Diabetes And Dental Health
As you are probably aware, diabetes is best managed with a team approach. Your team includes your diabetes medical providers , diabetes care and education specialists, dietitians, exercise experts, nurses, pharmacists, mental health professionals and, most importantly, you! But did you know that your team should also include dental specialists? It is important to establish an ongoing relationship with a dental hygienist and dentist for your oral health care. Your dental hygienist will conduct a professional cleaning and provide instruction on routine home care and cleaning to maintain or reestablish oral health, while your dentist will perform an oral examination and diagnose conditions such as cavities, gum disease, and yeast and/or fungal infections. As part of your care, you should also receive an oral cancer screening during a dental visit.
In fact, taking care of your mouth and teeth is a big part of your diabetes health. It is very important to make every effort to ensure you keep up your daily oral hygiene practices and schedule regular visits with your dentist and dental hygienist for cleanings and oral health checkups.
Results Of Dental Implant Therapy
Diabetes affects bone metabolism via multiple different mechanisms that may impair bone healing and normal homeostatic bone turnover . Elevated glucose levels may inhibit differentiation and proliferation of osteoblasts, with resulting decreased formation of bone matrix . Both type 1 and type 2 diabetes have been associated with increased risk of hip fracture, but HbA1c was not correlated with the rate of fractures . Animal studies have shown that osseointegration is impaired in animals with chemically induced diabetes compared to animals without diabetes . However, human research on the impact of diabetes on dental implant failure or complications is equivocal. Some studies show that diabetes increases the risk of implant failure by two-fold to three-fold compared to patients without diabetes , while others show no difference in failure rates associated with diabetes . Reviews of the overall body of evidence suggest that implant failures in patient with diabetes tend to occur early after placement furthermore, the percentage of patients with diabetes who experience implant failures appears to be relatively high but the percentage of implants that fail is similar to that of patients without diabetes .
Hyperglycemia/dm And Oral Health Mutually Affect Each Other
While type 1 DM is due to no or insufficient insulin production affecting about 5% of patients with DM, type 2 DM is a syndrome characterized by elevated blood glucose levels due to insufficient insulin production, insufficient insulin uptake, or both . About 463 million adults suffer from DM, with 700 million expected by the year 2045 . An additional 374 million people have prediabetes and are at risk of developing T2DM .
Systemic hyperglycemia causes complications such as retinopathy nephropathy neuropathy heart, peripheral arterial, and cerebrovascular disease obesity, cataracts erectile dysfunction and non-alcoholic fatty liver disease . Regardless of DM type, it is the hyperglycemia, not the diagnosis of DM per se, that leads to several oral complications and oral health-related decreased quality of life .
These oral manifestations are described, followed by any effects in the opposite direction.
For succinct brevity, DM is used for any type of diabetes or hyperglycemia and the comparison group is non-traditionally omitted. For example, in the sentence People with DM have greater xxxx, the comparison than people without DM is implicit, but not shown.
Also Check: Freestyle Lite Blood Glucose Test Strips Stores
Conscious Sedation For The Dental Treatment Of Diabetic Patients
Currently conscious sedation for dentistry has an excellent safety record. In order to maintain this the following recommendations should be considered for Type 1 diabetics or Type 2 diabetics taking insulin .
Table 5 Conscious sedation for the patient with insulin-dependent diabetes
Sedation clinicians should still use the ASA rating system for assessing the most appropriate setting for sedation. A tightly-controlled insulin-dependent diabetic may well be an ASA2 and with due care and attention could be treated in primary care. Secondary care with the potential use of a multi-disciplinary team may be a more appropriate venue for a poorly-controlled diabetic with co-morbidities.
Hopefully, these relatively simple suggestions will help to maintain the excellent safety record of conscious sedation for dentistry. In NO way are they meant to dissuade the clinician from treating the diabetic patient.
The Patient With Undiagnosed Diabetes
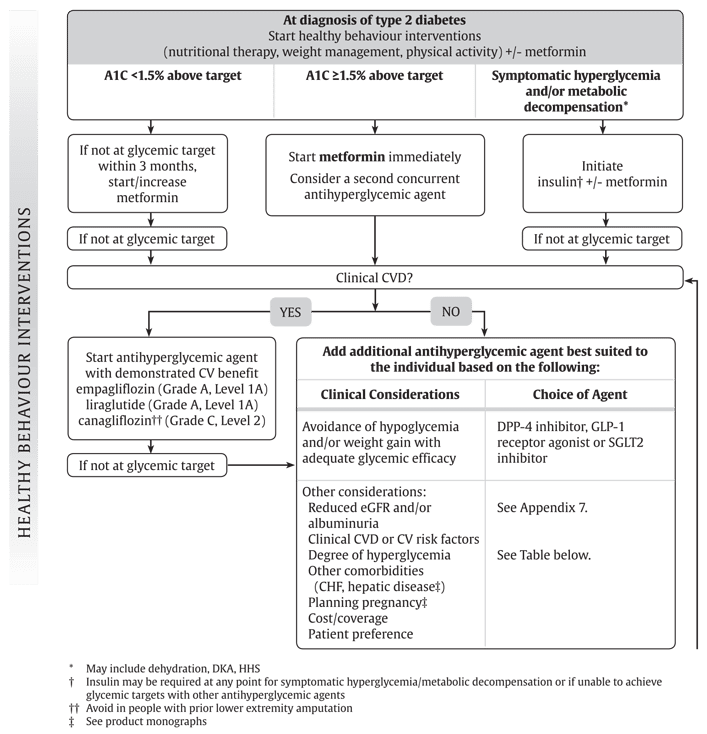
The U.S. Centers for Disease Control estimated in 2011 that approximately 25.8 million American have diabetes and that about 7 million of those individuals are undiagnosed . Patients with undiagnosed diabetes are a major target population for the dental office, because signs and symptoms of diabetes may present initially in the oral cavity . Dentists and dental hygienists may be the first to recognize signs and symptoms such as advanced periodontal diseases or other infections, burning mouth, xerostomia, or parotid enlargement. The medical history must be reviewed thoroughly to determine if the patient has been previously diagnosed with diabetes or if the patient has risk factors for diabetes such as prediabetes, overweight/obesity, racial risk factors, family history of diabetes, history of gestational diabetes, or others discussed in Chapter 2.
Diabetes is associated with an increased prevalence and severity of gingivitis and periodontitis, with the greatest risk in individuals with poor glycemic control . Poor glycemic control also increases the risk of periodontal disease progression over time . Signs and symptoms of undiagnosed diabetes may also be present in individuals with diagnosed diabetes in whom glycemic control is poor. These findings should initiate a clinical pathway of care directed toward medical evaluation of the patients diabetes condition. Interaction between the dentist and physician is a critical component of care.
Read Also: Alternatives To Glucose Test During Pregnancy
Totally Happy With Product
I bought this product because i had read that it removes deep body fat this is the fat that accumulates around your belly and many organs, this was confirmed on mayo clinic website. It also claims that it lowers blood sugar and cholesterol and boosts metabolism. all i know is that since i have started taking my weight has gradually decreased when all i am doing is trying to maintain. haven’t had sugar and cholesterol checked but definitely will continue to use. – J.S Wise
Dedicated To Improving Your Lifestyle Without Breaking The Bank
Here at Ezyabsorb, we developed our Berberine with the purpose of improving the lifestyle of people who have trouble keeping their blood sugar under control. Our goal is to provide the best possible supplement at the best possible value. We achieve this goal by providing you with a supplement that has seen positive results across the board in a real human study, at the incredible value of less than $30 per month, as well as a money back guarantee.
You May Like: Fasting Glucose 103 Should I Worry
Practical Considerations For Dentists Treating Diabetic Patients
Identifying the Diabetic Patient
In order to optimally treat diabetic patients, the first challenge for dentists is to identify those individuals who have diabetes. The most obvious way to accomplish this is to ask patients about their health status. Those who say that they have received a diabetes diagnosis should be asked which type they have. However, a negative response cannot be considered conclusive. The CDC reports that 27.8% of Americans with diabetes are undiagnosed, ie, more than 8 million diabetic Americans are unaware of their condition.1
Additional questions on the medical history form may help to alert dental office personnel to undiagnosed diabetes. These should include asking if patients have recently been tested for diabetes, if they have a first-degree relative with diabetes, how often they get up in the night to urinate, how much water they drink daily, and how quickly they become hungry again after being fully satiated . Female patients who have children should be asked if they ever developed gestational diabetes while pregnant, a significant risk factor.
Assessing the Diabetic Patients Glycemic Control
Treating the Diabetic Patient
Oral Changes Associated With Diabetes Mellitus
Poorly controlled diabetic patients are at risk for numerous oral complications such as periodontal disease, salivary gland dysfunction, infection, neuropathy, and poor healing. None of these complications are unique to diabetes. However, their presence may serve as an early clue to the possible presence of diabetes, prompting your dentist to perform or request further testing.
Periodontal Disease. Periodontal disease is a commonly observed dental problem for patients with diabetes. It is similar to the periodontal disease encountered among nondiabetic patients. However, as a consequence of the impaired immunity and healing associated with diabetes, it may be more severe and progress more rapidly . The potential for these changes points to the need for periodic professional evaluation and treatment.
Salivary Gland Dysfunction. Several changes to the salivary glands may occur in association with diabetes. The most commonly observed concern is dry mouth , but other findings may include gland enlargement, and an increased risk for developing salivary duct stones and gland infection.
Special Considerations for Patients with Diabetes in Need of Dental Care
You should see your dentist on a regular basis. Diabetic patients under good medical control are generally eligible and able to tolerate any and all types of dental care. One of the common complications your dentist wants to avoid having to manage is hypoglycemia .
You should always:
Also Check: How To Pass The Glucose Test
Oral Manifestations Of Diabetes
Besides previous mentioned complications, diabetes can also manifest with pathological changes and symptoms in the oral cavity. Moreover, the dentist may be the first health professional to suspect on presence of diabetes and refer patient for further examinations and treatment. Oral manifestations of diabetes are gingivitis and periodontitis, dry mouth, increased susceptibility to infections especially fungal, increased susceptibility to caries, burning sensation of oral mucosa and difficult wound healing.
Gingivitisand periodontitis are the most common oral complications of diabetes. Although both gingivitis and periodontal disease primarily are caused by bacteria from dental plaque, patients with diabetes have a three times greater risk of developing gingivitis and periodontitis compared with healthy population. There are several reasons for this. In patients with poorly controlled diabetes the number of destructive bacteria is increased than in patients with well-controlled diabetes and non-diabetic individuals.
There are also changes in the inflammatory response of the body polymorphonuclear leukocytes have reduced ability to migrate and they secrete more inflammatory mediators and proteolytic enzymes. All of this leads to more destruction of dental tissue than is the case in the normal healthy population.
Classification And Etiology Of Diabetes Mellitus
Most cases of DM can be classified as type 1 or type 2 . Prediabetes refers to a condition in which blood glucose levels are elevated, but not high enough to warrant a diagnosis of T2DM. People with prediabetes have an increased risk of developing DM in the future.4 To manage patients with DM adequately, a clinician should be able to understand and differentiate between T1DM and T2DM.
Type 1 Diabetes Mellitus
Approximately 510% of all DM cases are T1DM, which was formerly known as insulin-dependent DM.5 The condition is characterized by hyperglycemia that is secondary to cell-mediated autoimmune destruction of the pancreass insulin-producing beta cells.5 The etiology of pancreatic beta cell destruction is unknown, but is thought to result from a combination of poorly defined genetic and environmental factors. The autoimmune process can start in infancy, and, although most cases present in children or young adults, the disease can manifest at any age.6 Clinically, patients may present with polyuria, polydipsia or polyphagia, and, in many cases, T1DM results in absolute insulin deficiency and subsequent ketoacidosis.5 Despite increased hunger, weight loss is expected in a T1DM patient.6 This can be attributed to a compromised cellular glucose-uptake mechanism that is characteristic of individuals with impaired insulin function.
Type 2 Diabetes Mellitus
Read Also: Beat Type 2 Diabetes Diet
Diabetes And Dental Care
Having diabetes along with years of high glucose levels can cause problems with your teeth and gums. Learn why dental problems may occur, what to do about them, and how to prevent them.
People with diabetes, particularly those who over time have higher than recommended blood glucose levels, are at greater risk of developing dental problems, most commonly gum disease and loss of teeth.
Here is a list of daily self-care actions that can help keep teeth and gums healthy, as well as guidance on when and how often to seek dental care.
Transdisciplinary Care Initiated In The Dental Setting
Screening for T2DM in the Dental Office
Because about half the people with manifest DM and 90% of those with preDM are unaware thereof , the dental setting can be important for T2DM screening and referral , especially for dental patients who do not see a physician regularly . It is crucial to identify T2DM in its early stages during which the chances for reversal or mitigation are greatest . Periodontitis can serve as an early sign of T2DM , just like few teeth and recurrent periapical abscesses . Random blood glucose or HbA1c levels can be measured chairside by quick finger-prick blood sample analysis .
Interestingly, 3054% of dental patients who denied having DM had T2DM with 1.35.8% having manifest T2DM as reported from studies in Denmark , Saudi Arabia , Spain , United Kingdom , and the US , aided by electronic health records . Whereas, 7.8% of US minority elders , 17.2% of patients with Dutch periodontal, and, respectively, 14.6% and 19.1% of Indians had T2DM.
PreDM was found in 9.9% of unaware dental patients in Sweden , 28.7% in the US , and 46.6% among patients with Dutch periodontal .
Guidelines for Dental Care Providers and Their Patients
Such screening in dental offices is well-accepted by patients , dentists and physicians , and their professional organizations , and can lead to positive lifestyle changes and decreased HbA1c level .
You May Like: How I Reversed My Diabetes
Diabetes And Oral Health
Visit your dentist for regular checkups to prevent problems.
A healthy mouth is important for everyone, but high blood sugar can make it harder to keep your mouth healthy. If you have diabetes, learn how you can avoid oral health problems and keep a smile on your face.
Taking good care of your mouth is essential to general health and well-beingit even affects your self-esteem. Good oral health habits can help prevent pain and infections from tooth and gum disease.
If you have diabetes, taking care of your teeth is even more important. High blood sugar can weaken white blood cells. These are your bodys main way to fight infections that can occur in the mouth.
Keep that smile on your face, though! By managing your diabetes, you manage more than your blood sugaryoure helping to prevent gum disease and other infections in your mouth.
Treatment Plan And Therapy
After initial determination of the type of diabetes and medical management regimen, the dentist performs a thorough oral examination and develops a list of diagnoses. A preliminary treatment plan may also be formulated at this stage. If any acute lesions or conditions are found, they should be treated on an emergent basis . For example, if the patient has a periodontal abscess, it should be treated immediately in an appropriate fashion. The clinician should not delay treatment simply because the patient has diabetes. The presence of an acute infection may adversely influence glycemic control and should be treated as soon as it is recognized. The treatment done at this time is limited to managing the acute problem. To treat a periodontal abscess, the clinician may need to provide surgical or nonsurgical debridement of the defect, and systemic antibiotics may be indicated depending on the extent and severity of the infection. For routine dental treatment, there is little indication for routine use of prophylactic antibiotics in patients with diabetes. However, if an infection is present, antibiotics are generally indicated, especially if the patients glycemic control is poor.
Figure 5.3Clinical pathway of care: Treatment plan and therapy.
Don’t Miss: Low Blood Sugar With Type 2 Diabetes
Diabetes And Dental Treatment
Diabetes is a chronic disease characterized by elevated blood glucose level and metabolic disorders of carbohydrates, fats and proteins. Diabetes is caused by two reasons: when the pancreas stops completely or partially to produce hormone insulin or when the insulin is not effective in the body .
Type 1 diabetes occurs in 10% of patients, most often in children and adolescents. The etiology of this disease is still unclear. It is believed that this type of diabetes occurs as a result of an autoimmune destruction of insulin-producing beta cells in the pancreas . The disease has a sudden start with the appearance of symptoms such as frequent urination, excessive thirst, constant hunger, pronounced fatigue and lack of energy.
Type 2 diabetes occurs in 90% of patients, mainly adults over forty years of age. The disease occurs when the pancreas is not anymore able to produce sufficient amounts of hormone insulin to meet the needs of the organism or when the target cells become resistant to insulin . Symptoms of the disease develop gradually, are milder in intensity and in approximately 50% of cases are not present until the development of chronic complications. The most important risk factor for the development of type 2 diabetes is being overweight. At the time of diagnosis 60 to 80% of patients are overweight.
Results Of Periodontal Therapy
Many studies reviewed in other chapters in this text have examined the impact of diabetes on periodontal health and the potential impact of periodontal therapy on metabolic control of diabetes. However, there is much less research examining the outcomes of periodontal therapy in periodontitis patients with diabetes compared to those without diabetes. In many of the studies of the effects of periodontal therapy in patients with diabetes, the average changes in probing depth and attachment level seen following scaling and root planing are similar in magnitude to studies of scaling and root planing performed in people without diabetes. However, these are not controlled trials of periodontal treatment in individuals with and without diabetes and therefore provide only low-level evidence that patients with diabetes as a group respond well to periodontal therapy.
You May Like: How To Test Your Blood Sugar