When To See A Dermatologist
Diabetes can cause many other skin problems. Most skin problems are harmless, but even a minor one can become serious in people who have diabetes. A board-certified dermatologist can recognize skin problems due to diabetes and help you manage them.
Are all dermatologists board certified?
No. See what it takes to become board certified.
ImagesImage 1: Image Courtesy of Clark C. Otley, MD. All Rights Reserved
Images 3, 7, 8, 9: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2 from DermNetNZ
Some images used with permission of Journal of the American Academy of Dermatology
ReferencesCohen Sabban, EN. Cutaneous manifestations of diabetes mellitus from A to Z. Focus session presented at: 74th Annual Meeting of the American Academy of Dermatology March 4-8, 2016 Washington D.C.
Duff M, Demidova O, et al. Cutaneous manifestations of diabetes mellitus. Clinical Diabetes. 2015 33:40-8.
Kalus AA, Chien AJ, et al. Diabetes mellitus and other endocrine disorders. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine . McGraw Hill Medical, New York, 2008:1461-70.
McKinley-Grant L, Warnick M, et al. Cutaneous manifestations of systemic disease. In: Kelly AP and Taylor S. Dermatology for Skin of Color. . The McGraw-Hill Companies, Inc. China, 2009:481-4.
Morgan AJ and Schwartz RA. Diabetic dermopathy: A subtle sign with grave implications. J Am Acad Dermatol. 2008 58:447-51.
Is Diabetes Causing Your Skin Problems
Diabetes can affect every part of the human body, including the skin. Experts say that at least one-third of diabetic patients, in their lifetime, will have to deal with some kind of skin infection or the other. Such skin problems are sometimes the first sign that an individual has diabetes. Most of these skin conditions can be prevented or treated if diagnosed early.
Some of these skin problems are conditions anyone can have, but people suffering from diabetes may acquire these more easily. Other skin problems happen to people with diabetes. These include necrobiosis lipoidica diabeticorum, diabetic dermopathy, and diabetic blisters.
The Connection Between Diabetes And Itchy Skin
Diabetes can make the body lose too much fluid through urination and evaporation through the skin. The result: dry, itchy skin that can be bothersome and sometimes uncomfortable.
Itching, especially in the lower legs and feet, can also be caused by poor circulation, which is common with diabetes. Some people experience a skin reaction to their diabetes medication or insulin injections.
In addition, itching can be brought on by diabetes complications including nerve damage, kidney disease and liver disease. Certain medications for other health problems common in people with diabetes, such as high blood pressure and high cholesterol, can make the skin itchy, too.
Scientists suspect that those with type 2 diabetes may be vulnerable to itchy skin for yet another reason: Their skins barrier function is impaired. Exactly how and why this happens is still being studied.
Recommended Reading: When To Take Long Acting Insulin
Dry Skin Can Be Dangerous For Diabetics
Skin is an important barrier that protects the body from infection. Anthony says that people with diabetes really cant afford to have breaks in the skin. Having an intact barrier is really important. Kelly says, We think about dry skin and diabetes because dry skin can create openings in skin integrity that are a potential source of infection. With diabetes, the sugar in your blood could act as food for the infection and make it harder to heal.
What are the warning signs that your dry skin is about to turn from bad to worse?
Dog Diabetes Skin Problems
Mostly skin infection is the first symptom of underlying bad health conditions. Skin conditions in diabetes are alarming. Although they may not be an immediate emergency, you need to give special attention to their treatment. If you notice any slight change in color, luster, or texture of the skin, contact your vet.
A diabetic dog can get several skin conditions. Some of them are
Also Check: Safe Male Enhancement Pills For Diabetics
Skin Hydration: Avoiding The Progression
Dermocosmetic management through skin hydration and control of xerosis and callus symptoms are essential to avoid progression of skin lesions on DM patients . Regarding dermocosmetic approach, the most commonly used active ingredient is urea. In 2003, Schölermann et al. published the results of two studies with 10 % urea cream in dry skin treatment. In the first study, 603 patients with dry or extremely dry skin, of which 179 were DM patients, were treated with 10 % urea cream for 14 days, presenting a decrease on dryness, callosities and scaling compared to baseline. In the second study, 30 patients with diabetes and/or xerosis were treated in one foot with 10 % urea cream for 10 days, resulting in decreased callosities, dryness and scaling .
Federici et al. conducted a randomized controlled clinical trial with 40 type 2 DM patients who were allocated to receive urea 5 %, arginine and carnosine versus a glycerol-based emollient for 28 days. Patients treated with urea 5 %, arginine and carnosine presented an 89 % reduction on dryness according to DASI scale when compared to control emollient . Another study conducted with 54 type 1 and 2 DM patients treated with 10 % glycerin, 5 % urea, 1 % lactic acid and 8 % paraffin in an emulsion base versus placebo for 4 weeks also demonstrated a decrease of dryness and fissures and increased skin hydration on active-treated group .
Diabetic Blisters May Heal On Their Own
Its rare, but sometimes people with diabetes erupt in blisters . The blisters occur on the backs of fingers, hands, toes, feet, and sometimes on the legs or forearms. These skin sores resemble burn blisters. Having diabetic neuropathy puts you at higher risk of developing these blisters. Heres the good news: They are usually painless and heal on their own in a few weeks. Keeping blood glucose under control is the only treatment for this diabetes skin problem.
Also Check: Is Humalog A Fast Acting Insulin
How To Treat Blisters
- Don’t try to break or pop the blister. The skin that covers it protects it from infection.
- Gently wash the area with mild soap and warm water.
- Apply antibacterial ointment to the blister.
- Cover it with a cloth bandage or gauze pad. Secure that with hypoallergenic or paper tape.
- Change the bandage at least once a day.
- If the blister is on your foot and came from your shoes, wear a different pair until it heals.
Type 1 Diabetes Blood Sugar And Acne
The link between nutrition and acne has been investigated in numerous studies¹. As a result, a high-sugar diet has been linked to a greater risk of acne. Poorly controlled diabetes during adolescence, when pre-teens and teens sometimes find it difficult to accept their insulin treatment, may therefore cause more severe acne. And this acne may persist beyond the teenage years due to the hormonal problems that diabetes can cause. Watching what you eat, as well as your diabetes, can help limit these effects.
Don’t Miss: Protein Shake For Diabetic Patients
Why Diabetes Can Cause Dry Itchy Skin
Medical Review By: Richard Levine, MD
If you have diabetes, you may know it can affect your heart, kidneys and nerves, particularly if the disease is poorly controlled. But did you know it can also cause dry, itchy skin?
An estimated 79% of people who have diabetes mellitus, the most common form, experience skin issues such as dryness, itching and infections. These can develop at any point during the course of the disease. In some cases, they may even be the first sign that a person has diabetes.
Diabetes Can Cause Neuropathy
Diabetes can cause nerve damage called neuropathy, a common diabetes complication. Sometimes the damage causes a loss of sensation in the feet. If you step on something and injure your foot or develop a blister, you may not be able to feel it. An open skin sore called a foot ulcer can develop and could get infected. Take a look at your feet every day to make sure they are not injured in any way.
Also Check: Keto Diet Good For Type 2 Diabetes
Major Pathways On Skin Disorders In Dm
Skin disorders in DM patients are highly correlated with glycemic control. As an example, Foos et al. conducted a study with 403 DM patients in Brazil and evaluated their skin disorders and glycaemia control. Thus, the study demonstrated that 94 % of patients with inadequate glycaemia control had some skin disorder on the other hand, only 60 % of DM patients with adequate glycaemia control had some skin disorder .
DM affects the skin through several mechanisms, being hyperglycemia per se and AGEs the most well-described. Reaching pathological high levels of glycaemia strongly affects skin homeostasis by inhibiting keratinocyte proliferation and migration, protein biosynthesis, inducing endothelial cell apoptosis, decreasing nitric oxide synthesis and impairing phagocytosis and chemotaxis from several cells . Besides hyperglycemia induce direct damage, high glucose levels also induce AGE formation. AGEs are formed from glycation of proteins, lipids and nucleic acids that act in several pathways, inducing reactive oxygen species formation, impairing ROS clearance, as well as intra and extracellular proteins function, and inducing pro inflammatory cytokine through nuclear factor pathway .
Table summary of studies reporting skin disorders prevalence in DM 1 and DM 2 patients, with a subjects description , prevalence of skin condition and the most common skin condition in each study.
Open Sores And Wounds
Having high blood sugar for a long time can lead to poor circulation and nerve damage. You may have developed these if youve had uncontrolled diabetes for a long time.
Poor circulation and nerve damage can make it hard for your body to heal wounds. This is especially true on the feet. These open wounds are called diabetic ulcers.
Diabetes and feet
- Get immediate medical care for an open sore or wound.
- Work with your doctor to better control your diabetes.
Also Check: Good Glucose Reading Type 2 Diabetes
Dm Skin Disorders Progression And Potential Outcomes
An important variability on severity and potential outcomes is observed among skin disorders in DM. Early-stage skin disorders in DM, such as xerosis, callus and fissures, are usually neglected and frequently underdiagnosed . Lack of diagnosis and treatment on early-stage skin disorders can lead to clinical worsening, and progression to foot neuropathy, ulcers and even amputation . DM-induced neuropathy can reach sensory, motor and autonomic pathways, leading to different dermatologic conditions .
Fig. 1
Adapted from Boulton
Neuropathic foot ulcer pathophysiology. Neuropathic foot ulcer physiopathology pathways, with autonomic, motor and sensory neuropathies leading to foot neuropathy.
-
Sensory neuropathy: insensibility and decreased temperature sensation, affecting the sensibility on lesions .
-
Motor neuropathy: causes toe and gait deformity, leading to foot deformity and increased plantar pressure .
-
Autonomic neuropathy: leads to anhidrosis and vasodilation, causing dry skin, skin tears and fissures , also losing viscoelasticity .
All the neuropathies, alone or simultaneously, can lead to neuropathic foot ulcer, the most severe cutaneous lesion, in consequence of the poor healing potential of DM skin that frequently become infected, thus leading to amputation .
In conclusion, dermocosmetic strategy is an option to treat the biophysical alterations on DM skin, with efficacy on improving skin hydration, decreasing xerosis and scaling among other factors .
Why Does Diabetes Cause Dry Skin
Its not so much that diabetes itself causes dry skin — its the dehydration that results from poor blood sugar control. When your blood sugar level is high, that causes your body to lose fluid. In turn, that causes you to become dehydrated. The solution, of course, is to keep your blood sugar in check — which you want to do for many other reasons besides dry skin. So, control your diabetes, and you can control your dry skin! [There are good tips here if you want to add more: Diabetes may dry your skin because having high sugar levels in your blood causes your body to lose fluid, including moisture from your skin. Also, nerve damage caused by diabetes may interfere with your ability to perspire normally, lessening the amount of moisture on your skin. Dry skin can crack and become more prone to infection. To help keep your skin moist, avoid very hot showers and baths, use mild cleansers and apply moisturizer to your skin while it is still damp. Examine your skin daily, and if you notice any signs of infection, such as red or sore spots, see your doctor. Dry skin is a complication of diabetes. It is caused by high blood glucose levels in the blood which zap moisture away from the tissues such as the skin. Another cause of dry skin for a diabetic is due to poor circulation. Poor circulation can cause the sweat glands to slow down or even shut down. Without sweat to cool the skin, the skin becomes dry.Continue reading > >
You May Like: Can Diabetics Eat Mac And Cheese
Dryness Starts A Harmful Cycle
Diabetes makes people more prone to dry and itchy skin or infections. High blood sugar decreases the amount of fluid your body holds, leaving your skin parched and prickly. Nerve damage can also stifle your sweat response. As a result, your skin loses natural softness and moisture.
You may notice dry skin first on your legs, feet, and elbows, but it can occur anywhere on your body. Scratching can produce cracks, creating a way for bacteria and other germs to enter. Bacteria and fungi can also invade the glands of your eyelids, your hair follicles, the area around your nails, the spaces between your fingers and toes, and your armpits or groin, among other sites.
Harmful infections receive sustenance from blood sugar. Diabetics have generally weaker immune systems, making them less able to fight infections. Also, nerve damage and poor circulation slow tissue healing. As a result, people with diabetes often have more frequent and serious wounds and skin infections than people without the condition.
Infected tissues often burn, appear red or swollen, itch, or form blisters or scales. Talk with your doctor if you spot any of these signs. You may need prescription medicines such as the antifungal drug Diflucan to control an infection.
Diabetes And Your Skin
If you notice any unusual changes in your skin, it’s important to see your doctor. Early diagnosis and treatment are key to preventing serious complications.
Did you know that diabetes can affect many parts of your body, including your skin? In fact, skin changes are one of the most common signs of diabetes. Learn about the signs of diabetes that can appear on your skin.
The skin is the largest organ of the human body. Its packed with nerves and blood vessels that allow us to sense touch, temperature, pain, and pressure. Diabetes can affect the nerves and blood vessels in your body, including those in your skin. Changes in your skin can be a sign that something is going on beneath the surface.
When diabetes affects your skin, its often a sign that your blood sugar levels are too high over time. Some skin changes can appear even before youve been diagnosed with diabetes. Others could be a sign that your diabetes treatment needs to be adjusted. Either way, youll want to make an appointment with a doctor to be screened for diabetes or to talk about adjusting your treatment. They can help you prevent serious complications with your skin and other parts of your body.
Keep reading to learn about 9 skin conditions that can occur with diabetes and what you can do to treat or prevent them.
Recommended Reading: How To Count Carbs For Type 1 Diabetes
How Diabetes Affects Skin Health
Diabetes skin problems are a common complication of both type 1 diabetes and type 2 diabetes approximately a third of patients with diabetes will develop a skin disorder related to the disease at some point during their lifetime. Many skin complications, such as certain types of rashes and blisters, can directly manifest from diabetes or allergic reactions to insulin or diabetes medications. Other types of skin problems, such as fungal infections, skin irritation, and dry skin, can occur in otherwise healthy patients but tend to affect those with diabetes more frequently.
Hyperglycemia is behind most skin problems caused by diabetes. An excessive amount of sugar in the blood prompts the body to pull fluid from other cells to produce an adequate amount of urine to remove the sugar, resulting in xerosis . Skin that is dry, inflamed, and irritated can likewise result from diabetic neuropathy a result of nerve damage, particularly in the feet and legs. Early diagnosis and treatment from an experienced skin specialist are key to dealing with diabetes-related skin conditions, managing resulting symptoms, and preventing other health complications.
What Does A Diabetes Rash Look Like
Diabetes rashes look different depending on the type and cause.
Some diabetes rashes only affect people with diabetes. They usually go away when blood sugar is under control. These rashes include:
- Blisters : Painless blisters may form on the backs of hands and feet and on the legs and forearms. This rare condition most often affects people who have diabetes-related neuropathy.
- Diabetes-related dermopathy: Light-brown, round-shaped scaly patches, like age spots, appear on the shins. These harmless spots dont need treatment.
- Digital sclerosis: Some people with Type 1 diabetes develop hardened, thick, waxy skin on the backs of their hands. The finger joints stiffen, making movement difficult. A related rash is scleredema adultorum of Bushke which is tightness, thickening, and hardening of the back, neck, shoulders and face. There are various treatments that dermatologists can provide for this.
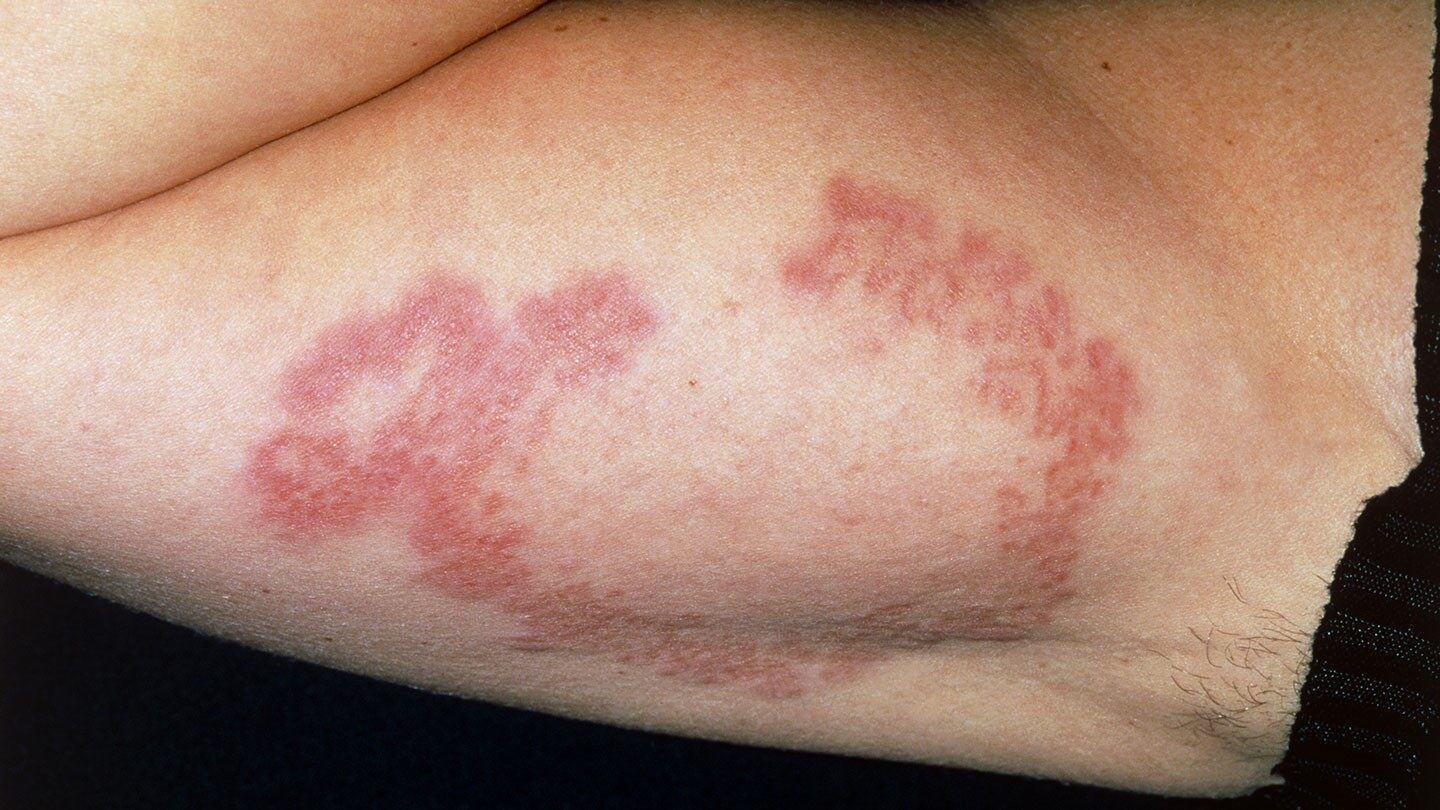
- Necrobiosis lipoidica diabeticorum : This lower leg rash is more common in women. NLD causes raised, red, shiny patches with a yellow center. Blood vessels may be more noticeable. The rash may be itchy and painful. You should see a dermatologist for treatment options.
- Diabetes Foot Syndrome: These are ulcers that develop from trauma to the skin. The ulcers can take a long time to heal and there is an increased risk for infection.
Also Check: 1000 Calorie Diabetic Diet Plan