Diabetes And Pancreatic Cancer
Pancreatic cancer is a type of cancer that starts in the pancreas. Type 2 diabetes can have a link to it as either something that raises your risk of having it or as a symptom.
If you have type 2 diabetes, you’re up to twice as likely to have pancreatic cancer as someone who doesn’t have the condition. It’s more likely to happen if youâve had diabetes for a while — 5 years or longer — than if you donât have it at all. If you have pancreatic cancer, but have had type 2 for less than 5 years, research hasn’t figured out if the disease plays a role in the cancer or if the abnormal cells cause the diabetes.
It’s rare, but pancreatic cancer can also cause diabetes, because it destroys the cells in the organ that make insulin. If you get type 2 diabetes when you’re over age 50, it may be a symptom of pancreatic cancer. If you had it before this age, it could be a red flag if your blood sugar levels suddenly change after you’ve had them under control. Symptoms of this type of cancer don’t usually happen until its later stages.
If doctors have taken out all or part of your pancreas to treat your pancreatic cancer , you can’t make insulin anymore, and you’ll end up with diabetes.
Several things make it more likely that you’ll get pancreatic cancer. You can change some of them, but others are out of your control. They include:
Show Sources
The Tech Solves The Night
One of the biggest challenges reported by families of young children with type 1 diabetes is poor sleep quality, as variability in insulin requirements and parental fear of hypoglycaemia are highest overnight. In their study, the researchers found that more than 80% of overnight sensor readings were within the target range, showing that hybrid closed-loop therapy addresses the night-time problem more effectively than sensor-augmented pump therapy.
When it comes to night-time, parents experience the terror of not knowing if their child will have secure blood sugar through those dark hours. This fear leads to poor sleep quality, as childhood differences in activity and food mean that insulin times change constantly. This change means parental fears of hypoglycaemia are highest overnight.
This study found that 80% of overnight readings were within the target range, putting parental fears at ease.
An Artificial Pancreas Could Soon Help Those People Living With Type 2 Diabetes Who Also Require Kidney Dialysis Tests Led By The University Of Cambridge And Inselspital University Hospital Of Bern Switzerland Show That The Device Can Help Patients Safely And Effectively Manage Their Blood Sugar Levels And Reduce The Risk Of Low Blood Sugar Levels
Patients living with type 2 diabetes and kidney failure are a particularly vulnerable group and managing their condition can be a challenge. Theres a real unmet need for new approaches to help them manage their condition safely and effectively
Charlotte Boughton
Diabetes is the most common cause of kidney failure, accounting for just under a third of cases. As the number of people living with type 2 diabetes increases, so too does the number of people requiring dialysis or a kidney transplant. Kidney failure increases the risk of hypoglycaemia and hyperglycaemia abnormally low or high levels of blood sugar respectively which in turn can cause complications from dizziness to falls and even to coma.
Managing diabetes in patients with kidney failure is challenging for both patients and healthcare professionals. Many aspects of their care are poorly understood, including targets for blood sugar levels and treatments. Most oral diabetes medications are not recommended for these patients, so insulin injections are the most commonly used diabetes therapy though optimal insulin dosing regimens are difficult to establish.
Unlike the artificial pancreas being used for type 1 diabetes, this version is a fully closed loop system whereas patients with type 1 diabetes need to tell their artificial pancreas that they are about to eat to allow adjustment of insulin, for example, with this new version they can leave the device to function entirely automatically.
Reference
Also Check: Type 2 Diabetes Blood Sugar Range
Artificial Pancreas Research In Cambridge
We fund artificial pancreas research in countries around the world, and each team brings its own expertise to the project.
One of these teams is led by University of Cambridge researcher Professor Roman Hovorka, a specialist in creating computer programs that mimic how the body works.
He is developing an artificial pancreas system, called CamAPS FX, that runs on an Android app.
Backed by 13 years of clinical research, the app first launched in March 2020 making it the worlds first licensed, downloadable artificial pancreas app for people with type 1 diabetes.
Hundreds Fitted With Artificial Pancreas In Nhs Type 1 Diabetes Trial
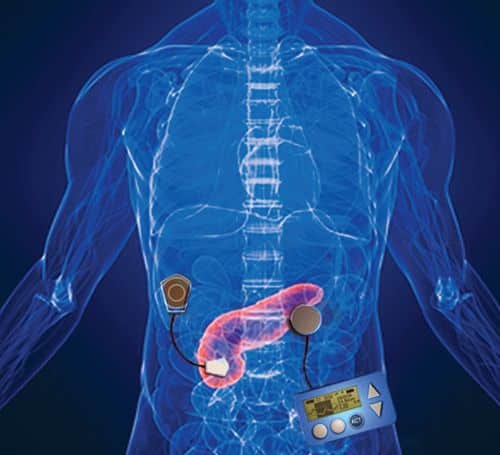
Adults and children wear device that monitors glucose level and adjusts amount of insulin delivered
Hundreds of adults and children with type 1 diabetes in England have been fitted with an artificial pancreas that experts say could become the holy grail for managing the disease, in a world-first trial on the NHS.
The groundbreaking device uses an algorithm to determine the amount of insulin that should be administered and reads blood sugar levels to keep them steady. The NHS trial has so far found the technology more effective at managing diabetes than current devices and that it requires far less input from patients.
Managing type 1 diabetes can be challenging, especially in young children, owing to variations in the levels of insulin required and unpredictability around how much patients eat and exercise. Children are particularly at risk of dangerously low blood sugar levels and high ones , which can damage the body or even lead to death.
Now a new artificial pancreas worn next to the body which continually monitors blood glucose levels and automatically adjusts insulin delivered via a pump is being tested in 30 NHS diabetes centres. About 875 people have benefited so far in the first nationwide study of its kind in the world.
Charlotte Abbott-Pierce, six, was diagnosed just over a year ago and initially started on insulin injections but has now become one of the first people to benefit from an artificial pancreas.
Also Check: Can You Diagnose Diabetes At Home
How Does The Niddk Support Artificial Pancreas Research
For more than 20 years, the NIDDK has funded technology to improve the lives of people with type 1 diabetes. Together with other federal government agencies and partner organizations, the NIDDK works to advance blood glucose monitoring, automate insulin delivery, and decrease complications of living with type 1 diabetes.
The NIDDK supports clinical trials to test artificial pancreas systems for children,3 adolescents,2,4 and adults4 with type 1 diabetes. New trials will test artificial pancreas systems in larger groups of people over longer periods of time.
Recent clinical trials funded by the NIDDK have shown that artificial pancreas systems control blood glucose levels better than other methods, especially through the nighta challenge for many people with type 1 diabetesand in children as young as 6 years old. Researchers continue to improve the design and components of artificial pancreas systems and to expand their use in different age groups and in real-life situations, such as during exercise.
What Is An Artificial Pancreas
An artificial pancreas is a system made of three parts that work together to mimic how a healthy pancreas controls blood glucose, also called blood sugar, in the body. An artificial pancreas is mainly used to help people with type 1 diabetes.
In type 1 diabetes, the pancreas does not produce insulin. People with type 1 diabetes control their blood glucose level by checking it and taking insulin, either by injection or through an insulin infusion pump, several times a day. An artificial pancreas automatically monitors your blood glucose level, calculates the amount of insulin you need at different points during the day, and delivers it.
Most artificial pancreas systems require you to count and enter the amount of carbohydrates you consume at mealtime. These are called hybrid artificial pancreas systems, because some of the insulin is given automatically and some is given based on the information you enter. These systems help control blood glucose levels throughout the day and night, making it easier for people with type 1 diabetes to keep their blood glucose level in range. Keeping blood glucose levels in range will prevent other health problems from developing and may improve daily life for people with type 1 diabetes.
Recommended Reading: Do Diabetics Have Skin Problems
What Is An Insulin Pump
An insulin pump is a device, about the size of a pager, that delivers insulin to the body through a catheter under the skin.
With most pumps, you have to manually adjust the rate at which they deliver insulin to the body.
This means regularly checking glucose levels using a fingerprick test, CGM, or flash glucose monitor and entering the data into the pump.
Artificial Pancreas For Type 1 Diabetes Patients
Type 1 diabetes requires constant monitoring. Patients need to check their blood sugar daily and adjust their medication and activities accordingly.
An artificial pancreas developed by researchers here at UVA could change that.
The system has two parts:
- A smartphone that uses an algorithm to automatically deliver the proper amount of insulin and control blood sugar levels
- An implanted insulin pump that receives blood sugar levels from the hand-held device every five minutes
Also Check: How Can I Check If I Have Diabetes
The Artificial Pancreas Or Closed Loop System
Hello, my name is Steven Green and Professor childs health at the London Diabetes Centre, London medical.
And Id like to just share with you some information around the new artificial pancreas systems, so called closed loop insulin pump, which were really quite interested in here at London medical as a way of treating type one diabetes, particularly in young people requiring insulin, intensive insulin therapy.
So closed loop systems, the concept has been around for a long time, and its been translated very much into practice in the last two to three years. And this is now gathering pace with several systems coming on board. Several new developments. Were particularly excited here at London medical about our relationship with the newest system which is out, which came out in April of this year, which came from Professor Romanov Walkers group in Cambridge. And this is the so called cam APS FX system, bit of a mouthful. This is the Cambridge, Artificial Pancreas System FX. Im not quite sure why theyve got such a complicated name, but its basically taking a standard insulin pump, in this case, a downer pump. Now in the future, they may well be able to link it to other pumps, but at the moment, its available with the downer insulin pump, which is very straightforward, very good, very safe insulin pump, and linking it to a continuous glucose monitoring system. In this case, the dexcom six continuous glucose monitor.
Future Directions In Closed
The past five to ten years have seen an explosion in research and published literature about closed-loop systems . Multiple further hybrid systems are expected to be commercialized in the near future, in addition to those already available. The DBLG1 has received the CE mark in Europe for use in adults with type 1 diabetes, while the Omnipod Horizon and insulin-only iLet are currently undergoing clinical trials . On the DIY front, Tidepool, the non-profit software organization responsible for Loop, has submitted an application to the United States Food and Drug Administration with the aim of releasing Loop as an FDA-regulated mobile application, supported by funding from the JDRF . Future directions in closed-loop research are principally aimed at the advanced generations of closed-loop systems as outlined by the JDRF: fully automated and multi-hormone systems.
Figure 4 A timeline of selected studies of closed-loop systems. CLS = closed-loop system HCLS = hybrid closed-loop system. References: Weinzimer et al., , Phillip et al., , Russell et al., , Thabit et al., , Bergenstal et al., , Stewart et al., , Kovatchev et al., , El-Khatib et al., , Brown et al., , Tauschmann et al., , Lal et al., .
You May Like: What Age Can You Get Type 2 Diabetes
Children Aged Between One To Seven
For 16 weeks, across seven places in the UK and Europe, a team examined how the hybrid closed-loop therapy with sensor-augmented pump therapy really worked.
They compared the artificial pancreas to a control treatment, which was just an insulin pump attached to a sensor.
The children, on average, spent 71.6% of their day in the target range for glucose levels when using the artificial pancreas via the CamAPS FX app. This is almost nine percentage points higher than the 16 weeks they spent on just the sensor-augmented pump.
That is essentially an extra 125 minutes per day in the target range.
The children also had less than a quarter of their time, 22.9%, with raised blood sugar levels while using the app. In the alternate therapy, these same children were in hyperglycaemia for nine more percentage points.
There was no difference in the time spent in hypoglycaemia.
Diabetes Smartphones And Robots: How An Artificial Pancreas Might Help People With Type 2 Diabetes And Kidney Failure
Managing blood glucose levels in people living with type 2 diabetes and kidney failure has historically been challenging. Good news, from an unlikely source, may be on the horizon.
A recent trial of an artificial pancreas has reported very positive results.
The technology, usually associated with managing type 1 diabetes, involves an external device that is made up of three components: a glucose sensor, a computer algorithm used to calculate insulin dosages, and an insulin pump. This is then connected to your smartphone. The software on your smartphone sends signals to the insulin pump to adjust the dosage as required.
The study, undertaken by the University of Cambridge and the University Hospital of Bern, Switzerland, shows that the use of an artificial pancreas device can safely and effectively help people with type 2 diabetes and kidney failure manage their blood glucose levels.
The study found that people using the artificial pancreas spent an additional 3.5 hours a day in the target blood glucose range. The study also found that the benefits of the device improved over time, as the computer algorithm adapted to the unique needs of the wearer.
An artificial pancreas should allow the wearer more freedom, as it means simpler management of blood glucose levels. At the end of the study, most users reported spending less time managing their diabetes, and less time being concerned about their blood glucose levels.
Read Also: Is Diabetes Considered A Disability Under Ada
An Artificial Pancreas Could Soon Help People Living With Type 2 Diabetes And Who Also Require Kidney Dialysis Tests Show That The Device Can Help Patients Safely And Effectively Manage Their Blood Sugar Levels And Reduce The Risk Of Low Blood Sugar Levels
An artificial pancreas could soon help people living with type 2 diabetes and who also require kidney dialysis. Tests led by the University of Cambridge and Inselspital, University Hospital of Bern, Switzerland, show that the device can help patients safely and effectively manage their blood sugar levels and reduce the risk of low blood sugar levels.
Diabetes is the most common cause of kidney failure, accounting for just under a third of cases. As the number of people living with type 2 diabetes increases, so too does the number of people requiring dialysis or a kidney transplant. Kidney failure increases the risk of hypoglycaemia and hyperglycaemia abnormally low or high levels of blood sugar respectively which in turn can cause complications from dizziness to falls and even to coma.
Managing diabetes in patients with kidney failure is challenging for both patients and healthcare professionals. Many aspects of their care are poorly understood, includingtargets for blood sugar levels and treatments. Most oral diabetes medications are not recommended for these patients, so insulin injections are the most commonly used diabetes therapy though optimal insulin dosing regimens are difficult to establish.
Mean blood sugar levels were lower with the artificial pancreas . The artificial pancreas reduced the amount of time patients spent with potentially dangerously low blood sugar levels, or hypos.
This story is republished here under a Creative Commons Licence.
Complications Of Type 1 Diabetes
Type 1 diabetes could affect the human body’s major organs over time. High blood glucose levels lead to various complications involving the heart, kidneys, eyes, blood vessels, and nerves.
Blood vessel and heart diseases
The complications involving the blood vessels and heart include coronary artery disease with angina , heart attack, stroke, atherosclerosis , and high blood pressure.
Nephropathy or kidney damage
High glucose levels in the blood could damage the kidneys over time and lead to end-stage kidney diseases. The treatment options for end-stage kidney diseases are dialysis and kidney transplant.
Eye damage
Diabetes can cause serious eye damage like diabetic retinopathy leading to blindness, cataract, and glaucoma.
Neuropathy or nerve damage
Injury to the walls of the capillaries that feed the nerves causes numbness, tingling, and pain or burning sensation. These sensations commonly begin at the tip of fingers and toes and move upwards. Failure to manage high blood glucose levels over some time could cause the loss of all sensations in the affected limb.
Mouth and skin diseases
Uncontrolled diabetes increases the risk of fungal and bacterial infections in the skin and mouth. Rashes, blisters, dry mouth, and gum diseases are common in patients.
Don’t Miss: What Is The Right Blood Sugar Level For A Diabetic
Mitigating The Effect Of Insulin When Hypoglycemia Is Projected
In the original controller of Albisser et al. , insulin was stopped and glucose infused to prevent hypoglycemia. This was possible since infusions were intravenous, which is not practicable long term. Alternately, automated subcutaneous glucagon administration has recently been implemented in a bihormonal controller, and preliminary data have demonstrated this to be effective at least under some conditions . As an alternative, Breton et al. have implemented a high level safety supervision module in their controller, which acts independently of the CTR modules and attenuates the infusion of insulin as a function of the risk of hypoglycemia. Alarms are also built in. Although the number of interventions by the SSM was not specified, clearly hypoglycemia is decreased relative to the degree of glycemic control, both for the sCTR and eCTR. Although it may degrade the optimization of, for example, the eCTR, the SSM is a critical and innovative modular approach to minimizing hypoglycemic events. The risk and possible extent of hypoglycemia can be extrapolated partly from estimates of insulin on board, or the amount of insulin accumulated in the three compartments of and their rates of removal.