How Is Afrezza Different From Injectable Insulins
Compared to injected mealtime insulin, Afrezza has a very fast onset and fast offset . Its blood-glucose-lowering action peaks just 12 minutes after inhaling, compared to over 30 minutes for typical rapid-acting mealtime insulins like Humalog and Novolog. Afrezzas blood-glucose-lowering action stops after 1.5-2 hours, while injectables can take upwards of four hours.
Mr. Harmel was a study coordinator for the STAT trial, which compared Afrezza to Novolog in people with type 1 diabetes. Compared to the participants on Novolog, Afrezza users experienced impressive benefits!
- Time-in-range was nearly 63% with Afrezza and just under 54% with Novolog. This translated to approximately two more hours per day of time-in-range – wow!
- Afrezza users experienced lower post-meal blood sugar spikes at one and two hours after meals. At one hour, Afrezza users had a blood sugar that was 38 mg/dl lower than Novolog users. At two hours, Afrezza users were still 18 mg/dl lower.
- Four times less time spent at under 50 mg/dl each day: three minutes with Afrezza vs. 12 minutes with Novolog.
There are other benefits to Afrezzas faster-acting profile: you can take it at the same time you start eating, rather than injecting 15-20 minutes before and since it clears out of your bloodstream quicker than other insulin, the risk of low blood sugar late after meals is much lower.
Intranasal Insulin Therapy: Brief Overview
Intranasal therapy uses inhalers as the mode to transport medicine and supplements. In this case, insulin is administered. Therapy is integral for people with Type 1 diabetes. And, for some people with diabetes with Type 2 diabetes, too.
In most cases, insulin is injected into the body. Injection pens, pumps, and patches are some of the ways diabetics take insulin. But, an intranasal avenue may be a less invasive way to receive therapy. Especially for those patients who dont like needles.
Role Of Basal Insulin In T2dm Treatment
According to the current American Diabetes Association Standards of Medical Care in Diabetes, insulin can be started at any point, even upon diagnosis, depending on the patients hemoglobin A1C level.3 After failure of lifestyle modifications, metformin should be initiated and titrated to an optimal dosage of 2,000 mg per day to provide enhanced glycemic control as well as the cardiovascular benefits established by the United Kingdom Prospective Diabetes Study.4-6 If the patients A1C is > 9% or remains above goal after 2 to 3 months on optimally dosed metformin therapy, then dual therapy with any other diabetes agent, including insulin, may be initiated. If a patients A1C is > 10% upon diagnosis, basal insulin should be initiated in addition to lifestyle modifications and metformin therapy. Prandial coverage with a single dose of bolus insulin at the patients largest meal or a glucagon-like peptide-1 receptor agonist may be added if the patient does not reach the A1C goal on basal therapy. After that, if glycemic control still has not been achieved, the patient should be advanced to a full basal-bolus regimen.3 It is important to note that the addition of insulin therapy should not be delayed, as earlier glycemic control has been shown to significantly reduce long-term cardiovascular complications and mortality risk.7
Also Check: What Blood Sugar Level Requires Insulin
Toujeo And Lantus: Efficacy And Safety
Insulin Glargine U-300 : A series of clinical trials compared concentrated insulin glargine U-300 with U-100 .20,22 Studies that included only patients with T2DM showed that concentrated U-300 demontrated no difference in A1C reductions compared with U-100 and no difference in rates of overall hypoglycemia, with the exception of patients on basal-bolus regimens.21,22 However, basal-bolus patients on U-300 exhibited a greater A1C reduction of 0.17% and less risk of hypoglycemia than patients on U-100.20 All study populations had a significantly lower risk of nocturnal hypoglycemia on U-300, ranging from a 16% RR reduction for patients on basal-bolus regimens and patients switched to U-300 on basal therapy alone , and up to a 24% RR in insulin-naïve patients .21,22 In addition, less weight gain was observed in patients on U-300, with an average of 0.42 kg gained in the U-300 group versus 1.14 kg gained in the U-100 group .21
Demographic And Baseline Cognitive Characteristics
Baseline group characteristics were similar per inclusion criteria . Baseline cognitive testing conducted on day 1 showed that the DM group performed worse than the control group on verbal learning measures , processing speed and executive function and had fewer years of education and lower global gray matter volume .
Read Also: Cinnamon For Diabetes Type 2
Cognition And Gait Outcomes
Primary outcomes were cognitive measures, NW and DTW speeds. The Cambridge Cognition computerized system was used to assess attention, memory and executive function using a battery of validated tests with parallel versions to reduce practice effects . Cognitive outcomes were converted to scaled z scores and summed to create composite measures .
The executive function composite score included the following: paired associates learning and spatial working memory . Lower score indicates better performance. Verbal memory composite score included verbal immediate free recall and immediate and delayed verbal recognition memory . Higher score indicates better performance.
Gait was measured during a 6 min walk at usual speed and 6 min dual-task walking using the Mobility Lab System . Gait speed was calculated from the total distance walked over six minutes in 45 m hallway, excluding turns.
Teplizumab’s Role In Delaying Onset Of Type 1 Diabetes
Please use one of the following formats to cite this article in your essay, paper or report:
-
Dr. Hena Mariam. . First Ever Drug Approved by FDA to Delay Onset of Type 1 Diabetes. Medindia. Retrieved on Nov 23, 2022 from https://www.medindia.net/news/healthwatch/first-ever-drug-approved-by-fda-to-delay-onset-of-type-1-diabetes-209364-1.htm.
-
Dr. Hena Mariam. “First Ever Drug Approved by FDA to Delay Onset of Type 1 Diabetes”. Medindia. Nov 23, 2022. < https://www.medindia.net/news/healthwatch/first-ever-drug-approved-by-fda-to-delay-onset-of-type-1-diabetes-209364-1.htm> .
-
Chicago
Dr. Hena Mariam. “First Ever Drug Approved by FDA to Delay Onset of Type 1 Diabetes”. Medindia. https://www.medindia.net/news/healthwatch/first-ever-drug-approved-by-fda-to-delay-onset-of-type-1-diabetes-209364-1.htm. .
-
Harvard
Dr. Hena Mariam. 2021. First Ever Drug Approved by FDA to Delay Onset of Type 1 Diabetes. Medindia, viewed Nov 23, 2022, https://www.medindia.net/news/healthwatch/first-ever-drug-approved-by-fda-to-delay-onset-of-type-1-diabetes-209364-1.htm.
Read Also: When To Take Basal Insulin
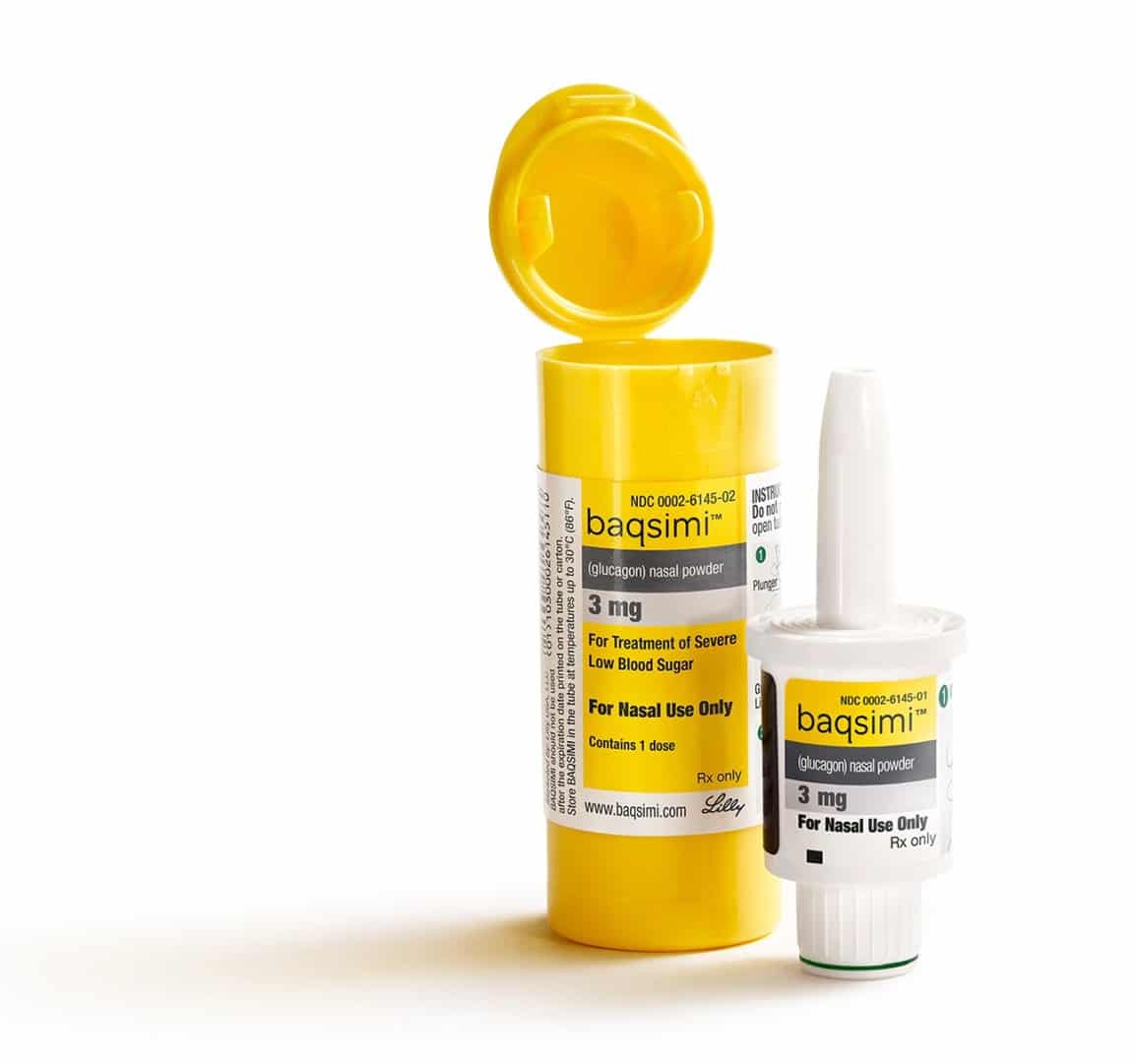
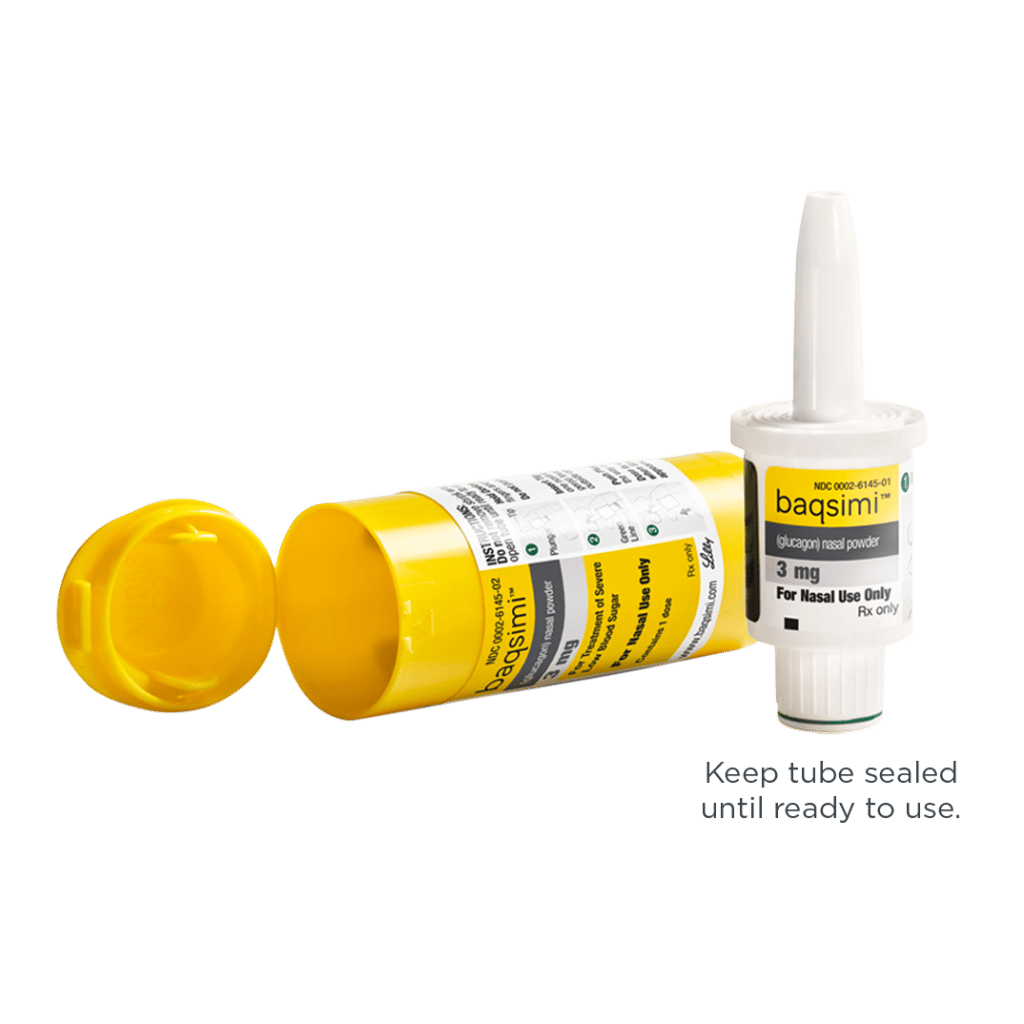
Insulin Dose Through The Nose
Dr Hamde Nazar from the University of Sunderland in the UK, who led the research said: “Our data highlights the potential of the formulation as a once-a-day dosage form for the delivery of insulin through the nasal route. However, its relative merit for the treatment of the human diabetes condition can only be assessed in the clinic.”
Associations Between Perfusion Vasoreactivity And Cognition
In the whole cohort, cognitive performance on the BVMT and verbal fluency measures upon insulin administration was related to perfusion and vasodilatation within the MCA territory and specifically to the insular cortex that regulates attention-related task performance.
Across all subjects, perfusion increases after insulin administration within the MCA territory were associated with an improvement of BVMT T3, and for the BVMT delayed recall in the right MCA territory and also with vasodilatation in the insular cortex . After insulin administration in the DM group, better visuospatial memory correlated with vasodilatation in the MCA territory for immediate recall T2 , BVMT T3 , and total recall . These relationships were not observed after placebo administration, as shown in for total recall .
A similar trend was observed between BVMT immediate recall and total recall vasodilatation in the whole ACA territory . After insulin administration within the control group, better performance on BVMT immediate recall T3 was also related to MCA vasodilatation . This relationship between visuospatial memory and vasodilatation was not observed after placebo administration in either group.
Don’t Miss: Is Stevia Safe For Type 2 Diabetes
Going By The Rules Insulin Is Recommended For Type 1 Diabetes And Oral Medication Alone Or Incombination With Insulin For Type 2
Have you ever wondered why despite taking your pills/insulin on time, your blood sugar levels never seem to normalize? With India housing more than 70 million people with diabetes, there is an evergoing buzz on what choice to make to maintain your blood sugar levels. Checking with your doctor regularly is key to deciphering what is happening inside your body and what you can do to keep it healthy. Read ahead to know the basics and differences in the working of the two types of regimen insulin and oral diabetes medication that doctors around the world stick to for keeping blood sugar in control.
Diabetes is of two types: Type 1 and Type 2. Most people with diabetes fall in the second category.
Type 1 diabetes
This is the condition when the pancreas does not produce insulin, the hormone responsible to deliver blood sugar to different sites where it can be utilised as a source of energy. In the absence of insulin, blood sugar levels are shot up. The condition becomes lethal if not taken care of . If blood sugar levels drop below average, the state is called hypoglycemia. Prolonged hypoglycemia, when left unattended, would starve the brain, altering its functions. Effects could range from difficulty in focusing to extremes like seizures, coma, and death.
Type 2 diabetes
Weeks Of Exercise Restores Insulin Sensitivity
For the study, 21 healthy participants with overweight and obesity were enrolled in an 8-week supervised aerobic exercise program.
The cohort included 14 men and 7 women with a body mass index ranging from 27.5 to 45.5 kg/m2. The participants led sedentary lifestyles and were deemed at risk for developing type 2 diabetes.
Three times a week, participants were led through 1-hour endurance training sessions. Each session included a combination of cycling and walking to bring individuals up to 80% of their peak oxygen intake, or VO2 max.
Using functional MRI after administering an insulin nasal spray to each individual, researchers assessed their brain insulin sensitivity at the start of the study and after 8 weeks.
The exercise program increased insulin action in the brains striatum and strengthenedfunctional connections in the hippocampus to levels of people without overweight or obesity.
The researchers found that improved insulin sensitivity in the brain had positive effects on participants metabolism and reduced their sensations of hunger. Participants also decreased their amount of visceral fat, which further benefited their health.
Ryan Glatt, CPT, NBC-HWC, personal trainer and brain health coach for the Pacific Neuroscience Institute at Providence Saint Johns Health Center in Santa Monica, CA, not involved in the study, noted the following to MNT:
Also Check: Beat Type 2 Diabetes Diet
Where Did The Story Come From
The study was carried out by researchers from the Institute of Medical Research and the Royal Melbourne Hospital, both in Victoria, Australia, and the St Vincent de Paul Hospital and University Paris Descartes, both in Paris, France. It was funded by the National Health and Medical Research Council of Australia, by a Victoria State government grant and by Frances INSERM research programme. The study was published in the peer-reviewed medical journal Diabetes.
The studys findings were described inaccurately by the Daily Express. The newspapers assertion that researchers had developed a nasal spray vaccine that can stop children developing diabetes was not supported by the research, which looked at adults who already had a rare form of the condition.
Inclusion Criteria And Study Procedures
Eligible participants were 5085 years old and able to walk for six minutes. T2DM participants were treated with diet, non-insulin oral or injectable agents. Controls had fasting plasma glucose.
and hemoglobin A1c . Excluded were persons with T1DM, T2DM-IDDM , intolerance to insulin, history of severe hypoglycemia, more than one hypoglycemic episode during the entire study , dementia or mini mental state exam scores20, serious systemic diseases, recent hospitalizations or drug abuse. INI or placebo was added to participants routine medication regimen.
Study procedures consisted of a phone screen, on-site screening , baseline , and four assessments at 8 week intervals, three medication refill visits during 24 week treatment , and four assessments during 24 week post-treatment . Baseline and the first intervention assessment were done on the same day . Visit nine was at 1 week after visit eight, and it was replaced by a phone call in 2017. Assessment visits included fasting metabolic panels, anthropometrics, cognitive, functional and mood tests, NW and DTW , duration about 3 h. Baseline Charlson co-morbidity index used ICD-10 codes . Participants kept a diary of daily medication usage and weekly self-monitored blood glucose . Safety outcomes, AEs and medication adherence were assessed at each visit. The study physicians evaluated participants at baseline and any AE occurrence.
Don’t Miss: Signs Of Diabetes In Young Children
Diabetes + Dementia: Using Nasal Insulin To Improve Brain Function
Coverage of the ADA Scientific Sessions is brought to you by the ADA x BT1 Collab.
While obesity is usually associated with type 2 diabetes, the rates of obesity in people with type 1 diabetes are also rising, making this research relevant to both types. The research presented in this session spoke specifically about type 2 diabetes.
Presentation: Dementia and Diabetes: What Are the Causes and How Do We Prevent It?
Speakers at this ADA Scientific Sessions presentation included:Auriel Willette, Ph.D. , Vera Novak, Ph.D. , and Valory Pavlik, Ph.D. .
Experts in dementia and Alzheimers research expect the cost of managing and treating the growing population of those with these cognitive disorders to increase significantly over the coming decades.
- Global cost of treating dementia: $270 billion annually
- Expected cost by 2050: $1.1 trillion annually
With rising rates of obesity and type 2 diabetes, understanding the impact of these conditions on long-term brain health and function is critical.
If we are not able to reduce the cases of dementia, explained Auriel Willette, Ph.D., the United States Medicare program could go bankrupt.
Dementia is a catch-all term for a variety of cognitive conditions, but late-onset Alzheimers accounts for about 85% of the cases in the United States.
Defined in simplest terms by the shrinking of the brain, Alzheimers starts in the temporal lobes and progresses to the frontal and parietal lobes which leads to a massive loss in brain volume.
Women Of South Asian Origin May Be More Likely To Experience Gestational Diabetes Due To The Same Complex Genetics That Increases Their Chance Of Acquiring Type 2 Diabetes According To A Study
Topics
of South Asian origin may be more likely to experience gestational due to the same complex genetics that increases their chance of acquiring type 2 diabetes, according to a study.
The findings of the study were published in eLife.
The discovery may lead to new ways to identify who would benefit from interventions to prevent during pregnancy.
People of South Asian descent have an elevated risk of developing type 2 . in this group are also twice as likely to develop a condition called gestational diabetes during pregnancy than women of European descent. But why South Asians are at an increased risk of these two conditions is not currently clear.
“Only a handful of studies have looked at how genetic and environmental factors interact in gestational diabetes in South Asian women,” says lead author Amel Lamri, a research associate at McMaster University and Population Health Research Institute in Ontario, Canada. “None have looked at how the genes associated with type 2 diabetes may interact with environmental factors to contribute to gestational diabetes in South Asian women.”
“These results show that a higher type 2 diabetes polygenic risk score and a family history of diabetes are strongly and independently associated with gestational diabetes in women of South Asian descent,” explained Lamri.
You May Like: What Is The A1c Range For Type 2 Diabetes
Regional Perfusion And Vasoreactivity
Regionally, changes in perfusion and vasoreactivity after insulin administration were observed in the MCA territory, which contains the insular cortex and integrative areas for learning, memory, and language within the temporal and parietal lobes. Baseline perfusion was lower in the DM group in the insular cortex as compared with control subjects . In the DM group, perfusion in the right insular cortex increased after insulin administration compared with placebo. Voxel-based analyses have shown that increase of perfusion on insulin was greater in the DM group compared with the control group . Perfusion did not differ in other regions.
Restoring Brain Insulin Sensitivity
For people with diagnosed brain insulin resistance or those concerned they might have it based on their symptoms, exercise is linked to improved health in general.
Making a change away from a sedentary lifestyle is unlikely to cause harm but its a good idea to speak with your doctor first.
I always say to my patients to just start however they can that is the first and hardest step, Dr. Kausel said.
Make sure they enjoy the activity so they can sustain it long-term, and every week add 5 minutes to it until they can do it for at least 45 mins. The activity doesnt matter, the point is to move.
Dr. Ergin added that exercising to restore insulin sensitivity may feel like a daunting task, which is why its important to start slow and set realistic goals.
Every journey begins with a single step, Dr. Ergin said. A person might begin by walking for 20 minutes each day and gradually increasing the length and intensity of their workouts over time.
Dr. Ergin emphasized exercises that build muscle, such as lifting weights or using resistance bands, which may help improve insulin sensitivity.
To stay motivated and consistent with your workout routine, Dr. Ergin recommends creating a support system with friends or family members who are also working to improve their health.
By following these simple tips, anyone can begin working toward a healthier lifestyle, he said.
Also Check: Life Insurance For Diabetic Patients