Keep Your Nails Clean
Whether you have diabetes or not, neglecting your toenails unclean and unhygienic. It is not advisable for diabetic patients to trim their nails. But dont let this be an excuse for you to go on with unclean toenails, as bacteria could easily reproduce and reach your wound, leading to infection. There are doctors who specialize in foot care called podiatrists, and they will help you keep your foot maintained and your foot ulcer safe.
How Should A Diabetic Foot Ulcer Be Treated
The primary goal in the treatment of foot ulcers is to obtain healing as soon as possible. The faster the healing of the wound, the less chance for an infection.
There are several key factors in the appropriate treatment of a diabetic foot ulcer:
- Prevention of infection
- Taking the pressure off the area, called off-loading
- Removing dead skin and tissue, called debridement
- Applying medication or dressings to the ulcer
- Managing blood glucose and other health problems
Not all ulcers are infected however, if your podiatric physician diagnoses an infection, a treatment program of antibiotics, wound care, and possibly hospitalization will be necessary.
Preventing Infection
There are several important factors to keep an ulcer from becoming infected:
- Keep blood glucose levels under tight control
- Keep the ulcer clean and bandaged
- Cleanse the wound daily, using a wound dressing or bandage
- Do not walk barefoot
Off-Loading
For optimum healing, ulcers, especially those on the bottom of the foot, must be off-loaded. Patients may be asked to wear special footgear, or a brace, specialized castings, or use a wheelchair or crutches. These devices will reduce the pressure and irritation to the ulcer area and help to speed the healing process.
Applying Medication and Dressings
For a wound to heal there must be adequate circulation to the ulcerated area. Your podiatrist may order evaluation test such as noninvasive studies and or consult a vascular surgeon.
Managing Blood Glucose
Treatment For Diabetic Foot Ulcers
If a diabetic foot ulcer does occur, its important to seek medical care as soon as possible this is not a wound you should attempt to treat at home on your own. The faster a foot ulcer is properly treated, the greater chance it will heal completely and without infection or complications.
A diabetic wound care specialist, such as the Wound Care Center at Harrington, can provide the most advanced and comprehensive diabetic wound treatment. Your primary care physician can provide a referral to the wound care center. Our Wound Care Center team will then continue working hand-in-hand with your doctor throughout the wound treatment process.
Our specialized diabetic wound treatment services include:
Read Also: Number Of Grams Of Sugar Per Day For Diabetic
How Can Diabetic Foot Ulcers Be Prevented
Looking after your feet can help prevent foot ulcers and avoid serious complications. Good foot care includes checking your feet every day, keeping them clean and dry, wearing proper footwear and trying to avoid doing things that could damage them.
Get a foot check at every healthcare visit and seek urgent medical advice if you notice a cut, ulcer or other injury on your foot.
Learn more about diabetes and foot care.
How Does Diabetes Affect Wound Healing
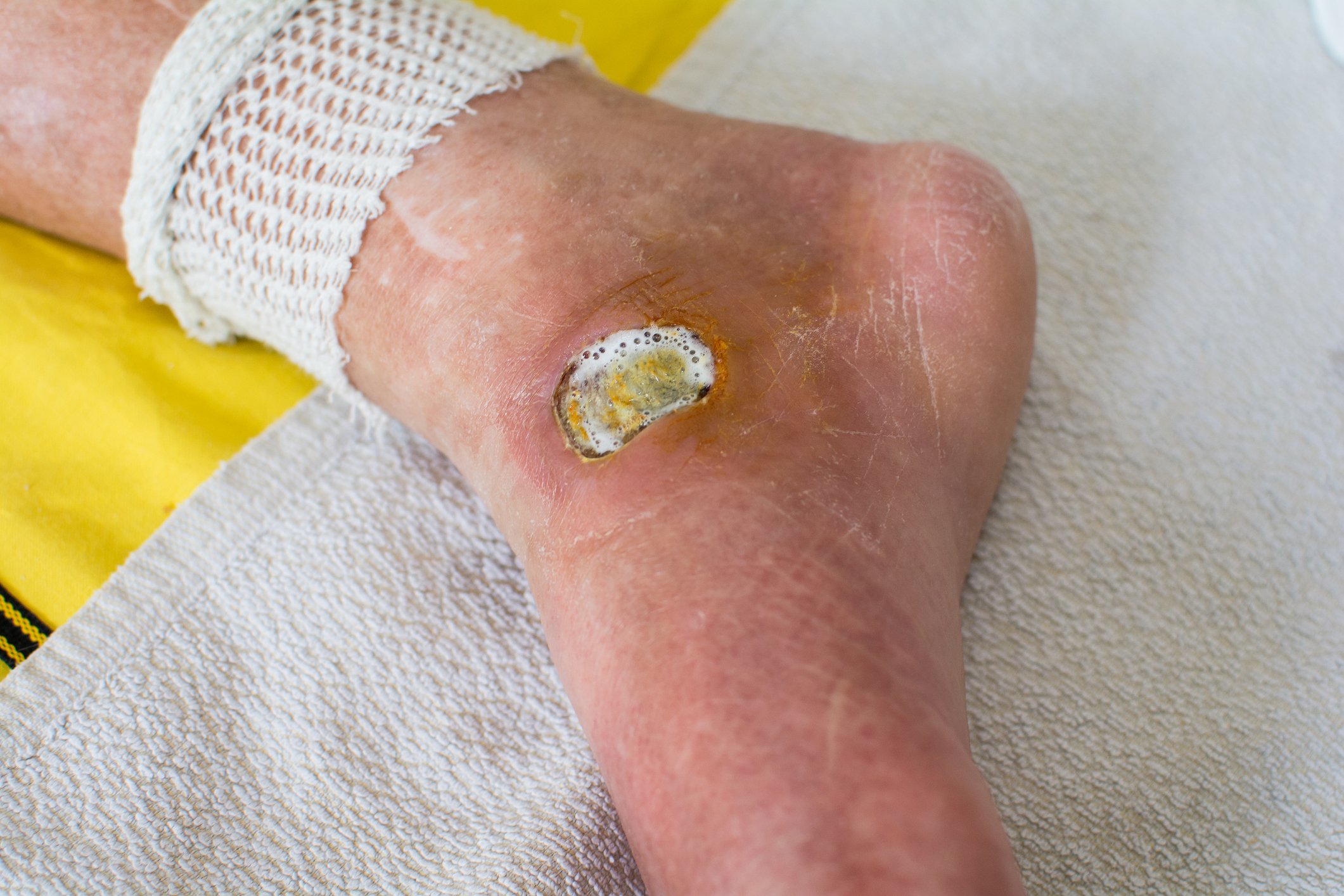
Diabetic ulcers and chronic wounds are made worse by prolonged periods of heightened blood sugar levels. High blood sugar leads to nerve damage and can impair the function of your blood vessels, thus restricting blood flow to your extremities. This reduction in blood flow leads to slower healing times and a higher risk for infection.
Read Also: Diabetes Kidney Failure Life Expectancy
Diabetic Leg Ulcers: Home Remedies To Heal Leg Sores
Among the more significant side effects of diabetes are diabetic leg ulcers, open leg sores that may afflict the feet or legs, once or recurrently, and break down the skin’s protective barrier so that infection may more easily enter the body to cause disease and further tissue damage at the site of the ulcer. These ulcers often occur with advanced diabetes because the diabetic patient does not feel the damage occurring to the skin, where neuropathy has affected pain receptors in the legs and feet.
There are other health concerns that can cause leg ulcers including trauma, impetigo, tuberculosis, and cellulitis. However, diabetic leg ulcers are the most common. These result from blocked arteries and as a secondary effect of the neuropathy that often comes with an uncontrolled diabetic condition. The atherosclerosis that blocks leg arteries causes arterial insufficiency, a lack of circulation to the area where ulcers subsequently occur.
> > > Click Here To Discover Which Breakfast Drink Could Be Increasing Your Diabetes And Why Its So Dangerous
Its important to maintain a healthy body weight. You should also make sure that you drink plenty of water, and limit your intake of sugary drinks. In addition, make sure that you get regular exercise. You should also avoid alcoholic beverages. Lastly, you should avoid alcohol. These beverages contain high amounts of sugar. If you dont drink enough, youre not doing anything to prevent diabetes. Besides, drinking alcohol can be harmful to your health.
The most important thing to do is to follow the recommended diet. Eat more healthy foods that have low amounts of fat and high amounts of fiber. The best way to lose weight is to lose 7 percent of your body weight. If youre overweight, you should try to lose 14 pounds to reduce your risk of developing type 2 diabetes. However, you should not attempt to lose weight while pregnant. Talk to your doctor about what kind of weight is safe for you.
Besides high blood glucose, diabetes can also affect the nerves and skin. It may affect your sexual response and your nervous system. It can also affect your fertility. Women with diabetes are more likely to miscarry or have a baby with a birth defect. It can cause a person to have difficulty hearing and sleep. If the condition is left untreated, it can lead to type 1 diabetes and can even lead to amputation.
Don’t Miss: Marijuana And Type 1 Diabetes
How Do You Treat A Diabetic Wound
People with diabetes have to take special care of their bodies, particularly their legs and feet. This is because diabetics are prone to wounds, and diabetic wounds take significantly longer to heal. The longer a wound takes to heal, the bigger the risk for it to get infected. If a diabetic develops a wound that does not heal or becomes infected, they are at a high risk of needing amputation.
According to the Centers for Disease Control , a high percentage of the 30 million diabetics in the United States suffer from complications due to wound infections. In order to protect yourself, its important to know how to treat a diabetic wound. Here are some tips.
Treatment For Diabetic Blisters
If you have diabetes, theres a good chance that infection and ulceration will occur. You could wish to have a dermatologist examine you for more serious skin diseases in light of the risk of infection and ulceration. Without treatment, diabetic sores generally heal in two to five weeks, according to Clinical Diabetes.
This will help maintain the skin as a covering for the injury since treating sores yourself could lead to shredded skin that does not act as an effective barrier.
Bandaging can be in use to protect sores from additional harm and treat them with antibiotic ointment or cream. If the itching is severe, your doctor may prescribe a steroidal lotion.
The most essential step you can take to avoid diabetic sores or speed their healing if you already have them is to maintain your blood sugar levels in control.
Don’t Miss: Diabetic Diet Plan To Lose Weight
Diabetic Wound Care & Treatment
Immediate wound care treatment is extremely important for people with diabetes, because an infection can lead to serious health problems. Always discuss any concerns you may have with your doctor and /or podiatrist, even for the care of minor wounds and skin cracks. Treat even small wounds as an emergency if you have diabetes. Here are some general guidelines for wound treatment:
TreatAntibiotic ointments can help prevent bacterial infection in minor cuts, scrapes, and burns. Follow the instructions of your doctor and/or podiatrist, and the directions on packaging when applying any antibiotic ointment.Keep an eye out for signs of bacterial infection until a cut, scrape, burn or ulcer is completely healed. These signs include:
- Tenderness
- Red streaks leading from the wound
- Throbbing
- Fever
- Itching
- Redness
- Small blisters and scales surrounding the redness.
Following these guidelines and continued adherence to a treatment plan from your doctor and/or podiatrist will help promote proper wound healing.
What Are The Signs And Symptoms Of Diabetic Foot Ulcers
Foot ulcers are open sores or wounds that occur most often on the ball of your foot or on the bottom of your big toe. They may also develop on the side of your foot, usually because of poorly fitting shoes. The ulcers are usually painless. Not all diabetic foot ulcers become infected but people with diabetes are at high risk of developing infection of the ulcer and the surrounding skin .
Depending on the severity of the wound and the presence of infection, diabetic foot ulcer can be classified in 4 ways:
- Uninfected the wound does not have signs of infection.
- Mild infection the area around the wound may be warm to the touch, red, slightly swollen, painful or tender, and the wound may ooze pus.
- Moderate infection foot infection that involves the deeper layers of your skin, into the muscle, tendons, bone or joints.
- Severe infection foot infection that causes . The symptoms of sepsis are high body temperature , fast heartbeat, and heavy or quick breathing.
Read Also: Surgical Treatment For Type 2 Diabetes
How Can Ulcers Be Prevented
Controlling risk factors can help you prevent ulcers from developing or getting worse. Here are some ways to reduce your risk factors:
- Quit smoking
- Manage your blood pressure
- Control your blood cholesterol and triglyceride levels by making dietary changes and taking medications as prescribed
- Limit your intake of sodium
- Manage your diabetes and other health conditions, if applicable
- Exercise â start a walking program after speaking with your doctor
- Lose weight if you are overweight
- Ask your doctor about aspirin therapy to prevent blood clots
Diabetic Foot Ulcer Symptoms
Normally a wound or sore on the skin would cause pain. But the same loss of feeling in the feet that often contributes to the development of a diabetic foot ulcer means that theres often no pain associated with the ulcer. This can make it difficult for people to realize that an ulcer is even there in the early stages, when treatment is most effective.
Aside from pain, another sign to look for is discharge or drainage from the wound in the socks. Ulcers that have been present for some time and that have become infected may also cause an unpleasant odor.
Read Also: Type 1 Diabetes Immune System
Diabetic Foot Ulcer: Treatment And Prevention
Estimates are that by 2030 there will be 550 million individuals with diabetes in the world. Because almost a quarter of all people with diabetes will develop a foot ulcer at some point, health care workers need to know the best practices for diabetic foot ulcer prevention and treatment.
Determining which diabetic foot ulcer type is important to determine an effective treatment. Here are the different types of these wounds:
- Neuropathic ulcers arise when the nerve damage from diabetic neuropathy causes the individual with diabetes to not feel pain from an injury, which often leads to the ulcer progressing substantially before the person is even aware of it. Foot and toe deformities, corns, calluses and areas repetitive stress are likely places of injury. Footwear can not only hide these issues, but can exacerbate the injury if the shoe is ill-fitting.
- Ischemic ulcers or arterial ulcers as they are sometimes called may occur due to lack of blood flow to the extremity. When an ulcer occurs as the result of an injury to the extremity, the lack of blood flow makes these ulcers difficult to heal.
- Neuroischemic ulcers occur in individuals with both neuropathy and poor arterial blood flow and are the most difficult to heal.
- Infected wounds occur in about half of patients with a diabetic foot ulcer and require particularly close care.
Wash Your Foot With Hot Water
Make sure that the water is at a bearable temperature, otherwise, youll risk scalding the skin, and thats one more thing to worry about. As bacteria are not capable of surviving in very warm temperatures, washing your foot in hot water will surely cleanse them. Not only that, but the heat can also loosen the veins in your foot, regulating blood circulation.
Also Check: Sure Comfort Insulin Syringes 30 Gauge
How To Help The Healing Process Along
To help the healing process along, follow these tips:
Do regular self-checks. Catching wounds early is the key to avoiding infections and complications. Make sure you do daily self-checks and look for new wounds, especially on your feet. Dont forget to check in between and under your toes.
Remove dead tissue. Necrosis and excess tissue often occur with diabetic wounds. This can promote bacteria and toxins and increase wound infection. It can also prevent you from being able to inspect the underlying tissue. Your doctor will often help you with the removal process.
Keep dressings fresh. Regularly changing dressings can help reduce bacteria and maintain appropriate moisture levels in the wound. Doctors often recommend special wound care dressings.
Keep pressure off the area. Pressure can cause wear and tear that damages the skin and leads to a deeper wound or ulcer.
If youre dealing with a foot wound, consider wearing white socks during the healing process. This will make it easier to see blood or other signs of drainage on your socks.
See your doctor if you experience any of the following:
- tingling
- persistent pain
- swelling
You should also see your doctor if your symptoms worsen or last longer than a week.
Evaluation And Treatment Of Diabetic Foot Ulcers
Ingrid Kruse, Steven Edelman Evaluation and Treatment of Diabetic Foot Ulcers. Clin Diabetes 1 April 2006 24 : 9193.
Diabetic foot problems, such as ulcerations, infections, and gangrene, are the most common cause of hospitalization among diabetic patients. Routine ulcer care, treatment of infections, amputations, and hospitalizations cost billions of dollars every year and place a tremendous burden on the health care system.
The average cost of healing a single ulcer is $8,000, that of an infected ulcer is $17,000, and that of a major amputation is $45,000. More than 80,000 amputations are performed each year on diabetic patients in the United States,and 50% of the people with amputations will develop ulcerations and infections in the contralateral limb within 18 months. An alarming 58% will have a contralateral amputation 3-5 years after the first amputation. In addition, the 3-year mortality after a first amputation has been estimated as high as 20-50%, and these numbers have not changed much in the past 30 years,despite huge advances in the medical and surgical treatment of patients with diabetes.
Recommended Reading: Can You Reverse Blindness From Diabetes
Promising Treatments For The Healing Of Diabetic Foot Ulcers
The number of Canadians with #diabetes is rapidly increasing. According to the Canadian Diabetes Association, more than 20 Canadians are diagnosed with the disease every hour of every day.
#Diabetic foot ulcers are the most common chronic complication from diabetes, affecting four to 10 per cent of patients. DFUs can last a year or longer and can happen again in up to 70 per cent of people who have previously been affected. Patients are more likely to develop DFUs if they have had diabetes for a long time, have poorly controlled blood sugar, have foot injuries or infection, are older, or smoke. However, neuropathy, damage to the nerves, which may result in a lack of feeling in the feet, and peripheral artery disease, which reduces the blood flow to the limbs, may be the most significant causes. Because of nerve damage and numbness, an individual with diabetes may not be aware that they have a sore or wound, leading to even minor injuries getting worse or becoming infected. Decreased blood flow caused by peripheral vascular disease may prevent healing once an injury occurs.
When DFUs become infected, the bone or skin can also become infected. This can lead to significant pain and suffering poor quality of life for patients amputation of a leg, foot, or toe increased treatment and hospitalization costs and can even lead to death.
Off-Loading Devices
Also Check: Dee Dee Blanchard Diabetes
What Is A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, and approximately 14 to 24 percent of patients with diabetes who develop a foot ulcer have an amputation. Research, however, has shown that the development of a foot ulcer is preventable.
Read Also: Is Keto Diet Safe For Type 1 Diabetes