How To Get Free Prescriptions For Diabetes Medicine
You’re entitled to free prescriptions for your diabetes medicine.
To claim your free prescriptions, you’ll need to apply for an exemption certificate. This is known as a PF57 form. To do this:
- fill in a form at your GP surgery
- you should get the certificate in the post about a week later it’ll last for 5 years
- take it to your pharmacy with your prescriptions
Save your receipts if you have to pay for diabetes medicine before you receive your exemption certificate. You can claim the money back if you include the receipts along with your completed PF57 form.
Analogue Versus Human Insulin
Glucose control, adverse effects, cost, adherence, and quality of life need to be considered when choosing a type of insulin. In general, analogue insulin is similar to human insulin in controlling diabetes, although some trials have found higher mean A1C levels in patients taking analogue insulin compared with human insulin. 17 Analogue insulin usually causes less postprandial hyperglycemia and delayed hypoglycemia. 18,19 In a recent meta-analysis, glycemic control was not improved with analogue insulin compared with human insulin, but nocturnal hypoglycemia was reduced.17
An industry-funded cost-effectiveness analysis found that the increased cost of medication is more than off set by the reduction in hypoglycemic events. 20 However, the analysis assumed a cost differential of 14 percent, which is inconsistent with current pricing . 20,21 Cost-effectiveness analyses have differed regarding the long-term cost savings of using analogue insulin in patients with type 2 diabetes, with industry-sponsored studies finding reduced cost22 and government-sponsored studies finding no cost reduction. 23 Measures of adherence and quality of life have been improved with analogue insulin compared with human insulin. 24,25
Continuous Subcutaneous Insulin Infusion
In patients with type 2 diabetes already using at least one daily insulin injection, the introduction of intensive insulin therapy with continuous subcutaneous insulin infusion resulted in comparable glycemic control, weight gain, and hypoglycemia risk as multiple daily injection therapy . Although continuous subcutaneous insulin infusion was associated with greater improvements in treatment satisfaction in one study , we recommend that its use be restricted to selected patients in experienced centers only.
Read Also: What Is Worse Diabetes 1 Or Diabetes 2
What Other Information Should I Know
Keep all appointments with your doctor and the laboratory. Your blood sugar and glycosylated hemoglobin should be checked regularly to determine your response to human insulin. Your doctor will also tell you how to check your response to human insulin by measuring your blood or urine sugar levels at home. Follow these directions carefully.
You should always wear a diabetic identification bracelet to be sure you get proper treatment in an emergency.
Do not let anyone else use your medication. Ask your pharmacist any questions you have about refilling your prescription.
It is important for you to keep a written list of all of the prescription and nonprescription medicines you are taking, as well as any products such as vitamins, minerals, or other dietary supplements. You should bring this list with you each time you visit a doctor or if you are admitted to a hospital. It is also important information to carry with you in case of emergencies.
Throwing Away Your Needles And Lancets
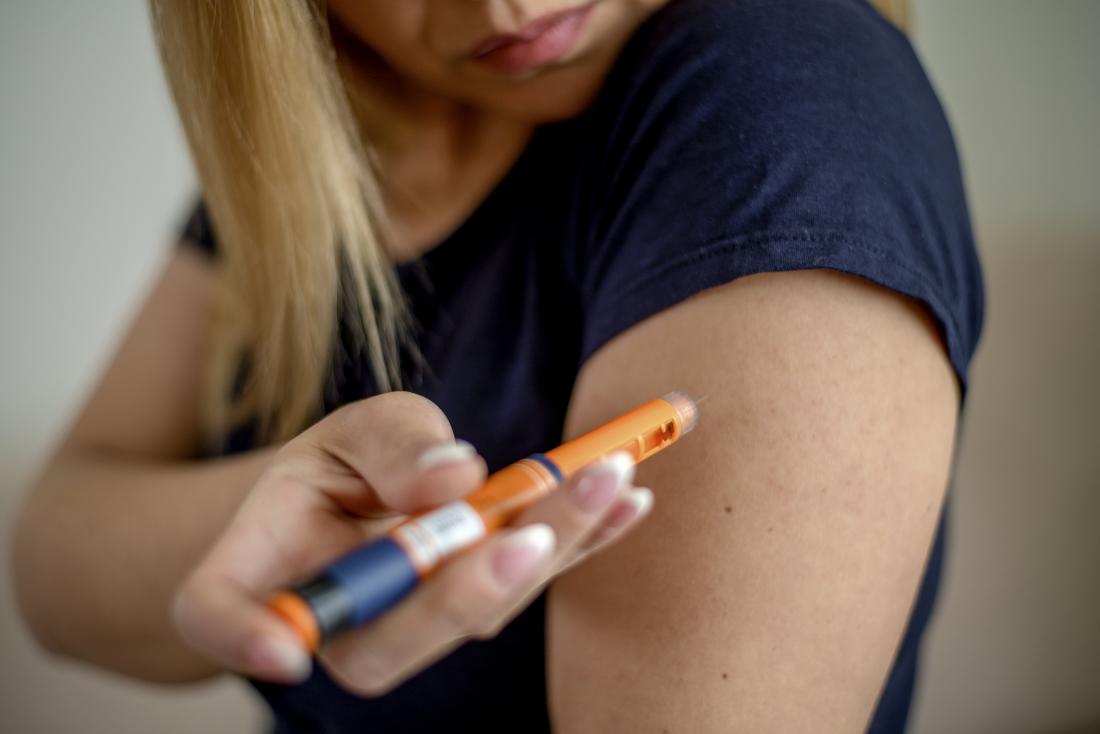
Sharps bins and needle clippers are the safest way of disposing of your insulin needles and your lancets. A needle clipper removes the needle from your insulin pen, and is useful when youre out and about. How you get rid of your sharps bin depends on where you live. Your healthcare team should have information to help you get rid of your bin.
Read Also: What Is Considered Low Blood Sugar For Type 2 Diabetes
Is It An Emergency
If you or someone in your care has chest pains, difficulty breathing, or severe bleeding, it could be a life-threatening emergency. Call 9-1-1 or the local emergency number immediately.
If you are concerned about a possible poisoning or exposure to a toxic substance, call Poison Control now at 1-800-567-8911.
Thanks to our partners and endorsers:
What Are The 6 Different Types Of Insulin
If you need insulin, your doctor will recommend a specific type depending on your lifestyle, the type of diabetes you have, and your blood sugar levels at different times of the day. You may need more insulin coverage at mealtimes, overnight, or throughout the entire day. Currently, there are 5 types of injectable insulins and 1 inhaled insulin.
Types of insulin and how they work in your body
| How long it takes to start working | How long it lasts |
|---|---|
| Inhaled insulin |
Don’t Miss: Diabetes Feet Tingling At Night
Insulin Treatment In Type 2 Diabetes
The decision to take insulin is never an easy one. For many patients, it comes after years of having type 2 diabetes and trying multiple weight-loss regimens, diets, and oral medications. For other patients, the decision to take insulin is made when blood glucose levels are simply too high to control with other drugs.
The good news is that insulin almost always works. Daily injections, however inconvenient or painful at first, can be very effective at controlling blood glucose. Anxious about giving injections? Help is available. If your health care provider prescribes insulin, a trained diabetes educator or pharmacist can teach you how to measure out the proper dose and administer your daily injections.
Why should I use insulin?
With type 2 diabetes, over time, the pancreas is often unable to produce insulin on its own. When that happens, your blood glucose levels will become very difficult to control without daily injections of insulin. Injectable insulin is identical to the insulin made by the body, but can be categorized into two main types: basal insulin keeps your blood glucose stable all day long, even when not eating, while bolus insulin helps your body respond to the quick rise in blood glucose after meals.
Work Out When To Inject Insulin
The time of your insulin injection depends on when your blood glucose level is highest. Most people need to have insulin at bedtime, because your body makes glucose during the night, causing your blood glucose levels to be higher in the morning when you wake. Therefore, an evening dose of insulin helps to maintain lower blood glucose levels overnight. A few people find that their blood glucose levels are highest later in the day. In these people, it’s best to start insulin in the morning. Some people may need to use insulin 2 or more times a day to get better glucose control. Your doctor or nurse will help you decide on the right schedule for you. It usually takes a few weeks to get your dose and timing right.
You May Like: Can You Lose Weight If You Have Diabetes
Why Insulin Can Become Necessary For A Person With Type 2 Diabetes
Starting insulin treatment should not be seen as a setback.
People with type 2 diabetes may require insulin when their meal plan, weight loss, exercise and antidiabetic drugs do not achieve targeted blood glucose levels.
Diabetes is a progressive disease and the body may require insulin injections to compensate for declining insulin production by the pancreas. That is why starting insulin treatment should never be seen as a failure.
Starting insulin treatment should never be seen as a failure.
Treatment with insulin may be added to an antidiabetic medication or completely replace it. Regardless of the treatment, lifestyle habits are essential to managing diabetes.
Many people are reluctant to inject insulin for various reasons:
- Fear of pain or needles
- Guilt
- Impression that this is the last resort
- Fear of hypoglycemic attacks
- Fear of weight gain
- Memories of loved one who had to take insulin
If this is the case, do not hesitate to discuss your concerns with a health care professional. Some of your fears may be due to false beliefs. Learning more about todays insulin treatment will probably allay your fears. For many people, insulin is an effective way to achieve good blood-sugar control, which can prevent or delay certain diabetes complications over the long term.
Store And Dispose Of Your Insulin And Needles Safely
Insulin you are not using should be stored in the door of your fridge. You can keep the insulin you are using out of the fridge for a month, as injecting insulin at room temperature is less painful.
Never put your used needles in the rubbish bin. Your GP or diabetes nurse can give you a container to put used needles in and can organise a place where you can dispose of the container once its full.
Recommended Reading: Type 2 Diabetes Age Range
Can I Mix Rapid
You can mix a rapid-acting insulin with an intermediate-acting insulin, according to your doctors instructions. Rapid-acting insulin should always be drawn into the syringe first. This will keep the intermediate-acting insulin from getting into the rapid-acting insulin bottle. After mixing rapid-acting insulin in the same syringe with an intermediate-acting insulin, you must inject the mixture under your skin within 15 minutes. Remember to eat within 15 minutes after the injection.
Do I Need To Monitor My Blood Sugar Level
Yes. Monitoring and controlling your blood sugar is key to preventing the complications of diabetes. If you dont already monitor your blood sugar level, you will need to learn how. Checking your blood sugar involves pricking your finger to get a small drop of blood that you put on a test strip. You can read the results yourself or insert the strip into a machine called an electronic glucose meter. The results will tell you whether your blood sugar is in a healthy range. Your doctor will give you additional information about monitoring your blood sugar.
Read Also: Patient Teaching On Diabetic Diet
Managing Diabetes With Insulin
Injections of insulin can help manage both types of diabetes. The injected insulin acts as a replacement for, or a supplement to, your bodys natural insulin.
People living with type 1 diabetes cant make insulin, so they must inject insulin to control their blood glucose levels.
Many people living with type 2 diabetes can manage their blood glucose levels with lifestyle changes and oral medication. However, if these treatments dont help control glucose levels, people living with type 2 diabetes may also need supplemental insulin.
Insulin And Weight Gain
When first starting insulin therapy, many people complain that they are eating and exercising the same amount as before but gaining weight. This occurs because with insulin, the body is able to use glucose that was previously wasted in the urine. Glucose that is not needed right away for energy is stored as fat. Studies have shown that weight gain may lead people, particularly women, to not follow their prescribed insulin regimen. This is a dangerous practice that can lead to sustained high blood glucose and a higher risk of long-term complications. Weight gain with insulin therapy is not inevitable, but avoiding it or reversing it generally requires eating fewer calories and/or exercising more.
Don’t Miss: T Slim Insulin Pump 3ml Cartridge
Producing Less Insulin Naturally Over Time
Research has shown that type 2 diabetes progresses as the ability of the body’s pancreatic beta cells to produce insulin dwindles over time. Your beta cells — the cells in the pancreas that produce insulin — slowly lose function. Experts believe that by the time you’re diagnosed with type 2 diabetes, you’ve already lost 50-80 percent of your beta cell function and perhaps the number of beta cells you had. And the loss continues over the years.
“About six years after being diagnosed, most people have about a quarter of their beta cell function left,” says Anthony McCall, M.D., Ph.D., endocrinologist and James M. Moss Professor in Diabetes at the University of Virginia School of Medicine. “With this minimal function, the need for injected insulin increases.”
Some experts say initiating insulin or other blood glucose-lowering medications early in the course of type 2 diabetes can lower blood glucose and even preserve some beta cell function.
Guidelines For Starting Insulin
Know your health care provider’s plan up front. Ask what A1C and blood glucose measures are used and how you will start taking insulin.
Think short-term, not long-term. Start taking insulin when your health care provider recommends it, and notice if you feel better and have more energy. Don’t try to put it off from appointment to appointment.
Ask to be referred to a diabetes education program to learn the ins and outs of taking insulin and get the support you need.
Have a plan with your health care provider to be in touch regularly to increase your dose until you hit your blood glucose targets.
Get the inside scoop from people who have successfully transitioned to insulin. Try attending a support group or connecting with people willing to support you in one or more of the diabetes online communities.
Explore your options for insulin delivery — using the traditional vial and syringe, or using the more contemporary and convenient pens or possibly an insulin pump. Check your health insurance plan to see what it covers.
Continue to eat well and exercise regularly.
Strive for consistency. Take your insulin and eat at similar times every day when possible.
Store insulin properly. Keep the pen or vial of insulin at room temperature , and store extras in the refrigerator.
Carry a source of carbohydrate to treat low blood sugar, such as glucose tablets or hard candy. Start by using 15 grams of carbohydrate.
Also Check: Fruits For Type 1 Diabetes
How To Start Insulin
When first prescribing insulin for a person with Type 2 diabetes, doctors generally start with a single daily injection of long-acting insulin. Determining what dose of insulin to begin with can be done in different ways. One option is to choose a starting dose based on a persons weight. Eventually, many people with Type 2 diabetes will require 12 units of insulin for every kilogram of body weight that is, an 80-kilogram person will require at least 80 units of insulin each day. To start, however, your doctor may begin by prescribing 0.15 units of insulin per kilogram. For an 80-kilogram person, this would be 12 units.
Another option is simply to start with 10 units of insulin, a large enough dose to decrease blood glucose levels for most people but not so large that it is likely to cause hypoglycemia. The dose can then be increased every 37 days based on fasting blood glucose values. A morning blood glucose reading of 80100 mg/dl is ideal, so with numbers that fall in this range, you would not make any changes. If your morning blood glucose readings were under 80 mg/dl, you would decrease your insulin dose by 2 units. Most people, however, will need to increase their dose of insulin above the initial level. It is generally safe to adjust ones basal insulin according to this scale.
When Should Insulin Therapy Be Initiated
Type 2 diabetes is a progressive disease, and thus, ultimately this question will arise for many of our patients. Unfortunately, there is no unequivocal answer, which was nicely illustrated by a recent interactive case vignette. The polling results demonstrated once again that the management of patients with type 2 diabetes uncontrolled by two oral glucose-lowering agents is controversial. Furthermore, the preferred treatment option was found to be related to the respondents’ locations and self-reported specialties .
You May Like: How Do You Screen For Diabetes
Myths About Insulin And Type 2 Diabetes
When you hear the word insulin, do you picture giant needles or pop culture portrayals of insulin users with low blood sugar ?Either way, most people think of insulin as a difficult, painful, or potentially scary medical treatment.The problem is that if you have type 2 diabetes, you need to know the real deal before you can make an informed choice about whether or not this potentially lifesaving therapy is right for you.Here, we take a look at the facts and fiction about insulin when it comes to treating type 2 diabetes.
Insulin Management Of Type 2 Diabetes Mellitus
ALLISON PETZNICK, DO, Northern Ohio Medical Specialists, Sandusky, Ohio
Am Fam Physician. 2011 Jul 15 84:183-190.
Insulin therapy is recommended for patients with type 2 diabetes mellitus and an initial A1C level greater than 9 percent, or if diabetes is uncontrolled despite optimal oral glycemic therapy. Insulin therapy may be initiated as augmentation, starting at 0.3 unit per kg, or as replacement, starting at 0.6 to 1.0 unit per kg. When using replacement therapy, 50 percent of the total daily insulin dose is given as basal, and 50 percent as bolus, divided up before breakfast, lunch, and dinner. Augmentation therapy can include basal or bolus insulin. Replacement therapy includes basal-bolus insulin and correction or premixed insulin. Glucose control, adverse effects, cost, adherence, and quality of life need to be considered when choosing therapy. Metformin should be continued if possible because it is proven to reduce all-cause mortality and cardiovascular events in overweight patients with diabetes. In a study comparing premixed, bolus, and basal insulin, hypoglycemia was more common with premixed and bolus insulin, and weight gain was more common with bolus insulin. Titration of insulin over time is critical to improving glycemic control and preventing diabetes-related complications.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Analogue insulin is as effective as human insulin but is associated with less postprandial hyperglycemia and delayed hypoglycemia.
Don’t Miss: When To Take Basal Insulin
Insulin Starting For Type 2 Diabetes
Most people with type 2 diabetes are able to control their blood glucose with oral diabetes medications , healthy eating and regular exercise. With time, some people with type 2 diabetes will need to also use insulin injections with their tablets.
This can improve control of blood glucose levels and reduce the risk of developing complications.
Insulin helps to move the glucose from your blood into your cells to give you energy. When you have type 2 diabetes your body has stopped making its own insulin or your body has stopped using what you make.