Accuracy In Interstitial Fluid Glucose Monitoring
Interstitial fluid glucose monitoring device manufacturers often use mean absolute relative difference to describe performance. MARD for an ISF glucose monitoring device is calculated quite different from blood glucose meter accuracy. Its not possible to say a blood glucose meter and an interstitial glucose monitoring device are equally accurate because their relative accuracy is assessed differently.
For an analogy: the height of a building depends on the height of each story and the pitch of the roof. For this reason, not all five-storey buildings are the same height. The accuracy of an ISF device depends on its sensor chemistry, the algorithm it uses, its calibration, and the wearers body chemistry. Its tempting to compare a CGM reading with a blood glucose meter reading to get a sense of whether the CGM is right. If the numbers are pretty close, thats great if they are very far apart, its probably best to rely on the fingerstick meter result at that point in time.
The Devices That Passed Were:
-
Contour Next from Ascensia 100%
-
Gmate Smart from Philosys 71%
Get the full data and all the accuracy information here.
While all of these meters received FDA clearance at some point, this study shows that not all are equivalent in terms of accuracy. The FDA looks at company-reported trials when it reviews new meters this study took an independent look, purchasing the meters directly through retailers and testing them rigorously at respected research centers. It should be noted that the study’s standards for accuracy were even higher than FDA standards.
The results may be particularly frustrating for those on Medicare. According to , about 68% of the Medicare mail orders for BGMs in 2016 were for meters that did not pass the DTS standards. It is not yet clear how the FDA will respond to the reports of particularly low-accuracy meters such as the Advocate Redi-Code+ and the GmateSmart, which have been criticized for inaccuracy before.
On the other hand, it is encouraging that two store-brand value meters, Walmarts ReliOn Confirm and CVS Advanced, showed great accuracy in this study.
This study was funded by Abbott but developed and run independently. . Its not clear if DTS will get funding to run this study on an ongoing basis, ensuring the meters on the market are accurate and reliable. Dr. Joan Parkes, a co-author of the study, expressed her hope that manufacturers would support DTS in doing more of these studies.
How Does A Cgm Measure Glucose
A continuous glucose monitor sensor is painlessly implanted into your arm or upper stomach and can be worn continuously for 10-14 days. A small filament on the backside of the CGM sensor sits just below the skin. The filament tracks and records the glucose levels in the interstitial fluid .
The sensor takes a glucose reading every 5-15 minutes, even while you sleep. The data is sent via Bluetooth to your smartphone where you can review trends or any noteworthy changes in blood sugar levels.
Recommended Reading: How To Control High Diabetes
The Problem With Variance In Todays Glucose Meters
The biggest problem with variance in a blood sugar reading is when people are dosing insulin based on that reading. And 15 to 20 percent of a blood sugar level at 100 mg/dL means your blood sugar level may actually be at 120 mg/dL or 80 mg/dL. That variance is significant if youre taking insulin. A ¼ unit of rapid-acting insulin could correct a blood sugar of 120 mg/dL , bringing it down to 90 mg/dL. Take that same correction when your blood sugar is actually 80 mg/dL, and youll find yourself plummeting towards 50 mg/dL.
Factors Associated With Error Of Blood
In six studies, risk factors for inaccuracy of glucose measurements were determined . Patient’s factors , except for age, were not significantly related to inaccuracy. Young age was significantly associated with increased risk of nonagreement for Gluco-C in one study . No laboratory data were associated with inaccuracy.
Table 5 Risk factors for inaccuracy of glucose monitoring
For Gluco-C, low perfusion index , use of a vasopressor and presence of edema were significantly associated with inaccuracy. For Gluco-A, use of a vasopressor , low peripheral perfusion, and low mean arterial pressure were associated with inaccuracy.
Don’t Miss: What Fast Food Can A Diabetic Eat
How Test Strips Work
Diabetes test strips pack a lot of technology into a small space. The plastic strips are coated with a very thin layer of gold. The gold is cut into a pattern that becomes the stripâs circuit.
One end of the strip also has a coating of chemicals. They soak up your blood like a sponge and turn the glucose into electricity.
An electrical signal travels from the strip to the meter. The number you see on the meter is the speed of the electrical current. More blood sugar means a stronger signal. A stronger signal means a higher number on your blood glucose meter.
You May Like: What Insulin Pumps Are Covered By Medicaid
What Blood Glucose Meters Do
People with diabetes rely on blood glucose meters to monitor their blood glucose levels throughout the day and night. Those who inject insulin use them to determine how much insulin to take.
A system consists of a meter, which tends to run between $10 and $50, and test stripsa long-term cost that can really add up. Insurance companies often cover these items, but many people need to cover the expenses of an extra meter or strips out of pocket.
A person with an inaccurate blood glucose meter could overdose on insulin, which could excessively lower their blood sugar and bring on hypoglycemia. Hypoglycemia can cause you to feel dizzy, become unconscious, or even go into a coma. If people underdose, theyre at risk of hyperglycemia. Hyperglycemia can cause a host of long-term health effects, including kidney damage, nerve damage, and blindness.
Blood glucose meters can be lifesaving devices when used correctly. Blood glucose monitors have transformed the ability of people with diabetes to take optimal care of themselves, said Dr. Marrero. It was the dark ages before that.
Read Also: Ready Made Food For Diabetics
How To Check Accuracy Of Blood Glucose Meter
Blood glucose is measured in two different ways
How are these two different?
When it comes to a personal blood glucose meter, then the device draws blood from the fingertip and then after complete analysis, the results are produced.
But in the case of laboratory tests, blood is drawn from the veins, and then based on lab results, the clinical output is provided. Now, one of the most important questions here is which of the two tests is accurate?
Which of the above two is accurate?
Out of the above-mentioned two tests, the lab test is considered to be far more accurate. The reason is that it is performed under the guidance of a trained health expert and thus this test is far more accurate.
But both the tests have a slight margin of error. There can be a 15-20% of result difference in both the tests. And this is considered acceptable.
Although the truth is that any tests, done from two different sources or methods, will always have two different outputs. So, a slight margin of error is always considered to be acceptable.
In case your lab tests are showing a measurement of 100mg/dl of blood glucose, then your home tests can show up to 85-115 mg/dl.
Who determines this accuracy?
The blood glucose meter has the ISO accuracy standard of 15197:2013. A minimum of 95% of glucose test results must be within the 15% range.
8 Major factors that affects the Glucose Meter Accuracy
Our Suggestion
How Accurate Are Glucose & Ketone Meters
Blood glucose and ketone meters are extremely valuable tools if you have diabetes, follow the ketogenic diet, or simply want to improve your metabolic health.
While at-home meters arent as accurate as gold standard lab tests, theyre still accurate enough to ensure you make safe decisions about glucose managementand theyre also strictly regulated by the FDA and other governing bodies as medical devices.
If youre feeling doubtful about the accuracy of your meter, this guide has the facts to help put your mind at ease.
But just as importantly, youll also learn how to check your meter for accuracy using a control solution if necessary, as well as the most common factors that can cause inaccurate readings .
Keep reading to learn the truth about meter accuracy, how accuracy is defined, how at-home meters compare to lab tests, how to test accuracy, and more.
Recommended Reading: Homemade Protein Shakes For Diabetics
Also Check: How Often Should Diabetics Exercise
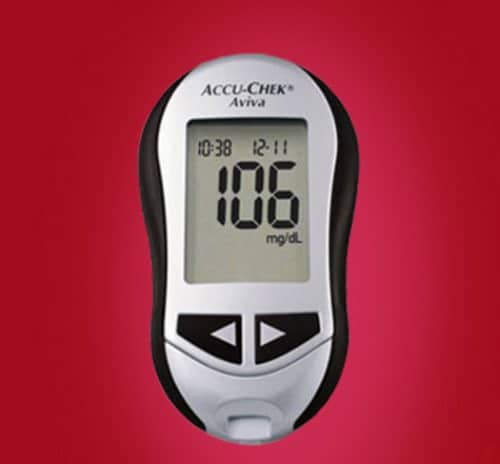
Blood Glucose Meter Calibration Quality And Coding
In order to trust the data your meter is providing you, make sure youre getting a quality meter. We discuss this more below, but manufacturers must meet certain standards to be considered accurate. If youre unsure about the quality of the meter, check for the latest updates and versions by the maker.
When you first set up your meter, follow the directions included with it. The calibration process can vary per manufacturer and meter. Finally, your meter will need to match a calibration code with the number on the test strip vial. Some meters are the exception to this. For example, with an Accu-Chek meter, theres no need to code it, so you have fewer steps in glucose testing.
You May Like: Antibiotic Cream For Diabetic Foot Ulcer
Types Of Glucometers And How To Choose The Best One
If you’re in the market for a glucometer , you’ve got choicesand lots of them. Aside from the two main types of glucometersbasic/standard and continuous monitoringthere are dozens of brands and models, each with a variety of features.
Certain glucometers may suit your needs better than others. For example, one may be more advantageous if you use insulin. But whatever you use, regular glucose testing can greatly reduce the risk of developing long-term complications of the disease.
Read on to learn more about the various types of monitors, how they work, and how to choose a glucometer so you can make an informed decision about which one to buy.
Read Also: How Do You Use Lantus Solostar Insulin Pen
A Crisis Of Accuracy Issues
In a 2014 statement, the American Association of Clinical Endocrinologists told the FDA, There is currently a crisis of post-market accuracy issues for blood glucose monitoring systems … Margins for accuracy are wide and reported in different ways, and the FDA does not test meters for accuracy either before or after they hit the market unless theres a widely reported problem.
If you test four times a day, you could get a completely useless reading at least once a week, and your meter would still meet the FDAs accuracy standards.
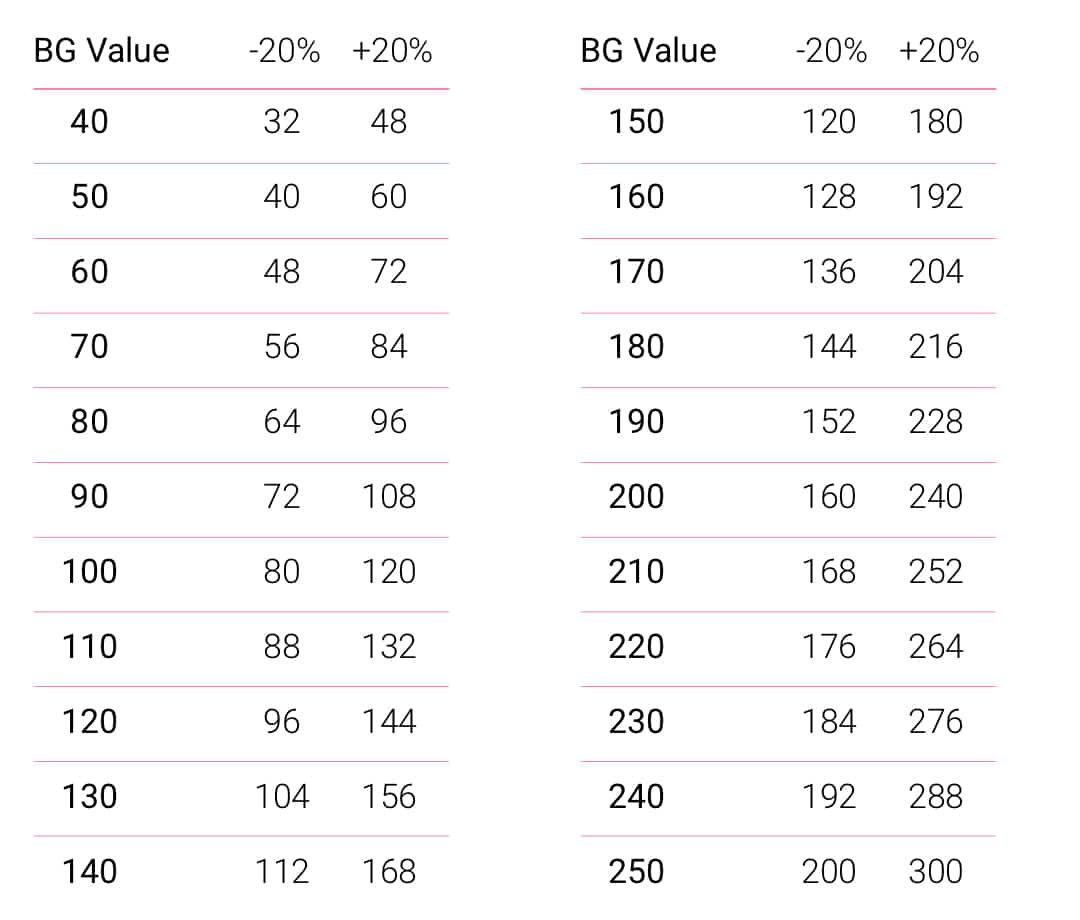
The FDA states that blood glucose meters readings must be accurate within 20 percent, 95 percent of the time for glucose levels above 75 mg/dl . For hypoglycemic levels , accuracy is less stringent: It must be within 15 points of the actual measurement .
This means if your actual blood sugar is 140 mg/dl, your blood glucose meter might tell you it measures 112 mg/dl, or 168 mg/dl. And up to 5 percent of the time, the reading can be completely wacky. If you test four times a day, you could get a completely useless reading at least once a week, and your meter would still meet the FDAs accuracy standards.
Beyond that, the margin for error gets wider: A 2015 literature review concluded that a quarter of the FDA-cleared blood glucose meters represented in those studies do not perform at the level for which they were cleared …
How You Prepare Before Pricking Your Finger
Especially among children , studies have found people with diabetes rarely wash their hands prior to glucose testing. Even if you werent recently touching food something that could easily lead to an inaccurate reading other things on your hands could potentially affect the accuracy. Hand lotion, ink from a newspaper, hair product, make-up, sweat, and even water after washing your hands if you dont dry them thoroughly.
Proper blood sugar checking technique for greatest accuracy:
- Wash your hands or use an alcohol swab on that finger
- Be sure your test strips are within their expiration date
- Use control solution to verify your strips and meter are reading within range
- Avoiding touching the end of the strip where blood will be applied
- Be sure to apply enough blood to completely fill the test strip
- Avoid testing in extremely hot or cold temperatures
- Be sure to completely close the test strip container to prevent humidity and other environmental factors from negatively impacting all of your strips
In real life diabetes management with type 1 diabetes or type 2 diabetes, its not always possible to control all of these variables. But keep in mind that if youre checking your blood sugar at the top of a mountain in New Mexico and your entire diabetes kit feels hot to the touch, your results may not be as accurate. The same goes for checking in the middle of a ski trip to Vermont when its 10 degrees outside!
Recommended Reading: How Does Diabetes Affect Your Eyesight
Average Margin Of Error For Cgms Vs Glucometers
Every blood glucose testing device will carry a different margin of error .
CGM
One comprehensive article published in European Endocrinology suggests that the MARD range across CGM devices on the market in 2018 is 9-15%11. For a reading to be considered 100% accurate, the MARD would need to fall between 3.3-5.3%11.
CGM technology continues to improve year by year, and future devices will offer even greater accuracy.
Fingerstick testing
Per FDA guidelines, a fingerstick blood testing device is expected to deliver readings with 95% accuracy2. This 2017 study published in the Journal of Diabetes Science and Technology reviewed several glucometers and observed a range of MARD from 5.6-20%3.
Why is there such a large range? Several factors can detract from the accuracy of fingerstick testing9:
- Using outdated or expired test strips
- Test strips can be damaged if exposed to light or air for an extended period
- Glucose meters need to be recalibrated before using new strips
- Missing a step in the manufacturer’s instructions
- Certain substances on the strips or on your hands may interfere with enzyme functioning2
Similar to CGM devices, there is great variability between individual fingerstick glucometer devices1. To truly get accurate results, the gold standard is to use a CGM device in conjunction with a blood glucometer.
Testing In Very Warm Or Very Cold Temperatures
Accuracy of blood glucose meters can be affected by temperature.
Blood glucose meters are designed to be at their most accurate at room temperature.
If you need to test in very warm or very cold temperatures, refer to your meters user guide to see what temperature range the meter is most accurate at.
Don’t Miss: 2 Hour Postprandial Glucose Normal Range
Most Accurate Blood Glucose Meters
Glucose meter accuracy has long been a hot topic of discussion. In a previous blog, Is my meter accurate, we discuss some of the technical details of meter accuracy. However, to us with diabetes, the accuracy of our meter becomes very personal.
According to the Diabetes Technology Society surveillance study in 2017, only 6 of the 18 meters passed the accepted standard of accuracy. Industry focus on accuracy resulted in the FDA issuing new guidance in October 2016. Meters cleared by the FDA before this guidance were not required to meet this guidance to continue to be sold. Even meters released after 2016 were allowed to bypass the requirement if they were substantially the same as previously cleared meters. New meters released after 2016 are required to meet the tighter 2016 guidance.
Fingerstick Blood Glucose Monitoring Vs Interstitial Fluid Glucose Monitoring
Traditional fingerstick blood glucose meters measure glucose in capillary blood. Flash glucose monitoring and continuous glucose monitoring devices are usually worn on the abdomen, upper buttock or back of the arm depending on the device where they measure glucose in interstitial fluid .
Capillary blood and ISF have different physiological characteristics. Changes in glucose levels will be seen more quickly in capillary blood . This phenomenon is often called lag. Interestingly, the lag between ISF glucose values and BG can vary between individuals, apart from the specific ISF glucose system they use. Algorithms in ISF glucose systems attempt to smooth out differences between the glucose values they detect and the expected BG value.
Recommended Reading: What Is The Earliest Sign Of Diabetes Nephropathy
How To Choose An Accurate Meter
Independent testing, like the study done by the Diabetes Technology Society, is helpful to compare the performance of top commercially available glucose meters. This study tested meters and test strips which were independently purchased from stores across the country, and representative of what a consumer would purchase.
After testing the products over 300 times at three different clinical sites, the results showed that over 66% of the top meters on the market today didnt pass the rigorous study.
A surprising number of name brand meters did not pass all studies. Check the list below to see the 12 meters that failed one or more study.
The following devices passed the test and received the Diabetes Technology Societys Seal of Approval:
Our Team Believes That Meters Should Be Within 10% Of Lab Values To Be Considered Accurate
One of the more important things you can do to ensure accurate results is to choose the right meter. Blood glucose meters vary widely in terms of accuracy. Accuracy is determined by comparing measurements obtained in a laboratory to the results obtained at the same time on the blood glucose meter. For example, if the lab generates a value of 100 mg/dl while the meter generates a reading of 110 mg/dl, there is a 10% difference between the results. If the lab result is 200 and the meter reading is 150, there is a 25% difference.
Our team believes that meters should be within 10% of lab values to be considered sufficiently accurate. The more often a meter falls within 10% of the lab value, the more reliable it will be.
Almost all meter manufacturers document their meters performance in the specifications section of the user guide. The chart below contains the accuracy figures for an assortment of commercially-available blood glucose meters, listed in order of how often they generate readings that are within 10% of lab values. Interestingly, alternate site monitoring tends to produce significantly less accurate results than fingerstick monitoring. This is likely due to the lag time inherent in alternate site testing similar to that seen with CGM.
Also Check: Does Metformin Lower Blood Sugar