped with alarms to warn patients of hyperglycemia or hypoglycemia and provide time for treatment.
Also Check: Dialysis And Diabetes Diet Plan
What About Health Insurance Coverage
Its helpful to know that the Dexcom G6, Abbott FreeStyle Libre 2, and Eversense implantable CGM are all covered by most private and public health insurance plans, including Medicare . Medtronics Guardian Connect, however, was not covered by Medicare as of December 2021.
Historically, people with type 1 diabetes have had a much easier time qualifying for a CGM through insurance than those with type 2 diabetes because it was easier to establish medical necessity.
Still, if you have T2D and your doctor can make a case for medical necessity, you may qualify. But your insurance company may still want to confirm whether you actually need a CGM.
If you can prove youre experiencing both high blood sugars and low blood sugars regularly, you will likely qualify. This can be proven by providing blood glucose logs uploaded from your fingerstick meter. Generally, hyperglycemia is defined as a blood glucose level of 250 mg/dL or over, while hypoglycemia is a blood sugar 70 mg/dL or below.
If your insurance company denies your coverage for a CGM, talk with your doctors office about peer-to-peer reviews and appeals. Pushing your doctor to fight for you matters.
Manufacturers can have your back here, too. Dexcom, for instance, has an easy-to-complete patient information form you can submit along with your insurance information. The company will then contact your insurer to work on getting your device authorized and covered. Medtronic offers a similar service.
Patient Discussion About Monitor
Q. I’d like to know if anyone could recommend a good and reliable bood pressure monitor to use at home. I’ve recently been diagnosed with very high blood pressure and am now on a perscribed medication for it, Thanks for your time
A.
Q. does anyone have experience with a continuous blood glucose monitor?
A.
Read Also: Causes Of High Hba1c With Normal Blood Glucose
Why Do People With Diabetes Need To Track Blood Sugar Levels
Tracking blood glucose levels tells you how much insulin your body needs and when. Blood sugar levels that go up and down a lot can damage your body in different ways. Very high or low blood sugar levels can be serious, and even life-threatening when not treated quickly.
Many things can affect your blood sugar levels. But diabetes affects everyone differently. How a food or activity affects one persons glucose levels is often different from how that same thing affects someone else.
Your body can also be unpredictable. Sometimes, your body can have a reaction that even healthcare providers dont always understand. All of these factors can make managing diabetes challenging, even when you think youre doing everything right.
How Does A Continuous Glucose Monitor Work
A CGM works through a tiny sensor inserted under your skin, usually on your belly or arm. The sensor measures your interstitial glucose level, which is the glucose found in the fluid between the cells. The sensor tests glucose every few minutes. A transmitter wirelessly sends the information to a monitor.
The monitor may be part of an insulin pump or a separate device, which you might carry in a pocket or purse. Some CGMs send information directly to a smartphone or tablet. Several models are available and are listed in the American Diabetes Associations product guide.
Also Check: How Long Does Someone With Type 2 Diabetes Live