Choosing The Right Cgm For You
Here are some details that might help you determine which CGM is best for you:
If youre looking for long-standing reputation and the authority of market share, Dexcom fits that bill. The longest player in CGM technology, Dexcom generally boasts the most accurate readings, within 9 percent of lab-measured glucose readings. With its G6 model, Dexcom offers high and low alerts, customizable alarms, data sharing, and a water-resistant device. Its not cheap, though.
Medtronics Guardian Connect is the most similar to Dexcoms line, and the costs are on par. The Guardian Connect is reportedly close in accuracy , although many patients claim that Dexcom seems more accurate in real-world settings.
The Guardian Connect offers increased connectivity, with data automatically uploaded into the companys Carelink app. That means your doctors can get your numbers without you having to do a thing. The predictive alerts are an interesting feature as well.
If youre looking for a CGM that tries to predict your bodys future, and minimizes the amount of work you need to do in retrieving your data, the Guardian Connect might be for you. This one isnt cheap either, and the sensors only last 7 days compared to Dexcoms 7-day wear.
Abbotts FreeStyle Libre brings cost effectiveness and streamlined design to the forefront. Its relatively cheap and accurate .
What Does Cgm Measure
CGM is a tool for people with diabetes. It measures your glucose levels 24 hours a day when you are wearing the device.
Insulin is a hormone that helps your body regulate blood sugar levels. If you have Type 1 diabetes, your body doesnt produce enough of the hormone insulin. In Type 2 diabetes, your body makes insulin but doesnt use it effectively.
People with diabetes need to give themselves insulin regularly to keep blood sugar levels steady.
How Do I Get A Cgm
As with most medical technology, you need a prescription to get a CGM. Your doctor can write a prescription for any of the above CGM devices.
But getting a prescription for a CGM is often not as simple as just walking into your doctors office and asking for one. Instead, youll likely need a prior authorization to get a CGM through your health insurance. A PA is form/process that your doctor has to go through to prove medical necessity to obtain approval from your insurance plan to cover the costs associated with the prescribed treatment .
At this point, most major insurers require a PA before extending coverage for CGM. Heres how to go about securing a PA, according to JDRF, a leading T1D research and support organization:
Recommended Reading: How To Test Glucose Levels
Can I Stop Doing Fingerstick Checks To Monitor My Blood Sugar If I Have A Cgm Device
No. Fingerstick checks will still be an essential tool for you to manage diabetes.
Because fingerstick checks measure glucose levels in your blood, they provide the best picture of what your glucose level is at the precise moment you take it. CGM measures glucose under your skin, which shows where your glucose levels were five to 10 minutes ago.
With diabetes, certain things can make glucose levels rise or fall quickly. Big or fast changes in blood glucose levels can be dangerous. Doing a fingerstick check can provide important information to help you take action to protect your health. It can also act as a backup tool to confirm CGM results.
How Does It Help Me Manage My Diabetes
CGM can sound an alarm if the glucose level is changing rapidly. A hypo or the trend towards a hypo can trigger an alarm alerting the user or family/carer to treat immediately. Hypo refers to hypoglycaemia, when the blood glucose level has dropped too low. Alerts can prevent a hypo before it happens and is particularly useful overnight when parents and children are in separate rooms.
Recommended Reading: Where Do You Give Insulin Injections
Why Do People With Diabetes Need To Track Blood Sugar Levels
Tracking blood glucose levels tells you how much insulin your body needs and when. Blood sugar levels that go up and down a lot can damage your body in different ways. Very high or low blood sugar levels can be serious, and even life-threatening when not treated quickly.
Many things can affect your blood sugar levels. But diabetes affects everyone differently. How a food or activity affects one persons glucose levels is often different from how that same thing affects someone else.
Your body can also be unpredictable. Sometimes, your body can have a reaction that even healthcare providers dont always understand. All of these factors can make managing diabetes challenging, even when you think youre doing everything right.
How Long Does A Continuous Glucose Monitor Last
Once applied, youâll wear the continuous glucose monitor for 10 days at a time. You can place a flexible band-aid-type cover thatâs soft yet durable on top of the sensor, and youâll barely notice the CGM is there. This waterproof patch is ideal for protecting the CGM against bumping, during sports, and when exercising intensely. Keep the continuous glucose monitor on at all times, including in the shower, when getting your sweat on, and when you sleep.
The sensor can stay in place between 10 and 14 days before it needs to be replaced. The exact duration depends on the manufacturer, but you will be alerted when itâs time to replace the sensor.
You May Like: How Do Glucose Test Strips Work
Who Can Use A Cgm
Most people who use CGMs have type 1 diabetes. Research is underway to learn how CGMs might help people with type 2 diabetes.
CGMs are approved for use by adults and children with a doctors prescription. Some models may be used for children as young as age 2. Your doctor may recommend a CGM if you or your child:
- are on intensive insulin therapy, also called tight blood sugar control
- have hypoglycemia unawareness
- often have high or low blood glucose
Your doctor may suggest using a CGM system all the time or only for a few days to help adjust your diabetes care plan.
References And Further Reading
Linklater, A. undated. Continuous Glucose Monitoring in Veterinary Patients. Todays Veterinary Practice . Available from:
Hammond-Lenzer, M. et al. 2019. Flash Glucose Monitoring with FreeStyle Libre in Cats and Dogs. VIN . Available from:
Fennell, C. 2020. How to place a FreeStyle Libre in veterinary patients. The Veterinary Nurse . Available from:
Koening, A. et al. 2016. Effect of sensor location in dogs on performance of an interstitial glucose monitor. Journal of American Veterinary Research, 77, pp. 805-817.
Hafner, M. et al. 2013. Evaluation of sensor sites for continuous glucose monitoring in cats with diabetes mellitus. Journal of Feline Medicine and Surgery, 15, pp. 117-123.
You May Like: What Eye Problems Does Diabetes Cause
No : Understand Your Clients Why
If one of your clients shares with you that theyre using a continuous glucose monitor, getting a sense of their motivation for using the device will help inform the nutrition strategy you create. For example, is your client in the prediabetic range and using the CGM to see which foods may be causing her elevated blood sugar? Or, was your client lured by an Instagram ad or magazine article, and invested in a month-long CGM experience to gain more insights about how her body is responding to the food shes eating and what changes she can make to lose weight? While the reasons your clients will use a CGM will vary, understanding their why? is an essential first step to devise a plan thatll help each client make the most of using a CGM, says Koff.
How Does A Continuous Glucose Monitor Work
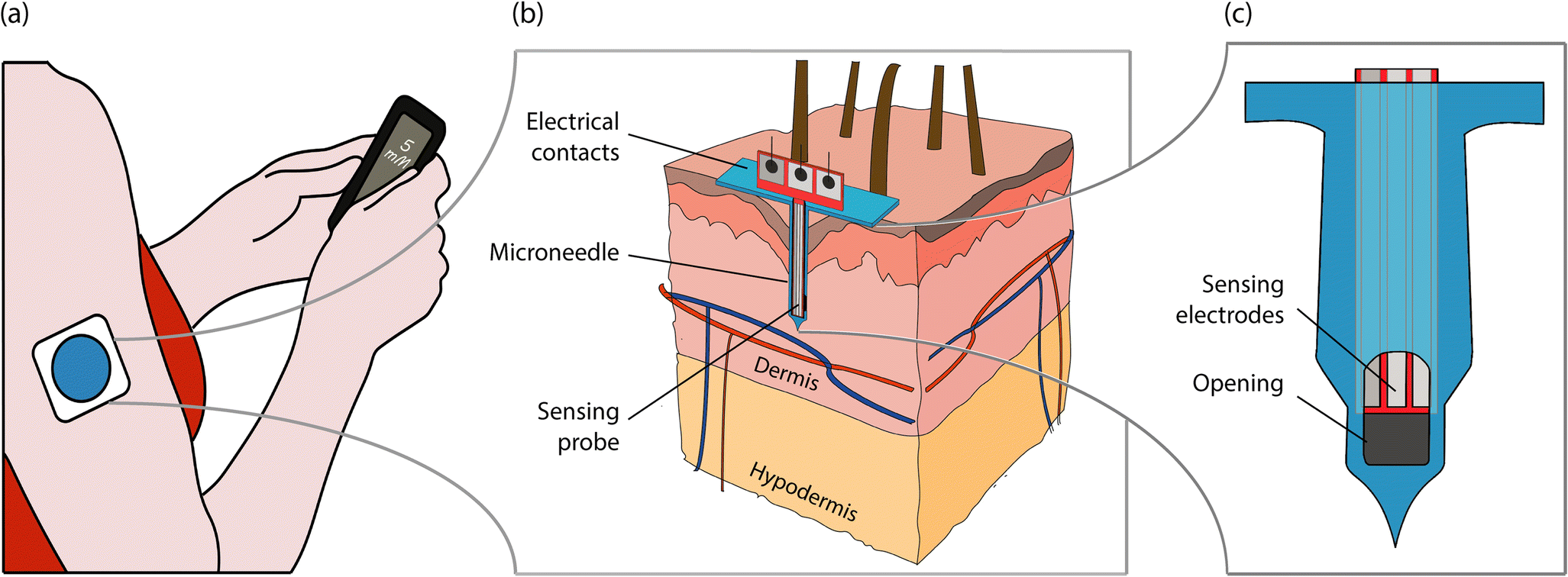
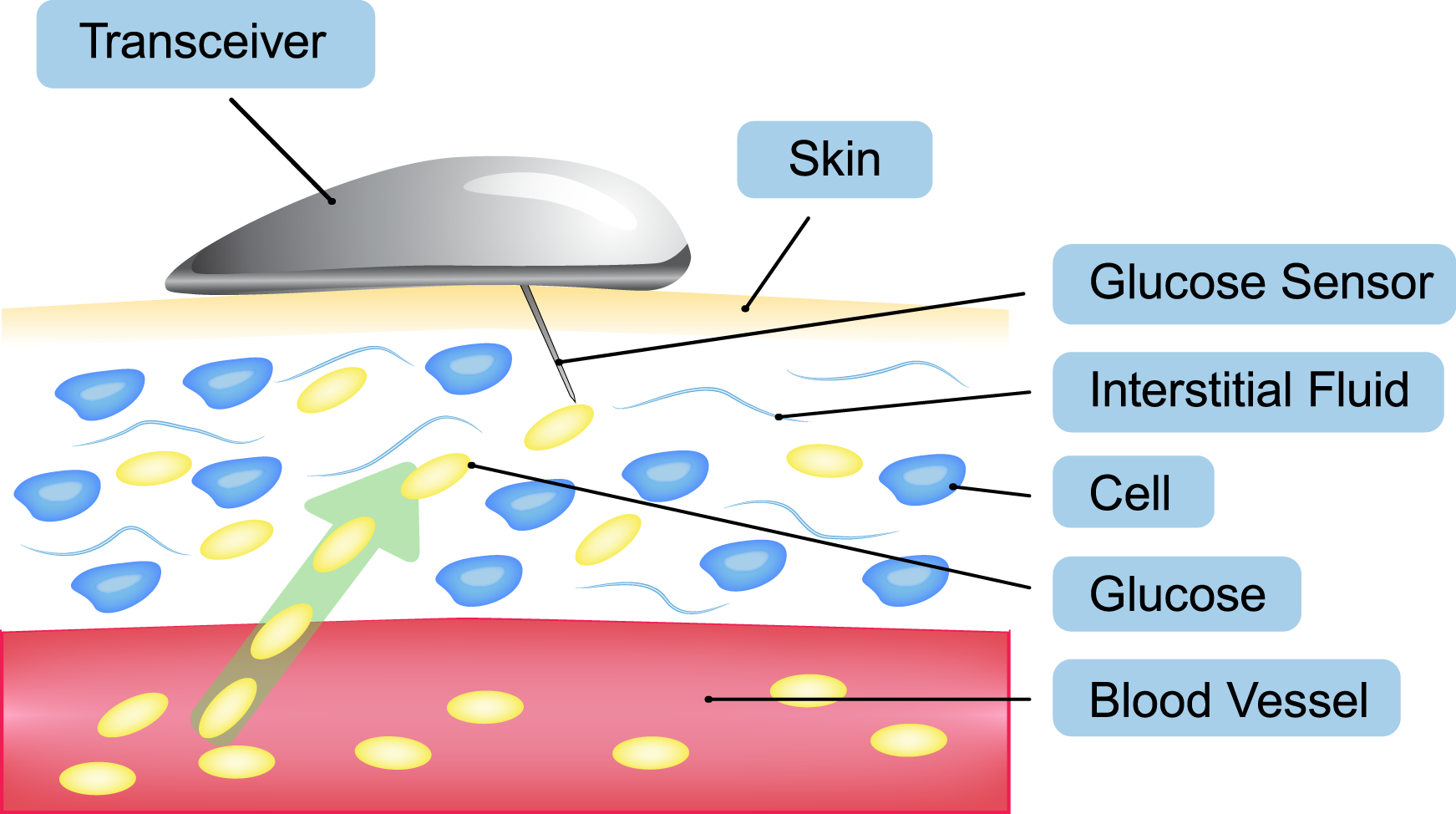
A CGM works through a tiny sensor inserted under your skin, usually on your belly or arm. The sensor measures your interstitial glucose level, which is the glucose found in the fluid between the cells. The sensor tests glucose every few minutes. A transmitter wirelessly sends the information to a monitor.
The monitor may be part of an insulin pump or a separate device, which you might carry in a pocket or purse. Some CGMs send information directly to a smartphone or tablet. Several models are available and are listed in the American Diabetes Associations product guide.
Also Check: Blood Sugar Goes Up Without Eating
No : Keep Personalizing By Adding Routine Reassessments
When youre working with clients who are using a CGM to manage Type 2 diabetes, reassessment and continual changes to their nutrition and medication plans are key. Excellent compliance often the result of using a CGM to actually see what their choices do often translates into the opportunity for a reduction in medication. Awesome sauce!
For clients who are using a CGM as more of an experiment, reassessment may not be as crucial medically speakingbut it is an incredibly important piece in helping people create a healthy relationship with food and to tee them up for nutrition success even when theyre not using a CGM.
The ultimate goal for your clients is to discover how all their choices work together, better, for their body. This takes time to implement recommendations and track their impact. Using a CGM, the Better Nutrition Journal, key evaluations, and labs help you personalize most effectively, says Koff. The business bonus is that this approach more easily sells packages and helps to ensure client retention. You can divide up your work together into phases: assessment, implementation, monitoring, and optimizing. Once youve identified a plan that works for them, move them to maintenance. During this phase you will revisit assessments like the digestive evaluation and repeat the CGM as a seasonal or annual offering.
Can I Still Do Sports With A Cgm
The easy answer to this question is yes!!
The CGM is such a great tool to have when you are doing sports!
Number one, it is waterproof so you can even go swimming with it on. There is even research proving safety and accuracy while scuba diving.
Number two, because you risk fluctuations of your blood sugars while exercising, you will maintain your safety by wearing your CGM. After strenuous or vigorous exercise, you are at risk of a high blood glucose initially due to spurts of adrenaline, then low blood sugars for many hour afterwards wearing your CGM will continue to keep you safe by alerting you to any deviations in blood glucose values.
Don’t Miss: What Is In Insulin Shots
What Are The Contraindications For Blood Glucose Monitoring
A comprehensive study of the effects of CGM conducted in 2013 by the German Diabetes Association revealed the following contraindications meaning these factors do not predict success with CGM devices:
-
lack of motivation and compliance
-
fear of technology/lack of trust in technology
-
alcohol and drug abuse
-
unrelated psychological conditions like psychoses or eating disorders
What About Health Insurance Coverage
Its helpful to know that the Dexcom G6, Abbott FreeStyle Libre 2, and Eversense implantable CGM are all covered by most private and public health insurance plans, including Medicare . Medtronics Guardian Connect, however, was not covered by Medicare as of December 2021.
Historically, people with type 1 diabetes have had a much easier time qualifying for a CGM through insurance than those with type 2 diabetes because it was easier to establish medical necessity.
Still, if you have T2D and your doctor can make a case for medical necessity, you may qualify. But your insurance company may still want to confirm whether you actually need a CGM.
If you can prove youre experiencing both high blood sugars and low blood sugars regularly, you will likely qualify. This can be proven by providing blood glucose logs uploaded from your fingerstick meter. Generally, hyperglycemia is defined as a blood glucose level of 250 mg/dL or over, while hypoglycemia is a blood sugar 70 mg/dL or below.
If your insurance company denies your coverage for a CGM, talk with your doctors office about peer-to-peer reviews and appeals. Pushing your doctor to fight for you matters.
Manufacturers can have your back here, too. Dexcom, for instance, has an easy-to-complete patient information form you can submit along with your insurance information. The company will then contact your insurer to work on getting your device authorized and covered. Medtronic offers a similar service.
Recommended Reading: Type 1 Diabetes Blurred Vision
Traveling With Your Cgm
When flying, TSA is very familiar with insulin pumps and continuous glucose monitoring systems. Just show them the device that you are wearing, tell them exactly what it is and show them your monitor. Ask that the monitor or sensors not be put through the x ray machine because they may become damaged from the x rays. The following excerpt was taken from Dexcom’s website regarding this important information:
X-Ray Machines
Receiver, Extra Sensors
Dont put your Dexcom G5® Mobile CGM System components through baggage x-ray machines. Before your screening process begins, ask the TSA Officer to perform a visual inspection of the receiver and your extra sensors. Place all Dexcom G5® Mobile components in a separate bag before handing over to the Security Officer. For other medical supplies, such as medications, meters, and strips, check manufacturers instructions or the TSA website.
to download our “Notice of Medical Device” letter. This can be filled out by your physician and presented to airport security to better explain your Dexcom CGM System.
Use of AIT body scanners has not been studied and therefore we recommend hand-wanding or full body pat down and visual inspection in those situations.
When Is It Used
A monitors is used to look for trends in glucose levels, like whats happening overnight or high blood sugar levels between meals, or early morning spikes in blood sugar.Its not meant to replace monitoring your blood sugars with a meter though. The main advantage of continuous glucose monitoring is that it can help identify fluctuations and trends that would otherwise go unnoticed with standard A1C tests and finger stick measurements, and allow you to take action to avoid severe highs or lows.
Don’t Miss: Healthy Snacks For Diabetic Kids
No : Personalize To Meet Their Needs
While a continuous glucose monitor reveals data about what is happening, it only gives you partial data on the why. Working with you, a patient can get the whole picture and thus make her truly better choices. For a type 2 diabetic, CGM data reveals that less oatmeal each morning would be better for her blood sugar. However, just reducing oatmeal intake isnt better overall. That reductions translates to less fiber, B vitamins and magnesium. With better nutrition assessments you can show her this shift. Your BNP Toolkit complements the CGM results to show her what to add not just subtract to truly optimize her total nutrition, says Koff.
Continuous Glucose Monitor Use For Diabetics
Diabetics either don’t make enough insulin or the insulin isnât as effective. This causes glucose to rise unchecked, leading to a host of serious health complications including heart disease, blindness, kidney failure, and lower-extremity amputations.
CGMs help diabetics monitor and manage their blood glucose. With a CGM, you can see trends and gain insight into the impact of meals, exercise, and illness on glucose levels. CGM wearers can be alerted when glucose spikes or drops outside of a specific range.
For diabetics, the American Diabetes Association suggests the following blood glucose targets:
- 80 to 130 mg/dL before eating
- < 180 mg/dL two hours after starting a meal
Continuous glucose monitors were created initially for diabetics and pre-diabetics to better manage their health by monitoring their blood glucose. Recent discoveries linking better blood sugar management to benefits like weight loss and increased energy are helping CGMs gain mainstream adoption.
You May Like: What Is Meant By Insulin
Dexcom Continuous Glucose Monitoring System
Dexcoms G5 Mobile CGM System recently gained FDA approval for making treatment decisions without using fingersticksin certain situations. You will still need to calibrate every 12 hours, if too low or too high of course, or if your blood glucose is changing rapidly. This approval does mark a change in the way people with a CGM will treat their diabetes, so it is quite remarkable.
How To Remove A Cgm Sensor

Sensor removal can be tricky, especially when patches are too sticky, or there is just simply too many of them. This is where the NJaP patches come to the rescue! Our CGM patches are not only useful to keep the sensor in place, but also to easily remove it after its job is done. We also wrote down some great tips on how to keep your sensor from falling off.
Also Check: How To Deal With Gestational Diabetes
Learning To Use Your Cgm Or Freestyle Libre
Your diabetes healthcare team will set you up with your CGM or Freestyle Libre if its free on the NHS and show you how to use it. Sometimes manufacturers will help you set up the technology this is fine and can help your healthcare team get more people on to the technology more quickly.
Abbott, which supply the FreeStyle Libre, also provide free online learning for people with diabetes using the technology to help them get the most from it.
You may also benefit from going on a diabetes education course if you use Flash or CGM. Ask your GP or other diabetes healthcare professional to refer you.
If you want to share your experiences about using tech or find out information by asking others using it, go to our forum.